Brain metastasis
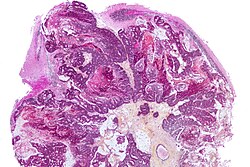
A brain metastasis is a cancer that has metastasized (spread) to the brain from another location in the body and is therefore considered a secondary brain tumor.[1][2] The metastasis typically shares a cancer cell type with the original site of the cancer.[3] Metastasis is the most common cause of brain cancer, as primary tumors that originate in the brain are less common.[4] The most common sites of primary cancer which metastasize to the brain are lung, breast, colon, kidney, and skin cancer. Brain metastases can occur months or even years after the original or primary cancer is treated. Brain metastases have a poor prognosis for cure, but modern treatments allow patients to live months and sometimes years after the diagnosis.[5]
Symptoms and signs[edit]
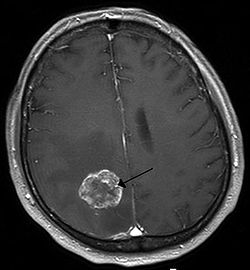
Because different parts of the brain are responsible for different functions, symptoms vary depending on the site of metastasis within the brain. However, brain metastases should be considered in any cancer patient who presents with neurological or behavioral changes.[6]
Brain metastases can cause a wide variety of symptoms which can also be present in minor, more common conditions. Neurological symptoms are often caused by increased intracranial pressure,[7] with severe cases resulting in coma.[8] The most common neurological symptoms include:
- New onset headaches: headaches occur in roughly half of brain metastasis patients, especially in those with many tumors.[6]
- Paresthesias: patients often present with (hemiparesis), or weakness on only one side of the body, which is often a result of damage to neighboring brain tissue.[7]
- Ataxia: when metastasis occurs to the cerebellum, patients will experience various difficulties with spatial awareness and coordination.[9]
- Seizures: when present, often indicates disease involvement of the cerebral cortex.[10]
Causes[edit]
The most common sources of brain metastases in a case series of 2,700 patients undergoing treatment at the Memorial Sloan–Kettering Cancer Center were:[11]
- Lung cancer, 48%
- Breast cancer, 15%
- Genitourinary tract cancers, 11%
- Osteosarcoma, 10%
- Melanoma, 9%
- Head and neck cancer, 6%
- Neuroblastoma, 5%
- Gastrointestinal cancers, especially colorectal and pancreatic carcinoma, 3%
- Lymphoma, 1%
Lung cancer and melanoma are most likely to present with multiple metastasis, whereas breast, colon, and renal cancers are more likely to present with a single metastasis.[3]
Diagnosis[edit]

Brain imaging (neuroimaging such as CT or MRI) is needed to determine the presence of brain metastases.[6] In particular, contrast-enhanced MRI is the best method of diagnosing brain metastases, although primary detection may be done using CT.[10] Biopsy is often recommended to confirm diagnosis.[6]
The diagnosis of brain metastases typically follows a diagnosis of a primary cancer.[10] Occasionally, brain metastases will be diagnosed concurrently with a primary tumor or before the primary tumor is found.
