Head and neck cancer
| Head and neck cancer | |
|---|---|
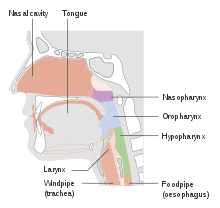 | |
| Parts of the head and neck that can be affected by cancer. | |
| Specialty | Oncology, oral and maxillofacial surgery |
| Symptoms | Lump or sore that does not heal, sore throat that does not go away, trouble swallowing, change in voice[1] |
| Risk factors | Alcohol, tobacco, betel quid, human papillomavirus, radiation exposure, certain workplace exposures, Epstein–Barr virus[1][2] |
| Diagnostic method | Tissue biopsy[1] |
| Prevention | Not using tobacco or alcohol[2] |
| Treatment | Surgery, radiation therapy, chemotherapy, targeted therapy[1] |
| Frequency | 5.5 million (affected during 2015)[3] |
| Deaths | 379,000 (2015)[4] |
Head and neck cancer develops from tissues in the lip and oral cavity (mouth), larynx (throat), salivary glands, nose, sinuses, or skin of the face.[5] The most common types of head and neck cancer occur in the lips, mouth, and larynx.[5] Symptoms predominantly include a sore that does not heal or a change in the voice.[1] In those with advanced disease, there may be unusual bleeding, facial pain, numbness or swelling, and visible lumps on the outside of the neck or oral cavity. Given the location of these cancers, it is possible for an afflicted individual to experience difficulty breathing.[6]
The majority of head and neck cancer is caused by the use of alcohol or tobacco, including smokeless tobacco, with increasing cases linked to the human papillomavirus (HPV).[6][2] Other risk factors include the Epstein–Barr virus, betel quid, radiation exposure, and certain workplace exposures.[6] About 90% are pathologically classified as squamous cell cancers.[7][2] The diagnosis is confirmed by a tissue biopsy.[6] The degree of surrounding tissue invasion and distant spread may be determined by medical imaging and blood tests.[6]
Not using tobacco or alcohol can reduce the risk of head and neck cancer.[2] The HPV vaccine may reduce the lifetime risk of oral cancer if taken prior to the onset of sexual activity, but confirmation will likely not be known until around 2060.[8] This is because oropharyngeal cancer typically presents in the 4th–6th decade of life, and this is a relatively new vaccine. While screening in the general population does not appear to be useful, screening high-risk groups by examination of the throat might be useful.[2] Head and neck cancer is often curable if it is diagnosed early; however, outcomes are typically poor if it is diagnosed late.[2] Treatment may include a combination of surgery, radiation therapy, chemotherapy, and targeted therapy.[6] Previous diagnosis and treatment of a head and neck cancer confer a higher risk of developing a second head and neck cancer or recurrence.[6]
Globally, head and neck cancer accounts for 650,000 new cases of cancer and 330,000 deaths annually on average. In 2018, it was the seventh most common cancer worldwide, with 890,000 new cases documented and 450,000 people dying from the disease.[8] In the United States, head and neck cancer makes up 3% of all cancer cases (averaging 53,000 new diagnoses per year) and 1.5% of cancer deaths.[9] The 2017 worldwide figure cites head and neck cancers as representing 5.3% of all cancers (not including non-melanoma skin cancers).[10][5] Notably, head and neck cancer secondary to chronic alcohol or tobacco use has been steadily declining as less of the population chronically smokes tobacco.[8] However, HPV-associated oropharyngeal cancer is rising, particularly in younger people in westernized nations, which is thought to be reflective of changes in oral sexual practices, specifically with regard to the number of oral sexual partners.[5][8] This increase since the 1970s has mostly affected wealthier nations and male populations.[11][12][5] This is due to evidence suggesting that transmission rates of HPV from women to men are higher than from men to women, as women often have a higher immune response to infection.[5][13]
The usual age at diagnosis is between 55 and 65 years old.[14] The average 5-year survival following diagnosis in the developed world is 42–64%.[14][15]
Signs and symptoms[edit]
Head and neck cancers can cause a broad range of symptoms, many of which occur together. These can be categorised local (head and neck cancer-specific), general and gastrointestinal symptoms. Local symptoms include changes in taste and voice, inflammation of the mouth or throat (mucositis), dry mouth (xerostomia), and difficulty swallowing (dysphagia). General symptoms include difficulty sleeping, tiredness, depression, nerve damage (peripheral neuropathy). Gastrointestinal symptoms are typically nausea and vomiting.[16]
Symptoms predominantly include a sore on the face or oral cavity that does not heal, trouble swallowing, or a change in voice. In those with advanced disease, there may be unusual bleeding, facial pain, numbness or swelling, and visible lumps on the outside of the neck or oral cavity.[17] Head and neck cancer often begins with benign signs and symptoms of the disease, like an enlarged lymph node on the outside of the neck, a hoarse-sounding voice, or a progressive worsening cough or sore throat. In the case of head and neck cancer, these symptoms will be notably persistent and become chronic. There may be a lump or a sore in the throat or neck that does not heal or go away. There may be difficulty or pain in swallowing. Speaking may become difficult. There may also be a persistent earache.[18]
Other symptoms can include: a lump in the lip, mouth, or gums; ulcers or mouth sores that do not heal; bleeding from the mouth or numbness; bad breath; discolored patches that persist in the mouth; a sore tongue; and slurring of speech if the cancer is affecting the tongue. There may also be congested sinuses, weight loss, and some numbness or paralysis of facial muscles.
Mouth[edit]

Squamous cell cancers are common in areas of the mouth, including the inner lip, tongue, floor of the mouth, gums, and hard palate. Cancers of the mouth are strongly associated with tobacco use, especially the use of chewing tobacco or dipping tobacco, as well as heavy alcohol use. Cancers of this region, particularly the tongue, are more frequently treated with surgery than other head and neck cancers. Lip and oral cavity cancers are the most commonly encountered types of head and neck cancer.[5]
Surgeries for oral cancers include:
- Maxillectomy (can be done with or without orbital exenteration)
- Mandibulectomy (removal of the lower jaw or part of it)
- Glossectomy (tongue removal; can be total, hemi, or partial)
- Radical neck dissection
- Combinational (e.g., glossectomy and laryngectomy done together).
The defect is typically covered or improved by using another part of the body and/or skin grafts and/or wearing a prosthesis.
Nose[edit]
Paranasal sinus and nasal cavity cancer affects the nasal cavity and the paranasal sinuses. Most of these cancers are squamous cell carcinomas.[19]
Nasopharynx[edit]
Nasopharyngeal cancer arises in the nasopharynx, the region in which the nasal cavities and the Eustachian tubes connect with the upper part of the throat. While some nasopharyngeal cancers are biologically similar to the common head and neck squamous cell carcinomas (HNSCCs), "poorly differentiated" nasopharyngeal carcinoma is lymphoepithelioma, which is distinct in its epidemiology, biology, clinical behavior, and treatment and is treated as a separate disease by many experts.
Throat[edit]
Most oropharyngeal cancers are squamous cell carcinomas that begin in the oropharynx (throat), the middle part of the throat that includes the soft palate, the base of the tongue, and the tonsils.[1] Squamous cell cancers of the tonsils are more strongly associated with human papillomavirus infection than are cancers of other regions of the head and neck. HPV-positive oropharyngeal cancer generally has a better outcome than HPV-negative disease, with a 54% better survival rate,[20] but this advantage for HPV-associated cancer applies only to oropharyngeal cancers.[21]
People with oropharyngeal carcinomas are at high risk of developing a second primary head and neck cancer.[22]
Hypopharynx[edit]
The hypopharynx includes the pyriform sinuses, the posterior pharyngeal wall, and the postcricoid area. Tumors of the hypopharynx frequently have an advanced stage at diagnosis and have the most adverse prognoses of pharyngeal tumors. They tend to metastasize early due to the extensive lymphatic network around the larynx.
Larynx[edit]
Laryngeal cancer begins in the larynx, or "voice box", and is the second most common type of head and neck cancer encountered.[5] Cancer may occur on the vocal folds themselves ("glottic" cancer) or on tissues above and below the true cords ("supraglottic" and "subglottic" cancers, respectively). Laryngeal cancer is strongly associated with tobacco smoking.
Surgery can include laser excision of small vocal cord lesions, partial laryngectomy (removal of part of the larynx), or total laryngectomy (removal of the whole larynx). If the whole larynx has been removed, the person is left with a permanent tracheostomy. Voice rehabilitation in such patients can be achieved in three important ways: esophageal speech, tracheoesophageal puncture, or electrolarynx. One would likely require intensive teaching, speech therapy, and/or an electronic device.
Trachea and salivary glands[edit]
Cancer of the trachea is a rare cancer usually classified as a lung cancer.[23]
Most tumors of the salivary glands differ from the common squamous cell carcinomas of the head and neck in cause, histopathology, clinical presentation, and therapy. Other uncommon tumors arising in the head and neck include teratomas, adenocarcinomas, adenoid cystic carcinomas, and mucoepidermoid carcinomas.[24] Rarer still are melanomas and lymphomas of the upper aerodigestive tract.
