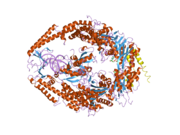
MSH6
MSH6 or mutS homolog 6 is a gene that codes for DNA mismatch repair protein Msh6 in the budding yeast Saccharomyces cerevisiae. It is the homologue of the human "G/T binding protein," (GTBP) also called p160 or hMSH6 (human MSH6). The MSH6 protein is a member of the Mutator S (MutS) family of proteins that are involved in DNA damage repair.
Defects in hMSH6 are associated with atypical hereditary nonpolyposis colorectal cancer not fulfilling the Amsterdam criteria for HNPCC. hMSH6 mutations have also been linked to endometrial cancer and the development of endometrial carcinomas.
Discovery[edit]
MSH6 was first identified in the budding yeast S. cerevisiae because of its homology to MSH2. The identification of the human GTBP gene and subsequent amino acid sequence availability showed that yeast MSH6 and human GTBP were more related to each other than any other MutS homolog, with a 26.6% amino acid identity.[5] Thus, GTBP took on the name human MSH6, or hMSH6.
Structure[edit]
In the human genome, hMSH6 is located on chromosome 2. It contains the Walker-A/B adenine nucleotide binding motif, which is the most highly conserved sequence found in all MutS homologs.[6] As with other MutS homologs, hMSH6 has an intrinsic ATPase activity. It functions exclusively when bound to hMSH2 as a heterodimer, although hMSH2 itself can function as a homomultimer or as a heterodimer with hMSH3.[7]
Function[edit]
Importance of mismatch repair[edit]
Mismatches commonly occur as a result of DNA replication errors, genetic recombination, or other chemical and physical factors.[8] Recognizing those mismatches and repairing them is extremely important for cells, because failure to do so results in microsatellite instability, an elevated spontaneous mutation rate (mutator phenotype), and susceptibility to HNPCC.[6][9] hMSH6 combines with hMSH2 to form the active protein complex, hMutS alpha, also called hMSH2-hMSH6.
Mismatch recognition[edit]
Mismatch recognition by this complex is regulated by the ADP to ATP transformation, which provides evidence that hMutS alpha complex functions as a molecular switch.[10] In normal DNA, adenine (A) bonds with thymine (T) and cytosine (C) bonds with guanine (G). Sometimes there will be a mismatch where T will bind with G, which is called a G/T mismatch. When a G/T mismatch is recognized, hMutS alpha complex binds and exchanges ADP for ATP.[9] The ADP-->ATP exchange causes a conformational change to convert hMutS alpha into a sliding clamp that can diffuse along the DNA backbone.[9] The ATP induces a release of the complex from the DNA and allows the hMutS alpha to dissociate along the DNA like a sliding clamp. This transformation helps trigger downstream events to repair the damaged DNA.[9]
Cancer[edit]
Although mutations in hMSH2 cause a strong general mutator phenotype, mutations in hMSH6 cause only a modest mutator phenotype.[5] At the gene level, the mutations were found to cause primarily single-base substitution mutations, which suggests that the role of hMSH6 is primarily for correcting single-base substitution mutations and to a lesser extent single base insertion/deletion mutations.[5]
Mutations in the hMSH6 gene cause the protein to be nonfunctional or only partially active, thus reducing its ability to repair mistakes in DNA. The loss of MSH6 function results in instability at mononucleotide repeats.[5] HNPCC is most commonly caused by mutations in hMSH2 and hMLH1, but mutations in hMSH6 are linked to an atypical form of HNPCC.[11] The penetrance of colorectal cancer seems to be lower in these mutations, meaning that a low proportion of hMSH6 mutation carriers present with the disease. Endometrial cancer, on the other hand, seems to be a more important clinical manifestation for female mutation carriers. The onset of endometrial cancer and also colon cancer in families with hMSH6 mutations is about 50 years. This is delayed compared to the age 44 onset of hMSH2-related tumors.[11]
Epigenetic control of MSH6 in cancer[edit]
Two microRNAs, miR21 and miR-155, target the DNA mismatch repair (MMR) genes hMSH6 and hMSH2, to cause reduced expression of their proteins.[12][13] If one or the other of these two microRNAs is over-expressed, hMSH2 and hMSH6 proteins are under-expressed, resulting in reduced DNA mismatch repair and increased microsatellite instability.
