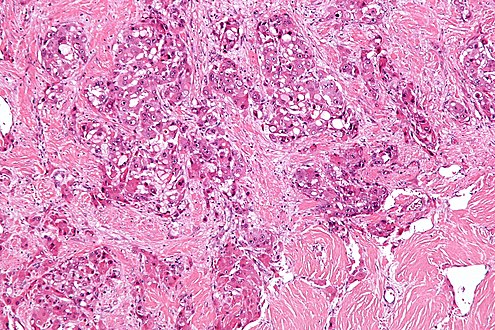
Fibrolamellar hepatocellular carcinoma
| Fibrolamellar hepatocellular carcinoma | |
|---|---|
| Other names | FHCC |
 | |
| Micrograph of fibrolamellar hepatocarcinoma showing the characteristic laminated fibrosis between the tumor cells with a low NC ratio. H&E stain. | |
| Specialty | Oncology |
Fibrolamellar carcinoma (FLC) is a rare form of carcinoma that typically affects young adults and is characterized, under the microscope, by laminated fibrous layers interspersed between the tumor cells.[1] It has been estimated that 200 new cases are diagnosed worldwide each year.[2] However, in light of recent advances in our molecular understanding, this has recently been revised to suggest it may be at least ten times more common.[3] FLC, also known as fibrolamellar hepatocellular carcinoma, is different from the more common hepatocellular carcinoma (HCC) in that it afflicts young people with normal liver function and no known risk factors.[1][2][4][5]
Cause[edit]
A 2014 study showed the presence of the DNAJB1-PRKACA chimeric transcript (resulting from a 400kb somatic deletion on chromosome 19) in 100% of the FLCs examined (15/15).[6][7] This gene fusion has been confirmed in many other studies.[8][9][10] That this genomic deletion is sufficient to produce FLC was shown by creating this deletion, and formation of the DNAJB1::PRKACA chimeric gene, using CRISPR/Cas9 in the livers of mice.[11][12] That the actual formation of the DNAJB1::PRKACA was responsible, and not the deletion, was shown by expression of the DNAJB1::PRKACA from a transposon.[11] To determine if the DNAJB1::PRKACA was only involved in triggering the tumor, or if it continued to drive the tumor, a small hairpin RNA was used to eliminate the DNAJB1::PRKACA. The tumors died, which demonstrated not only that DNAJB1::PRKACA is continuing to drive FLC, but that the tumor has become oncogenically addicted.[13]
Pathology[edit]
The histopathology of FLC is characterized by laminated fibrous layers, interspersed between the tumor cells. Cytologically, the tumor cells have a low nuclear to cytoplasmic ratio with abundant eosinophilic cytoplasm.[1] Tumors are non-encapsulated, but well circumscribed, when compared to conventional HCC (which typically has an invasive border).[citation needed]
Diagnosis[edit]
Due to lack of symptoms, until the tumor is sizable, this form of cancer is often advanced when diagnosed. Symptoms include vague abdominal pain, nausea, abdominal fullness, malaise and weight loss. They may also include a palpable liver mass.[14] Other presentations include jaundice, ascites, fulminant liver failure, encephalopathy, gynecomastia (males only), thrombophlebitis of the lower limbs, recurrent deep vein thrombosis, anemia and hypoglycemia.[citation needed]
The usual markers for liver disease – aspartate aminotransferase, alanine aminotransferase and alkaline phosphatase – are often normal or only slightly elevated. FLC often does not produce alpha fetoprotein (AFP), a widely used marker for conventional hepatocellular carcinoma. In a subset of FLC patients elevated plasma neurotensin levels may be present.[15] Likewise, in a subset of FLC patients, elevated serum vitamin B12 binding globulin levels may be present.[16]
Diagnosis is normally made by imaging (ultrasound, CT or MRI) and biopsy.[17] However, even with a biopsy, there is often disagreement over the diagnosis.[17] Since the characterization of the DNAJB1::PRKACA fusion, the most reliable diagnosis is through molecular characterization such as PCR to detect the fusion,[7][18] or genomic sequencing, or using a fluorescent in-situ hybridization.[8]
Treatment[edit]
FLC can often be surgically removed. Liver resection is the optimal treatment and may need to be performed more than once, since this disease has a very high recurrence rate.[19] Due to such recurrence, periodic follow-up medical imaging (CT or MRI) is necessary.[19]
When the tumor cannot be removed surgically or when there is distant spread, many different systemic therapies are currently being used to treat the disease. However, no standard of care currently exists for FLC. Consequently, there remains a pressing need to identify proven, effective systemic therapies for the cancer.[2][20][5] Radiotherapy has been used but data is limited concerning its use.