Causes[edit]
Alcohol and tobacco[edit]
Alcohol and tobacco use are major risk factors for head and neck cancer. 72% of head and neck cancer cases are caused by using both alcohol and tobacco.[25] This rises to 89% when looking specifically at laryngeal cancer.[26]
There is thought to be a dose-dependent relationship between alcohol use and development of head and neck cancer where higher rates of alcohol consumption contribute to an increased risk of developing head and neck cancer.[27][28] Alcohol use following a diagnosis of head and neck cancer also contributes to other negative outcomes. These include physical effects such as an increased risk of developing a second primary cancer or other malignancies,[29][30] cancer recurrence,[31] and worse prognosis[32] in addition to an increased chance of having a future feeding tube placed and osteoradionecrosis of the jaw. Negative social factors are also increased with sustained alcohol use after diagnosis including unemployment and work disability.[33][34]
The way in which alcohol contributes to cancer development is not fully understood. It is thought to be related to permanent damage of DNA strands by a metabolite of alcohol called acetaldehyde. Other suggested mechanisms include nutritional deficiencies and genetic variations.[33]
Tobacco smoking is one of the main risk factors for head and neck cancer. Cigarette smokers have a lifetime increased risk for head and neck cancer that is 5 to 25 times higher than the general population.[35] The ex-smoker's risk of developing head and neck cancer begins to approach the risk in the general population 15 years after smoking cessation.[36] In addition, people who smoke have a worse prognosis than those who have never smoked.[37] Furthermore, people who continue to smoke after diagnosis of head and neck cancer have the highest probability of dying compared to those who have never smoked.[38][39] This effect is seen in patients with HPV-positive head and neck cancer as well.[40][41][42] It has also been demonstrated that passive smoking, both at work and at home, increases the risk of head and neck cancer.[25]
A major carcinogenic compound in tobacco smoke is acrylonitrile.[43] Acrylonitrile appears to indirectly cause DNA damage by increasing oxidative stress, leading to increased levels of 8-oxo-2'-deoxyguanosine (8-oxo-dG) and formamidopyrimidine in DNA.[44] (see image). Both 8-oxo-dG and formamidopyrimidine are mutagenic.[45][46] DNA glycosylase NEIL1 prevents mutagenesis by 8-oxo-dG[47] and removes formamidopyrimidines from DNA.[48]
Smokeless tobacco (including products where tobacco is chewed) is a cause of oral cancer. This link has been established in the United States but particularly in Southeast Asian countries where the use of smokeless tobacco is common.[5][49][50] Smokeless tobacco is associated with a higher risk of developing head and neck cancer due to the presence of the tobacco-specific carcinogen N’-nitrosonornicotine.[50]
Cigar and pipe smoking are also important risk factors for oral cancer.[51] They have a dose dependent relationship with more consumption leading to higher chances of developing cancer.[25] The use of electronic cigarettes may also lead to the development of head and neck cancers due to the substances like propylene glycol, glycerol, nitrosamines, and metals contained therein, which can cause damage to the airways.[52][5] Exposure to e-vapour has been shown to reduce cell viability and increase the rate of cell death via apoptosis or necrosis with or without nicotine.[53] This area of study requires more research, however.[52][5] Use of marijuana, has currently not been shown to be associated with head and neck cancer risk.[54]
Diet[edit]
Many dietary nutrients are associated with cancer protection and its development. Generally, foods with a protective effect with respect to oral cancer demonstrate antioxidant and anti-inflammatory effects such as fruits, vegetables, curcumin and green tea. Conversely, pro-inflammatory food substances such as red meat, processed meat and fried food can increase the risk of developing head and neck cancer.[25][55] An increased adherence to the Mediterranean diet is also related to a lower risk of cancer mortality and a reduced risk of developing multiple cancers including head and neck cancer.[56] Elevated levels of nitrites in preserved meats and salted fish have been shown to increase the risk of nasopharyngeal cancer.[57][58] Overall, a poor nutritional intake (often associated with alcoholism) with subsequent vitamin deficiencies is a risk factor for head and neck cancer.[57][24]
In terms of nutritional supplements, antioxidants such as vitamin E and beta-carotene might reduce the toxic effect of radiotherapy in people with head and neck cancer but they can also increase recurrence rates, especially in smokers.[59]
Betel nut[edit]
Betel nut chewing is associated with an increased risk of squamous cell carcinoma of the head and neck.[1][60] When chewed with additional tobacco in its preparation (like in gutka), there is an even higher risk, especially for oral and oropharyngeal cancers.[25]
Genetics[edit]
People who develop head and neck cancer may have a genetic predisposition for the condition. There are seven known genetic variations (loci) which specifically increase the chances of developing oral and pharyngeal cancer.[61][62] Family history, that is having a first-degree relative with head and neck cancer, is also a risk factor. In addition, genetic variations in pathways involved in alcohol metabolism (for example alcohol dehydrogenase) have been associated with an increased head and neck cancer risk.[25]
Radiation[edit]
It is known that prior exposure to radiation of the head and neck is associated with an increased risk of cancer, particularly thyroid, salivary gland and squamous cell carcinomas, although there is a time-delay of many years and the overall risk is still low. [57]
Infection[edit]
Human papillomavirus[edit]
Some head and neck cancers, and in particular oropharyngeal cancer, are caused by the human papillomavirus (HPV),[1][63] and 70% of all head and neck cancer cases are related to HPV.[63] Risk factors for HPV-positive oropharyngeal squamous-cell carcinomas (OSCC) include multiple sexual partners, anal and oral sex and a weak immune system.[57]
The incidence of HPV-related head and neck cancer is increasing, especially in the Western world. In the United States, the incidence of HPV-positive oropharyngeal cancer has overtaken HPV-positive cervical cancer as the leading HPV related cancer type.[64] An increased incidence has particularly affected males. As a result, recent changes have resulted in the HPV vaccine being offered to adolescent boys between 12-13 (previously only offered to girls between this age due to cervical cancer risks) and men under 45 who have sex with men in the UK.[65][66]
Over 20 different high-risk HPV subtypes have been implicated in causing head and neck squamous-cell carcinomas (HNSCC). In particular, HPV-16 is responsible for up to 90% of oropharyngeal squamous cell carcinomas in North America.[57] Approximately 15–25% of HNSCC contain genomic DNA from HPV,[67] and the association varies based on the site of the tumor.[68] In the case of HPV-positive oropharyngeal cancer, the highest distribution is in the tonsils, where HPV DNA is found in 45–67% of the cases,[69] and it is less often in the hypopharynx (13–25%), and least often in the oral cavity (12–18%) and larynx (3–7%).[70][71]
Positive HPV16 status is associated with a improved prognosis over HPV-negative oropharyngeal cancer due to better response to radiotherapy and chemotherapy.[72]
HPV can induce tumors by several mechanisms:[72][73]
- E6 and E7 oncogenic proteins.
- Disruption of tumor suppressor genes.
- High-level DNA amplifications, for example, oncogenes.
- Generating alternative nonfunctional transcripts.
- Interchromosomal rearrangements.
- Distinct host genome methylation and expression patterns, produced even when the virus is not integrated into the host genome.
There are observed biological differences between HPV-positive and HPV-negative head and neck cancer, for example in terms of mutation patterns. In HPV-negative disease, genes frequently mutated include TP53, CDKN2A and PIK3CA.[74] In HPV-positive disease, these genes are less frequently mutated, and the tumour suppressor gene p53 and pRb (protein retinoblastoma) are commonly inactivated by HPV oncoproteins E6 and E7 respectively.[75] In addition, viral infections such as HPV can cause aberrant DNA methylation during cancer development. HPV-positive head and neck cancers demonstrate higher levels of such DNA methylation compared to HPV-negative disease.[76]
E6 sequesters p53 to promote p53 degradation, while E7 inhibits pRb. Degradation of p53 results in cells being unable to respond to checkpoint signals that are normally present to activate apoptosis when DNA damage is signalled. Loss of pRb leads to deregulation of cell proliferation and apoptosis. Both mechanisms therefore leave cell proliferation unchecked and increase the chance of carcinogenesis.[77]
Epstein–Barr virus[edit]
Epstein–Barr virus (EBV) infection is associated with nasopharyngeal cancer. Nasopharyngeal cancer caused by EBV commonly occurs in some countries of the Mediterranean and Asia, where EBV antibody titers can be measured to screen high-risk populations.[78][79]
Gastroesophageal reflux disease[edit]
The presence of gastroesophageal reflux disease (GERD) or laryngeal reflux disease can also be a major factor. Stomach acids that flow up through the esophagus can damage its lining and raise susceptibility to throat cancer.
Hematopoietic stem cell transplantation[edit]
People after hematopoietic stem cell transplantation (HSCT) are at a higher risk for oral squamous cell carcinoma. Post-HSCT oral cancer may have more aggressive behavior and a poorer prognosis when compared to oral cancer in non-HSCT patients.[80] This effect is supposed to be due to continuous, lifelong immune suppression and chronic oral graft-versus-host disease.[80]
Other risk factors[edit]
Several other risk factors have been identified in the development of head and neck cancer. These include occupational environmental carcinogen exposure such as asbestos, wood dust, mineral acid, sulfuric acid mists and metal dusts. In addition, weakened immune systems, age greater than 55 years, poor socioeconomic factors such as lower incomes and occupational status, and low body mass index (<18.5 kg/m2) are also risk factors.[57][81][25] Poor oral hygiene and chronic oral cavity inflammation (for example secondary to chronic gum inflammation) are also linked to an increased head and neck cancer risk.[82][83] The presence of leukoplakia, which is the appearance of white patches or spots in the mouth, can develop into cancer in about 1⁄3 of cases.[24]
Diagnosis[edit]
A significant proportion of people with head and neck cancer will present to their physicians with an already advanced stage disease.[84] This can either be down to patient factors (delays in seeking medical attention), or physician factors (such as delays in referral from primary care, or non-diagnostic investigation results).[85]
A person usually presents to the physician complaining of one or more of the typical symptoms. These symptoms may be site specific (such as a laryngeal cancer causing hoarse voice), or not site specific (earache can be caused by multiple types of head and neck cancers).[16]
The physician will undertake a thorough history to determine the nature of the symptoms and the presence or absence of any risk factors. The physician will also ask about other illnesses such as heart or lung diseases as they may impact their fitness for potentially curative treatment. Clinical examination will involve examination of the neck for any masses, examining inside the mouth for any abnormalities and assessing the rest of the pharynx and larynx with a nasendoscope.[86]
Further investigations will be directed by the symptoms discussed and any abnormalities identified during the exam.