One of these microRNAs, miR21, is regulated by the epigenetic methylation state of the CpG islands in one or the other of its two promoter regions.[14] Hypomethylation of its promoter region is associated with increased expression of an miRNA.[15] High expression of a microRNA causes repression of its target genes (see microRNA silencing of genes). In 66% to 90% of colon cancers, miR-21 was over-expressed,[12] and generally the measured level of hMSH2 was decreased (and hMSH6 is unstable without hMSH2[13]).
The other microRNA, miR-155, is regulated both by epigenetic methylation of the CpG islands in its promoter region[16] and by epigenetic acetylation of histones H2A and H3 at the miR-155 promoter (where acetylation increases transcription).[17] Measured by two different methods, miR-155 was over-expressed in sporadic colorectal cancers by either 22% or 50%.[13] When miR-155 was elevated, hMSH2 was under-expressed in 44% to 67% of the same tissues (and hMSH6 is likely under-expressed as well, and also unstable in the absence of hMSH2).[13]
Interactions[edit]
MSH6 has been shown to interact with MSH2,[18][19][20][21][22] PCNA[23][24][25] and BRCA1.[18][26]
See also[edit]
References[edit]
- ^ a b c GRCh38: Ensembl release 89: ENSG00000116062 – Ensembl, May 2017
- ^ a b c GRCm38: Ensembl release 89: ENSMUSG00000005370 – Ensembl, May 2017
- ^ "Human PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ "Mouse PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ a b c d Marsischky GT, et al. (1996). "Redundancy of Saccharomyces cerevisiae MSH3 and MSH6 in MSH2-dependent mismatch repair". Genes Dev. 10 (4): 407–20. doi:10.1101/gad.10.4.407. PMID 8600025.
- ^ a b Fishel R, Kolodner RD (1995). "Identification of mismatch repair genes and their role in the development of cancer". Current Opinion in Genetics & Development. 5 (3): 382–95. doi:10.1016/0959-437X(95)80055-7. PMID 7549435.
- ^ Acharya S, et al. (1996). "hMSH2 forms specific mispair-binding complexes with hMSH3 and hMSH6". PNAS. 93 (24): 13629–34. Bibcode:1996PNAS...9313629A. doi:10.1073/pnas.93.24.13629. PMC 19374. PMID 8942985.
- ^ Friedberg EC, Walker GC, Siede W. (1995). DNA repair and mutagenesis. American Society for Microbiology, Washington DC.
- ^ a b c d Gradia S, et al. (1999). "hMSH2-hMSH6 forms a hydrolysis-independent sliding clamp on mismatched DNA". Molecular Cell. 3 (2): 255–61. doi:10.1016/S1097-2765(00)80316-0. PMID 10078208.
- ^ Gradia S, Acharya S, Fishel R (1997). "The human mismatch recognition complex hMSH2-hMSH6 functions as a novel molecular switch". Cell. 91 (7): 995–1005. doi:10.1016/S0092-8674(00)80490-0. PMID 9428522. S2CID 3551402.
- ^ a b Wagner A, et al. (2001). "Atypical HNPCC owing to MSH6 germline mutations: analysis of a large Dutch pedigree". J. Med. Genet. 38 (5): 318–22. doi:10.1136/jmg.38.5.318. PMC 1734864. PMID 11333868.
- ^ a b Valeri N, Gasparini P, Braconi C, Paone A, Lovat F, Fabbri M, Sumani KM, Alder H, Amadori D, Patel T, Nuovo GJ, Fishel R, Croce CM (2010). "MicroRNA-21 induces resistance to 5-fluorouracil by down-regulating human DNA MutS homolog 2 (hMSH2)". Proc. Natl. Acad. Sci. U.S.A. 107 (49): 21098–103. Bibcode:2010PNAS..10721098V. doi:10.1073/pnas.1015541107. PMC 3000294. PMID 21078976.
- ^ a b c d Valeri N, Gasparini P, Fabbri M, Braconi C, Veronese A, Lovat F, Adair B, Vannini I, Fanini F, Bottoni A, Costinean S, Sandhu SK, Nuovo GJ, Alder H, Gafa R, Calore F, Ferracin M, Lanza G, Volinia S, Negrini M, McIlhatton MA, Amadori D, Fishel R, Croce CM (2010). "Modulation of mismatch repair and genomic stability by miR-155". Proc. Natl. Acad. Sci. U.S.A. 107 (15): 6982–7. Bibcode:2010PNAS..107.6982V. doi:10.1073/pnas.1002472107. PMC 2872463. PMID 20351277.
