Ovotesticular syndrome
| Ovotesticular Syndrome | |
|---|---|
| Other names | Ovotesticular disorder, OT-DSD |
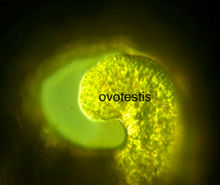 | |
| A gonad with both ovarian and testicular tissue. | |
| Specialty | Obstetrics and gynaecology, endocrinology |
Ovotesticular syndrome (also known as ovotesticular disorder or OT-DSD) is a rare congenital condition where an individual is born with both ovarian and testicular tissue.[1][2] It is one of the rarest DSDs, with only 500 reported cases.[3] Commonly, one or both gonads is an ovotestis containing both types of tissue.[3] Although it is similar in some ways to mixed gonadal dysgenesis, the conditions can be distinguished histologically.[4]
Terminology[edit]
In the past, ovotesticular syndrome was referred to as true hermaphroditism, which is considered outdated as of 2006.[5] The term "true hermaphroditism" was considered incredibly misleading by many medical organizations and by many advocacy groups,[6][7][8][9] as hermaphroditism refers to a species that produces both sperm and ova, something that is impossible in humans.[10]
Symptoms[edit]
Physical[edit]
- Gynecomastia (present in 75% of cases)[11]
- Small phallus midway in size between a clitoris and a penis[12]
- Incompletely closed urogenital opening (shallow vagina)[12]
- Abnormal urethra opening on the perineum[12]
Cognitive[edit]
Studies on the limited amount of cases on ovotesticular syndrome shows the condition does not impair cognitive impairment.[13]
History[edit]
The first medical attempts to document cases appeared in the 16th century. Up until the Late Middle Ages individuals with these conditions were looked down upon.[14]
Causes[edit]
There are several ways in which this may occur.
- It can be caused by the division of one ovum, followed by fertilization of each haploid ovum and fusion of the two zygotes early in development.
- Alternately, an ovum can be fertilized by two sperm followed by trisomic rescue in one or more daughter cells.
- Two ova fertilized by two sperm cells will occasionally fuse to form a tetragametic chimera, if one male zygote and one female zygote fuse.
- It can be associated with a mutation in the SRY gene.[15]
Note: The SRY gene has a 10 to 30% of showing up in those that are found to have ovotesticular syndrome. Due to the genetic makeup of an SRY gene, it implies that ovotesticular syndrome is more of a heterogeneous condition.[16]
Variations[edit]
It is documented to show up in 4 different variations. Those being Bilateral, Unilateral, Lateral, and Indeterminate.[17]
- Bilateral - both the ovaries and testicle tissues appear on both sides.[17]
- Unilateral - on one side there is what is known as ovotestis (both ovary and testicle tissue), and the other side has either ovary tissue or testicular tissue - not both.[17]
- Lateral - both testicular and ovary tissue are present, but are on opposite sides.[17]
- Indeterminate - it is known that the condition is present, but it isn't evident as to where the testicular or ovary tissue is located.[17]
Karyotypes[edit]
In ovotesticular syndrome, XX is the most common (55-80% of cases); most individuals with this form are SRY negative.[18]
Next most common are XX/XY (20-30% of cases) and XY (5-15% of cases), with the remainder being a variety of other chromosomal anomalies and mosaicisms.[19][18]
Some degree of mosaicism is present in about 25%.[18] Encountered karyotypes include 46XX/46XY, or 46XX/47XXY or XX & XY with SRY mutations, mixed chromosomal anomalies or hormone deficiency/excess disorders, 47XXY. Less than 1% have XX/XY chimerism.[18]
Prevalence[edit]
Ovotesticular syndrome represents 5% of all sex disorder differentiations.[20]
The exact number of confirmed cases is uncertain, but by 1991 approximately 500 cases had been confirmed.[3]
It has also been estimated that more than 525 have been documented.[14] While it can appear anywhere in the world, and be reported or unreported, the greatest amounts reported of ovotesticular syndrome is from Africa and Europe.[21]
Fertility[edit]
The gonad most likely to function is the ovary.[22] The ovotestes show evidence of ovulation in 50% of cases.[23] Spermatogenesis has only been observed in solitary testes and not in the testicular portions of ovotestes.[24][23] According to a 1994 study, spermatogenesis has only been proven in two cases.[25] In one of the two cases, a phenotypically male individual with XX,46/XY,46 mixture had fathered a child.[26] It has been estimated that 80% of cases could be fertile as females with the right surgeries.[14]
Documented cases of fertility[edit]
There are extremely rare cases of fertility in humans with ovotesticular syndrome.[25][27]