Neck masses typically undergo assessment with ultrasound and a fine-needle aspiration (FNA, a type of needle biopsy). Concerning lesions that are readily accessible (such as in the mouth) can be biopsied with a local anaesthetic. Lesions less readily available can be biopsied either with the patient awake or under a general anaesthetic depending on local expertise and availability of specialist equipment.[87]
The cancer will also need to be staged (accurately determine its size, association with nearby structures, and spread to distant sites). This is typically done by scanning the patient with a combination of magnetic resonance imaging (MRI), computed tomography (CT) and/or positron emission tomography (PET). Exactly which investigations are required will depend on a variety of factors such as the site of concern and the size of the tumour.[88]
Some people will present with a neck lump containing cancer cells (identified by FNA) that have spread from elsewhere, but with no identifiable primary site on initial assessment. In such cases people will undergo additional testing to attempt to find the initial site of cancer, as this has significant implications for their treatment. These patients undergo MRI scanning, PET-CT and then panendoscopy and biopsies of any abnormal areas. If the scans and panendoscopy still do not identify a primary site for the cancer, affected people will undergo a bilateral tonsillectomy and tongue base mucosectomy (as these are the most common subsites of cancer that spread to the neck). This procedure can be done with or without robotic assistance.[89]
Once a diagnosis is confirmed, a multidisciplinary discussion of the optimal treatment strategy will be undertaken between the radiation oncologist, surgical oncologist, and medical oncologist. A histopathologist and a radiologist will also be present to discuss the biopsy and imaging findings.[88] Most (90%) cancers of the head and neck are squamous cell-derived, termed "head-and-neck squamous-cell carcinomas".[7]
Histopathology[edit]
Throat cancers are classified according to their histology or cell structure and are commonly referred to by their location in the oral cavity and neck. This is because where the cancer appears in the throat affects the prognosis; some throat cancers are more aggressive than others, depending on their location. The stage at which the cancer is diagnosed is also a critical factor in the prognosis of throat cancer. Treatment guidelines recommend routine testing for the presence of HPV for all oropharyngeal squamous cell carcinoma tumors.[90]
Squamous-cell carcinoma[edit]
Squamous-cell carcinoma is a cancer of the squamous cell, a kind of epithelial cell found in both the skin and mucous membranes. It accounts for over 90% of all head and neck cancers,[91] including more than 90% of throat cancer.[24] Squamous cell carcinoma is most likely to appear in males over 40 years of age with a history of heavy alcohol use coupled with smoking.
All squamous cell carcinomas arising from the oropharynx, and all neck node metastases of unknown primary should undergo testing for HPV status. This is essential to adequately stage the tumour and adequately plan treatment. Due to the different biology of HPV positive and negative cancers, differentiating HPV status is also important for ongoing research to determine the best treatments.[92]
Nasopharyngeal carcinomas, or neck node metastases possibly arising from the nasopharynx will also be tested for Ebstein Barr virus.[93]
The tumor marker Cyfra 21-1 may be useful in diagnosing squamous cell carcinoma of the head and neck (SCCHN).[94]
Adenocarcinoma[edit]
Adenocarcinoma is a cancer of the epithelial tissue that has glandular characteristics. Several head and neck cancers are adenocarcinomas (either of intestinal or non-intestinal cell types).[91]
Prevention[edit]
Avoidance of recognized risk factors (such as smoking and alcohol) is the single most effective form of prevention. Regular dental examinations may identify pre-cancerous lesions in the oral cavity.[1]
When diagnosed early, oral, head, and neck cancers can be treated more easily, and the chances of survival increase tremendously.[1] The HPV vaccine helps to prevent the development of HPV-related oropharyngeal cancer.[95]
Management[edit]
Improvements in diagnosis and local management, as well as targeted therapy, have led to improvements in quality of life and survival for people with head and neck cancer.[96]
After a histologic diagnosis has been established and tumor extent determined, such as with the use of PET-CT,[97] the selection of appropriate treatment for a specific cancer depends on a complex array of variables, including tumor site, relative morbidity of various treatment options, concomitant health problems, social and logistic factors, previous primary tumors, and the person's preference. Treatment planning generally requires a multidisciplinary approach involving specialist surgeons, medical oncologists, and radiation oncologists. [citation needed]
Surgical resection and radiation therapy are the mainstays of treatment for most head and neck cancers and remain the standard of care in most cases. For small primary cancers without regional metastases (stage I or II), wide surgical excision alone or curative radiation therapy alone is used. For more extensive primary tumors or those with regional metastases (stage III or IV), planned combinations of pre- or postoperative radiation and complete surgical excision are generally used. More recently, as historical survival and control rates have been recognized as less than satisfactory, there has been an emphasis on the use of various induction or concomitant chemotherapy regimens.
Surgery[edit]
Surgery as a treatment is frequently used for most types of head and neck cancer. Usually, the goal is to remove the cancerous cells entirely. This can be particularly tricky if the cancer is near the larynx and can result in the person being unable to speak. Surgery is also commonly used to resect (remove) some or all of the cervical lymph nodes to prevent further spread of the disease. Transoral robotic surgery (TORS) is gaining popularity worldwide as the technology and training become more accessible. It now has an established role in the treatment of early stage oropharyngeal cancer.[98] There is also a growing trend worldwide towards TORS for the surgical treatment of laryngeal and hypopharyngeal tumours.[99][100]
CO2 laser surgery is also another form of treatment. Transoral laser microsurgery allows surgeons to remove tumors from the voice box with no external incisions. It also allows access to tumors that are not reachable with robotic surgery. During the surgery, the surgeon and pathologist work together to assess the adequacy of excision ("margin status"), minimizing the amount of normal tissue removed or damaged.[101] This technique helps give the person as much speech and swallowing function as possible after surgery.[102]
Radiation therapy[edit]

Radiation therapy is the most common form of treatment. There are different forms of radiation therapy, including 3D conformal radiation therapy, intensity-modulated radiation therapy, particle beam therapy, and brachytherapy, which are commonly used in the treatment of cancers of the head and neck. Most people with head and neck cancer who are treated in the United States and Europe are treated with intensity-modulated radiation therapy using high-energy photons. At higher doses, head and neck radiation is associated with thyroid dysfunction and pituitary axis dysfunction.[103] Radiation therapy for head and neck cancers can also cause acute skin reactions of varying severity, which can be treated and managed with topically applied creams or specialist films.[104]
Chemotherapy[edit]
Chemotherapy for throat cancer is not generally used to cure the cancer as such. Instead, it is used to provide an inhospitable environment for metastases so that they will not establish themselves in other parts of the body. Typical chemotherapy agents are a combination of paclitaxel and carboplatin. Cetuximab is also used in the treatment of throat cancer.
Docetaxel-based chemotherapy has shown a very good response in locally advanced head and neck cancer. Docetaxel is the only taxane approved by the FDA for head and neck cancer, in combination with cisplatin and fluorouracil for the induction treatment of inoperable, locally advanced squamous cell carcinoma of the head and neck.[105]
While not specifically a chemotherapy, amifostine is often administered intravenously by a chemotherapy clinic prior to IMRT radiotherapy sessions. Amifostine protects the gums and salivary glands from the effects of radiation.[citation needed]
There is no evidence that erythropoietin should be routinely given with radiotherapy.[106]
Photodynamic therapy[edit]
Photodynamic therapy may have promise for treating mucosal dysplasia and small head and neck tumors.[24] Amphinex is showing good results in early clinical trials for the treatment of advanced head and neck cancer.[107]
Targeted therapy[edit]
Targeted therapy, according to the National Cancer Institute, is "a type of treatment that uses drugs or other substances, such as monoclonal antibodies, to identify and attack specific cancer cells without harming normal cells." Some targeted therapies used in squamous cell carcinomas of the head and neck include cetuximab, bevacizumab, and erlotinib.
Cetuximab is used for treating people with advanced-stage cancer who cannot be treated with conventional chemotherapy (cisplatin).[108][109] However, cetuximab's efficacy is still under investigation by researchers.[110]
Gendicine is a gene therapy that employs an adenovirus to deliver the tumor suppressor gene p53 to cells. It was approved in China in 2003 for the treatment of head and neck squamous cell carcinoma.[111]
The mutational profiles of HPV+ and HPV- head and neck cancer have been reported, further demonstrating that they are fundamentally distinct diseases. [112][non-primary source needed]
Immunotherapy[edit]
Immunotherapy is a type of treatment that activates the immune system to fight cancer. One type of immunotherapy, immune checkpoint blockade, binds to and blocks inhibitory signals on immune cells to release their anti-cancer activities.
In 2016, the FDA granted accelerated approval to pembrolizumab for the treatment of people with recurrent or metastatic HNSCC with disease progression on or after platinum-containing chemotherapy.[113] Later that year, the FDA approved nivolumab for the treatment of recurrent or metastatic HNSCC with disease progression on or after platinum-based chemotherapy.[114] In 2019, the FDA approved pembrolizumab for the first-line treatment of metastatic or unresectable recurrent HNSCC.[115]
Treatment side effects[edit]
Depending on the treatment used, people with head and neck cancer may experience the following symptoms and treatment side effects:[24][104]
- Eating problems
- Pain associated with lesions
- Mucositis
- Nephrotoxicity and ototoxicity
- Xerostomia
- Gastroesophageal reflux
- Radiation-induced osteonecrosis of the jaw
- Radiation-induced acute skin reactions
Psychosocial[edit]
Programs to support the emotional and social well-being of people who have been diagnosed with head and neck cancer may be offered.[116] There is no clear evidence on the effectiveness of these interventions or any particular type of psychosocial program or length of time that is most helpful for those with head and neck cancer.[116]
Prognosis[edit]
Although early-stage head and neck cancers (especially laryngeal and oral cavity) have high cure rates, up to 50% of people with head and neck cancer present with advanced disease.[117] Cure rates decrease in locally advanced cases, whose probability of cure is inversely related to tumor size and even more so to the extent of regional node involvement. [citation needed] HPV-associated oropharyngeal cancer has been shown to respond better to chemoradiation and, subsequently, have a better prognosis compared to non-associated HPV head and neck cancer.[8]
Consensus panels in America (AJCC) and Europe (UICC) have established staging systems for head and neck squamous-cell cancers. These staging systems attempt to standardize clinical trial criteria for research studies and define prognostic categories of disease. Squamous cell cancers of the head and neck are staged according to the TNM classification system, where T is the size and configuration of the tumor, N is the presence or absence of lymph node metastases, and M is the presence or absence of distant metastases. The T, N, and M characteristics are combined to produce a "stage" of the cancer, from I to IVB.[118]
Problem of second primaries[edit]
Survival advantages provided by new treatment modalities have been undermined by the significant percentage of people cured of head and neck squamous cell carcinoma (HNSCC) who subsequently develop second primary tumors. The incidence of second primary tumors ranges in studies from 9%[119] to 23%[120] at 20 years. Second primary tumors are the major threat to long-term survival after successful therapy of early-stage HNSCC.[121] Their high incidence results from the same carcinogenic exposure responsible for the initial primary process, called field cancerization.
