Public health mitigation of COVID-19

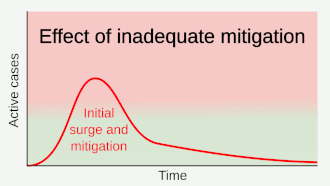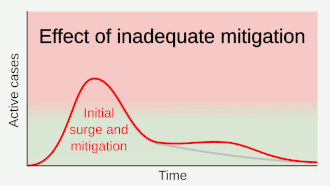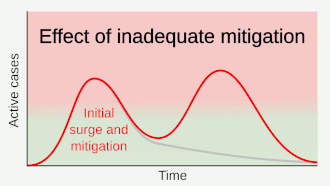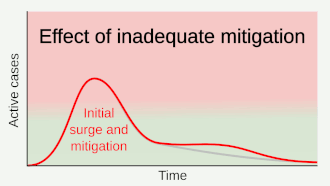
Part of managing an infectious disease outbreak is trying to delay and decrease the epidemic peak, known as flattening the epidemic curve.[1] This decreases the risk of health services being overwhelmed and provides more time for vaccines and treatments to be developed.[1] Non-pharmaceutical interventions that may manage the outbreak include personal preventive measures such as hand hygiene, wearing face masks, and self-quarantine; community measures aimed at physical distancing such as closing schools and cancelling mass gathering events; community engagement to encourage acceptance and participation in such interventions; as well as environmental measures such surface cleaning.[5] It has also been suggested that improving ventilation and managing exposure duration can reduce transmission.[6][7]
During early outbreaks, speed and scale were considered key to mitigation of COVID-19, due to the fat-tailed nature of pandemic risk and the exponential growth of COVID-19 infections.[8] For mitigation to be effective, (a) chains of transmission must be broken as quickly as possible through screening and containment, (b) health care must be available to provide for the needs of those infected, and (c) contingencies must be in place to allow for effective rollout of (a) and (b).[citation needed]
By May 2023, in most countries restrictions had been lifted and everyday life had returned to how it was before the pandemic due to improvement in the pandemic's situation.[9][10]
| Part of a series on the |
| COVID-19 pandemic |
|---|
 |
|
|
|
Initial containment measures[edit]
More drastic actions aimed at containing the outbreak were taken in China once the severity of the outbreak became apparent, such as quarantining entire cities or imposing strict travel bans.[11] Other countries also adopted a variety of measures aimed at limiting the spread of the virus, including resorting to states of emergency.[12] South Korea introduced the mass screening and localised quarantines and issued alerts on the movements of infected individuals. Singapore provided financial support for those infected who quarantined themselves and imposed large fines for those who failed to do so. Taiwan increased face mask production and penalised hoarding of medical supplies.[13] The zero-COVID approach aims to prevent viral transmission, using a number of different measures, including vaccination and non-pharmaceutical interventions such as contact-tracing and quarantine. Different combinations of measures are used during the initial containment phase, when the virus is first eliminated from a region, and the sustained containment phase, when the goal is to prevent reestablishment of viral transmission within the community.[14] Experts differentiate between zero-COVID, which is an elimination strategy, and mitigation strategies that attempt to lessen the effects of the virus on society, but which still tolerate some level of transmission within the community.[15][16] These initial strategies can be pursued sequentially or simultaneously during the acquired immunity phase through natural and vaccine-induced immunity.[17]
Costs and challenges[edit]
Simulations for Great Britain and the United States show that mitigation (slowing but not stopping epidemic spread) and suppression (reversing epidemic growth) have major challenges. Optimal mitigation policies might reduce peak healthcare demand by two-thirds and deaths by half, but still result in hundreds of thousands of deaths and overwhelmed health systems. Suppression can be preferred but needs to be maintained for as long as the virus is circulating in the human population (or until a vaccine becomes available), as transmission otherwise quickly rebounds when measures are relaxed. Until now, the evidence for public health (nonpharmaceutical) interventions such as social distancing, school closure, and case isolation comes mainly from epidemiological compartmental models and, in particular, agent-based models (ABMs).[18] Such models have been criticized for being based on simplifying and unrealistic assumptions.[19][20] Still, they can be useful in informing decisions regarding mitigation and suppression measures in cases when ABMs are accurately calibrated.[21] An Argentinian modelling study asserted that complete lockdowns and healthcare system overextension could be avoided if 45 percent of asymptomatic patients were detected and isolated.[22] Long-term intervention to suppress the pandemic has considerable social and economic costs.[23]
Efficacy[edit]
This section needs to be updated. (December 2021) |
This article may lend undue weight to certain ideas, incidents, or controversies. (December 2021) |
