Dupilumab
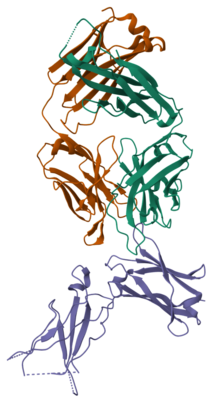 Dupilumab antigen binding fragment (orange and green) bound to a human IL-4 receptor alpha (purple) | |
| Monoclonal antibody | |
|---|---|
| Type | Whole antibody |
| Source | Human |
| Target | Interleukin 4 (IL4) receptor alpha |
| Clinical data | |
| Pronunciation | /duˈpɪljumæb/ doo-PIL-yoo-mab |
| Trade names | Dupixent |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a617021 |
| License data | |
| Pregnancy category |
|
| Routes of administration | Subcutaneous |
| ATC code | |
| Legal status | |
| Legal status | |
| Identifiers | |
| CAS Number | |
| DrugBank | |
| ChemSpider |
|
| UNII | |
| KEGG | |
| Chemical and physical data | |
| Formula | C6512H10066N1730O2052S46 |
| Molar mass | 146898.98 g·mol−1 |
Dupilumab, sold under the brand name Dupixent, is a monoclonal antibody blocking interleukin 4 and interleukin 13, used for allergic diseases such as atopic dermatitis (eczema), asthma and nasal polyps which result in chronic sinusitis.[6][7][8][4] It is also used for the treatment of eosinophilic esophagitis[9] and prurigo nodularis.[10]
The most common side effects reported by the US Food and Drug Administration (FDA) include injection site reactions, upper respiratory tract infections, joint pain, and herpes viral infections.[9] The most common side effects reported by the European Medicines Agency (EMA) include injection-site reactions (such as redness, swelling including due to fluid build-up, itching and pain), conjunctivitis (redness and discomfort in the eye) including conjunctivitis due to allergy, joint pain, cold sores, and increased blood levels of a type of white blood cell called eosinophils.[5] It was developed by Regeneron Pharmaceuticals and Sanofi Genzyme.[11][12] It received approval from the US Food and Drug Administration (FDA) for moderate-to-severe atopic dermatitis in 2017,[7] and for asthma in 2018.[4] The FDA considers it to be a first-in-class medication.[13]
Dupilumab is the first treatment for eosinophilic esophagitis approved by the U.S. Food and Drug Administration (FDA).[9] Eosinophilic esophagitis is a chronic inflammatory disorder in which eosinophils, a type of white blood cell, are found in the tissue of the esophagus.[9] In adults and adolescents with eosinophilic esophagitis, common symptoms include difficulty swallowing, difficulty eating, and food getting stuck in the esophagus.[9] Dupilumab is a monoclonal antibody that acts to inhibit part of the inflammatory pathway.[9] Dupilumab is the first treatment for prurigo nodularis approved by the FDA.[10] Prurigo nodularis is a rare skin disease that causes hard, itchy lumps (nodules) to form on the skin.[10]
Medical uses[edit]

Dupilumab is indicated for the treatment of moderate-to-severe atopic dermatitis, moderate-to-severe asthma, and for the treatment of chronic rhinosinusitis with nasal polyps (CRSwNP).[4][5][14][15][9] It has been shown to be effective at treating aspirin-exacerbated respiratory disease (AERD), a typically difficult to treat condition where aspirin intolerant patients have both CRSwNP and asthma.[16][17]
In May 2022, the indication for dupilumab was updated to include the treatment of eosinophilic esophagitis in people aged twelve years of age and older weighing at least 40 kilograms (88 lb).[9]
In September 2022, the indication for dupilumab was updated to include the treatment of adults with prurigo nodularis (PN).[10]
In March 2023, the EMA approved dupilumab for the treatment of severe atopic dermatitis in children aged six months to five years who are candidates for systemic therapy.[18][19]
Investigational uses[edit]
In March of 2023, Sanofi announced the results of a Phase 3 trial examining the efficacy of dupilumab in the treatment of chronic obstructive pulmonary disease (COPD). In this randomized, double-blind, placebo-controlled trial,[20] dupilumab demonstrated a 30% reduction in moderate or severe acute exacerbations of COPD, as well as significant improvements in lung function and quality of life in people with COPD.[21]
Side effects[edit]
Injection site reactions such as redness and pain are common, occurring in approximately 11.4% of cases.[22] Dupilumab can cause allergic reactions, conjunctivitis, and keratitis and, due to its immunosuppressive effects, reactivation of cold sores.[7] In clinical trials, people receiving dupilumab had decreased levels of T helper cells.[23]
Pharmacology[edit]
Mechanism of action[edit]
Dupilumab binds to the alpha subunit of the interleukin-4 receptor (IL-4Rα), making it a receptor antagonist.[24] Through blockade of IL-4Rα, dupilumab modulates signaling of both the interleukin 4 and interleukin 13 pathways.[23]
Pharmacokinetics[edit]
