User:Mr. Ibrahem/Obstructive sleep apnea
| Obstructive sleep apnea | |
|---|---|
| Other names | Obstructive sleep apnoea; obstructive sleep apnea syndrome (OSAS); obstructive sleep apnea–hypopnea syndrome (OSAHS)[1] |
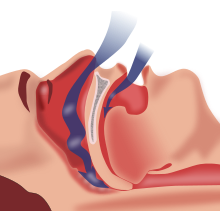 | |
| Obstructive sleep apnea: As soft tissue falls to the back of the throat, it impedes the passage of air (blue arrows) through the trachea. | |
| Specialty | Sleep medicine |
| Symptoms | Daytime sleepiness, snoring, periods of interrupted breathing, nighttime urination, morning headaches[2][1] |
| Usual onset | Age over 40[1] |
| Types | Mild (AHI 5 to 15), moderate (AHI 16 to 30), severe (AHI > 30) |
| Risk factors | Overweight, sedatives, large tonsils, smoking, nasal congestion, family history[1] |
| Diagnostic method | Polysomnography, home sleep testing[2] |
| Differential diagnosis | COPD, central sleep apnea, narcolepsy, periodic limb movement disorder[3] |
| Treatment | CPAP, weight loss, avoiding sedatives, mandibular advancement device, surgery[2][1] |
| Prognosis | Decreased life expectancy[3] |
| Frequency | Common[2] |
Obstructive sleep apnea (OSA) is recurrent episodes of narrowing or blockage of the throat during sleep.[1] Symptoms may include daytime sleepiness, snoring, short periods of interrupted breathing, nighttime urination, and headaches in the morning.[1][2] Complications may include heart disease, stroke, diabetes, and motor vehicle collisions.[2]
Risk factors include being overweight, taking sedatives, large tonsils, smoking, nasal congestion, and family history.[1] The underlying mechanism involves a fall in oxygen levels which results in partial or complete waking.[1] Symptoms are often first noticed by family or friends rather than the person themselves.[1] Diagnosis is based on an apnea–hypopnea index (AHI) of at least 5 per hour as measured by polysomnography or home sleep testing.[2][4] It is a type of sleep apnea, along with the less common central sleep apnea.[1]
Continuous positive airway pressure (CPAP) is the recommended treatment in those with moderate to severe disease.[2] While it improves daytime sleepiness and quality of life, affects on risk of heart disease or death is unclear.[5][6][7] Weight loss and avoiding sedatives are also recommended.[2] Other options may be used in those who cannot tolerate CPAP, including a mandibular advancement device or surgery.[1][2] Life expectancy is lower among those effected, particularly if they do not tolerate CPAP.[3]
Obstructive sleep apnea is common; affecting about a billion people worldwide.[3] In the United States it occurs in about 34% of middle aged males and 17% of females.[2][8] It occurs more commonly in those over the age of 40.[1] Some countries limit the ability to drive among those affected until the condition is well controlled.[1] Interest in the condition grew in part from Charles Dickens' novel The Posthumous Papers of the Pickwick Club in 1837; with the link with airway obstruction recognized in the 1960s.[9][10]
References[edit]
- ^ a b c d e f g h i j k l m n "Obstructive sleep apnoea (OSA)". www.nhsinform.scot. Archived from the original on 10 May 2023. Retrieved 27 June 2023.
- ^ a b c d e f g h i j k Veasey, Sigrid C.; Rosen, Ilene M. (11 April 2019). "Obstructive Sleep Apnea in Adults". New England Journal of Medicine. 380 (15): 1442–1449. doi:10.1056/NEJMcp1816152.
- ^ a b c d Slowik, JM; Sankari, A; Collen, JF (January 2023). "Obstructive Sleep Apnea". StatPearls. PMID 29083619.
- ^ "Obstructive sleep apnoea (OSA)". www.nhsinform.scot. Archived from the original on 10 May 2023. Retrieved 27 June 2023.
- ^ Ton, Joey (20 August 2018). "#218 CPAP—Breath of life, or just hot air?". CFPCLearn. Archived from the original on 25 March 2023. Retrieved 16 June 2023.
- ^ Laratta, Cheryl R.; Ayas, Najib T.; Povitz, Marcus; Pendharkar, Sachin R. (4 December 2017). "Diagnosis and treatment of obstructive sleep apnea in adults". Canadian Medical Association Journal. 189 (48): E1481–E1488. doi:10.1503/cmaj.170296.
- ^ Gottlieb, Daniel J.; Punjabi, Naresh M. (14 April 2020). "Diagnosis and Management of Obstructive Sleep Apnea: A Review". JAMA. 323 (14): 1389. doi:10.1001/jama.2020.3514.
- ^ Yeghiazarians, Yerem; Jneid, Hani; Tietjens, Jeremy R.; Redline, Susan; Brown, Devin L.; El-Sherif, Nabil; Mehra, Reena; Bozkurt, Biykem; Ndumele, Chiadi Ericson; Somers, Virend K. (20 July 2021). "Obstructive Sleep Apnea and Cardiovascular Disease: A Scientific Statement From the American Heart Association". Circulation. 144 (3). doi:10.1161/CIR.0000000000000988.
- ^ Guilleminault, Christian (November 1985). "Obstructive Sleep Apnea: The Clinical Syndrome and Historical Perspective". Medical Clinics of North America. 69 (6): 1187–1203. doi:10.1016/s0025-7125(16)30982-8.
- ^ Kryger, Meir H.; Roth, Thomas; Dement, William C. (29 December 2015). Principles and Practice of Sleep Medicine E-Book. Elsevier Health Sciences. p. 627. ISBN 978-0-323-37752-2. Archived from the original on 1 July 2023. Retrieved 1 July 2023.