In August 2020, a working paper by the National Bureau of Economic Research (NBER) questioned major effects of many mitigation and suppression measures. The authors compared the development of casualties connected to SARS-CoV-2 until July 2020, in 25 US states and 23 countries that had counted more than 1.000 overall deaths each. From the date a state passed a threshold of 25 deaths, the statistical study observed a largely uniform development, independently from type and time frame of governmental interactions. Thus, the growth rate of casualties dropped to zero within 20–30 days, and the variability between regions was low, except at the beginning of the epidemics. The authors computed the effective reproduction number Reff with the aid of different models like the SIR model, and found it hovering around one everywhere after the first 30 days of the epidemic. Hence, they did not find evidence for an influence of lockdowns, travel restrictions or quarantines on virus transmission.[24] For contradicting studies, they assume an omitted variable bias. Candidates for ignored effects could be voluntary social distancing, the structure of social interaction networks (some people contact more networks faster than others), and a natural tendency of an epidemics to spread quickly at first and slow down, which has been observed in former Influenza pandemics, but not yet completely understood. The reviewer Stephen C. Miller concludes “that human interaction does not conform to simple epidemiological models”.[25][24]
Many reviews find high efficacy of mitigation measures such as vaccines, face masks and social distancing. For instance, a systematic review and meta-analysis found that mask-wearing cuts the incidence of COVID-19 by 53% overall.[26][27] The efficacy may also be substantially higher, especially if certain types of masks are worn or under specific conditions and settings.
Contact tracing[edit]
Contact tracing is an important method for health authorities to determine the source of infection and to prevent further transmission.[28] The use of location data from mobile phones by governments for this purpose has prompted privacy concerns, with Amnesty International and more than a hundred other organisations issuing a statement calling for limits on this kind of surveillance.[29]
An unincentivized and always entirely voluntary use of such digital contact tracing apps by the public was found to be low[30][31][32] even if the apps are built to preserve privacy (which may however compete with alternative domestic apps that don't do so and can't always be used), leading to low usefulness of the software for pandemic mitigation as of April 2021. A lack of possible features, prevalent errors and possibly other issues reduced their usefulness further.[33] Use of such an app in general or during specific times is in many or all cases not provable or requirable.
Moreover, contact-tracing apps may be designed criteria (<1 metre; and > 15 minutes contact) insufficient for controlling danger.[34]
Information technology[edit]
Several mobile apps have been implemented or proposed for voluntary use, and as of 7 April 2020 more than a dozen expert groups were working on privacy-friendly solutions such as using Bluetooth to log a user's proximity to other cellphones.[29] (Users are alerted if they have been near someone who subsequently tests positive.)[29]
On 10 April 2020, Google and Apple jointly announced an initiative for privacy-preserving contact tracing based on Bluetooth technology and cryptography.[35][36] The system is intended to allow governments to create official privacy-preserving coronavirus tracking apps, with the eventual goal of integration of this functionality directly into the iOS and Android mobile platforms.[37] In Europe and in the U.S., Palantir Technologies is also providing COVID-19 tracking services.[38]
In February 2020, China launched a mobile app to deal with the disease outbreak.[39] Users are asked to enter their name and ID number. The app can detect 'close contact' using surveillance data and therefore a potential risk of infection. Every user can also check the status of three other users. If a potential risk is detected, the app not only recommends self-quarantine, it also alerts local health officials.[40]