Digestive system[edit]
Many people with head and neck cancer are also not able to eat sufficiently. A tumor may impair a person's ability to swallow and eat, and throat cancer may affect the digestive system. The difficulty in swallowing can cause a person to choke on their food in the early stages of digestion and interfere with the food's smooth travel down into the esophagus and beyond.
The treatments for throat cancer can also be harmful to the digestive system as well as other body systems. Radiation therapy can lead to nausea and vomiting, which can deprive the body of vital fluids (although these may be obtained through intravenous fluids if necessary). Frequent vomiting can lead to an electrolyte imbalance, which has serious consequences for the proper functioning of the heart. Frequent vomiting can also upset the balance of stomach acids, which has a negative impact on the digestive system, especially the lining of the stomach and esophagus.
Enteral feeding, a method that adds nutrients directly into a person's stomach using a nasogastric feeding tube or a gastrostomy tube, may be necessary for some people.[122] Further research is required to determine the most effective method of enteral feeding to ensure that people undergoing radiotherapy or chemoradiation treatment are able to stay nourished during their treatment.[122]
Mental health[edit]
Cancer in the head or neck may impact a person's mental well-being and can sometimes lead to social isolation.[116] This largely results from a decreased ability or inability to eat, speak, or effectively communicate. Physical appearance is often altered by the cancer itself and/or as a consequence of treatment side effects. Psychological distress may occur, and feelings such as uncertainty and fear may arise.[116] Some people may also have a changed physical appearance, differences in swallowing or breathing, and residual pain to manage.[116]
Caregiver stress
Caregivers for people with head and neck cancer show higher rates of caregiver stress and poorer mental health compared to both the general population and those caring for non-head and neck cancer patients.[123] The high symptom burden patients' experience necessitates complex caregiver roles, often requiring hospital staff training, which caregivers can find distressing when asked to do so for the first time. It is becoming increasingly apparent that caregivers (most often spouses, children, or close family members) might not be adequately informed about, prepared for, or trained for the tasks and roles they will encounter during the treatment and recovery phases of this unique patient population, which span both technical and emotional support.[124] Of note, caregivers of patients who report lower quality of life demonstrate increased burden and fatigue that extend beyond the treatment phase.
Examples of technically difficult caregiver duties include tube feeding, oral suctioning, wound maintenance, medication delivery safe for tube feeding, and troubleshooting home medical equipment. If the cancer affects the mouth or larynx, caregivers must also find a way to effectively communicate among themselves and with their healthcare team. This is in addition to providing emotional support for the person undergoing cancer therapy.[124]
Others[edit]
Like any cancer, metastasis affects many areas of the body as the cancer spreads from cell to cell and organ to organ. For example, if it spreads to the bone marrow, it will prevent the body from producing enough red blood cells and affect the proper functioning of the white blood cells and the body's immune system; spreading to the circulatory system will prevent oxygen from being transported to all the cells of the body; and throat cancer can throw the nervous system into chaos, making it unable to properly regulate and control the body.
Epidemiology[edit]

The number of new cases of head and neck cancer in the United States was 40,490 in 2006, accounting for about 3% of adult malignancies. A total of 11,170 people died of their disease in 2006.[126] The worldwide incidence exceeds half a million cases annually. In North America and Europe, the tumors usually arise from the oral cavity, oropharynx, or larynx, whereas nasopharyngeal cancer is more common in the Mediterranean countries and in the Far East. In Southeast China and Taiwan, head and neck cancer, specifically nasopharyngeal cancer, is the most common cause of death in young men.[127]
- In 2008, there were 22,900 cases of oral cavity cancer, 12,250 cases of laryngeal cancer, and 12,410 cases of pharyngeal cancer in the United States.[24]
- In 2002, 7,400 Americans were projected to die of these cancers.[128]
- More than 70% of throat cancers are at an advanced stage when discovered.[129]
- Men are 89% more likely than women to be diagnosed with these cancers and are almost twice as likely to die of them.[128]
- African Americans are disproportionately affected by head and neck cancer, with younger ages of incidence, increased mortality, and more advanced disease at presentation.[117] Laryngeal cancer incidence is higher in African Americans relative to white, Asian, and Hispanic populations. There is a lower survival rate for similar tumor states in African Americans with head and neck cancer.[24]
- Smoking and tobacco use are directly related to oropharyngeal (throat) cancer deaths.[130]
- The risk of developing head and neck cancer increases with age, especially after 50 years. Most people who do so are between 50 and 70 years old.[24]
Research[edit]
Immunotherapy with immune checkpoint inhibitors is being investigated in head and neck cancers.[131]
References[edit]
- ^ a b c d e f g h i j "Oropharyngeal Cancer Treatment (Adult) (PDQ®)–Patient Version". National Cancer Institute. 22 November 2019. Retrieved 28 November 2019.
- ^ a b c d e f g World Cancer Report 2014. World Health Organization. 2014. pp. Chapter 5.8. ISBN 978-9283204299.
- ^ Vos T, Allen C, Arora M, Barber RM, Bhutta ZA, Brown A, et al. (GBD 2015 Disease and Injury Incidence and Prevalence Collaborators) (October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMC 5055577. PMID 27733282.
- ^ Wang H, Naghavi M, Allen C, Barber RM, Bhutta ZA, Carter A, et al. (GBD 2015 Mortality and Causes of Death Collaborators) (October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1459–1544. doi:10.1016/s0140-6736(16)31012-1. PMC 5388903. PMID 27733281.
- ^ a b c d e f g h i j k Aupérin A (May 2020). "Epidemiology of head and neck cancers: an update". Current Opinion in Oncology. 32 (3): 178–186. doi:10.1097/CCO.0000000000000629. PMID 32209823. S2CID 214644380.
- ^ a b c d e f g "Head and Neck Cancers". NCI. 29 March 2017. Retrieved 7 February 2021.
- ^ a b Vigneswaran N, Williams MD (May 2014). "Epidemiologic trends in head and neck cancer and aids in diagnosis". Oral and Maxillofacial Surgery Clinics of North America. 26 (2): 123–141. doi:10.1016/j.coms.2014.01.001. PMC 4040236. PMID 24794262.
- ^ a b c d e Chow LQ (January 2020). "Head and Neck Cancer". The New England Journal of Medicine. 382 (1): 60–72. doi:10.1056/nejmra1715715. PMID 31893516. S2CID 209482428.
- ^ Siegel RL, Miller KD, Jemal A (January 2020). "Cancer statistics, 2020". CA: A Cancer Journal for Clinicians. 70 (1): 7–30. doi:10.3322/caac.21590. PMID 31912902.
- ^ Fitzmaurice C, Abate D, Abbasi N, Abbastabar H, Abd-Allah F, Abdel-Rahman O, et al. (Global Burden of Disease Cancer Collaboration) (December 2019). "Global, Regional, and National Cancer Incidence, Mortality, Years of Life Lost, Years Lived With Disability, and Disability-Adjusted Life-Years for 29 Cancer Groups, 1990 to 2017: A Systematic Analysis for the Global Burden of Disease Study". JAMA Oncology. 5 (12): 1749–1768. doi:10.1001/jamaoncol.2019.2996. PMC 6777271. PMID 31560378.
- ^ Gillison ML, Castellsagué X, Chaturvedi A, Goodman MT, Snijders P, Tommasino M, et al. (February 2014). "Eurogin Roadmap: comparative epidemiology of HPV infection and associated cancers of the head and neck and cervix". International Journal of Cancer. 134 (3): 497–507. doi:10.1002/ijc.28201. PMID 23568556. S2CID 37877664.
- ^ Gillison ML, Chaturvedi AK, Anderson WF, Fakhry C (October 2015). "Epidemiology of Human Papillomavirus-Positive Head and Neck Squamous Cell Carcinoma". Journal of Clinical Oncology. 33 (29): 3235–3242. doi:10.1200/JCO.2015.61.6995. PMC 4979086. PMID 26351338.
- ^ Giuliano AR, Nyitray AG, Kreimer AR, Pierce Campbell CM, Goodman MT, Sudenga SL, et al. (June 2015). "EUROGIN 2014 roadmap: differences in human papillomavirus infection natural history, transmission and human papillomavirus-related cancer incidence by gender and anatomic site of infection". International Journal of Cancer. 136 (12): 2752–2760. doi:10.1002/ijc.29082. PMC 4297584. PMID 25043222.
- ^ a b "SEER Stat Fact Sheets: Oral Cavity and Pharynx Cancer". SEER. April 2016. Archived from the original on 15 November 2016. Retrieved 29 September 2016.
- ^ Beyzadeoglu M, Ozyigit G, Selek U (2014). Radiation Therapy for Head and Neck Cancers: A Case-Based Review. Springer. p. 18. ISBN 9783319104133. Archived from the original on 2017-09-10.