Dupilumab shows a non-linear rate in regard to the target.[23] Dupilumab is also reported to have a bioavailability of 64%, with the average concentration occurring one week after injection.[23]
History[edit]
Regeneron Pharmaceuticals and Sanofi Genzyme jointly developed dupilumab,[25] the latter of which provided 130 million dollars to Regeneron for research and development towards monoclonal antibodies.[26] Phase II trials for asthma treatment showed increased lung function with increased forced expiratory volume for patients.[23]
In October 2016, Regeneron completed a phase III trial comparing dupilumab with topical corticosteroids, in which subjects had a larger decrease in symptoms with both dupilumab and topical steroids than with steroids alone.[27] In these trials 38% and 36% of patients respectively, met the primary efficacy goal of the trial, compared to 8% and 10% under placebo.[23]
The US Food and Drug Administration (FDA) granted the application for dupilumab priority review designation[28][29] and in March 2017, the FDA approved dupilumab injection to treat adults with moderate-to-severe eczema.[7]
The efficacy and safety of dupilumab in eosinophilic esophagitis was studied in a randomized, double-blind, parallel-group, multicenter, placebo-controlled trial, that included two 24-week treatment periods (Part A and Part B) that were conducted independently in separate groups of participants.[9] In Part A and Part B, participants received either placebo or 300 milligrams of dupilumab every week.[9] The two primary measurements of efficacy were the proportion of participants who achieved a certain level of reduced eosinophils in the esophagus at week 24, as determined by assessing participants' esophageal tissue under a microscope, and the change in the participant-reported Dysphagia Symptom Questionnaire (DSQ) score from baseline to week 24.[9] The DSQ is a questionnaire designed to measure difficulty swallowing associated with eosinophilic esophagitis, with total scores ranging from 0 to 84; higher DSQ scores indicate worse symptoms.[9]
The efficacy and safety of dupilumab to treat prurigo nodularis among adults were evaluated in two clinical trials, EFC16459 (PRIME) and EFC16460 (PRIME2).[10] Each trial evaluated 300 mg of dupilumab administered every 2 weeks following an initial dose of 600 mg.[10] The treatment lasted for 24 weeks.[10] Effectiveness was mainly assessed by the proportion of subjects whose itchy skin (pruritus) improved by more than four points on the Worst Itch Numeric Rating Scale, the proportion of subjects who achieved score of 0 or 1 on Investigator's Global Assessment PN-stage scale (the equivalent of 0-5 nodules), and the proportion of subjects who achieved a response on both scales at week 24.[10]
References[edit]
- ^ a b "AusPAR: Dupilumab". Therapeutic Goods Administration (TGA). 4 May 2022. Retrieved 4 May 2022.
- ^ "Regulatory Decision Summary for Dupixent". Drug and Health Products Portal. 14 April 2023. Retrieved 2 April 2024.
- ^ "Skin health". Health Canada. 9 May 2018. Retrieved 13 April 2024.
- ^ a b c d "Dupixent- dupilumab injection, solution". DailyMed. 25 June 2020. Archived from the original on 24 March 2021. Retrieved 17 September 2020.
- ^ a b c "Dupixent EPAR". European Medicines Agency (EMA). 17 September 2018. Archived from the original on 28 December 2021. Retrieved 23 September 2021. Text was copied from this source which is copyright European Medicines Agency. Reproduction is authorized provided the source is acknowledged.
- ^ "Statement on a Nonproprietary Name Adopted By The USAN Council - Dupilumab" Archived 21 May 2021 at the Wayback Machine, American Medical Association.
- ^ a b c d "FDA approves new eczema drug Dupixent". U.S. Food and Drug Administration (FDA). 10 September 2019. Archived from the original on 28 March 2017. Retrieved 29 March 2017.
- ^ "FDA approves first treatment for chronic rhinosinusitis with nasal polyps". U.S. Food and Drug Administration (FDA). 26 June 2019. Archived from the original on 29 December 2020. Retrieved 27 June 2019.
- ^ a b c d e f g h i j k l "FDA Approves First Treatment for Eosinophilic Esophagitis, a Chronic Immune Disorder". U.S. Food and Drug Administration (FDA) (Press release). 20 May 2022. Archived from the original on 5 August 2022. Retrieved 20 May 2022.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ a b c d e f g h "FDA approves first treatment for prurigo nodularis". U.S. Food and Drug Administration (FDA). 29 September 2022. Archived from the original on 29 September 2022. Retrieved 30 September 2022.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ "Sanofi - Commercial collaboration". Sanofi. Archived from the original on 8 November 2017. Retrieved 9 March 2017.