In the setting of brain metastasis due to malignant melanoma, MRI imaging showed high T1 and low T2 intensity due to the deposition of melanin in the brain. In susceptibility weighted imaging (SWI), it usually shows abnormal SWI hypointensity in larger proportion than brain metastasis caused by breast carcinoma.[12]
Treatment[edit]
Treatment for brain metastases is primarily palliative, with the goals of therapy being reduction of symptoms and prolongation of life. However, brain metastases harboring a mutation in the BRAF kinase at position V600 are effectively druggable with small molecule inhibitors such as dabrafenib. Unfortunately, drug resistance is observed within 4-6 months after treatment.[13] Recently, expression of NGFR was associated with progressive intracranial disease in melanoma patients [14] Additionally, there is limited evidence that the treatments that are offered takes account of patient-focused comparative effectiveness.[1] However, in some patients, particularly younger, healthier patients, aggressive therapy consisting of open craniotomy with maximal excision, chemotherapy, and radiosurgical intervention (Gamma Knife therapy) may be attempted.[1]
Symptomatic care[edit]
Symptomatic care should be given to all patients with brain metastases, as they often cause severe, debilitating symptoms. Treatment consists mainly of:
- Corticosteroids – Corticosteroid therapy is essential for all patients with brain metastases, as it prevents development of cerebral edema, as well as treating other neurological symptoms such as headaches, cognitive dysfunction, and emesis. Dexamethasone is the corticosteroid of choice.[10] Although neurological symptoms may improve within 24 to 72 hours of starting corticosteroids, cerebral edema may not improve for up to a week.[15] In addition, patients may experience adverse side effects from these drugs, such as myopathy and opportunistic infections, which can be alleviated by decreasing the dose.[15]
- Anticonvulsants – Anticonvulsants should be used for patients with brain metastases who experience seizures, as there is a risk of status epilepticus and death.[16] Newer generation anticonvulsants including Lamotrigine and Topiramate are recommended due to their relatively limited side effects.[16] It is not recommended to prophylactically give anti-seizure medications when a seizure has not yet been experienced by a patient with brain metastasis.[16]
Radiotherapy[edit]
Radiotherapy plays a critical role in the treatment of brain metastases, and includes whole-brain irradiation, fractionated radiotherapy, and radiosurgery.[6] Whole-brain irradiation is used as a primary treatment method in patients with multiple lesions and is also used alongside surgical resection when patients have single and accessible tumors.[6] However, it often causes severe side effects, including radiation necrosis, dementia, toxic leukoencephalopathy, partial to complete hair loss, nausea, headaches, and otitis media.[17] In children this treatment may cause intellectual impairment, psychiatric disturbances, and other neuropsychiatric effects.[18] Results from a 2021 systematic review on radiation therapy for brain metastases found that despite much research on radiation therapy, there is little evidence to inform comparative effectiveness and such patient-centered outcomes as quality of life, functional status, or cognitive effects.[1] In addition, whole-brain irradiation in combination with surgery showed no effect on overall survival when compared to whole-brain irradiation alone as demonstrated by a systematic review by the Agency for Healthcare Research and Quality.[1]
Surgery[edit]
Brain metastases are often managed surgically if they are accessible. Surgical resection followed by stereotactic radiosurgery or whole-brain irradiation deliver superior survival compared to whole brain irradiation alone.[6] Therefore, in patients with only one metastatic brain lesion and controlled or limited systemic disease, a life expectancy of at least 3 months with maintenance of performance status might be expected.[19]
Chemotherapy[edit]
Chemotherapy is rarely used for the treatment of brain metastases, as chemotherapeutic agents penetrate the blood brain barrier poorly.[2] However, some cancers such as lymphomas, small cell lung carcinomas (SCLC) and breast cancer may be highly chemosensitive and chemotherapy may be used to treat extracranial sites of metastatic disease in these cancers.[2] The effectiveness and safety of using chemotherapy to treat a brain metastasis that came from a SCLC is not clear.[20] An experimental treatment for brain metastases is intrathecal chemotherapy, a technique in which a chemotherapeutic drug is delivered via intralumbar injection into the cerebrospinal fluid.[21] Current research on the treatment of brain metastases includes creating new drug molecules to effectively target the blood-brain barrier and studying the relationship between tumors and various genes.[22] In 2015, the United States FDA approved Alecensa (alectinib) for use in patients with a specific type of non-small cell lung cancer (NSCLC; ALK-positive), a type of cancer which often metastasizes to the brain, whose condition worsened after use or were unable to take another medication, Xalkori (crizotinib).[23]
Immunotherapy[edit]
Immunotherapy, for instance Anti-PD-1 alone or in combination with anti-CTLA-4, appears to be effective in some patients with brain metastases especially when these are asymptomatic, stable and not previously treated.[24] In 2022, OMICs-based approaches such as single-cell and bulk RNA-sequencing revealed molecular subgroups in melanoma brain metastases (MBM) that may explain the variable response of MBM to therapeutic interventions.[25][26]Moreover, methylome and transcriptome profiling of MBM revealed immune cell and microglia-enriched tumor subsets showing favorable outcome.[27]
Prognosis[edit]
The prognosis for brain metastases is variable; it depends on the type of primary cancer, the age of the patient, the absence or presence of extracranial metastases, and the number of metastatic sites in the brain.[6] For patients who do not undergo treatment the average survival is between one and two months.[6] However, in some patients, such as those with no extracranial metastases, those who are younger than 65, and those with a single site of metastasis in the brain only, prognosis is much better, with median survival rates of up to 13.5 months.[2] Because brain metastasis can originate from various different primary cancers, the Karnofsky performance score is used for a more specific prognosis.[6]
Epidemiology[edit]
It is estimated that the worldwide incidence rate for brain metastases lies around 9% to 17%, based on the region of diagnosis.[28][29] However, the baseline incidence rate of brain metastases were found to increase with improvements to brain imaging technology.[30] Approximately 5-11% of brain metastasis were found to be deadly at 30 days, and 14 - 23% were found to be deadly at three months.[31]
More cases of brain metastases were found in adults, compared to children.[32] 67% to 80% of all cancer patients were found to develop brain metastases, as of 2012. Lung cancer, breast cancer and melanoma patients were found to be at the highest risk of developing brain metastases.[33][34][35][36][37] However, recent trends in brain metastasis epidemiology have shown an increase in incidence for patients with renal, colorectal, or ovarian cancers.[38] Brain metastases are most commonly diagnosed within multiple intracranial areas within the context of extracranial diseases.