The Fibrolamellar Registry,[21] a patient and family run medical registry has collected data from over 250 patients. This work has been used in multiple publications which include extended information on patient outcomes, efficacy of immune checkpoint inhibitors, efficacy of specific drugs and understanding the basis of high ammonia in FLC.[19][22][23][18]
The survival rate for FLC largely depends on whether (and to what degree) the cancer has metastasized, i.e. spread to the lymph nodes or other organs. Distant spread (metastases), significantly reduces the median survival rate.[19] Five-year survival rates vary between 40 and 90%.[19]
Epidemiology[edit]
FLC accounts for 1–10% of primary liver cancers.[24] It typically has a young age at presentation when compared to conventional HCC. Previously it was estimated to be 20–40 years, mean ages 27 years,[25] but when analysis is restricted to those patients who are confirmed with a molecular test to have FLC, the age range is 10-40 and mean age of 21 years.[19] Unlike the more common HCC, patients most often do not have coexistent liver disease such as cirrhosis.
History[edit]
This disease was first described by Hugh Edmondson in a 14-year-old female with no underlying liver disease.[26] The name fibrolamellar hepatocellular carcinoma was coined by Craig et al. in 1980.[27] It was not recognized as a distinct form of cancer by the WHO until 2010.[28]
Starting in 2010, some patients and their family members started to examine the molecular basis of FLC.[20] They gathered samples through social media,[29][30] sequenced the genome, and analyzed the immunological response. Since there are few patients at any one institution, they formed their own medical registry, which allowed them to follow patients as they changed institutions (Fibroregistry.org).[21] This work led to the identification of the chimeric fusion driver and the first characterization of the transcriptome and proteome. The work was heralded by Francis Collins when he presented to the Senate Appropriations committee[31] and was used by President Obama at the launch of The Precision Medicine Initiative at the White House.[32]
Additional images[edit]
-
Intermed. mag.
-
High mag.
References[edit]
- ^ a b c Torbenson, Michael (2012). "Fibrolamellar Carcinoma: 2012 Update". Scientifica. 2012: 743790. doi:10.6064/2012/743790. PMC 3820672. PMID 24278737.
- ^ a b c O'Neill, Allison F.; Church, Alanna J.; Perez-Atayde, Antonio R.; Shaikh, Raja; Marcus, Karen J.; Vakili, Khashayar (August 2021). "Fibrolamellar carcinoma: An entity all its own". Current Problems in Cancer. 45 (4): 100770. doi:10.1016/j.currproblcancer.2021.100770. PMID 34272087. S2CID 236001418.
- ^ Zack, Travis; Losert, Kurt P.; Maisel, Samantha M.; Wild, Jennifer; Yaqubie, Amin; Herman, Michael; Knox, Jennifer J.; Mayer, Robert J.; Venook, Alan P.; Butte, Atul; O'Neill, Allison F.; Abou-Alfa, Ghassan K.; Gordan, John D. (23 March 2023). "Defining incidence and complications of fibrolamellar liver cancer through tiered computational analysis of clinical data". npj Precision Oncology. 7 (1): 29. doi:10.1038/s41698-023-00371-2. PMC 10034241. PMID 36959495.
- ^ Lalazar, Gadi; Simon, Sanford (February 2018). "Fibrolamellar Carcinoma: Recent Advances and Unresolved Questions on the Molecular Mechanisms". Seminars in Liver Disease. 38 (1): 051–059. doi:10.1055/s-0037-1621710. PMC 6020845. PMID 29471565.
- ^ a b "What is Fibrolamellar Carcinoma?". Fibrolamellar Cancer Foundation. 20 February 2021. Retrieved 2023-01-10.
- ^ "Teen Makes Genetic Discovery of Her Own Rare Cancer". NBC News. 16 April 2014.
- ^ a b Honeyman JN, Simon EP, Robine N, Chiaroni-Clarke R, Darcy DG, Lim II, Gleason CE, Murphy JM, Rosenberg BR, Teegan L, Takacs CN, Botero S, Belote R, Germer S, Emde AK, Vacic V, Bhanot U, LaQuaglia MP, Simon SM (28 February 2014). "Detection of a Recurrent DNAJB1-PRKACA Chimeric Transcript in Fibrolamellar Hepatocellular Carcinoma". Science. 343 (6174): 1010–4. Bibcode:2014Sci...343.1010H. doi:10.1126/science.1249484. PMC 4286414. PMID 24578576.