- ^ a b Mathew A, Tirkey AJ, Li H, Steffen A, Lockwood MB, Patil CL, Doorenbos AZ (2 October 2021). "Symptom Clusters in Head and Neck Cancer: A Systematic Review and Conceptual Model". Seminars in Oncology Nursing. 37 (5): 151215. doi:10.1016/j.soncn.2021.151215. PMC 8492544. PMID 34483015.
- ^ McIlwain WR, Sood AJ, Nguyen SA, Day TA (May 2014). "Initial symptoms in patients with HPV-positive and HPV-negative oropharyngeal cancer". JAMA Otolaryngology–Head & Neck Surgery. 140 (5): 441–447. doi:10.1001/jamaoto.2014.141. PMID 24652023.
- ^ Ensley JF (2003). Head and neck cancer : emerging perspectives. Amsterdam: Academic Press. ISBN 978-0-08-053384-1. OCLC 180905431.
- ^ "Paranasal Sinus and Nasal Cavity Cancer Treatment (Adult) (PDQ®)–Patient Version". National Cancer Institute. 8 November 2019. Retrieved 4 December 2019.
- ^ O'Rorke MA, Ellison MV, Murray LJ, Moran M, James J, Anderson LA (December 2012). "Human papillomavirus related head and neck cancer survival: a systematic review and meta-analysis". Oral Oncology. 48 (12): 1191–1201. doi:10.1016/j.oraloncology.2012.06.019. PMID 22841677. Archived (PDF) from the original on 2017-09-10.
- ^ Ragin CC, Taioli E (October 2007). "Survival of squamous cell carcinoma of the head and neck in relation to human papillomavirus infection: review and meta-analysis". International Journal of Cancer. 121 (8): 1813–1820. doi:10.1002/ijc.22851. PMID 17546592.
- ^ Krishnatreya M, Rahman T, Kataki AC, Das A, Das AK, Lahkar K (2013). "Synchronous primary cancers of the head and neck region and upper aero digestive tract: defining high-risk patients". Indian Journal of Cancer. 50 (4): 322–326. doi:10.4103/0019-509x.123610. PMID 24369209.
- ^ "Throat cancer | Head and neck cancers | Cancer Research UK". www.cancerresearchuk.org. Retrieved 28 November 2019.
- ^ a b c d e f g h i Ridge JA, Glisson BS, Lango MN, Feigenberg S, Horwitz EM (2008). "Head and neck tumors." (PDF). In Pazdur R, Wagman LD, Camphausen KA, Hoskins WJ (eds.). Cancer management: a multidisciplinary approach (11th ed.). pp. 39–86. ISBN 978-1-891483-62-2.
- ^ a b c d e f g Gormley M, Creaney G, Schache A, Ingarfield K, Conway DI (2022-11-11). "Reviewing the epidemiology of head and neck cancer: definitions, trends and risk factors". British Dental Journal. 233 (9): 780–786. doi:10.1038/s41415-022-5166-x. ISSN 0007-0610. PMC 9652141. PMID 36369568.
- ^ Hashibe M, Brennan P, Chuang Sc, Boccia S, Castellsague X, Chen C, Curado MP, Dal Maso L, Daudt AW, Fabianova E, Fernandez L, Wünsch-Filho V, Franceschi S, Hayes RB, Herrero R (2009-02-01). "Interaction between Tobacco and Alcohol Use and the Risk of Head and Neck Cancer: Pooled Analysis in the International Head and Neck Cancer Epidemiology Consortium". Cancer Epidemiology, Biomarkers & Prevention. 18 (2): 541–550. doi:10.1158/1055-9965.EPI-08-0347. ISSN 1055-9965. PMC 3051410. PMID 19190158.
- ^ Tramacere I, Negri E, Bagnardi V, Garavello W, Rota M, Scotti L, Islami F, Corrao G, Boffetta P, La Vecchia C (4 May 2010). "A meta-analysis of alcohol drinking and oral and pharyngeal cancers. Part 1: Overall results and dose-risk relation". Oral Oncology. 46 (7): 497–503. doi:10.1016/j.oraloncology.2010.03.024. PMID 20444641.
- ^ Bagnardi V, Rota M, Botteri E, Tramacere I, Islami F, Fedirko V, Scotti L, Jenab M, Turati F, Pasquali E, Pelucchi C, Galeone C, Bellocco R, Negri E, Corrao G (25 November 2014). "Alcohol consumption and site-specific cancer risk: a comprehensive dose–response meta-analysis". British Journal of Cancer. 112 (3): 580–593. doi:10.1038/bjc.2014.579. ISSN 0007-0920. PMC 4453639. PMID 25422909.
- ^ Leoncini E, Vukovic V, Cadoni G, Giraldi L, Pastorino R, Arzani D, Petrelli L, Wünsch-Filho V, Toporcov TN, Moyses RA, Matsuo K, Bosetti C, La Vecchia C, Serraino D, Simonato L (19 May 2018). "Tumour stage and gender predict recurrence and second primary malignancies in head and neck cancer: a multicentre study within the INHANCE consortium". European Journal of Epidemiology. 33 (12): 1205–1218. doi:10.1007/s10654-018-0409-5. ISSN 0393-2990. PMC 6290648. PMID 29779202.
- ^ Chuang SC, Scelo G, Tonita JM, Tamaro S, Jonasson JG, Kliewer EV, Hemminki K, Weiderpass E, Pukkala E, Tracey E, Friis S, Pompe-Kirn V, Brewster DH, Martos C, Chia KS (2008-11-15). "Risk of second primary cancer among patients with head and neck cancers: A pooled analysis of 13 cancer registries". International Journal of Cancer. 123 (10): 2390–2396. doi:10.1002/ijc.23798. ISSN 0020-7136. PMID 18729183.
- ^ Cadoni G, Giraldi L, Petrelli L, Pandolfini M, Giuliani M, Paludetti G, Pastorino R, Leoncini E, Arzani D, Almadori G, Boccia S (December 2017). "Prognostic factors in head and neck cancer: a 10-year retrospective analysis in a single-institution in Italy" (PDF). Acta Otorhinolaryngologica Italica. 37 (6): 458–466. doi:10.14639/0392-100X-1246. ISSN 0392-100X. PMC 5782422. PMID 28663597.
- ^ Sawabe M, Ito H, Oze I, Hosono S, Kawakita D, Tanaka H, Hasegawa Y, Murakami S, Matsuo K (2017-01-26). "Heterogeneous impact of alcohol consumption according to treatment method on survival in head and neck cancer: A prospective study". Cancer Science. 108 (1): 91–100. doi:10.1111/cas.13115. ISSN 1347-9032. PMC 5276823. PMID 27801961.
- ^ a b Marziliano A, Teckie S, Diefenbach MA (27 November 2019). "Alcohol-related head and neck cancer: Summary of the literature". Head & Neck. 42 (4): 732–738. doi:10.1002/hed.26023. ISSN 1097-0347. PMID 31777131.
- ^ Simcock R, Simo R (2016-04-16). "Follow-up and Survivorship in Head and Neck Cancer". Clinical Oncology. 28 (7): 451–458. doi:10.1016/j.clon.2016.03.004. PMID 27094976.
- ^ Andre K, Schraub S, Mercier M, Bontemps P (September 1995). "Role of alcohol and tobacco in the aetiology of head and neck cancer: a case-control study in the Doubs region of France". European Journal of Cancer, Part B. 31B (5): 301–309. doi:10.1016/0964-1955(95)00041-0. PMID 8704646.
- ^ La Vecchia C, Franceschi S, Bosetti C, Levi F, Talamini R, Negri E (April 1999). "Time since stopping smoking and the risk of oral and pharyngeal cancers". Journal of the National Cancer Institute. 91 (8): 726–728. doi:10.1093/jnci/91.8.726a. hdl:2434/520105. PMID 10218516.
- ^ Fortin A, Wang CS, Vigneault É (2008-11-25). "Influence of Smoking and Alcohol Drinking Behaviors on Treatment Outcomes of Patients With Squamous Cell Carcinomas of the Head and Neck". International Journal of Radiation Oncology*Biology*Physics. 74 (4): 1062–1069. doi:10.1016/j.ijrobp.2008.09.021. PMID 19036528.
- ^ Merlano MC, Denaro N, Galizia D, Abbona A, Paccagnella M, Minei S, Garrone O, Bossi P (20 April 2023). "Why Oncologists Should Feel Directly Involved in Persuading Patients with Head and Neck Cancer to Quit Smoking". Oncology. 101 (4): 252–256. doi:10.1159/000528345. ISSN 0030-2414. PMID 36538910.
- ^ von Kroge PR, Bokemeyer F, Ghandili S, Bokemeyer C, Seidel C (18 September 2020). "The Impact of Smoking Cessation and Continuation on Recurrence and Survival in Patients with Head and Neck Cancer: A Systematic Review of the Literature". Oncology Research and Treatment. 43 (10): 549–558. doi:10.1159/000509427. ISSN 2296-5270. PMID 32950990.
- ^ Descamps G, Karaca Y, Lechien JR, Kindt N, Decaestecker C, Remmelink M, Larsimont D, Andry G, Hassid S, Rodriguez A, Khalife M, Journe F, Saussez S (2016-07-01). "Classical risk factors, but not HPV status, predict survival after chemoradiotherapy in advanced head and neck cancer patients". Journal of Cancer Research and Clinical Oncology. 142 (10): 2185–2196. doi:10.1007/s00432-016-2203-7. ISSN 0171-5216. PMC 5018052. PMID 27370781.
- ^ Desrichard A, Kuo F, Chowell D, Lee KW, Riaz N, Wong RJ, Chan TA, Morris LG (2018-12-01). "Tobacco Smoking-Associated Alterations in the Immune Microenvironment of Squamous Cell Carcinomas". JNCI: Journal of the National Cancer Institute. 110 (12): 1386–1392. doi:10.1093/jnci/djy060. ISSN 0027-8874. PMC 6292793. PMID 29659925.