- ^ Baer C, Claus R, Plass C (2013). "Genome-wide epigenetic regulation of miRNAs in cancer". Cancer Res. 73 (2): 473–7. doi:10.1158/0008-5472.CAN-12-3731. PMID 23316035.
- ^ Aure MR, Leivonen SK, Fleischer T, Zhu Q, Overgaard J, Alsner J, Tramm T, Louhimo R, Alnæs GI, Perälä M, Busato F, Touleimat N, Tost J, Børresen-Dale AL, Hautaniemi S, Troyanskaya OG, Lingjærde OC, Sahlberg KK, Kristensen VN (2013). "Individual and combined effects of DNA methylation and copy number alterations on miRNA expression in breast tumors". Genome Biol. 14 (11): R126. doi:10.1186/gb-2013-14-11-r126. PMC 4053776. PMID 24257477.
- ^ Krzeminski P, Sarasquete ME, Misiewicz-Krzeminska I, Corral R, Corchete LA, Martín AA, García-Sanz R, San Miguel JF, Gutiérrez NC (2015). "Insights into epigenetic regulation of microRNA-155 expression in multiple myeloma". Biochim. Biophys. Acta. 1849 (3): 353–66. doi:10.1016/j.bbagrm.2014.12.002. PMID 25497370.
- ^ Chang S, Wang RH, Akagi K, Kim KA, Martin BK, Cavallone L, Haines DC, Basik M, Mai P, Poggi E, Isaacs C, Looi LM, Mun KS, Greene MH, Byers SW, Teo SH, Deng CX, Sharan SK (2011). "Tumor suppressor BRCA1 epigenetically controls oncogenic microRNA-155". Nat. Med. 17 (10): 1275–82. doi:10.1038/nm.2459. PMC 3501198. PMID 21946536.
- ^ a b Wang Y, Cortez D, Yazdi P, Neff N, Elledge SJ, Qin J (Apr 2000). "BASC, a super complex of BRCA1-associated proteins involved in the recognition and repair of aberrant DNA structures". Genes & Development. 14 (8): 927–39. doi:10.1101/gad.14.8.927. PMC 316544. PMID 10783165.
- ^ Wang Y, Qin J (Dec 2003). "MSH2 and ATR form a signaling module and regulate two branches of the damage response to DNA methylation". Proceedings of the National Academy of Sciences of the United States of America. 100 (26): 15387–92. Bibcode:2003PNAS..10015387W. doi:10.1073/pnas.2536810100. PMC 307577. PMID 14657349.
- ^ Guerrette S, Wilson T, Gradia S, Fishel R (Nov 1998). "Interactions of human hMSH2 with hMSH3 and hMSH2 with hMSH6: examination of mutations found in hereditary nonpolyposis colorectal cancer". Molecular and Cellular Biology. 18 (11): 6616–23. doi:10.1128/mcb.18.11.6616. PMC 109246. PMID 9774676.
- ^ Bocker T, Barusevicius A, Snowden T, Rasio D, Guerrette S, Robbins D, Schmidt C, Burczak J, Croce CM, Copeland T, Kovatich AJ, Fishel R (Feb 1999). "hMSH5: a human MutS homologue that forms a novel heterodimer with hMSH4 and is expressed during spermatogenesis". Cancer Research. 59 (4): 816–22. PMID 10029069.
- ^ Acharya S, Wilson T, Gradia S, Kane MF, Guerrette S, Marsischky GT, Kolodner R, Fishel R (Nov 1996). "hMSH2 forms specific mispair-binding complexes with hMSH3 and hMSH6". Proceedings of the National Academy of Sciences of the United States of America. 93 (24): 13629–34. Bibcode:1996PNAS...9313629A. doi:10.1073/pnas.93.24.13629. PMC 19374. PMID 8942985.
- ^ Kleczkowska HE, Marra G, Lettieri T, Jiricny J (Mar 2001). "hMSH3 and hMSH6 interact with PCNA and colocalize with it to replication foci". Genes & Development. 15 (6): 724–36. doi:10.1101/gad.191201. PMC 312660. PMID 11274057.
- ^ Clark AB, Valle F, Drotschmann K, Gary RK, Kunkel TA (Nov 2000). "Functional interaction of proliferating cell nuclear antigen with MSH2-MSH6 and MSH2-MSH3 complexes". The Journal of Biological Chemistry. 275 (47): 36498–501. doi:10.1074/jbc.C000513200. PMID 11005803.