- ^ a b Graham, Rondell P; Jin, Long; Knutson, Darlene L; Kloft-Nelson, Sara M; Greipp, Patricia T; Waldburger, Nina; Roessler, Stephanie; Longerich, Thomas; Roberts, Lewis R; Oliveira, Andre M; Halling, Kevin C; Schirmacher, Peter; Torbenson, Michael S (June 2015). "DNAJB1-PRKACA is specific for fibrolamellar carcinoma". Modern Pathology. 28 (6): 822–829. doi:10.1038/modpathol.2015.4. PMID 25698061.
- ^ Xu, Lei; Hazard, Florette K.; Zmoos, Anne-Flore; Jahchan, Nadine; Chaib, Hassan; Garfin, Phillip M.; Rangaswami, Arun; Snyder, Michael P.; Sage, Julien (1 January 2015). "Genomic analysis of fibrolamellar hepatocellular carcinoma". Human Molecular Genetics. 24 (1): 50–63. doi:10.1093/hmg/ddu418. PMC 4262492. PMID 25122662.
- ^ Dinh TA, Vitucci EC, Wauthier E, Graham RP, Pitman WA, Oikawa T, Chen M, Silva G, Greene KG, Torbenson MS, Reid LM, Sethupathy P (2017) Comprehensive analysis of The Cancer Genome Atlas reveals a unique gene and non-coding RNA signature of fibrolamellar carcinoma. Sci Rep 7:44653. doi: 10.1038/srep44653
- ^ a b Kastenhuber, Edward R.; Lalazar, Gadi; Houlihan, Shauna L.; Tschaharganeh, Darjus F.; Baslan, Timour; Chen, Chi-Chao; Requena, David; Tian, Sha; Bosbach, Benedikt; Wilkinson, John E.; Simon, Sanford M.; Lowe, Scott W. (12 December 2017). "DNAJB1–PRKACA fusion kinase interacts with β-catenin and the liver regenerative response to drive fibrolamellar hepatocellular carcinoma". Proceedings of the National Academy of Sciences. 114 (50): 13076–13084. Bibcode:2017PNAS..11413076K. doi:10.1073/pnas.1716483114. PMC 5740683. PMID 29162699.
- ^ Engelholm, Lars H.; Riaz, Anjum; Serra, Denise; Dagnæs-Hansen, Frederik; Johansen, Jens V.; Santoni-Rugiu, Eric; Hansen, Steen H.; Niola, Francesco; Frödin, Morten (December 2017). "CRISPR/Cas9 Engineering of Adult Mouse Liver Demonstrates That the Dnajb1–Prkaca Gene Fusion Is Sufficient to Induce Tumors Resembling Fibrolamellar Hepatocellular Carcinoma". Gastroenterology. 153 (6): 1662–1673.e10. doi:10.1053/j.gastro.2017.09.008. PMC 5801691. PMID 28923495.
- ^ Neumayer, Christoph; Ng, Denise; Jiang, Caroline S.; Qureshi, Adam; Lalazar, Gadi; Vaughan, Roger; Simon, Sanford M. (4 January 2023). "Oncogenic Addiction of Fibrolamellar Hepatocellular Carcinoma to the Fusion Kinase DNAJB1-PRKACA". Clinical Cancer Research. 29 (1): 271–278. doi:10.1158/1078-0432.CCR-22-1851. PMC 9811160. PMID 36302174.
- ^ Yen, JB.; Chang, KW. (2009). "Fibrolamellar hepatocellular carcinoma- report of a case". Chang Gung Med J. 32 (3): 336–9. PMID 19527614.
- ^ Collier, N.A.; Bloom, S.R.; Hodgson, H.J.F.; Weinbren, K.; Lee, Y.C.; Blumgart, L.H. (March 1984). "Neurotensin Secretion by Fibrolamellar Carcinoma of the Liver". The Lancet. 323 (8376): 538–540. doi:10.1016/s0140-6736(84)90934-6. PMID 6199633. S2CID 28566123.
- ^ Paradinas, F J; Melia, W M; Wilkinson, M L; Portmann, B; Johnson, P J; Murray-Lyon, I M; Williams, R (25 September 1982). "High serum vitamin B12 binding capacity as a marker of the fibrolamellar variant of hepatocellular carcinoma". BMJ. 285 (6345): 840–842. doi:10.1136/bmj.285.6345.840. PMC 1499744. PMID 6288165.