In 1994, a study on 283 cases found 21 pregnancies from 10 individuals with ovotesticular syndrome, while one allegedly fathered a child.[25]
As of 2010, there have been at least 11 reported cases of fertility in humans with ovotesticular syndrome in the scientific literature,[4] with one case of a person with XY-predominant (96%) mosaic giving birth.[28] All known offspring have been male.[29] There has been at least one case of an individual being fertile as a male.[26]
There is a hypothetical scenario, in which it could be possible for a human to self-fertilize.[30] If a human chimera is formed from a male and female zygote fusing into a single embryo, giving an individual functional gonadal tissue of both types, such self-fertilization is feasible. Indeed, it is known to occur in non-human species where hermaphroditic animals are common[31] and has been observed in a rabbit.[32] However, no such case of functional self-fertilization or "true bi-sexuality" has been documented in humans.[24][20]
Society and culture[edit]
Having Ovotesticular syndrome of sexual development can make one inadmissible for service in the United States Armed Forces.[33]
M.C. v. Aaronson[edit]
The U.S. legal case of M.C. v. Aaronson, advanced by intersex civil society organization interACT with the Southern Poverty Law Center, was brought before the courts in 2013.[34][35][36][37] The child in the case was born in December 2004 with ovotestes, initially determined as male, but subsequently assigned female and placed in the care of South Carolina Department of Social Services in February 2005.[38] Physicians responsible for M.C. initially concluded that surgery was not urgent or necessary and M.C. had potential to identify as male or female, but, in April 2006, M.C. was subjected to feminizing medical interventions.[38] According to the Encyclopedia Britannica, "The reconstruction of female genitalia was more readily performed than the reconstruction of male genitalia, so ambiguous individuals often were made to be female."[39] He was adopted in December 2006. M.C. identified as male at the time the case was brought, at age eight. The defendant in the case, Dr. Ian Aaronson, had written in 2001 that "feminizing genitoplasty on an infant who might eventually identify herself as a boy would be catastrophic".[40][38]
The defendants sought to dismiss the case and seek a defense of qualified immunity, but these were denied by the District Court for the District of South Carolina. In January 2015, the Court of Appeals for the Fourth Circuit reversed this decision and dismissed the complaint, stating that, it did not "mean to diminish the severe harm that M.C. claims to have suffered" but that in 2006 it was not clear that there was precedent that the surgery on a sixteen-month-old violated an established constitutional right.[41] The Court did not rule on whether or not the surgery violated M.C.'s constitutional rights.[42]
State suits were subsequently filed.[41] In July 2017, it was reported that the case had been settled out of court by the Medical University of South Carolina for $440,000. The university denied negligence, but agreed to a "compromise" settlement to avoid "costs of litigation."[43]
See also[edit]
References[edit]
- ^ Barseghyan, Hayk; Vilain, Eric (2014). "The Genetics of Ovotesticular Disorders of Sex Development". Genetic Steroid Disorders. pp. 261–263. doi:10.1016/B978-0-12-416006-4.00020-X. ISBN 978-0-12-416006-4.
- ^ Lee, Peter A.; Houk, Christopher P.; Ahmed, S. Faisal; Hughes, Ieuan A. (1 August 2006). "Consensus Statement on Management of Intersex Disorders". Pediatrics. 118 (2): e488–e500. doi:10.1542/peds.2006-0738. PMC 2082839. PMID 16882788.
- ^ a b c Nistal, Manuel; Paniagua, Ricardo; González-Peramato, Pilar; Reyes-Múgica, Miguel (2015-09-01). "Perspectives in Pediatric Pathology, Chapter 7. Ovotesticular DSD (True Hermaphroditism)". Pediatric and Developmental Pathology. 18 (5): 345–352. doi:10.2350/14-04-1466-PB.1. ISSN 1093-5266. PMID 25105460. S2CID 34009652.
- ^ a b Kim, Kyu-Rae; Kwon, Youngmee; Joung, Jae Young; Kim, Kun Suk; Ayala, Alberto G.; Ro, Jae Y. (October 2002). "True Hermaphroditism and Mixed Gonadal Dysgenesis in Young Children: A Clinicopathologic Study of 10 Cases". Modern Pathology. 15 (10): 1013–1019. doi:10.1097/01.MP.0000027623.23885.0D. PMID 12379746.
- ^ Lee, Peter A.; Houk, Christopher P.; Ahmed, S. Faisal; Hughes, Ieuan A. (1 August 2006). "Consensus Statement on Management of Intersex Disorders". Pediatrics. 118 (2): e488–e500. doi:10.1542/peds.2006-0738. PMID 16882788. S2CID 11236329. Retrieved 1 May 2023.
- ^ Herndon A. "Getting Rid of "Hermaphroditism" Once and For All". Intersex Society of North America. Archived from the original on 27 September 2011. Retrieved 2 October 2011.