- ^ Ohta S, Shiomi Y, Sugimoto K, Obuse C, Tsurimoto T (Oct 2002). "A proteomics approach to identify proliferating cell nuclear antigen (PCNA)-binding proteins in human cell lysates. Identification of the human CHL12/RFCs2-5 complex as a novel PCNA-binding protein". The Journal of Biological Chemistry. 277 (43): 40362–7. doi:10.1074/jbc.M206194200. PMID 12171929.
- ^ Wang Q, Zhang H, Guerrette S, Chen J, Mazurek A, Wilson T, Slupianek A, Skorski T, Fishel R, Greene MI (Aug 2001). "Adenosine nucleotide modulates the physical interaction between hMSH2 and BRCA1". Oncogene. 20 (34): 4640–9. doi:10.1038/sj.onc.1204625. PMID 11498787.
Further reading[edit]
- Drummond JT, Li GM, Longley MJ, Modrich P (Jun 1995). "Isolation of an hMSH2-p160 heterodimer that restores DNA mismatch repair to tumor cells". Science. 268 (5219): 1909–12. Bibcode:1995Sci...268.1909D. doi:10.1126/science.7604264. PMID 7604264.
- Palombo F, Gallinari P, Iaccarino I, Lettieri T, Hughes M, D'Arrigo A, Truong O, Hsuan JJ, Jiricny J (Jun 1995). "GTBP, a 160-kilodalton protein essential for mismatch-binding activity in human cells". Science. 268 (5219): 1912–4. Bibcode:1995Sci...268.1912P. doi:10.1126/science.7604265. PMID 7604265.
- Papadopoulos N, Nicolaides NC, Liu B, Parsons R, Lengauer C, Palombo F, D'Arrigo A, Markowitz S, Willson JK, Kinzler KW (Jun 1995). "Mutations of GTBP in genetically unstable cells". Science. 268 (5219): 1915–7. Bibcode:1995Sci...268.1915P. doi:10.1126/science.7604266. PMID 7604266.
- Risinger JI, Umar A, Boyd J, Berchuck A, Kunkel TA, Barrett JC (Sep 1996). "Mutation of MSH3 in endometrial cancer and evidence for its functional role in heteroduplex repair". Nature Genetics. 14 (1): 102–5. doi:10.1038/ng0996-102. PMID 8782829. S2CID 25456490.
- Nicolaides NC, Palombo F, Kinzler KW, Vogelstein B, Jiricny J (Feb 1996). "Molecular cloning of the N-terminus of GTBP". Genomics. 31 (3): 395–7. doi:10.1006/geno.1996.0067. PMID 8838326.
- Acharya S, Wilson T, Gradia S, Kane MF, Guerrette S, Marsischky GT, Kolodner R, Fishel R (Nov 1996). "hMSH2 forms specific mispair-binding complexes with hMSH3 and hMSH6". Proceedings of the National Academy of Sciences of the United States of America. 93 (24): 13629–34. Bibcode:1996PNAS...9313629A. doi:10.1073/pnas.93.24.13629. PMC 19374. PMID 8942985.
- Miyaki M, Konishi M, Tanaka K, Kikuchi-Yanoshita R, Muraoka M, Yasuno M, Igari T, Koike M, Chiba M, Mori T (Nov 1997). "Germline mutation of MSH6 as the cause of hereditary nonpolyposis colorectal cancer". Nature Genetics. 17 (3): 271–2. doi:10.1038/ng1197-271. PMID 9354786. S2CID 22473295.
- Yin J, Kong D, Wang S, Zou TT, Souza RF, Smolinski KN, Lynch PM, Hamilton SR, Sugimura H, Powell SM, Young J, Abraham JM, Meltzer SJ (1998). "Mutation of hMSH3 and hMSH6 mismatch repair genes in genetically unstable human colorectal and gastric carcinomas". Human Mutation. 10 (6): 474–8. doi:10.1002/(SICI)1098-1004(1997)10:6<474::AID-HUMU9>3.0.CO;2-D. PMID 9401011. S2CID 2564806.
- Gradia S, Acharya S, Fishel R (Dec 1997). "The human mismatch recognition complex hMSH2-hMSH6 functions as a novel molecular switch". Cell. 91 (7): 995–1005. doi:10.1016/S0092-8674(00)80490-0. PMID 9428522. S2CID 3551402.
- Shiwaku HO, Wakatsuki S, Mori Y, Fukushige S, Horii A (Oct 1997). "Alternative splicing of GTBP in normal human tissues". DNA Research. 4 (5): 359–62. doi:10.1093/dnares/4.5.359. PMID 9455487.