Big data analytics on cellphone data, facial recognition technology, mobile phone tracking, and artificial intelligence are used to track infected people and people whom they contacted in South Korea, Taiwan, and Singapore.[41][42] In March 2020, the Israeli government enabled security agencies to track mobile phone data of people supposed to have coronavirus. According to the Israeli government, the measure was taken to enforce quarantine and protect those who may come into contact with infected citizens. The Association for Civil Rights in Israel, however, said the move was "a dangerous precedent and a slippery slope".[43] Also in March 2020, Deutsche Telekom shared aggregated phone location data with the German federal government agency, Robert Koch Institute, to research and prevent the spread of the virus.[44] Russia deployed facial recognition technology to detect quarantine breakers.[45] Italian regional health commissioner Giulio Gallera said he has been informed by mobile phone operators that "40% of people are continuing to move around anyway".[46] The German Government conducted a 48-hour weekend hackathon, which had more than 42,000 participants.[47][48] Three million people in the UK used an app developed by King's College London and Zoe to track people with COVID-19 symptoms.[49][50] The president of Estonia, Kersti Kaljulaid, made a global call for creative solutions against the spread of coronavirus.[51]
Health care[edit]

Increasing capacity and adapting healthcare for the needs of COVID-19 patients is described by the WHO as a fundamental outbreak response measure.[52] The ECDC and the European regional office of the WHO have issued guidelines for hospitals and primary healthcare services for shifting of resources at multiple levels, including focusing laboratory services towards COVID-19 testing, cancelling elective procedures whenever possible, separating and isolating COVID-19 positive patients, and increasing intensive care capabilities by training personnel and increasing the number of available ventilators and beds.[52][53] In addition, in an attempt to maintain physical distancing, and to protect both patients and clinicians, in some areas non-emergency healthcare services are being provided virtually.[54][55][56]
Research and development[edit]
There are research-based developments that aim to mitigate COVID-19 spread beyond vaccines, repurposed and new medications and similar conventional measures.
Researchers investigate for safe ways of public transport during the COVID-19 pandemic.[57][58]
Novel vaccine passports have been developed.
Researchers are developing face-masks which could be more effective at reducing SARS-CoV-2 spread than existing ones and/or have other desired properties such as biodegradability and better breathability.[59][60][61][62][63][64] Some are also researching attachments to existing face-masks to make them more effective[63] or to add self-cleaning features.[63] The pandemic has increased efforts to develop such masks and some have received government grants for their development.[63]
Ventilation and air cleaners are also the subject of research and development.[65][66]
Researchers report the development of chewing gums that could mitigate COVID-19 spread. The ingredients – CTB-ACE2 proteins grown via plants – bind to the virus.[67][68]
On 23 April 2020, NASA reported building, in 37 days, a ventilator (called VITAL).[69][70] On April 30, NASA reported receiving fast-track approval for emergency use by the United States Food and Drug Administration for the new ventilator.[71] As of March 2020[update], 26 manufacturers around the world have been licensed to make the device.[72] The COVID-19 pandemic increased the demand for oxygen concentrators. During the pandemic open source oxygen concentrators were developed, locally manufactured – with prices below imported products – and used, especially during a COVID-19 pandemic wave in India.[73][74] Due to capacity limitations in the standard supply chains, some manufacturers are 3D printing healthcare material such as nasal swabs and ventilator parts.[75][76] In one example, when an Italian hospital urgently required a ventilator valve, and the supplier was unable to deliver in the timescale required, a local startup received legal threats due to alleged patent infringement after reverse-engineering and printing the required hundred valves overnight.[77][78][79]
Living with COVID-19[edit]
COVID-19 is predicted to become an endemic disease by many experts. The observed behavior of SARS-CoV-2, the virus that causes COVID-19, suggests it is unlikely it will die out, and the lack of a COVID-19 vaccine that provides long-lasting immunity against infection means it cannot immediately be eradicated;[80] thus, a future transition to an endemic phase appears probable. In an endemic phase, people would continue to become infected and ill, but in relatively stable numbers.[80] Such a transition may take years or decades.[81] Precisely what would constitute an endemic phase is contested.[82]
COVID-19 endemicity is distinct from the COVID-19 public health emergency of international concern, which was ended by the World Health Organization on May 5, 2023.[83] Endemic is a frequently misunderstood and misused word outside the realm of epidemiology. Endemic does not mean mild, or that COVID-19 must become a less hazardous disease. Some politicians and commentators have conflated what they termed endemic COVID-19 with the lifting of public health restrictions or a comforting return to pre-pandemic normality.
