User:Jhd247/sandbox1
Background and Details of the Disaster[edit]
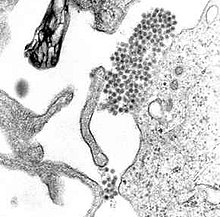
In 2017 Sri Lanka experienced its largest neglected tropical disease outbreak of dengue fever since the first recorded Sri Lankan case in 1962.[1][2][3] This biological hazard, transmitted via female mosquito bites, caused 186,101 dengue cases, significantly higher than in previous years (table 1), and 440 deaths.[4] [5] [6]
| Year | 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 | 2017 | 2018 | 2019 | 2020 | 2021 | 2022 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Annual Dengue Cases | 34,188 | 28,473 | 44,461 | 32,063 | 47,502 | 29,777 | 50,592 | 186,101 | 51,659 | 105,049 | 31,162 | 25,067 | 51,005 (Jan-Oct) |
Sri Lanka's Ministry of Health (MoH) reported a rise in cases from January, with the highest number of cases reported in July (table 2 & figure 1).[7] Most cases were recorded in the west and north of the country, specifically in the urban Colombo district (figure 2).[6]
| Month | Jan | Feb | Mar | Apr | May | Jun | Jul | Aug | Sep | Oct | Nov | Dev |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Reported Dengue Case Number | 10,927 | 8,724 | 13,540 | 12,510 | 15,963 | 25,319 | 41,121 | 22,270 | 9519 | 6614 | 8868 | 10,753 |
Causes[edit]
Climate[edit]
- Sri Lanka's tropical climate offers prime mosquito breeding conditions.[8]
- The 2017 monsoon rains (May-August) coincided with the peak of the dengue outbreak (table 2). Triggering floods and disrupting refuse collection, providing mosquito breedings sites.[3] [9]
- However, annual rainfall and El Nino conditions were lower on average than previous years, suggesting that climate was not completely responsible for the outbreak.[6]
Political[edit]
- MoH failed to prepare and take appropriate mosquito vector control.[2] [10]
- Insufficiencies in the virologic surveillance programme failed to identify dengue serotypes and genotypes.[3] [2] [11] Leaving Sri Lanka unprepared for new strains (DENV-2), for which their population would have little immunity.[6][11] [12]
Socio-economic[edit]
- Sri Lanka is a middle-income country with a GDP per capita of US $12,600 (2017).[13] This restricts investment in healthcare infrastructure resulting in an overstretched healthcare system.[3]
- High urban population density in western districts (figure 2) created higher probability of transmission.[6]
- In 2017, 42% of Sri Lankans were in extreme poverty (below US$5.50 a day) which limits a family's access to healthcare and increases risk of disease.[14] [15] [16]
- Regional disparities, due to the Sri Lankan civil conflict (1983-2009), displaced people to IDP camps and marginalised ethnic groups (Tamils) in north and eastern districts, reducing support and increasing disease risk.[17][18]
Short- and Long- term Impacts[edit]
Short-term Impacts[edit]
- Unexpected high death toll.[3]
- Significant disruption to workplaces, household income and education as the majority of cases were of people aged 10-29 (figure 3).[6]
- Direct and indirect impacts of the dengue outbreak affected 600,000 people, in all 25 districts, prominently in urban areas.[12] However, some districts may have been under-reported due to ethnic marginalisation and the presence of IDP camps.[19][17]
- Dengue treatment strained national economic resources costing Sri Lanka US $12.7 million (LKR 1.938 billion).[6]
Long-term Impacts[edit]
Today dengue cases are declining in Sri Lanka, with 25,067 total cases in 2021 (table 1).[7] Yet, as dengue is still present in Sri Lanka there are concerns for future outbreaks. Vulnerabilities include:
- New serotypes DENV-3 and DENV-4 are becoming more prominent in Sri Lanka, therefore threatening a new outbreak as population immunity has not developed.[11]
- The COVID-19 pandemic has placed immense pressures on healthcare and economic/trade systems reducing Sri Lanka's ability to prepare for future dengue outbreaks.[20]
- In 2022, Sri Lanka experienced a economic crisis which has triggered food insecurity issues.[21][22] This will increase food prices, reduce available nutritious food and potentially increase individuals risk of disease.[23]
Future[edit]
Climate change models suggest that Sri Lanka's climate is becoming more conducive to mosquito breeding, this combined with economic instability could trigger a future epidemic.[24][25] However, this could be mitigated if the MoH, supported by institutions like WHO, engage in proactive strategies.[26] At the cost of US$78 per person a licensed vaccine is now available Dengvaxia® (CYD-TDV) with five more in development.[26] However, Sri Lanka's current expenditure is US$161 per capita on healthcare (2021), the vaccine is a significant proportion of that budget and in uncertain economic times may not be a priority.[27]