Both population studies and autopsy studies have historically been used to calculate the incidence of brain metastases. However, many researchers have stated that population studies may express inaccurate data for brain metastases, given that surgeons have, in the past, been hesitant to take in patients with the condition. As a result, population studies regarding brain metastases have historically been inaccurate and incomplete.[39][40]
Advances in systemic treatments of brain metastases, such as radiosurgery, whole-brain radiotherapy and surgical resection has led to an increase in median survival rate of brain metastases patients.[41]
See also[edit]
References[edit]
- ^ a b c d e Garsa A, Jang JK, Baxi S, Chen C, Akinniranye O, Hall O, Larkin J, Motala A, Hempel S (2021). "Radiation Therapy for Brain Metastases: A Systematic Review". Pract Radiat Oncol. 11 (5): 354–365. doi:10.1016/j.prro.2021.04.002. PMID 34119447. S2CID 236256085.
- ^ a b c d Tse V (10 November 2009). "Brain Metastasis". Medscape. Retrieved 13 January 2010.
- ^ a b "Metastatic Brain Tumors" (PDF). Archived from the original (PDF) on 29 August 2017. Retrieved 13 August 2017.
- ^ "Tumor Types - National Brain Tumor Society". National Brain Tumor Society. Retrieved 1 August 2017.[permanent dead link]
- ^ "Radiation Therapy for Brain Metastases: What are brain metastases?". Archived from the original on 2010-04-06. Retrieved 2010-03-17.
- ^ a b c d e f g h i j Loeffler JS. Wen PY, Eichler AF (eds.). "Epidemiology, clinical manifestations, and diagnosis of brain metastases". UpToDate. Retrieved 2 August 2017.
- ^ a b Sawaya R (September 2001). "Considerations in the diagnosis and management of brain metastases". Oncology. 15 (9). Williston Park, N.Y.: 1144–54, 1157–8, discussion 1158, 1163–5. PMID 11589063. Archived from the original on 2022-10-04. Retrieved 2017-08-13.
- ^ "Metastatic Brain Tumors". American Association of Neurological Surgeons. Retrieved 3 August 2017.
- ^ "Metastatic Brain Tumors". Memorial Sloan Kettering Cancer Center. Retrieved 3 August 2017.
- ^ a b c d Wen PY, Loeffler JS (July 1999). "Management of brain metastases". Oncology. 13 (7). Williston Park, N.Y.: 941–54, 957–61, discussion 961–2, 9. PMID 10442342.
- ^ Ts V (10 November 2009). "Brain Metastasis - Morbidity/Mortality". Medscape. Retrieved 13 January 2010.
- ^ Pope WB (2018). "Brain metastases: neuroimaging". Metastatic Disease of the Nervous System. Handbook of Clinical Neurology. Vol. 149. Elsevier. pp. 89–112. doi:10.1016/b978-0-12-811161-1.00007-4. ISBN 978-0-12-811161-1. PMC 6118134. PMID 29307364.
- ^ Redmer T (July 2018). "Deciphering mechanisms of brain metastasis in melanoma - the gist of the matter". Molecular Cancer. 17 (1): 106. doi:10.1186/s12943-018-0854-5. PMC 6064184. PMID 30053879.