The severity of endemic disease would be dependent on various factors, including the evolution of the virus, population immunity, and vaccine development and rollout.[81][84][85]See also[edit]
- Treatment and management of COVID-19#Prevention of onward transmission
- Impact of the COVID-19 pandemic on science and technology
References[edit]
- ^ a b c d Anderson RM, Heesterbeek H, Klinkenberg D, Hollingsworth TD (March 2020). "How will country-based mitigation measures influence the course of the COVID-19 epidemic?". Lancet. 395 (10228): 931–934. doi:10.1016/S0140-6736(20)30567-5. PMC 7158572. PMID 32164834.
A key issue for epidemiologists is helping policy makers decide the main objectives of mitigation—e.g. minimising morbidity and associated mortality, avoiding an epidemic peak that overwhelms health-care services, keeping the effects on the economy within manageable levels, and flattening the epidemic curve to wait for vaccine development and manufacture on scale and antiviral drug therapies.
- ^ Qualls N, Levitt A, Kanade N, Wright-Jegede N, Dopson S, Biggerstaff M, et al. (April 2017). "Community Mitigation Guidelines to Prevent Pandemic Influenza - United States, 2017". MMWR. Recommendations and Reports. 66 (1): 1–34. doi:10.15585/mmwr.rr6601a1. PMC 5837128. PMID 28426646.
- ^ Barclay E, Scott D, Animashaun C (2020-04-07). "The US doesn't just need to flatten the curve. It needs to "raise the line."". Vox. Archived from the original on 2020-04-07.
- ^ Wiles S (2020-03-14). "After 'Flatten the Curve', we must now 'Stop the Spread'. Here's what that means". The Spinoff. Archived from the original on 2020-03-26. Retrieved 2020-03-13.
- ^ "Community Mitigation Guidelines to Prevent Pandemic Influenza—United States, 2017". Recommendations and Reports. 66 (1). 2017-04-12.
- ^ Epperly DE, Rinehart KR, Caney DN (2020). "COVID-19 Aerosolized Viral Loads, Environment, Ventilation, Masks, Exposure Time, Severity, And Immune Response: A Pragmatic Guide Of Estimates". medRxiv 10.1101/2020.10.03.20206110.
- ^ "Viral Load Exposure Factors". ReallyCorrect.com.
- ^ Cirillo, Pasquale and Nassim Nicholas Taleb (2020). "Tail Risk of Contagious Diseases". Nature Physics. 16 (6): 606–613. arXiv:2004.08658. Bibcode:2020NatPh..16..606C. doi:10.1038/s41567-020-0921-x. S2CID 215828381.
- ^ "From emergency response to long-term COVID-19 disease management: sustaining gains made during the COVID-19 pandemic". www.who.int. World Health Organization. Retrieved 9 May 2023.
- ^ Heyward G, Silver M. "WHO ends global health emergency declaration for COVID-19". Retrieved 9 May 2023.
- ^ Qin A (2020-03-07). "China May Be Beating the Coronavirus, at a Painful Cost". The New York Times.
- ^ Lundgren M, Klamberg M, Sundström K, Dahlqvist J (2020). "Emergency Powers in Response to COVID-19: Policy Diffusion, Democracy, and Preparedness". Nordic Journal of Human Rights. 38 (4): 305–318. arXiv:2007.00933. doi:10.1080/18918131.2021.1899406.
- ^ McCurry J, Ratcliffe R, Davidson H (2020-03-11). "Mass testing, alerts and big fines: the strategies used in Asia to slow coronavirus". The Guardian.
- ^ Anna Llupià, Rodríguez-Giralt, Anna Fité, Lola Álamo, Laura de la Torre, Ana Redondo, Mar Callau and Caterina Guinovart (2020) What Is a Zero-COVID Strategy Archived 2022-01-03 at the Wayback Machine, Barcelona Institute for Global Health - COVID-19 & response strategy.