- ^ "A powerful research and development engine". www.regeneron.com. Archived from the original on 30 April 2019. Retrieved 9 March 2017.
- ^ New Drug Therapy Approvals 2017 (PDF) (Report). U.S. Food and Drug Administration (FDA). January 2018. Archived from the original on 23 October 2020. Retrieved 16 September 2020.
- ^ Kraft M, Worm M (April 2017). "Dupilumab in the treatment of moderate-to-severe atopic dermatitis". Expert Review of Clinical Immunology. 13 (4): 301–310. doi:10.1080/1744666X.2017.1292134. PMID 28165826. S2CID 3404484.
- ^ Humbert M, Busse W, Hanania NA (January 2018). "Controversies and opportunities in severe asthma". Current Opinion in Pulmonary Medicine. 24 (1): 83–93. doi:10.1097/MCP.0000000000000438. PMID 29059087. S2CID 4433743.
- ^ Buchheit KM, Sohail A, Hacker J, Maurer R, Gakpo D, Bensko JC, et al. (August 2022). "Rapid and sustained effect of dupilumab on clinical and mechanistic outcomes in aspirin-exacerbated respiratory disease". The Journal of Allergy and Clinical Immunology. 150 (2): 415–424. doi:10.1016/j.jaci.2022.04.007. PMC 9378638. PMID 35460728.
- ^ Oykhman P, Paramo FA, Bousquet J, Kennedy DW, Brignardello-Petersen R, Chu DK (April 2022). "Comparative efficacy and safety of monoclonal antibodies and aspirin desensitization for chronic rhinosinusitis with nasal polyposis: A systematic review and network meta-analysis". The Journal of Allergy and Clinical Immunology. 149 (4): 1286–1295. doi:10.1016/j.jaci.2021.09.009. PMID 34543652.
- ^ EMA (17 September 2018). "Dupixent". European Medicines Agency. Retrieved 22 March 2023.
- ^ Devarasetti H (22 March 2023). "Sanofi Dupixent receives EC approval for atopic dermatitis". Pharmaceutical Technology. Retrieved 22 March 2023.
- ^ Clinical trial number NCT03930732 for "Randomized, Double-blind, Placebo-controlled, Parallel-group, 52-week Pivotal Study to Assess the Efficacy, Safety and Tolerability of Dupilumab in Patients with Moderate-to-severe Chronic Obstructive Pulmonary Disease (COPD) with Type 2 Inflammation" at ClinicalTrials.gov
- ^ "Dupixent® demonstrates potential to become first biologic to treat COPD by showing significant reduction in exacerbations in pivotal trial". Globe Newswire. Retrieved 14 May 2023.
- ^ Kim PJ, Lansang RP, Vender R (July 2023). "A Systematic Review and Meta-Analysis of Injection Site Reactions in Randomized-Controlled Trials of Biologic Injections". Journal of Cutaneous Medicine and Surgery. 27 (4): 358–367. doi:10.1177/12034754231188444. PMC 10486173. PMID 37533141.
- ^ a b c d e f Shirley M (July 2017). "Dupilumab: First Global Approval". Drugs. 77 (10): 1115–1121. doi:10.1007/s40265-017-0768-3. PMID 28547386. S2CID 207489287.
- ^ Wenzel S, Ford L, Pearlman D, Spector S, Sher L, Skobieranda F, et al. (June 2013). "Dupilumab in persistent asthma with elevated eosinophil levels". The New England Journal of Medicine. 368 (26): 2455–66. doi:10.1056/NEJMoa1304048. PMID 23688323.
- ^ Spencer D (8 March 2020). "Sanofi Genzyme Head on Incredible Success of "Once-in-a-Career" Product Dupixent". Pharmaboardroom. Archived from the original on 18 May 2021. Retrieved 18 May 2021.
- ^ "SEC 10-Q Filing of Regeneron". SEC.gov. 30 June 2017. Archived from the original on 21 October 2017. Retrieved 20 October 2017.
- ^ Hamilton JD, Ungar B, Guttman-Yassky E (2015). "Drug evaluation review: dupilumab in atopic dermatitis". Immunotherapy. 7 (10): 1043–58. doi:10.2217/imt.15.69. PMID 26598956.
- ^ "Novel Biologic Dupilumab Improves Eczema Symptoms". October 2016. Archived from the original on 11 March 2017. Retrieved 30 October 2017.
- ^ Walker J (30 May 2016). "New Eczema Treatments Could Be Available Soon". The Wall Street Journal. ISSN 0099-9660. Archived from the original on 5 January 2018. Retrieved 31 May 2016.