National and International Responses[edit]
National Responses[edit]
Pre-outbreak the MoH did engage in routine preventative strategies including premise inspections, removal of mosquito breeding sites, health education, and purchases of fogging machines.[6] However, the flooding in 2017 meant that these strategies were not sufficient.[3] Criticism has also been levied against Sri Lanka’s limited virologic surveillance programme which failed to monitor dengue serotypes and failure to invest in health infrastructure contributing to the high death toll.[6]

During the 2017 outbreak, additional three emergency wards were built 38km north of Colombo.[12] The military conducted house-to-house visits and formed vector control brigades aiming to remove mosquito breeding sites using Bacillus Thuringiensis Israelensis (Bti) spray.[10] This was supported further by fining landowners who failed to respond to removal instructions.[12] Additional funds were also made available for public health staff to take on extra hours during the outbreak months.[6] Several, issues occurred at this time, including failure to provide adequate health care in rural and remote areas, poor data collection outside of Colombo and western districts, and the use of the ineffective Bti spray which failed to have an impact on vector control.[6][12][10]
International Responses[edit]

In 2017, the Sri Lankan MoH received international support from the World Health Organisation (WHO), the Regional Office for South-East Asia (SEARO), and NGOs such as the Red Cross.[12] These international organisations assisted by providing practical supplies such as hospital beds and 50 fogging machines.[12] Personnel and expertise were also given through the provision of an epidemiologist, an entomologist and two dengue management experts from the WHO Collaborating Centre to assist with planning and control. [12] Multi-lateral aid was also provided through WHO, from donors such as Australia which contributed US $500,000.[28] In total, the World Bank states that Sri Lanka received US $316,170,013 in aid during the year of 2017, yet there is little information on what this humanitarian aid was used for, whether it reached those on the ground, and if it was appropriate.[29][30]
References[edit]
- ^ "CDC - Neglected Tropical Diseases - Diseases". www.cdc.gov. 2022-03-07. Retrieved 2022-10-27.
- ^ a b c Ngwe Tun, Mya Myat; Muthugala, Rohitha; Nabeshima, Takeshi; Rajamanthri, Lakmali; Jayawardana, Dulani; Attanayake, Shanthi; Soe, Aung Min; Dumre, Shyam Prakash; Ando, Tsuyoshi; Hayasaka, Daisuke; Inoue, Shingo; Buerano, Corazon C.; Morita, Kouichi (2020-04). "Unusual, neurological and severe dengue manifestations during the outbreak in Sri Lanka, 2017". Journal of Clinical Virology. 125: 104304. doi:10.1016/j.jcv.2020.104304.
{{cite journal}}: Check date values in:|date=(help) - ^ a b c d e f Ali, Shahid; Khan, Abdul Waheed; Taylor-Robinson, Andrew W.; Adnan, Muhammad; Malik, Shahana; Gul, Saba (2018-06). "The unprecedented magnitude of the 2017 dengue outbreak in Sri Lanka provides lessons for future mosquito-borne infection control and prevention". Infection, Disease & Health. 23 (2): 114–120. doi:10.1016/j.idh.2018.02.004.
{{cite journal}}: Check date values in:|date=(help) - ^ "What is a disaster? | IFRC". www.ifrc.org. Retrieved 2022-10-27.
- ^ Stanaway, Jeffrey D; Shepard, Donald S; Undurraga, Eduardo A; Halasa, Yara A; Coffeng, Luc E; Brady, Oliver J; Hay, Simon I; Bedi, Neeraj; Bensenor, Isabela M; Castañeda-Orjuela, Carlos A; Chuang, Ting-Wu; Gibney, Katherine B; Memish, Ziad A; Rafay, Anwar; Ukwaja, Kingsley N (2016-06). "The global burden of dengue: an analysis from the Global Burden of Disease Study 2013". The Lancet Infectious Diseases. 16 (6): 712–723. doi:10.1016/S1473-3099(16)00026-8. PMC 5012511. PMID 26874619.
{{cite journal}}: Check date values in:|date=(help)CS1 maint: PMC format (link) - ^ a b c d e f g h i j k Tissera, Hasitha A.; Jayamanne, Bernard D.W.; Raut, Rajendra; Janaki, Sakunthala M.D.; Tozan, Yesim; Samaraweera, Preshila C.; Liyanage, Prasad; Ghouse, Azhar; Rodrigo, Chaturaka; de Silva, Aravinda M.; Fernando, Sumadhya D. (2020-04). "Severe Dengue Epidemic, Sri Lanka, 2017". Emerging Infectious Diseases. 26 (4): 682–691. doi:10.3201/eid2604.190435. ISSN 1080-6040. PMC 7101108. PMID 32186490.
{{cite journal}}: Check date values in:|date=(help)CS1 maint: PMC format (link) - ^ a b c d Sri Lanka Ministry of Health (2022). "Trends". www.epid.gov.lk. Retrieved 2022-10-27.
- ^ WHO (2022). "Dengue and severe dengue". www.who.int. Retrieved 2022-10-27.
- ^ Guha-Sapir, Debarati; van Panhuis, Willem Gijsbert (2009-12). "Health Impact of the 2004 Andaman Nicobar Earthquake and Tsunami in Indonesia". Prehospital and Disaster Medicine. 24 (6): 493–499. doi:10.1017/S1049023X00007391. ISSN 1049-023X.