- ^ Oliu-Barton M, Pradelski BS, Aghion P, Artus P, Kickbusch I, Lazarus JV, et al. (28 April 2021). "SARS-CoV-2 elimination, not mitigation, creates best outcomes for health, the economy, and civil liberties". The Lancet. 397 (10291): 2234–2236. doi:10.1016/S0140-6736(21)00978-8. PMC 8081398. PMID 33932328.
- ^ Li Z, Chen Q, Feng L, Rodewald L, Xia Y, Yu H, et al. (4 June 2020). "Active case finding with case management: the key to tackling the COVID-19 pandemic". The Lancet. 396 (10243): 63–70. doi:10.1016/S0140-6736(20)31278-2. PMC 7272157. PMID 32505220.
- ^ Bhopal RS (9 September 2020). "To achieve "zero covid" we need to include the controlled, careful acquisition of population (herd) immunity". BMJ. 370: m3487. doi:10.1136/bmj.m3487. eISSN 1756-1833. hdl:20.500.11820/59628557-672e-47bb-b490-9c9965179a27. PMID 32907816. S2CID 221538577.
- ^ Adam D (April 2020). "Special report: The simulations driving the world's response to COVID-19". Nature. 580 (7803): 316–318. Bibcode:2020Natur.580..316A. doi:10.1038/d41586-020-01003-6. PMID 32242115. S2CID 214771531.
- ^ Squazzoni F, Polhill JG, Edmonds B, Ahrweiler P, Antosz P, Scholz G, et al. (2020). "Computational Models That Matter During a Global Pandemic Outbreak: A Call to Action". Journal of Artificial Societies and Social Simulation. 23 (2): 10. doi:10.18564/jasss.4298. hdl:10037/19057. ISSN 1460-7425. S2CID 216426533.
- ^ Sridhar D, Majumder MS (April 2020). "Modelling the pandemic". BMJ. 369: m1567. doi:10.1136/bmj.m1567. PMID 32317328. S2CID 216074714.
- ^ Maziarz M, Zach M (October 2020). "Agent-based modelling for SARS-CoV-2 epidemic prediction and intervention assessment: A methodological appraisal". Journal of Evaluation in Clinical Practice. 26 (5): 1352–1360. doi:10.1111/jep.13459. PMC 7461315. PMID 32820573.
- ^ Mayorga L, García Samartino C, Flores G, Masuelli S, Sánchez MV, Mayorga LS, et al. (2020). "A modelling study highlights the power of detecting and isolating asymptomatic or very mildly affected individuals for COVID-19 epidemic management". BMC Public Health. 20 (1): 1809. doi:10.1186/s12889-020-09843-7. PMC 7691976. PMID 33246432.
- ^ "Impact of non-pharmaceutical interventions (NPIs) to reduce COVID19 mortality and healthcare demand" (PDF). Imperial College COVID-19 Response Team. 2020-03-16.
- ^ a b Stephen C. Miller (2020-08-26). American Institute for Economic Research (ed.). "Lockdowns and Mask Mandates Do Not Lead to Reduced COVID Transmission Rates or Deaths, New Study Suggests". Retrieved 2020-09-11. With link to the complete NBER Working Paper, August 2020, there Figure 2, p. 18.
- ^ Andrew Atkeson, Karen Kopecky und Tao Zha: Four stylized facts about Covid-19. NBER Working Paper, August 2020, Introduction p. 2–4, Conclusion p. 15–16. Retrieved 2020-09-12.
- ^ "Mask-wearing cuts Covid incidence by 53%, says global study". The Guardian. 18 November 2021. Retrieved 18 November 2021.
- ^ Talic S, Shah S, Wild H, Gasevic D, Maharaj A, Ademi Z, et al. (18 November 2021). "Effectiveness of public health measures in reducing the incidence of covid-19, SARS-CoV-2 transmission, and covid-19 mortality: systematic review and meta-analysis". BMJ. 375: e068302. doi:10.1136/bmj-2021-068302. ISSN 1756-1833. PMC 9423125. PMID 34789505. S2CID 244271780.
- ^ "Expert interview: What is contact tracing?". Blog: Public Health Matters. Public Health England, Government of the United Kingdom. 13 February 2020. Retrieved 2020-02-28.