- ^ Ang KK, Harris J, Wheeler R, Weber R, Rosenthal DI, Nguyen-Tân PF, Westra WH, Chung CH, Jordan RC, Lu C, Kim H, Axelrod R, Silverman CC, Redmond KP, Gillison ML (2010-06-07). "Human Papillomavirus and Survival of Patients with Oropharyngeal Cancer". New England Journal of Medicine. 363 (1): 24–35. doi:10.1056/NEJMoa0912217. ISSN 0028-4793. PMC 2943767. PMID 20530316.
- ^ Cunningham FH, Fiebelkorn S, Johnson M, Meredith C (November 2011). "A novel application of the Margin of Exposure approach: segregation of tobacco smoke toxicants". Food and Chemical Toxicology. 49 (11): 2921–2933. doi:10.1016/j.fct.2011.07.019. PMID 21802474.
- ^ Pu X, Kamendulis LM, Klaunig JE (September 2009). "Acrylonitrile-induced oxidative stress and oxidative DNA damage in male Sprague-Dawley rats". Toxicological Sciences. 111 (1): 64–71. doi:10.1093/toxsci/kfp133. PMC 2726299. PMID 19546159.
- ^ Kalam MA, Haraguchi K, Chandani S, Loechler EL, Moriya M, Greenberg MM, Basu AK (2006). "Genetic effects of oxidative DNA damages: comparative mutagenesis of the imidazole ring-opened formamidopyrimidines (Fapy lesions) and 8-oxo-purines in simian kidney cells". Nucleic Acids Research. 34 (8): 2305–2315. doi:10.1093/nar/gkl099. PMC 1458282. PMID 16679449.
- ^ Jena NR, Mishra PC (October 2013). "Is FapyG mutagenic?: Evidence from the DFT study". ChemPhysChem. 14 (14): 3263–3270. doi:10.1002/cphc.201300535. PMID 23934915.
- ^ Suzuki T, Harashima H, Kamiya H (May 2010). "Effects of base excision repair proteins on mutagenesis by 8-oxo-7,8-dihydroguanine (8-hydroxyguanine) paired with cytosine and adenine". DNA Repair. 9 (5): 542–550. doi:10.1016/j.dnarep.2010.02.004. hdl:2115/43021. PMID 20197241. S2CID 207147128.
- ^ Nemec AA, Wallace SS, Sweasy JB (October 2010). "Variant base excision repair proteins: contributors to genomic instability". Seminars in Cancer Biology. 20 (5): 320–328. doi:10.1016/j.semcancer.2010.10.010. PMC 3254599. PMID 20955798.
- ^ Wyss AB, Hashibe M, Lee YA, Chuang SC, Muscat J, Chen C, et al. (November 2016). "Smokeless Tobacco Use and the Risk of Head and Neck Cancer: Pooled Analysis of US Studies in the INHANCE Consortium". American Journal of Epidemiology. 184 (10): 703–716. doi:10.1093/aje/kww075. PMC 5141945. PMID 27744388.
- ^ a b Hecht SS, Hatsukami DK (3 January 2022). "Smokeless tobacco and cigarette smoking: chemical mechanisms and cancer prevention". Nature Reviews Cancer. 22 (3): 143–155. doi:10.1038/s41568-021-00423-4. ISSN 1474-175X. PMC 9308447. PMID 34980891.
- ^ Wyss A, Hashibe M, Chuang SC, Lee YC, Zhang ZF, Yu GP, Winn DM, Wei Q, Talamini R, Szeszenia-Dabrowska N, Sturgis EM, Smith E, Shangina O, Schwartz SM, Schantz S (2013-09-01). "Cigarette, Cigar, and Pipe Smoking and the Risk of Head and Neck Cancers: Pooled Analysis in the International Head and Neck Cancer Epidemiology Consortium". American Journal of Epidemiology. 178 (5): 679–690. doi:10.1093/aje/kwt029. ISSN 1476-6256. PMC 3755640. PMID 23817919.
- ^ a b Ralho A, Coelho A, Ribeiro M, Paula A, Amaro I, Sousa J, et al. (December 2019). "Effects of Electronic Cigarettes on Oral Cavity: A Systematic Review". The Journal of Evidence-Based Dental Practice. 19 (4): 101318. doi:10.1016/j.jebdp.2019.04.002. PMID 31843181. S2CID 145920823.
- ^ Esteban-Lopez M, Perry MD, Garbinski LD, Manevski M, Andre M, Ceyhan Y, Caobi A, Paul P, Lau LS, Ramelow J, Owens F, Souchak J, Ales E, El-Hage N (23 June 2022). "Health effects and known pathology associated with the use of E-cigarettes". Toxicology Reports. 9: 1357–1368. doi:10.1016/j.toxrep.2022.06.006. PMC 9764206. PMID 36561957.
- ^ Ghasemiesfe M, Barrow B, Leonard S, Keyhani S, Korenstein D (2019-11-27). "Association Between Marijuana Use and Risk of Cancer: A Systematic Review and Meta-analysis". JAMA Network Open. 2 (11): e1916318. doi:10.1001/jamanetworkopen.2019.16318. ISSN 2574-3805. PMC 6902836. PMID 31774524.
- ^ Rodríguez-Molinero J, Migueláñez-Medrán Bd, Puente-Gutiérrez C, Delgado-Somolinos E, Martín Carreras-Presas C, Fernández-Farhall J, López-Sánchez AF (2021-04-15). "Association between Oral Cancer and Diet: An Update". Nutrients. 13 (4): 1299. doi:10.3390/nu13041299. ISSN 2072-6643. PMC 8071138. PMID 33920788.
- ^ Morze J, Danielewicz A, Przybyłowicz K, Zeng H, Hoffmann G, Schwingshackl L (April 2021). "An updated systematic review and meta-analysis on adherence to mediterranean diet and risk of cancer". European Journal of Nutrition. 60 (3): 1561–1586. doi:10.1007/s00394-020-02346-6. ISSN 1436-6207. PMC 7987633. PMID 32770356.
- ^ a b c d e f Barsouk A, Aluru JS, Rawla P, Saginala K, Barsouk A (2023-06-13). "Epidemiology, Risk Factors, and Prevention of Head and Neck Squamous Cell Carcinoma". Medical Sciences. 11 (2): 42. doi:10.3390/medsci11020042. ISSN 2076-3271. PMC 10304137. PMID 37367741.
- ^ Lian M (30 January 2022). "Salted fish and processed foods intake and nasopharyngeal carcinoma risk: a dose–response meta-analysis of observational studies". European Archives of Oto-Rhino-Laryngology. 279 (5): 2501–2509. doi:10.1007/s00405-021-07210-9. ISSN 0937-4477. PMID 35094122.
- ^ Harvie M (2014-05-30). "Nutritional Supplements and Cancer: Potential Benefits and Proven Harms". American Society of Clinical Oncology Educational Book (34): e478–e486. doi:10.14694/EdBook_AM.2014.34.e478. ISSN 1548-8748. PMID 24857143.
- ^ Jeng JH, Chang MC, Hahn LJ (September 2001). "Role of areca nut in betel quid-associated chemical carcinogenesis: current awareness and future perspectives". Oral Oncology. 37 (6): 477–492. doi:10.1016/S1368-8375(01)00003-3. PMID 11435174.
- ^ Lesseur C, Diergaarde B, Olshan AF, Wünsch-Filho V, Ness AR, Liu G, Lacko M, Eluf-Neto J, Franceschi S, Lagiou P, Macfarlane GJ, Richiardi L, Boccia S, Polesel J, Kjaerheim K (17 October 2016). "Genome-wide association analyses identify new susceptibility loci for oral cavity and pharyngeal cancer". Nature Genetics. 48 (12): 1544–1550. doi:10.1038/ng.3685. ISSN 1061-4036. PMC 5131845. PMID 27749845.
- ^ Shete S, Liu H, Wang J, Yu R, Sturgis EM, Li G, Dahlstrom KR, Liu Z, Amos CI, Wei Q (2020-06-15). "A Genome-Wide Association Study Identifies Two Novel Susceptible Regions for Squamous Cell Carcinoma of the Head and Neck". Cancer Research. 80 (12): 2451–2460. doi:10.1158/0008-5472.CAN-19-2360. ISSN 0008-5472. PMC 7299763. PMID 32276964.
- ^ a b El Hussein MT, Dhaliwal S (October 2023). "HPV vaccination for prevention of head and neck cancer among men". The Nurse Practitioner. 48 (10): 25–32. doi:10.1097/01.NPR.0000000000000099. ISSN 0361-1817. PMID 37751612.
- ^ Roman BR, Aragones A (23 September 2021). "Epidemiology and incidence of HPV-related cancers of the head and neck". Journal of Surgical Oncology. 124 (6): 920–922. doi:10.1002/jso.26687. ISSN 0022-4790. PMC 8552291. PMID 34558067.
- ^ Merriel SW, Nadarzynski T, Kesten JM, Flannagan C, Prue G (2018-08-30). "'Jabs for the boys': time to deliver on HPV vaccination recommendations". British Journal of General Practice. 68 (674): 406–407. doi:10.3399/bjgp18X698429. ISSN 0960-1643. PMC 6104855. PMID 30166370.
- ^ "HPV vaccine". NHS. 2024-03-06. Retrieved 2024-05-28.
- ^ Kreimer AR, Clifford GM, Boyle P, Franceschi S (February 2005). "Human papillomavirus types in head and neck squamous cell carcinomas worldwide: a systematic review". Cancer Epidemiology, Biomarkers & Prevention. 14 (2): 467–475. doi:10.1158/1055-9965.EPI-04-0551. PMID 15734974.
- ^ Joseph AW, D'Souza G (August 2012). "Epidemiology of human papillomavirus-related head and neck cancer". Otolaryngologic Clinics of North America. 45 (4): 739–764. doi:10.1016/j.otc.2012.04.003. PMID 22793850.