- ^ Radke J, Schumann E, Onken J, Koll R, Acker G, Bodnar B, et al. (November 2022). "Decoding molecular programs in melanoma brain metastases". Nature Communications. 13 (1): 7304. Bibcode:2022NatCo..13.7304R. doi:10.1038/s41467-022-34899-x. PMC 9701224. PMID 36435874.
- ^ a b Drappatz J. Wen PY, Eichler AF (eds.). "Management of Vasogenic Edema in Patients with Primary and Metastatic Brain Tumors". UpToDate. Retrieved 2 August 2017.
- ^ a b c Drappatz J. Avila EK, Schachter SC, Wen PY, Dashe JF (eds.). "Seizures in Patients with Primary and Metastatic Brain Tumors". UpToDate. Retrieved 2 August 2017.
- ^ Loeffler JS. Wen PY, Eichler AF (eds.). "Overview of the Treatment of Brain Metastases". UpToDate. Retrieved 2 August 2017.
- ^ "What are the real benefits versus risks of preventative brain radiation for patients with non-small cell lung cancer?" (PDF). Archived from the original (PDF) on 2010-06-13. Retrieved 2010-03-17.
- ^ "IIS7". Archived from the original on 2010-01-29. Retrieved 2010-01-16.
- ^ Reveiz L, Rueda JR, Cardona AF (June 2012). "Chemotherapy for brain metastases from small cell lung cancer". The Cochrane Database of Systematic Reviews (6): CD007464. doi:10.1002/14651858.CD007464.pub2. PMID 22696370.
- ^ "Definition of intrathecal chemotherapy". 2011-02-02. Retrieved 2017-08-13.
- ^ El-Habashy SE, Nazief AM, Adkins CE, Wen MM, El-Kamel AH, Hamdan AM, Hanafy AS, Terrell TO, Mohammad AS, Lockman PR, Nounou MI (May 2014). "Novel treatment strategies for brain tumors and metastases". Pharmaceutical Patent Analyst. 3 (3): 279–96. doi:10.4155/ppa.14.19. PMC 4465202. PMID 24998288.
- ^ "FDA approves new oral therapy to treat ALK-positive lung cancer". FDA. 11 December 2015. Retrieved 4 August 2017.
- ^ Caponnetto S, Draghi A, Borch TH, Nuti M, Cortesi E, Svane IM, Donia M (May 2018). "Cancer immunotherapy in patients with brain metastases". Cancer Immunology, Immunotherapy. 67 (5): 703–711. doi:10.1007/s00262-018-2146-8. hdl:11573/1298742. PMID 29520474. S2CID 3782427.
- ^ Biermann, Jana; et al. (2022). "Dissecting the treatment-naive ecosystem of human melanoma brain metastasis". Cell. 185 (14): 2591–2608.e30. doi:10.1016/j.cell.2022.06.007. PMC 9677434. PMID 35803246. S2CID 250343194.
- ^ Radke, Josefine; Schumann, Elisa; Onken, Julia; Koll, Randi; Acker, Güliz; Bodnar, Bohdan; Senger, Carolin; Tierling, Sascha; Möbs, Markus; Vajkoczy, Peter; Vidal, Anna; Högler, Sandra; Kodajova, Petra; Westphal, Dana; Meier, Friedegund; Heppner, Frank; Kreuzer-Redmer, Susanne; Grebien, Florian; Jürchott, Karsten; Redmer, Torben (2022). "Decoding molecular programs in melanoma brain metastases". Nature Communications. 13 (1): 7304. Bibcode:2022NatCo..13.7304R. doi:10.1038/s41467-022-34899-x. PMC 9701224. PMID 36435874.
- ^ Redmer, Torben; Schumann, Elisa; Peters, Kristin; Weidemeier, Martin E.; Nowak, Stephan; Schroeder, Henry W. S.; Vidal, Anna; Radbruch, Helena; Lehmann, Annika; Kreuzer-Redmer, Susanne; Jürchott, Karsten; Radke, Josefine (2024). "MET receptor serves as a promising target in melanoma brain metastases". Acta Neuropathologica. 147 (1): 44. doi:10.1007/s00401-024-02694-1. PMC 10884227. PMID 38386085.
- ^ Park DM, Posner JB, "Management of Intracranial Metastases: History", Intracranial Metastases, Blackwell Publishing, Inc., pp. 1–19, ISBN 9780470753064
- ^ Kintomo T (1982). Metastatic tumors of the central nervous system. Igaku-Shoin. ISBN 978-0896400672. OCLC 805657369.