- ^ a b c Ingram D, Ward J (2020-04-07). "Behind the global efforts to make a privacy-first coronavirus tracking app". NBC News. Retrieved 2020-04-10.
- ^ "Too few Germans using coronavirus pandemic tracing app | DW | 17.09.2020". Deutsche Welle. Retrieved 8 April 2021.
- ^ "Vaccine passport apps are here. But the technical challenges are still coming". The Seattle Times. Retrieved 8 April 2021.
- ^ "96% of Canadians who test positive for coronavirus aren't using COVID Alert app properly". Global News. Retrieved 8 April 2021.
- ^ "Corona-Warn-App 2.0: Check-in per QR-Code startet nach Ostern". t3n Magazin (in German). 31 March 2021. Retrieved 8 April 2021.
- ^ Rowe F, Ngwenyama O, Richet JL (2 September 2020). "Contact-tracing apps and alienation in the age of COVID-19". European Journal of Information Systems. 29 (5): 545–562. doi:10.1080/0960085X.2020.1803155. hdl:10536/DRO/DU:30143215. ISSN 0960-085X. S2CID 224891520.
- ^ "Apple and Google are launching a joint COVID-19 tracing tool for iOS and Android". TechCrunch. Archived from the original on 2020-05-22. Retrieved 2020-04-10.
- ^ "Privacy-Preserving Contact Tracing". Apple. 2020-04-10.
- ^ "Apple and Google partner on COVID-19 contact tracing technology". 2020-04-10. Retrieved 2020-04-10.
- ^ "Palantir provides COVID-19 tracking software to CDC and NHS, pitches European health agencies". TechCrunch. Retrieved 2020-04-22.
- ^ "China launches coronavirus 'close contact' app". BBC News. 11 February 2020. Archived from the original on 28 February 2020. Retrieved 7 March 2020.
- ^ Chen A. "China's coronavirus app could have unintended consequences". MIT Technology Review. Retrieved 7 March 2020.
- ^ "Gov in the Time of Corona". GovInsider. 19 March 2020. Archived from the original on 20 March 2020. Retrieved 20 March 2020.
- ^ Manancourt V (10 March 2020). "Coronavirus tests Europe's resolve on privacy". POLITICO. Archived from the original on 20 March 2020. Retrieved 20 March 2020.
- ^ Tidy J (17 March 2020). "Coronavirus: Israel enables emergency spy powers". BBC News. Archived from the original on 18 March 2020. Retrieved 18 March 2020.
- ^ Bünte O (18 March 2020). "Corona-Krise: Deutsche Telekom liefert anonymisierte Handydaten an RKI" [Corona crisis: Deutsche Telekom delivers anonymized cell phone data to RKI]. Heise Online (in German). Archived from the original on 24 March 2020. Retrieved 25 March 2020.
- ^ "Moscow deploys facial recognition technology for coronavirus quarantine". Reuters. 21 February 2020. Archived from the original on 22 February 2020. Retrieved 20 March 2020.
- ^ "Italians scolded for flouting lockdown as death toll nears 3,000". Pittsburgh Post-Gazette. Archived from the original on 20 March 2020. Retrieved 20 March 2020.
- ^ "Kreative Lösungen gesucht". Startseite (in German). 18 March 2020. Archived from the original on 24 March 2020. Retrieved 23 March 2020.
- ^ Dannewitz J (23 March 2020). "Hackathon Germany: #WirvsVirus". Datenschutzbeauftragter (in German).
- ^ Staff (8 April 2020). "Lockdown is working, suggests latest data from symptom tracker app". King's College London News Centre. Retrieved 20 April 2020.
- ^ Lydall R (4 May 2020). "Three million download app to track coronavirus symptoms". Evening Standard. Retrieved 8 May 2020.
- ^ Whyte A (21 March 2020). "President makes global call to combat coronavirus via hackathon". ERR. Archived from the original on 24 March 2020. Retrieved 23 March 2020.
- ^ a b "Hospital readiness checklist for COVID-19". euro.who.int. 2020-03-25. Retrieved 2020-03-27.
- ^ Checklist for hospitals preparing for the reception and care of coronavirus 2019 (COVID-19) patients (Report). European Centre for Disease Prevention and Control. 2020-02-26. Retrieved 2020-03-27.