- ^ Perez-Ordoñez B, Beauchemin M, Jordan RC (May 2006). "Molecular biology of squamous cell carcinoma of the head and neck". Journal of Clinical Pathology. 59 (5): 445–453. doi:10.1136/jcp.2003.007641. PMC 1860277. PMID 16644882.
- ^ Paz IB, Cook N, Odom-Maryon T, Xie Y, Wilczynski SP (February 1997). "Human papillomavirus (HPV) in head and neck cancer. An association of HPV 16 with squamous cell carcinoma of Waldeyer's tonsillar ring". Cancer. 79 (3): 595–604. doi:10.1002/(SICI)1097-0142(19970201)79:3<595::AID-CNCR24>3.0.CO;2-Y. PMID 9028373.
- ^ Hobbs CG, Sterne JA, Bailey M, Heyderman RS, Birchall MA, Thomas SJ (August 2006). "Human papillomavirus and head and neck cancer: a systematic review and meta-analysis" (PDF). Clinical Otolaryngology. 31 (4): 259–266. doi:10.1111/j.1749-4486.2006.01246.x. PMID 16911640. S2CID 2502403. Archived (PDF) from the original on 2017-08-11.
- ^ a b Sabatini ME, Chiocca S (2020-02-04). "Human papillomavirus as a driver of head and neck cancers". British Journal of Cancer. 122 (3): 306–314. doi:10.1038/s41416-019-0602-7. ISSN 0007-0920. PMC 7000688. PMID 31708575.
- ^ Schmitz M, Driesch C, Beer-Grondke K, Jansen L, Runnebaum IB, Dürst M (September 2012). "Loss of gene function as a consequence of human papillomavirus DNA integration". International Journal of Cancer. 131 (5): E593–E602. doi:10.1002/ijc.27433. PMID 22262398. S2CID 21515048.
- ^ Stransky N, Egloff AM, Tward AD, Kostic AD, Cibulskis K, Sivachenko A, Kryukov GV, Lawrence MS, Sougnez C, McKenna A, Shefler E, Ramos AH, Stojanov P, Carter SL, Voet D (2011-08-26). "The Mutational Landscape of Head and Neck Squamous Cell Carcinoma". Science. 333 (6046): 1157–1160. Bibcode:2011Sci...333.1157S. doi:10.1126/science.1208130. ISSN 0036-8075. PMC 3415217. PMID 21798893.
- ^ van Kempen PM, Noorlag R, Braunius WW, Stegeman I, Willems SM, Grolman W (29 Oct 2013). "Differences in methylation profiles between HPV-positive and HPV-negative oropharynx squamous cell carcinoma: A systematic review". Epigenetics. 9 (2): 194–203. doi:10.4161/epi.26881. ISSN 1559-2294. PMC 3962529. PMID 24169583.
- ^ Nakagawa T, Kurokawa T, Mima M, Imamoto S, Mizokami H, Kondo S, Okamoto Y, Misawa K, Hanazawa T, Kaneda A (2021-04-10). "DNA Methylation and HPV-Associated Head and Neck Cancer". Microorganisms. 9 (4): 801. doi:10.3390/microorganisms9040801. ISSN 2076-2607. PMC 8069883. PMID 33920277.
- ^ Hickman E (2002-02-01). "The role of p53 and pRB in apoptosis and cancer". Current Opinion in Genetics & Development. 12 (1): 60–66. doi:10.1016/S0959-437X(01)00265-9. PMID 11790556.
- ^ "Risks and causes | Nasopharyngeal cancer | Cancer Research UK". www.cancerresearchuk.org. Retrieved 4 December 2019.
- ^ Li W, Duan X, Chen X, Zhan M, Peng H, Meng Y, Li X, Li XY, Pang G, Dou X (2023-01-11). "Immunotherapeutic approaches in EBV-associated nasopharyngeal carcinoma". Frontiers in Immunology. 13. doi:10.3389/fimmu.2022.1079515. ISSN 1664-3224. PMC 9875085. PMID 36713430.
- ^ a b Elad S, Zadik Y, Zeevi I, Miyazaki A, de Figueiredo MA, Or R (December 2010). "Oral cancer in patients after hematopoietic stem-cell transplantation: long-term follow-up suggests an increased risk for recurrence". Transplantation. 90 (11): 1243–1244. doi:10.1097/TP.0b013e3181f9caaa. PMID 21119507.
- ^ Khlifi R, Hamza-Chaffai A (2010-10-15). "Head and neck cancer due to heavy metal exposure via tobacco smoking and professional exposure: A review". Toxicology and Applied Pharmacology. 248 (2): 71–88. doi:10.1016/j.taap.2010.08.003. PMID 20708025.
- ^ Bosetti C, Carioli G, Santucci C, Bertuccio P, Gallus S, Garavello W, Negri E, La Vecchia C (2020-08-15). "Global trends in oral and pharyngeal cancer incidence and mortality". International Journal of Cancer. 147 (4): 1040–1049. doi:10.1002/ijc.32871. ISSN 0020-7136. PMID 31953840.
- ^ Miranda-Filho A, Bray F (25 January 2020). "Global patterns and trends in cancers of the lip, tongue and mouth". Oral Oncology. 102: 104551. doi:10.1016/j.oraloncology.2019.104551. PMID 31986342.
- ^ Johnson DE, Burtness B, Leemans CR, Lui VW, Bauman JE, Grandis JR (2020-11-26). "Head and neck squamous cell carcinoma". Nature Reviews Disease Primers. 6 (1). doi:10.1038/s41572-020-00224-3. ISSN 2056-676X.
- ^ Karp EE, Yin LX, Moore EJ, Elias AJ, O’Byrne Thomas J., Glasgow AE, Habermann EB, Price DL, Kasperbauer JL, Van Abel KM (26 January 2021). "Barriers to Obtaining a Timely Diagnosis in Human Papillomavirus–Associated Oropharynx Cancer". Otolaryngology–Head and Neck Surgery. 165 (2): 300–308. doi:10.1177/0194599820982662. ISSN 0194-5998.
{{cite journal}}: Vancouver style error: non-Latin character in name 5 (help) - ^ Schache A, Kerawala C, Ahmed O, Brennan PA, Cook F, Garrett M, Homer J, Hughes C, Mayland C, Mihai R, Newbold K, O’Hara James, Roe J, Sibtain A, Smith M (3 March 2021). "British Association of Head and Neck Oncologists (BAHNO) standards 2020". Journal of Oral Pathology & Medicine. 50 (3): 262–273. doi:10.1111/jop.13161. ISSN 0904-2512.
{{cite journal}}: Vancouver style error: non-Latin character in name 12 (help) - ^ Marcus S, Timen M, Dion GR, Fritz MA, Branski RC, Amin MR (19 February 2018). "Cost Analysis of Channeled, Distal Chip Laryngoscope for In-office Laryngopharyngeal Biopsies". Journal of Voice. 33 (4): 575–579. doi:10.1016/j.jvoice.2018.01.011.
- ^ a b Homer JJ, Winter SC, Abbey EC, Aga H, Agrawal R, ap Dafydd D, Arunjit T, Axon P, Aynsley E, Bagwan IN, Batra A, Begg D, Bernstein JM, Betts G, Bicknell C (14 March 2024). "Head and Neck Cancer: United Kingdom National Multidisciplinary Guidelines, Sixth Edition". The Journal of Laryngology & Otology. 138 (S1): S1–S224. doi:10.1017/S0022215123001615. ISSN 0022-2151.
- ^ Ye W, Arnaud EH, Langerman A, Mannion K, Topf MC (1 May 2021). "Diagnostic approaches to carcinoma of unknown primary of the head and neck". European Journal of Cancer Care. 30 (6). doi:10.1111/ecc.13459. ISSN 0961-5423.
- ^ "Routine HPV Testing in Head and Neck Squamous Cell Carcinoma. EBS 5-9". May 2013. Archived from the original on 30 September 2016. Retrieved 22 May 2017.
- ^ a b Haines III GK (24 May 2013). "Pathology of Head and Neck Cancers I: Epithelial and Related Tumors". In Radosevich JA (ed.). Head & Neck Cancer: Current Perspectives, Advances, and Challenges. Springer Science & Business Media. pp. 257–87. ISBN 978-94-007-5827-8. Archived from the original on 7 January 2016.
- ^ "Cancer of the upper aerodigestive tract: assessment and management in people aged 16 and over - Recommendations". NICE. 2016-02-10. Retrieved 2024-05-28.
- ^ Helliwell T, Woolgar J (November 2013). "Standards and datasets for reporting cancers. Dataset for histopathology reporting of salivary gland neoplasms" (PDF). Royal College of Pathologists. Retrieved 2024-05-28.
- ^ Wang YX, Hu D, Yan X (September 2013). "Diagnostic accuracy of Cyfra 21-1 for head and neck squamous cell carcinoma: a meta-analysis". European Review for Medical and Pharmacological Sciences. 17 (17): 2383–2389. PMID 24065233.
- ^ Macilwraith P, Malsem E, Dushyanthen S (2023-04-24). "The effectiveness of HPV vaccination on the incidence of oropharyngeal cancers in men: a review". Infectious Agents and Cancer. 18 (1). doi:10.1186/s13027-022-00479-3. ISSN 1750-9378. PMC 10127083. PMID 37095546.
{{cite journal}}: CS1 maint: PMC format (link) CS1 maint: unflagged free DOI (link) - ^ Al-Sarraf M (2002). "Treatment of locally advanced head and neck cancer: historical and critical review". Cancer Control. 9 (5): 387–399. doi:10.1177/107327480200900504. PMID 12410178.
- ^ Eyassu E, Young M (2023), "Nuclear Medicine PET/CT Head and Neck Cancer Assessment, Protocols, and Interpretation", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 34424632, retrieved 2023-11-24
- ^ Oliver JR, Persky MJ, Wang B, Duvvuri U, Gross ND, Vaezi AE, Morris LG, Givi B (2022-02-15). "Transoral robotic surgery adoption and safety in treatment of oropharyngeal cancers". Cancer. 128 (4): 685–696. doi:10.1002/cncr.33995. ISSN 0008-543X. PMC 9446338. PMID 34762303.