- ^ "Is a person who is intersex a hermaphrodite?". Intersex Society of North America. Retrieved 2024-01-20.
The mythological term "hermaphrodite" implies that a person is both fully male and fully female. This is a physiologic impossibility. The words "hermaphrodite" and "pseudo-hermaphrodite" are stigmatizing and misleading words.
- ^ Knight, Kyle (2017-07-25). ""I Want to Be Like Nature Made Me": Medically Unnecessary Surgeries on Intersex Children in the US". Human Rights Watch.
It is now considered pejorative and outdated, although a small number of intersex people have reclaimed the term.
- ^ "What is Intersex? Frequently Asked Questions". interACT: Advocates for Intersex Youth. Retrieved 2022-10-31.
Some intersex people have reclaimed this word for themselves, but it is usually considered a slur. There are many ways to have an intersex body, but it is not possible for one person to have both a fully developed penis and vagina.
- ^ Mills A (2018-01-01). Biology of Sex. University of Toronto Press. p. 309. ISBN 978-1-4875-9337-7.
In the past, the term hermaphrodite was widely applied in such cases, but humans are not hermaphroditic. In a truly hermaphroditic species, individuals have functional sets of male and female organs.
- ^ Mancino, Anne T.; Young, Zachary T.; Bland, Kirby I. (2018-01-01). "Gynecomastia". The Breast: 104–115.e5. doi:10.1016/B978-0-323-35955-9.00007-6. ISBN 9780323359559.
- ^ a b c Fitzgerald, PH; Donald, RA; Kirk, RL (1979). "A true hermaphrodite dispermic chimera with 46, XX and 46, XY karyotypes". Clin Genet. 15 (1): 89–96. doi:10.1111/j.1399-0004.1979.tb02032.x. PMID 759058. S2CID 39280592.
- ^ Aruna, N; Purushottam, RM; Rajangam, S (2006). "46,XX/46,XY chimerism - a case report". J Anat Soc India. 55 (1): 24–26.
- ^ a b c Wynbrandt, James; Ludman, Mark D. (2010-05-12). The Encyclopedia of Genetic Disorders and Birth Defects. Infobase Publishing. ISBN 978-1-4381-2095-9.
- ^ Braun, A; Kammerer, S; Cleve, H; Löhrs, U; Schwarz, H P; Kuhnle, U (March 1993). "True hermaphroditism in a 46,XY individual, caused by a postzygotic somatic point mutation in the male gonadal sex-determining locus (SRY): molecular genetics and histological findings in a sporadic case". American Journal of Human Genetics. 52 (3): 578–585. PMC 1682159. PMID 8447323.
- ^ Martini, Luciano (2004). Encyclopedia of Endocrine Diseases. Academic Press.
- ^ a b c d e Bland, Kirby; Copeland iii, Edward; Klimberg, V. Suzanne; Gradishar, William (2018). The Breast: Comprehensive Management of Benign and Malignant Diseases. Elsevier Health Sciences.
- ^ a b c d Al-Salem, Ahmed H. (2020), Al-Salem, Ahmed H. (ed.), "Ovotestis Disorders of Sexual Development", Pediatric Gynecology: An Illustrated Guide for Surgeons, Cham: Springer International Publishing, pp. 469–478, doi:10.1007/978-3-030-49984-6_24, ISBN 978-3-030-49984-6, S2CID 226562793, retrieved 2021-04-23
- ^ Bouvattier, Claire (2010-01-01), Gearhart, John P.; Rink, Richard C.; Mouriquand, Pierre D. E. (eds.), "CHAPTER 35 - DISORDERS OF SEX DEVELOPMENT: ENDOCRINE ASPECTS", Pediatric Urology (Second Edition), Philadelphia: W.B. Saunders, pp. 459–475, ISBN 978-1-4160-3204-5, retrieved 2020-09-08
- ^ a b Ceci, Michelle; Calleja, Edward; Said, Edith; Gatt, Noel (2015-02-03). "A Case of True Hermaphroditism Presenting as a Testicular Tumour". Case Reports in Urology. 2015: 598138. doi:10.1155/2015/598138. PMC 4333191. PMID 25774314.
- ^ Moshang, Thomas (2005). Pediatric Endocrinology: The Requisites.
- ^ Hutson, John M.; Warne, Garry L.; Grover, Sonia R. (2012-02-02). Disorders of Sex Development: An Integrated Approach to Management. Springer Science & Business Media. pp. 84–85. ISBN 978-3-642-22963-3.
- ^ a b Bhattacharya, Niranjan; Stubblefield, Phillip G. (2016-05-17). Human Fetal Growth and Development: First and Second Trimesters. Springer. ISBN 978-3-319-14874-8.