- ^ Smith AC, Thomas E, Snoswell CL, Haydon H, Mehrotra A, Clemensen J, et al. (June 2020). "Telehealth for global emergencies: Implications for coronavirus disease 2019 (COVID-19)". Journal of Telemedicine and Telecare. 26 (5): 309–313. doi:10.1177/1357633x20916567. PMC 7140977. PMID 32196391.
- ^ Ohannessian R, Duong TA, Odone A (April 2020). "Global Telemedicine Implementation and Integration Within Health Systems to Fight the COVID-19 Pandemic: A Call to Action". JMIR Public Health and Surveillance. 6 (2): e18810. doi:10.2196/18810. PMC 7124951. PMID 32238336.
- ^ Keshvardoost S, Bahaadinbeigy K, Fatehi F (July 2020). "Role of Telehealth in the Management of COVID-19: Lessons Learned from Previous SARS, MERS, and Ebola Outbreaks". Telemedicine Journal and e-Health. 26 (7): 850–852. doi:10.1089/tmj.2020.0105. PMID 32329659. S2CID 216111135.
- ^ "How safe is it to travel on public transport amid COVID-19?". News-Medical.net. 12 November 2021. Retrieved 15 November 2021.
- ^ Ku D, Yeon C, Lee S, Lee K, Hwang K, Li YC, et al. (2021). "Safe traveling in public transport amid COVID-19". Science Advances. 7 (43): eabg3691. Bibcode:2021SciA....7.3691K. doi:10.1126/sciadv.abg3691. PMC 8535823. PMID 34678065.
- ^ Layt S (14 April 2020). "Queensland researchers hit sweet spot with new mask material". Brisbane Times. Retrieved 17 May 2020.
- ^ QUT. "New mask material can remove virus-size nanoparticles". Queensland University of Technology. Retrieved 17 May 2020.
- ^ Leichman AK (28 January 2020). "New antiviral masks from Israel may help stop deadly coronavirus". Israel21c. Retrieved 17 May 2020.
- ^ "Israel to receive 120,000 coronavirus-repelling face masks". The Jerusalem Post | JPost.com. Retrieved 17 May 2020.
- ^ a b c d Karlin S (12 May 2020). "Scientists are racing to design a face mask that can rip coronavirus apart". Fast Company. Retrieved 17 May 2020.
- ^ Vavra C (18 April 2020). "Self-sanitizing face mask project for COVID-19 research receives NSF grant". Control Engineering. Retrieved 17 May 2020.
- ^ Lindsley WG, Derk RC, Coyle JP, Martin SB, Mead KR, Blachere FM, et al. (9 July 2021). "Efficacy of Portable Air Cleaners and Masking for Reducing Indoor Exposure to Simulated Exhaled SARS-CoV-2 Aerosols — United States, 2021". Morbidity and Mortality Weekly Report. 70 (27): 972–976. doi:10.15585/mmwr.mm7027e1. PMC 8312755. PMID 34237047.
- ^ He R(, Liu W(, Elson J, Vogt R, Maranville C, Hong J( (1 May 2021). "Airborne transmission of COVID-19 and mitigation using box fan air cleaners in a poorly ventilated classroom". Physics of Fluids. 33 (5): 057107. Bibcode:2021PhFl...33e7107H. doi:10.1063/5.0050058. ISSN 1070-6631. PMC 8142835. PMID 34040337.
- ^ "A chewing gum that could reduce SARS-CoV-2 transmission". University of Pennsylvania. Retrieved 13 December 2021.
- ^ Daniell H, Nair SK, Esmaeili N, Wakade G, Shahid N, Ganesan PK, et al. (10 November 2021). "Debulking SARS-CoV-2 in saliva using angiotensin converting enzyme 2 in chewing gum to decrease oral virus transmission and infection". Molecular Therapy. 30 (5): 1966–1978. doi:10.1016/j.ymthe.2021.11.008. ISSN 1525-0016. PMC 8580552. PMID 34774754.
- ^ Good A, Greicius T (2020-04-23). "NASA Develops COVID-19 Prototype Ventilator in 37 Days". NASA. Retrieved 2020-04-24.