- Wei Q, Guan Y, Cheng L, Radinsky R, Bar-Eli M, Tsan R, Li L, Legerski RJ (1998). "Expression of five selected human mismatch repair genes simultaneously detected in normal and cancer cell lines by a nonradioactive multiplex reverse transcription-polymerase chain reaction". Pathobiology. 65 (6): 293–300. doi:10.1159/000164141. PMID 9491849.
- Guerrette S, Wilson T, Gradia S, Fishel R (Nov 1998). "Interactions of human hMSH2 with hMSH3 and hMSH2 with hMSH6: examination of mutations found in hereditary nonpolyposis colorectal cancer". Molecular and Cellular Biology. 18 (11): 6616–23. doi:10.1128/mcb.18.11.6616. PMC 109246. PMID 9774676.
- Wang Q, Lasset C, Desseigne F, Saurin JC, Maugard C, Navarro C, Ruano E, Descos L, Trillet-Lenoir V, Bosset JF, Puisieux A (1999). "Prevalence of germline mutations of hMLH1, hMSH2, hPMS1, hPMS2, and hMSH6 genes in 75 French kindreds with nonpolyposis colorectal cancer". Human Genetics. 105 (1–2): 79–85. doi:10.1007/s004399900064. PMID 10480359.
- Wijnen J, de Leeuw W, Vasen H, van der Klift H, Møller P, Stormorken A, Meijers-Heijboer H, Lindhout D, Menko F, Vossen S, Möslein G, Tops C, Bröcker-Vriends A, Wu Y, Hofstra R, Sijmons R, Cornelisse C, Morreau H, Fodde R (Oct 1999). "Familial endometrial cancer in female carriers of MSH6 germline mutations". Nature Genetics. 23 (2): 142–4. doi:10.1038/13773. PMID 10508506. S2CID 30251596.
- Wu Y, Berends MJ, Mensink RG, Kempinga C, Sijmons RH, van Der Zee AG, Hollema H, Kleibeuker JH, Buys CH, Hofstra RM (Nov 1999). "Association of hereditary nonpolyposis colorectal cancer-related tumors displaying low microsatellite instability with MSH6 germline mutations". American Journal of Human Genetics. 65 (5): 1291–8. doi:10.1086/302612. PMC 1288281. PMID 10521294.
- Kolodner RD, Tytell JD, Schmeits JL, Kane MF, Gupta RD, Weger J, Wahlberg S, Fox EA, Peel D, Ziogas A, Garber JE, Syngal S, Anton-Culver H, Li FP (Oct 1999). "Germ-line msh6 mutations in colorectal cancer families". Cancer Research. 59 (20): 5068–74. PMID 10537275.
- Wang Y, Cortez D, Yazdi P, Neff N, Elledge SJ, Qin J (Apr 2000). "BASC, a super complex of BRCA1-associated proteins involved in the recognition and repair of aberrant DNA structures". Genes & Development. 14 (8): 927–39. doi:10.1101/gad.14.8.927. PMC 316544. PMID 10783165.
- Ceccotti S, Ciotta C, Fronza G, Dogliotti E, Bignami M (Jul 2000). "Multiple mutations and frameshifts are the hallmark of defective hPMS2 in pZ189-transfected human tumor cells". Nucleic Acids Research. 28 (13): 2577–84. doi:10.1093/nar/28.13.2577. PMC 102707. PMID 10871409.
- Christmann M, Kaina B (Nov 2000). "Nuclear translocation of mismatch repair proteins MSH2 and MSH6 as a response of cells to alkylating agents". The Journal of Biological Chemistry. 275 (46): 36256–62. doi:10.1074/jbc.M005377200. PMID 10954713.
- Clark AB, Valle F, Drotschmann K, Gary RK, Kunkel TA (Nov 2000). "Functional interaction of proliferating cell nuclear antigen with MSH2-MSH6 and MSH2-MSH3 complexes". The Journal of Biological Chemistry. 275 (47): 36498–501. doi:10.1074/jbc.C000513200. PMID 11005803.
External links[edit]
- FAQs on HNPCC Archived 2007-08-15 at the Wayback Machine from the National Institute of Health
- GeneReviews/NCBI/NIH/UW entry on Lynch syndrome
- MSH6+protein,+human at the U.S. National Library of Medicine Medical Subject Headings (MeSH)