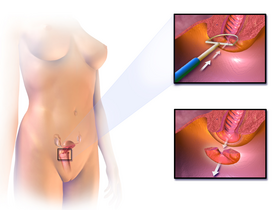
Loop electrical excision procedure
| Loop electrical excision procedure | |
|---|---|
 | |
| Other names | Large loop excision of the transformation zone |
| Specialty | Gynaecology |
The loop electrosurgical excision procedure (LEEP) is one of the most commonly used approaches to treat high grade cervical dysplasia (CIN II/III, HGSIL) and early stage cervical cancer discovered on colposcopic examination. In the UK, it is known as large loop excision of the transformation zone (LLETZ). It is considered a type of conization.[1] It has been in use since the 1970s, after its invention by Dr. Sheldon Weinstein. [2]
LEEP has many advantages including low cost and a high success rate.[3] The procedure can be done in an office setting and usually only requires a local anesthetic, though sometimes IV sedation or a general anesthetic is used.[4] Disadvantages include reports of decreased sexual satisfaction [5] and potential for preterm labor, though a meta-analysis published in 2014 suggested that in patients with existing CIN lesions as opposed to controls, the risk is not more than their baseline risk.[6] Approximately 500,000 LEEP procedures are performed in the U.S. annually. [7]
Process[edit]
When performing a LEEP, the physician uses a wire loop through which an electric current is passed at variable power settings. Various shapes and sizes of loop can be used depending on the size and orientation of the lesion. The cervical transformation zone and lesion are excised to an adequate depth, which in most cases is at least 8 mm, and extending 4 to 5 mm beyond the lesion. A second pass with a more narrow loop can also be done to obtain an endocervical specimen for further histologic evaluation.[8]
The LEEP technique results in some thermal artifact in all specimens obtained due to the use of electricity which simultaneously cuts and cauterizes the lesion, but this does not generally interfere with pathological interpretation provided depth is not exceeded.[9] The thermal artifact can be a function of depth and time.
Complications[edit]
Complications are less frequent in comparison to a cold-knife conization but can include infection and hemorrhage.[10]
LEEP effectively reduces the risk of cancer developing or spreading but it causes an increased risk of premature birth in future pregnancies.[11][12][13] Following LEEP there is a 10% chance of cancer recurrence and 11% chance of preterm birth.[11][12] This perspective carries significant implications when it comes to pregnancy timing and decision making in women of child bearing age who have cervical dysplasia and would like to decide whether they should have the lesions removed before or after pregnancy. As pregnancy is generally understood to be an immune suppressed state, the viral mediated character of cervical lesions might also inform revisions to treatment recommendations in such instances.[6]
Some women report a small decrease in sexual arousal and satisfaction following LEEP but there is a lack of high quality research showing how LEEP affects sexual function.[14]
See also[edit]
References[edit]
- ^ "Loop Electrosurgical Excision Procedure (LEEP): Pre-Procedure, Technique, Post-Procedure". 2022-12-22.
{{cite journal}}: Cite journal requires|journal=(help) - ^ "Loop Electrosurgical Excision Procedure (LEEP) | Embryo Project Encyclopedia". embryo.asu.edu. Retrieved 2023-11-16.
- ^ "Loop electrosurgical excision procedure (LEEP) for abnormal cervical cell changes". Retrieved 2016-11-27.
- ^ Mayeaux, E.J. Jr. "Advantages of LEEP". Archived from the original on 2006-09-04. Retrieved 2007-12-28.
- ^ Inna, Namfon; Phianmongkhol, Yupin; Charoenkwan, Kittipat (1 March 2010). "Sexual function after loop electrosurgical excision procedure for cervical dysplasia". J Sex Med. 7 (3): 1291–1297. doi:10.1111/j.1743-6109.2009.01633.x. PMID 19968775.
- ^ a b Conner SN, Frey HA, Cahill AG, Macones GA, Colditz GA, Tuuli MG (April 2014). "Loop electrosurgical excision procedure and risk of preterm birth: a systematic review and meta-analysis". Obstetrics and Gynecology. 123 (4): 752–61. doi:10.1097/AOG.0000000000000174. PMC 4113318. PMID 24785601.
- ^ Sklavos, Martha M.; Spracklen, Cassandra N.; Saftlas, Audrey F.; Pinto, Ligia A. (2014). "Does Loop Electrosurgical Excision Procedure of the Uterine Cervix Affect Anti-Müllerian Hormone Levels?". BioMed Research International. 2014: 875438. doi:10.1155/2014/875438. ISSN 2314-6133. PMC 3953513. PMID 24707500.
- ^ Cornforth, Tracee. "LEEP Procedure — What is LEEP? — Loop Electrosurgical Excision Procedure". About.com. Archived from the original on 2007-05-02. Retrieved 2007-12-28.
- ^ Khunamornpong, S.; Raungrongmorakot, K.; Siriaunkgul, S. (April 2001). "Loop electrosurgical excision procedure (LEEP) at Maharaj Nakorn Chiang Mai Hospital: problems in pathologic evaluation". Journal of the Medical Association of Thailand = Chotmaihet Thangphaet. 84 (4): 507–514. ISSN 0125-2208. PMID 11460961.
- ^ Jiang, Yanming; Chen, Changxian; Li, Li (2017-01-26). "Comparison of Cold-Knife Conization versus Loop Electrosurgical Excision for Cervical Adenocarcinoma In Situ (ACIS): A Systematic Review and Meta-Analysis". PLOS ONE. 12 (1): e0170587. Bibcode:2017PLoSO..1270587J. doi:10.1371/journal.pone.0170587. ISSN 1932-6203. PMC 5268480. PMID 28125627.
- ^ a b Athanasiou, Antonios; Veroniki, Areti Angeliki; Efthimiou, Orestis; Kalliala, Ilkka; Naci, Huseyin; Bowden, Sarah; Paraskevaidi, Maria; Arbyn, Marc; Lyons, Deirdre; Martin-Hirsch, Pierre; Bennett, Phillip; Paraskevaidis, Evangelos; Salanti, Georgia; Kyrgiou, Maria (2022-07-25). "Comparative effectiveness and risk of preterm birth of local treatments for cervical intraepithelial neoplasia and stage IA1 cervical cancer: a systematic review and network meta-analysis". The Lancet Oncology. 23 (8): 1097–1108. doi:10.1016/S1470-2045(22)00334-5. PMC 9630146. PMID 35835138.
- ^ a b "Prevention of cervical cancer: what are the risks and benefits of different treatments?". NIHR Evidence (Plain English summary). National Institute for Health and Care Research. 2023-11-10. doi:10.3310/nihrevidence_60599. S2CID 265201829.
- ^ Kyrgiou M, Athanasiou A, Kalliala IE, Paraskevaidi M, Mitra A, Martin-Hirsch PP, Arbyn M, Bennett P, Paraskevaidis E (November 2017). "Obstetric outcomes after conservative treatment for cervical intraepithelial lesions and early invasive disease". The Cochrane Database of Systematic Reviews. 11 (11): CD012847. doi:10.1002/14651858.CD012847. PMC 6486192. PMID 29095502.
- ^ Litman, Ethan A.; Cigna, Sarah T. (2022-04-07). "Female Sexual Dysfunction in Women After Treatment of Cervical Dysplasia". Sexual Medicine Reviews. 10 (3): 360–366. doi:10.1016/j.sxmr.2022.02.003. PMID 35400602. S2CID 248029304.