- ^ Wall M (2020-04-24). "NASA engineers build new COVID-19 ventilator in 37 days". Space.com. Retrieved 2020-04-24.
- ^ Inclán B, Rydin M, Northon K, Good A (30 April 2020). "NASA-Developed Ventilator Authorized by FDA for Emergency Use". NASA. Retrieved 1 May 2020.
- ^ "VITAL. THE COVID-19 VENTILATOR DEVICE. Learn More About the Licensee". Jet Propulsion Laboratory. California Institute of Technology. Retrieved 2021-03-04.
- ^ "Indian tech cos join hands to make open source based oxygen concentrators; to be priced at around Rs 40k". The Economic Times. Retrieved 13 June 2021.
- ^ "Open Source Oxygen Concentrators Reference Designs | Three Examples". Electronics For You. 2021-05-11. Retrieved 13 June 2021.
- ^ Temple J. "How 3D printing could save lives in the coronavirus outbreak". MIT Technology Review. Retrieved 2020-04-05.
- ^ Tibken S. "3D printing may help supply more essential coronavirus medical gear". CNET. Retrieved 2020-04-05.
- ^ "[Updating] Italian hospital saves Covid-19 patients lives by 3D printing valves for reanimation devices". 3D Printing Media Network. 2020-03-14. Retrieved 2020-03-20.
- ^ Peters J (2020-03-17). "Volunteers produce 3D-printed valves for life-saving coronavirus treatments". The Verge. Retrieved 2020-03-20.
- ^ "Engineers 3D-print patented valves for free to save coronavirus patients in Italy". Global News.
- ^ a b Antia R, Halloran ME (October 2021). "Transition to endemicity: Understanding COVID-19". Immunity (Review). 54 (10): 2172–2176. doi:10.1016/j.immuni.2021.09.019. PMC 8461290. PMID 34626549.
- ^ a b Markov PV, Ghafari M, Beer M, Lythgoe K, Simmonds P, Stilianakis NI, et al. (June 2023). "The evolution of SARS-CoV-2". Nat Rev Microbiol (Review). 21 (6): 361–379. doi:10.1038/s41579-023-00878-2. PMID 37020110. S2CID 257983412.
In the absence of eradication, the virus will likely become endemic, a process that could take years to decades. We will be able to establish that endemic persistence has been reached if the virus shows repeatable patterns in prevalence year on year, for example, regular seasonal fluctuations and no out-of-season peaks. The form this endemic persistence will take remains to be determined, and the eventual infection prevalence and disease burden will depend on the rate of emergence of antigenically distinct lineages, our ability to roll out and update vaccines, and the future trajectory of virulence (Fig. 4c)....Meanwhile, focusing on the epidemiology of the pathogen, it is important to bear in mind that the transition from a pandemic to future endemic existence of SARS-CoV-2 is likely to be long and erratic, rather than a short and distinct switch, and that endemic SARS-CoV-2 is by far not a synonym for safe infections, mild COVID-19 or a low population mortality and morbidity burden.
- ^ Steere-Williams J (May 2022). "Endemic fatalism and why it will not resolve COVID-19". Public Health. 206: 29–30. doi:10.1016/j.puhe.2022.02.011. ISSN 0033-3506. PMC 8841151. PMID 35316742.
- ^ "WHO downgrades COVID-19 pandemic, says it's no longer a global emergency". CBC. Retrieved 29 July 2023.
- ^ Koelle K, Martin MA, Antia R, Lopman B, Dean NE (2022-03-11). "The changing epidemiology of SARS-CoV-2". Science. 375 (6585): 1116–1121. Bibcode:2022Sci...375.1116K. doi:10.1126/science.abm4915. ISSN 1095-9203. PMC 9009722. PMID 35271324.
- ^ Cohen LE, Spiro DJ, Viboud C (30 June 2022). "Projecting the SARS-CoV-2 transition from pandemicity to endemicity: Epidemiological and immunological considerations". PLOS Pathogens. 18 (6): e1010591. doi:10.1371/journal.ppat.1010591. ISSN 1553-7374. PMC 9246171. PMID 35771775.