- ^ a b Malouf, G; Falissard, B; Azoulay, D; Callea, F; Ferrell, L D; Goodman, Z D; Hayashi, Y; Hsu, H-C; Hubscher, S G; Kojiro, M; Ng, I O; Paterson, A C; Reynes, M; Zafrani, E-S; Emile, J-F (1 June 2009). "Is histological diagnosis of primary liver carcinomas with fibrous stroma reproducible among experts?". Journal of Clinical Pathology. 62 (6): 519–524. doi:10.1136/jcp.2008.062620. PMID 19155239. S2CID 206987786.
- ^ a b Levin, Solomon N.; Tomasini, Michael D.; Knox, James; Shirani, Mahsa; Shebl, Bassem; Requena, David; Clark, Jackson; Heissel, Søren; Alwaseem, Hanan; Surjan, Rodrigo; Lahasky, Ron; Molina, Henrik; Torbenson, Michael S.; Lyons, Barbara; Migler, Rachael D.; Coffino, Philip; Simon, Sanford M. (23 June 2023). "Disruption of proteome by an oncogenic fusion kinase alters metabolism in fibrolamellar hepatocellular carcinoma". Science Advances. 9 (25): eadg7038. Bibcode:2023SciA....9G7038L. doi:10.1126/sciadv.adg7038. PMC 10284549. PMID 37343102.
- ^ a b c d e f Berkovitz, Amichai; Migler, Rachael D.; Qureshi, Adam; Rosemore, Carly; Torbenson, Michael S.; Vaughan, Roger; Marcotte, Erin; Simon, Sanford M. (December 2022). "Clinical and demographic predictors of survival for fibrolamellar carcinoma patients—A patient community, registry‐based study". Hepatology Communications. 6 (12): 3539–3549. doi:10.1002/hep4.2105. PMC 9701473. PMID 36245434.
- ^ a b Simon, Sanford M. (May 2023). "Fighting rare cancers: lessons from fibrolamellar hepatocellular carcinoma". Nature Reviews Cancer. 23 (5): 335–346. doi:10.1038/s41568-023-00554-w. PMC 10022574. PMID 36932129.
- ^ a b "Home". The Fibrolamellar Registry.
- ^ Chen, Krista Y.; Popovic, Aleksandra; Hsiehchen, David; Baretti, Marina; Griffith, Paige; Bista, Ranjan; Baghdadi, Azarakhsh; Kamel, Ihab R.; Simon, Sanford M.; Migler, Rachael D.; Yarchoan, Mark (30 October 2022). "Clinical Outcomes in Fibrolamellar Hepatocellular Carcinoma Treated with Immune Checkpoint Inhibitors". Cancers. 14 (21): 5347. doi:10.3390/cancers14215347. PMC 9655068. PMID 36358766.
- ^ Shebl, Bassem; Ng, Denise; Lalazar, Gadi; Rosemore, Carly; Finkelstein, Tova M.; Migler, Rachael D.; Zheng, Guangrong; Zhang, Peiyi; Jiang, Caroline S.; Qureshi, Adam; Vaughan, Roger; Yarchoan, Mark; de Jong, Ype P.; Rice, Charles M.; Coffino, Philip; Ortiz, Michael V.; Zhou, Daohong; Simon, Sanford M. (8 September 2022). "Targeting BCL-XL in fibrolamellar hepatocellular carcinoma". JCI Insight. 7 (17): e161820. doi:10.1172/jci.insight.161820. PMC 9536265. PMID 36073545.
- ^ Lafaro KJ, Pawlik TM (2015) Fibrolamellar hepatocellular carcinoma: current clinical perspectives. J Hepatocell Carcinoma 2:151–157 doi: 10.2147/JHC.S75153
- ^ Stipa F, Yoon SS, Liau KH, et al. (March 2006). "Outcome of patients with fibrolamellar hepatocellular carcinoma". Cancer. 106 (6): 1331–8. doi:10.1002/cncr.21703. PMID 16475212.
- ^ Edmondson HA (1956) Differential diagnosis of tumors and tumor-like lesions of liver in infancy and childhood. AMA J Dis Child 91(2):168–186
- ^ Craig JR, Peters RL, Edmondson HA, Omata M. Fibrolamellar carcinoma of the liver: a tumor of adolescents and young adults with distinctive clinico-pathologic features. Cancer 46(2):372–379
- ^ Bosman FT (2010) World Health Organization. WHO Classification of Tumours of the Digestive System. 4th ed. Lyon: International Agency for Research on Cancer
- ^ "Teen Makes Genetic Discovery of Her Own Rare Cancer". NBC News. 16 April 2014.
- ^ "Fibrolamellar Liver Cancer Research". YouTube.
- ^ "Senate Appropriation Hearings on the NIH: Francis Collins". YouTube.
- ^ "Launching of the Precision Medicine Initiative Jan 30, 2015". YouTube.