User:Mr. Ibrahem/Creutzfeldt–Jakob disease
| Creutzfeldt–Jakob disease | |
|---|---|
| Other names | Classic Creutzfeldt–Jakob disease[1] |
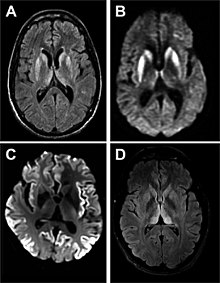 | |
| Magnetic resonance image of sporadic CJD[2] | |
| Pronunciation | |
| Specialty | Neurology |
| Symptoms | Early: memory problems, behavioral changes, poor coordination, visual disturbances[4] Later: dementia, involuntary movements, blindness, weakness, coma[4] |
| Usual onset | Around 60[4] |
| Types | Sporadic, hereditary, acquired[4] |
| Causes | Prion[4] |
| Diagnostic method | After ruling out other possible causes[4] |
| Differential diagnosis | Encephalitis, chronic meningitis, Huntington’s disease, Alzheimer's disease[4] |
| Treatment | Supportive care[4] |
| Prognosis | Universally fatal; 70% die within a year of diagnosis[4] |
| Frequency | 1 per million per year[4] |
Creutzfeldt–Jakob disease (CJD), also known as classic Creutzfeldt–Jakob disease, is a fatal degenerative brain disorder.[4][1] Early symptoms include memory problems, behavioral changes, poor coordination, and visual disturbances.[4] Later symptoms include dementia, involuntary movements, blindness, weakness, and coma.[4] About 70% of people die within a year of diagnosis.[4]
CJD is caused by a protein known as a prion.[5] Infectious prions are misfolded proteins that can cause normally folded proteins to become misfolded.[4] About 85% occur spontaneously, while about 7.5% of cases are inherited from a person's parents in an autosomal dominant manner.[4][6] Exposure to brain or spinal tissue from an infected person may also result in spread.[4] There is no evidence that it can spread between people via normal contact or blood transfusions.[4] Diagnosis involves ruling out other potential causes.[4] An electroencephalogram, spinal tap, or magnetic resonance imaging may support the diagnosis.[4]
There is no specific treatment for CJD.[4] Opioids may be used to help with pain, while clonazepam or sodium valproate may help with involuntary movements.[4] CJD affects about one per million people per year.[4] Onset is typically around 60 years of age.[4] The condition was first described in 1920.[4] It is classified as a type of transmissible spongiform encephalopathy.[7] Inherited CJD accounts for about 10% of prion disease cases.[6] CJD is different from bovine spongiform encephalopathy (mad cow disease) and variant Creutzfeldt–Jakob disease (vCJD).[8]
References[edit]
- ^ a b "Creutzfeldt-Jakob Disease, Classic (CJD)". CDC. 2 October 2018. Archived from the original on 18 July 2017. Retrieved 21 November 2018.
- ^ Mead S, Rudge P (April 2017). "CJD mimics and chameleons". Practical Neurology. 17 (2): 113–121. doi:10.1136/practneurol-2016-001571. PMC 5520355. PMID 28153848.
- ^ Wells, John C. (2008), Longman Pronunciation Dictionary (3rd ed.), Longman, ISBN 9781405881180
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y "Creutzfeldt–Jakob Disease Fact Sheet | National Institute of Neurological Disorders and Stroke". NINDS. March 2003. Archived from the original on 4 July 2017. Retrieved 16 July 2017.
- ^ "Creutzfeldt-Jakob Disease, Classic (CJD) | Prion Diseases | CDC". www.cdc.gov. 1 February 2019. Archived from the original on 18 July 2017. Retrieved 17 June 2019.
Classic CJD is a human prion disease
- ^ a b Manix, Marc; Kalakoti, Piyush; Henry, Miriam; Thakur, Jai; Menger, Richard; Guthikonda, Bharat; Nanda, Anil (2015-11-01). "Creutzfeldt-Jakob disease: updated diagnostic criteria, treatment algorithm, and the utility of brain biopsy". Neurosurgical Focus. 39 (5): E2. doi:10.3171/2015.8.FOCUS15328. ISSN 1092-0684. PMID 26646926.
- ^ "About CJD | Creutzfeldt–Jakob Disease, Classic (CJD) | Prion Disease". CDC. 11 February 2015. Archived from the original on 8 August 2017. Retrieved 16 July 2017.
- ^ "Creutzfeldt–Jakob Disease, Classic (CJD) | Prion Diseases". CDC. 6 February 2015. Archived from the original on 18 July 2017. Retrieved 16 July 2017.