- ^ a b Bayraktar, Zeki (28 February 2017). "Potential autofertility in true hermaphrodites". The Journal of Maternal-Fetal & Neonatal Medicine. 31 (4): 542–547. doi:10.1080/14767058.2017.1291619. PMID 28282768. S2CID 22100505.
- ^ a b c Krob, G.; Braun, A.; Kuhnle, U. (January 1994). "True hermaphroditism: Geographical distribution, clinical findings, chromosomes and gonadal histology". European Journal of Pediatrics. 153 (1): 2–10. doi:10.1007/BF02000779. PMID 8313919. S2CID 1931001.
- ^ a b Parvin, Simon (May 1982). "Ovulation in a cytogenetically proved phenotypically male fertile hermaphrodite". British Journal of Surgery. 69 (5): 279–280. doi:10.1002/bjs.1800690517. PMID 7200380. S2CID 28027980.
- ^ Ahmad, M.; Saleem, M.; Jam, M. R.; Iqbal, M. Z. (2011). "True hermaphrodite: a case report". APSP Journal of Case Reports. 2 (2): 16. ISSN 2218-8185. PMC 3418019. PMID 22953283.
- ^ Schoenhaus, S. A.; Lentz, S. E.; Saber, P; Munro, M. G.; Kivnick, S (2008). "Pregnancy in a hermaphrodite with a male-predominant mosaic karyotype". Fertility and Sterility. 90 (5): 2016.e7–10. doi:10.1016/j.fertnstert.2008.01.104. PMID 18394621.
- ^ Schultz, Brett A. H.; Roberts, Soldrea; Rodgers, Allison; Ataya, Khalid (2009). "Pregnancy in True Hermaphrodites and All Male Offspring to Date". Obstetrics & Gynecology. 113 (2): 534–536. doi:10.1097/AOG.0b013e3181866456. PMID 19155947. S2CID 42128830.
- ^ Irmak, M. Kemal (2010-11-01). "Self-fertilization in human: Having a male embryo without a father". Medical Hypotheses. 75 (5): 448–451. doi:10.1016/j.mehy.2010.04.021.
- ^ Jarne, Philippe; Auld, Josh R. (2006). "Animals Mix It up Too: The Distribution of Self-Fertilization Among Hermaphroditic Animals". Evolution. 60 (9): 1816–24. doi:10.1554/06-246.1. PMID 17089966. S2CID 23849389.
- ^ Frankenhuis, M. T.; Smith-Buijs, C. M.; de Boer, L. E.; Kloosterboer, J. W. (1990-06-16). "A case of combined hermaphroditism and autofertilisation in a domestic rabbit". The Veterinary Record. 126 (24): 598–599. ISSN 0042-4900. PMID 2382355.
- ^ "DoD Instruction 6130.03 Medical Standards For Appointment, Enlistment, Or Induction Into The Military Services" (PDF). September 27, 2018. Archived from the original (PDF) on 2018-09-27 – via Wayback Machine.
- ^ "AIC's Landmark Lawsuit Makes History!". AIC. May 16, 2013. Archived from the original on February 6, 2017.
- ^ Southern Poverty Law Center (May 14, 2013). "M.C. v. Aaronson". Retrieved November 8, 2022.
- ^ Reis, Elizabeth (May 17, 2013). "Do No Harm: Intersex Surgeries and the Limits of Certainty". Nursing Clio. Retrieved 2015-07-20.
- ^ Dreger, Alice (May 16, 2013). "When to Do Surgery on a Child With 'Both' Genitalia". The Atlantic. Retrieved 2015-07-20.
- ^ a b c White, Ryan L. (2013). "Preferred Private Parts: Importing Intersex Autonomy for M.C. v. Aaronson". Fordham International Law Journal. 37: 777.
- ^ "Hermaphroditism | Definition, Types, & Effects | Britannica".
- ^ Aaronson, Ian A (July 2001). "The investigation and management of the infant with ambiguous genitalia: A surgeon's perspective". Current Problems in Pediatrics. 31 (6): 168–194. doi:10.1067/mps.2001.116127. PMID 11436003.
- ^ a b Largent, Emily (March 5, 2015). "M.C. v. Aaronson". Petrie-Flom Center, Harvard Law.
- ^ interACT (January 27, 2015). "Update on M.C.'s Case – The Road to Justice can be Long, but there is more than one path for M.C." Archived from the original on February 19, 2017. Retrieved 2017-02-18.
- ^ Ghorayshi, Azeen (July 27, 2017). "A Landmark Lawsuit About An Intersex Baby's Genital Surgery Just Settled For $440,000". BuzzFeed. Retrieved 2017-07-27.
External links[edit]
 Media related to Intersex at Wikimedia Commons
Media related to Intersex at Wikimedia Commons