{{cite journal}}: CS1 maint: PMC format (link) - ^ Lechien JR, Fakhry N, Saussez S, Chiesa-Estomba CM, Chekkoury-Idrissi Y, Cammaroto G, Melkane AE, Barillari MR, Crevier-Buchman L, Ayad T, Remacle M, Hans S (10 June 2020). "Surgical, clinical and functional outcomes of transoral robotic surgery for supraglottic laryngeal cancers: A systematic review". Oral Oncology. 109: 104848. doi:10.1016/j.oraloncology.2020.104848.
- ^ Lai KW, Lai R, Lorincz BB, Wang CC, Chan JY, Yeung DC (2022-04-07). "Oncological and Functional Outcomes of Transoral Robotic Surgery and Endoscopic Laryngopharyngeal Surgery for Hypopharyngeal Cancer: A Systematic Review". Frontiers in Surgery. 8. doi:10.3389/fsurg.2021.810581. ISSN 2296-875X. PMC 9021537. PMID 35464886.
{{cite journal}}: CS1 maint: PMC format (link) CS1 maint: unflagged free DOI (link) - ^ Maxwell JH, Thompson LD, Brandwein-Gensler MS, Weiss BG, Canis M, Purgina B, et al. (December 2015). "Early Oral Tongue Squamous Cell Carcinoma: Sampling of Margins From Tumor Bed and Worse Local Control". JAMA Otolaryngology–Head & Neck Surgery. 141 (12): 1104–1110. doi:10.1001/jamaoto.2015.1351. PMC 5242089. PMID 26225798.
- ^ [1] Archived March 5, 2012, at the Wayback Machine
- ^ Mahmood SS, Nohria A (July 2016). "Cardiovascular Complications of Cranial and Neck Radiation". Current Treatment Options in Cardiovascular Medicine. 18 (7): 45. doi:10.1007/s11936-016-0468-4. PMID 27181400. S2CID 23888595.
- ^ a b Yan J, Yuan L, Wang J, Li S, Yao M, Wang K, Herst PM (September 2020). "Mepitel Film is superior to Biafine cream in managing acute radiation-induced skin reactions in head and neck cancer patients: a randomised intra-patient controlled clinical trial". Journal of Medical Radiation Sciences. 67 (3): 208–216. doi:10.1002/jmrs.397. PMC 7476193. PMID 32475079.
- ^ "FDA Approval for Docetaxel - National Cancer Institute". Cancer.gov. Archived from the original on 2014-09-01. Retrieved 2014-08-07.
- ^ Lambin P, Ramaekers BL, van Mastrigt GA, Van den Ende P, de Jong J, De Ruysscher DK, Pijls-Johannesma M (July 2009). "Erythropoietin as an adjuvant treatment with (chemo) radiation therapy for head and neck cancer". The Cochrane Database of Systematic Reviews (3): CD006158. doi:10.1002/14651858.CD006158.pub2. PMID 19588382.
- ^ "Inoperable cancers killed by new laser surgery" The Times. UK. 3-April-2010 p15
- ^ Blick SK, Scott LJ (2007). "Cetuximab: A Review of its Use in Squamous Cell Carcinoma of the Head and Neck and Metastatic Colorectal Cancer". Drugs. 67 (17): 2585–2607. doi:10.2165/00003495-200767170-00008. ISSN 0012-6667. PMID 18034592. S2CID 195690071.
- ^ Cantwell LA, Fahy E, Walters ER, Patterson JM (26 November 2020). "Nutritional prehabilitation in head and neck cancer: a systematic review". Supportive Care in Cancer. 30 (11): 8831–8843. doi:10.1007/s00520-022-07239-4. ISSN 0941-4355. PMID 35913625. S2CID 251221072.
- ^ Muraro E, Fanetti G, Lupato V, Giacomarra V, Steffan A, Gobitti C, Vaccher E, Franchin G (10 July 2021). "Cetuximab in locally advanced head and neck squamous cell carcinoma: Biological mechanisms involved in efficacy, toxicity and resistance". Critical Reviews in Oncology/Hematology. 164: 103424. doi:10.1016/j.critrevonc.2021.103424. PMID 34245856. S2CID 235791305.
- ^ Pearson S, Jia H, Kandachi K (January 2004). "China approves first gene therapy". Nature Biotechnology. 22 (1): 3–4. doi:10.1038/nbt0104-3. PMC 7097065. PMID 14704685.
- ^ Lechner M, Frampton GM, Fenton T, Feber A, Palmer G, Jay A, et al. (2013). "Targeted next-generation sequencing of head and neck squamous cell carcinoma identifies novel genetic alterations in HPV+ and HPV- tumors". Genome Medicine. 5 (5): 49. doi:10.1186/gm453. PMC 4064312. PMID 23718828.
- ^ Center for Drug Evaluation and Research (2019-02-09). "pembrolizumab (KEYTRUDA)". FDA.
- ^ Center for Drug Evaluation and Research (2018-11-03). "Nivolumab for SCCHN". FDA.
- ^ Center for Drug Evaluation and Research (2019-06-11). "FDA approves pembrolizumab for first-line treatment of head and neck squamous cell carcinoma". FDA.
- ^ a b c d e Semple C, Parahoo K, Norman A, McCaughan E, Humphris G, Mills M (July 2013). "Psychosocial interventions for patients with head and neck cancer". The Cochrane Database of Systematic Reviews (7): CD009441. doi:10.1002/14651858.CD009441.pub2. hdl:10026.1/3146. PMID 23857592. S2CID 42090352.
- ^ a b Gourin CG, Podolsky RH (July 2006). "Racial disparities in patients with head and neck squamous cell carcinoma". The Laryngoscope. 116 (7): 1093–1106. doi:10.1097/01.mlg.0000224939.61503.83. PMID 16826042. S2CID 11140152.
- ^ Iro H, Waldfahrer F (November 1998). "Evaluation of the newly updated TNM classification of head and neck carcinoma with data from 3247 patients". Cancer. 83 (10): 2201–2207. doi:10.1002/(SICI)1097-0142(19981115)83:10<2201::AID-CNCR20>3.0.CO;2-7. PMID 9827726.
- ^ Jones AS, Morar P, Phillips DE, Field JK, Husband D, Helliwell TR (March 1995). "Second primary tumors in patients with head and neck squamous cell carcinoma". Cancer. 75 (6): 1343–1353. doi:10.1002/1097-0142(19950315)75:6<1343::AID-CNCR2820750617>3.0.CO;2-T. PMID 7882285.
- ^ Cooper JS, Pajak TF, Rubin P, Tupchong L, Brady LW, Leibel SA, et al. (September 1989). "Second malignancies in patients who have head and neck cancer: incidence, effect on survival and implications based on the RTOG experience". International Journal of Radiation Oncology, Biology, Physics. 17 (3): 449–456. doi:10.1016/0360-3016(89)90094-1. PMID 2674073.
- ^ Priante AV, Castilho EC, Kowalski LP (April 2011). "Second primary tumors in patients with head and neck cancer". Current Oncology Reports. 13 (2): 132–137. doi:10.1007/s11912-010-0147-7. PMID 21234721. S2CID 207335139.
- ^ a b Nugent B, Lewis S, O'Sullivan JM (January 2013). "Enteral feeding methods for nutritional management in patients with head and neck cancers being treated with radiotherapy and/or chemotherapy". The Cochrane Database of Systematic Reviews. 2013 (1): CD007904. doi:10.1002/14651858.CD007904.pub3. PMC 6769131. PMID 23440820.
- ^ Longacre ML, Ridge JA, Burtness BA, Galloway TJ, Fang CY (January 2012). "Psychological functioning of caregivers for head and neck cancer patients". Oral Oncology. 48 (1): 18–25. doi:10.1016/j.oraloncology.2011.11.012. PMC 3357183. PMID 22154127.
- ^ a b Sherrod AM, Murphy BA, Wells NL, Bond SM, Hertzog M, Gilbert J, et al. (2014-05-20). "Caregiving burden in head and neck cancer". Journal of Clinical Oncology. 32 (15_suppl): e20678. doi:10.1200/jco.2014.32.15_suppl.e20678. ISSN 0732-183X.
- ^ "WHO Disease and injury country estimates". World Health Organization. 2009. Archived from the original on 2009-11-11. Retrieved Nov 11, 2009.
- ^ Jemal A, Siegel R, Ward E, Murray T, Xu J, Smigal C, Thun MJ (2006). "Cancer statistics, 2006". CA: A Cancer Journal for Clinicians. 56 (2): 106–130. doi:10.3322/canjclin.56.2.106. PMID 16514137. S2CID 21618776.
- ^ Titcomb CP (2001). "High incidence of nasopharyngeal carcinoma in Asia". Journal of Insurance Medicine. 33 (3): 235–238. PMID 11558403.
- ^ a b Cancer Facts and Figures, [2] Archived 2007-09-29 at the Wayback Machine, American Cancer Society 2002.
- ^ "Throat Cancer". Patient information web page. NCH Healthcare Systems. 1999. Archived from the original on 2007-07-01. Retrieved 2007-06-17.
- ^ Reducing the Health Consequences of Smoking: 25 Years of Progress. A Report of the Surgeon General, U. S. Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, 1989.
- ^ Syn NL, Teng MW, Mok TS, Soo RA (December 2017). "De-novo and acquired resistance to immune checkpoint targeting". The Lancet. Oncology. 18 (12): e731–e741. doi:10.1016/s1470-2045(17)30607-1. PMID 29208439.
External links[edit]
- Head and Neck Cancer at MedlinePlus (National Library of Medicine)
- Head and Neck Cancer Treatment at RadiologyInfo
- Head and Neck Cancer at Cancer.net (American Society of Clinical Oncology)
- Head and Neck Cancer UK (HANCUK)