- ^ Barnholtz-Sloan JS, Sloan AE, Davis FG, Vigneau FD, Lai P, Sawaya RE (July 2004). "Incidence proportions of brain metastases in patients diagnosed (1973 to 2001) in the Metropolitan Detroit Cancer Surveillance System". Journal of Clinical Oncology. 22 (14): 2865–72. doi:10.1200/jco.2004.12.149. PMID 15254054.
- ^ Stelzer KJ (2013-05-02). "Epidemiology and prognosis of brain metastases". Surgical Neurology International. 4 (Suppl 4): S192-202. doi:10.4103/2152-7806.111296. PMC 3656565. PMID 23717790.
- ^ Bouffet E, Doumi N, Thiesse P, Mottolese C, Jouvet A, Lacroze M, Carrie C, Frappaz D, Brunat-Mentigny M (January 1997). "Brain metastases in children with solid tumors". Cancer. 79 (2): 403–10. doi:10.1002/(SICI)1097-0142(19970115)79:2<403::AID-CNCR25>3.0.CO;2-3. PMID 9010115.
- ^ Counsell CE, Collie DA, Grant R (August 1996). "Incidence of intracranial tumours in the Lothian region of Scotland, 1989-90". Journal of Neurology, Neurosurgery, and Psychiatry. 61 (2): 143–50. doi:10.1136/jnnp.61.2.143. PMC 1073987. PMID 8708681.
- ^ Fabi A, Felici A, Metro G, Mirri A, Bria E, Telera S, Moscetti L, Russillo M, Lanzetta G, Mansueto G, Pace A, Maschio M, Vidiri A, Sperduti I, Cognetti F, Carapella CM (January 2011). "Brain metastases from solid tumors: disease outcome according to type of treatment and therapeutic resources of the treating center". Journal of Experimental & Clinical Cancer Research. 30 (1): 10. doi:10.1186/1756-9966-30-10. PMC 3033846. PMID 21244695.
- ^ Stark AM, Stöhring C, Hedderich J, Held-Feindt J, Mehdorn HM (January 2011). "Surgical treatment for brain metastases: Prognostic factors and survival in 309 patients with regard to patient age". Journal of Clinical Neuroscience. 18 (1): 34–8. doi:10.1016/j.jocn.2010.03.046. PMID 20851611. S2CID 19575548.
- ^ Lagerwaard FJ, Levendag PC, Nowak PJ, Eijkenboom WM, Hanssens PE, Schmitz PI (March 1999). "Identification of prognostic factors in patients with brain metastases: a review of 1292 patients". International Journal of Radiation Oncology, Biology, Physics. 43 (4): 795–803. doi:10.1016/S0360-3016(98)00442-8. PMID 10098435.
- ^ Graf AH, Buchberger W, Langmayr H, Schmid KW (1988). "Site preference of metastatic tumours of the brain". Virchows Archiv A. 412 (5): 493–8. doi:10.1007/BF00750584. PMID 3128919. S2CID 23306094.
- ^ Barnholtz-Sloan JS, Sloan AE, Davis FG, Vigneau FD, Lai P, Sawaya RE (July 2004). "Incidence proportions of brain metastases in patients diagnosed (1973 to 2001) in the Metropolitan Detroit Cancer Surveillance System". Journal of Clinical Oncology. 22 (14): 2865–72. doi:10.1200/JCO.2004.12.149. PMID 15254054.
- ^ Percy AK, Elveback LR, Okazaki H, Kurland LT (January 1972). "Neoplasms of the central nervous system. Epidemiologic considerations". Neurology. 22 (1): 40–8. doi:10.1212/WNL.22.1.40. PMID 5061838. S2CID 20786479.
- ^ Walker AE, Robins M, Weinfeld FD (February 1985). "Epidemiology of brain tumors: the national survey of intracranial neoplasms". Neurology. 35 (2): 219–26. doi:10.1212/WNL.35.2.219. PMID 3969210. S2CID 43324791.
- ^ Tabouret E, Metellus P, Gonçalves A, Esterni B, Charaffe-Jauffret E, Viens P, Tallet A (March 2014). "Assessment of prognostic scores in brain metastases from breast cancer". Neuro-Oncology. 16 (3): 421–8. doi:10.1093/neuonc/not200. PMC 3922513. PMID 24311640.