{{cite journal}}: Check date values in:|date=(help) - ^ a b c Tissera, H. A.; Samaraweera, P. C.; Jayamanne, B. D. W.; Janaki, M. D. S.; U Chulasiri, M. P. P.; Rodrigo, C.; Fernando, S. D. (2018-02). "Use of Bacillus thuringiensis israelensis in integrated vector control of Aedes sp. in Sri Lanka: a prospective controlled effectiveness study". Tropical Medicine & International Health. 23 (2): 229–235. doi:10.1111/tmi.13015.
{{cite journal}}: Check date values in:|date=(help) - ^ a b c Ngwe Tun, Mya Myat; Muthugala, Rohitha; Rajamanthri, Lakmali; Nabeshima, Takeshi; Buerano, Corazon C.; Morita, Kouichi (2021-09-30). "Emergence of Genotype I of Dengue Virus Serotype 3 during a Severe Dengue Epidemic in Sri Lanka in 2017". Japanese Journal of Infectious Diseases. 74 (5): 443–449. doi:10.7883/yoken.JJID.2020.854. ISSN 1344-6304.
- ^ a b c d e f g h WHO. "Dengue fever – Sri Lanka". www.who.int. Retrieved 2022-10-27.
- ^ "Gapminder Tools". www.gapminder.org. Retrieved 2022-10-28.
- ^ "Gapminder Tools". www.gapminder.org. Retrieved 2022-10-28.
- ^ "World Bank and WHO: Half the world lacks access to essential health services, 100 million still pushed into extreme poverty because of health expenses". www.who.int. Retrieved 2022-10-28.
- ^ "Noncommunicable diseases Sri Lanka 2018 country profile". www.who.int. Retrieved 2022-10-28.
- ^ a b "Sri Lanka - World Directory of Minorities & Indigenous Peoples". Minority Rights Group. 2019-06-19. Retrieved 2022-10-27.
- ^ "Healthcare in Conflict Settings". World Innovation Summit for Health. Retrieved 2022-10-27.
- ^ Schratz, Alexander (2010). Important Helminth Infections in Southeast Asia : Diversity and Potential for Control and Elimination. Part A. Xiao-nong Zhou (First edition ed.). London. ISBN 978-0-12-381956-7. OCLC 689053662.
{{cite book}}:|edition=has extra text (help)CS1 maint: location missing publisher (link) - ^ "Vaccines and immunization: Dengue". www.who.int. Retrieved 2022-10-27.
- ^ Root and Win (2022-08-09). "How Sri Lanka went from topping Lonely Planet's list to almost 30% hunger levels". The New Humanitarian. Retrieved 2022-10-27.
- ^ Quiggin, John; Mallawaarachchi, Thilak. "How did Sri Lanka run out of money? 5 graphs that explain its economic crisis". The Conversation. Retrieved 2022-10-27.
- ^ Yngve, Agneta; Margetts, Barrie; Hughes, Roger; Tseng, Marilyn (2009-11). "Food insecurity – not just about rural communities in Africa and Asia". Public Health Nutrition. 12 (11): 1971–1972. doi:10.1017/S1368980009991650. ISSN 1475-2727.
{{cite journal}}: Check date values in:|date=(help) - ^ Quiggin, John; Mallawaarachchi, Thilak. "How did Sri Lanka run out of money? 5 graphs that explain its economic crisis". The Conversation. Retrieved 2022-10-28.
- ^ Bhatia, Surbhi; Bansal, Dhruvisha; Patil, Seema; Pandya, Sharnil; Ilyas, Qazi Mudassar; Imran, Sajida (2022). "A Retrospective Study of Climate Change Affecting Dengue: Evidences, Challenges and Future Directions". Frontiers in Public Health. 10. doi:10.3389/fpubh.2022.884645. ISSN 2296-2565. PMC 9197220. PMID 35712272.
{{cite journal}}: CS1 maint: PMC format (link) CS1 maint: unflagged free DOI (link) - ^ a b WHO (2022). "Vaccines and immunization: Dengue". www.who.int. Retrieved 2022-10-28.
- ^ "Current health expenditure (% of GDP) - Sri Lanka | Data". data.worldbank.org. Retrieved 2022-10-28.
- ^ Relief Web (2017). "Australian assistance to combat dengue in Sri Lanka - Sri Lanka | ReliefWeb". reliefweb.int. Retrieved 2022-10-27.
- ^ The World Bank. "Net official development assistance and official aid received (current US$) - Sri Lanka | Data". data.worldbank.org. Retrieved 2022-10-27.
- ^ Spiegel, Paul B. (2021-03). "Will this pandemic be the catalyst to finally reform humanitarian responses?". Nature Medicine. 27 (3): 365–365. doi:10.1038/s41591-021-01249-1. ISSN 1078-8956.
{{cite journal}}: Check date values in:|date=(help)

