Hematopoietic stem cell transplantation
| Hematopoietic stem cell transplantation | |
|---|---|
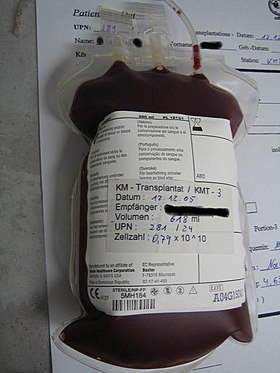 Bone marrow transplant | |
| ICD-9-CM | 41.0 |
| MeSH | D018380 |
| MedlinePlus | 003009 |
Hematopoietic stem-cell transplantation (HSCT) is the transplantation of multipotent hematopoietic stem cells, usually derived from bone marrow, peripheral blood, or umbilical cord blood in order to replicate inside of a patient and to produce additional normal blood cells.[1][2][3][4][5][6] It may be autologous (the patient's own stem cells are used), allogeneic (the stem cells come from a donor) or syngeneic (from an identical twin).[4][5]
It is most often performed for patients with certain cancers of the blood or bone marrow, such as multiple myeloma, leukemia, some types of lymphoma and immune deficiencies.[5] In these cases, the recipient's immune system is usually suppressed with radiation or chemotherapy before the transplantation. Infection and graft-versus-host disease are major complications of allogeneic HSCT.[5]
HSCT remains a dangerous procedure with many possible complications; it is reserved for patients with life-threatening diseases. As survival following the procedure has increased, its use has expanded beyond cancer to autoimmune diseases[7][8] and hereditary skeletal dysplasias, notably malignant infantile osteopetrosis[9][10] and mucopolysaccharidosis.[11]
Medical uses[edit]

Indications[edit]
Indications for stem-cell transplantation are:
Malignant (cancerous)[edit]
- Acute myeloid leukemia
- Chronic myeloid leukemia
- Acute lymphoblastic leukemia
- Juvenile myelomonocytic leukemia
- Hodgkin lymphoma (relapsed, refractory)
- Non-Hodgkin lymphoma (relapsed, refractory)
- Neuroblastoma
- Ewing sarcoma
- Multiple myeloma
- Myelodysplastic syndromes
- Gliomas, other solid tumors
Nonmalignant (noncancerous)[edit]
- Thalassemia
- Sickle cell anemia
- Aplastic anemia
- Fanconi anemia
- Malignant infantile osteopetrosis
- Mucopolysaccharidosis
- Paroxysmal nocturnal hemoglobinuria
- Pyruvate kinase deficiency
- Immune deficiency syndromes
- Autoimmune diseases,[12] including multiple sclerosis[13][14]
Many recipients of HSCTs are multiple myeloma[15] or leukemia patients[16] who would not benefit from prolonged treatment with, or are already resistant to, chemotherapy. Candidates for HSCTs include pediatric cases where the patient has an inborn defect such as severe combined immunodeficiency or congenital neutropenia with defective stem cells, and also children or adults with aplastic anemia[17] who have lost their stem cells after birth. Other conditions[18] treated with stem cell transplants include sickle cell disease, myelodysplastic syndrome, neuroblastoma, lymphoma, Ewing's sarcoma, desmoplastic small round cell tumor, chronic granulomatous disease, Hodgkin's disease and Wiskott–Aldrich syndrome. Non-myeloablative, so-called mini transplant (microtransplantation) procedures, have been developed requiring smaller doses of preparative chemotherapy and radiation therapy, allowing HSCT to be conducted in the elderly and other patients who would otherwise be considered too weak to withstand a conventional treatment regimen.[19]
Number of procedures[edit]
In 2006, 50,417 first HSCTs were recorded worldwide, according to a global survey of 1,327 centers in 71 countries conducted by the Worldwide Network for Blood and Marrow Transplantation. Of these, 28,901 (57%) were autologous and 21,516 (43%) were allogeneic (11,928 from family donors and 9,588 from unrelated donors). The main indications for transplant were lymphoproliferative disorders (55%) and leukemias (34%), and many took place in either Europe (48%) or the Americas (36%).[20]
The Worldwide Network for Blood and Marrow Transplantation reported the millionth transplant to have been undertaken in December 2012.[21]
In 2014, according to the World Marrow Donor Association, stem-cell products provided for unrelated transplantation worldwide had increased to 20,604 (4,149 bone-marrow donations, 12,506 peripheral blood stem-cell donations, and 3,949 cord-blood units).[22]
Graft types[edit]
Autologous[edit]
Autologous HSCT requires the extraction (apheresis) of hematopoietic stem cells (HSCs) from the patient and storage of the harvested cells in a freezer. The patient is then treated with high-dose chemotherapy with or without radiotherapy with the intention of eradicating the patient's malignant cell population at the cost of partial or complete bone marrow ablation (destruction of patient's bone marrow's ability to grow new blood cells). The patient's own stored stem cells are then transfused into his/her bloodstream, where they replace destroyed tissue and resume the patient's normal blood-cell production.[2] Autologous transplants have the advantage of lower risk of infection during the immune-compromised portion of the treatment, since the recovery of immune function is rapid. Also, the incidence of patients experiencing rejection is very rare (and graft-versus-host disease impossible) due to the donor and recipient being the same individual. These advantages have established autologous HSCT as one of the standard second-line treatments for such diseases as lymphoma.[23]
For other cancers such as acute myeloid leukemia, though, the reduced mortality of the autogenous relative to allogeneic HSCT may be outweighed by an increased likelihood of cancer relapse and related mortality, so the allogeneic treatment may be preferred for those conditions.[24]
Researchers have conducted small studies using nonmyeloablative HSCT as a possible treatment for type I (insulin dependent) diabetes in children and adults. Results have been promising, but as of 2019[update], speculating whether these experiments will lead to effective treatments for diabetes is premature.[25][26][27] Autologous HSCT is an effective treatment against aggressive Multiple Sclerosis.[28] The type of autologous HSCT used as a Multiple Sclerosis treatment is considered safe and the serious adverse events rare.[29]
Allogeneic[edit]
Allogeneic HSCT involves two people – the (healthy) donor and the (patient) recipient. Allogeneic HSC donors must have a tissue (human leukocyte antigen, HLA) type that matches the recipient. Matching is performed on the basis of variability at three or more loci of the HLA gene, and a perfect match at these loci is preferred. Even if a good match exists at these critical alleles, the recipient will require immunosuppressive medications to mitigate graft-versus-host disease. Allogeneic transplant donors may be related (usually a closely HLA-matched sibling), syngeneic (a monozygotic or identical twin of the patient – necessarily extremely rare since few patients have an identical twin, but offering a source of perfectly HLA-matched stem cells), unrelated (donor who is not related and found to have very close degree of HLA matching), or, as in the case of Haploidentical Transplantation (Haplo), a half-matched relative such as a parent, child, or sibling. Unrelated donors may be found through a registry of bone-marrow donors, such as the National Marrow Donor Program (NMDP) in the U.S. People who would like to be tested for a specific family member or friend without joining any of the bone-marrow registry data banks may contact a private HLA testing laboratory and be tested with a blood test or mouth swab to see if they are a potential match.[30] A "savior sibling" may be intentionally selected by preimplantation genetic diagnosis to match a child both regarding HLA type and being free of any obvious inheritable disorder. Allogeneic transplants are also performed using umbilical cord blood as the source of stem cells. In general, by transfusing healthy stem cells to the recipient's bloodstream to reform a healthy immune system, allogeneic HSCTs appear to improve chances for cure or long-term remission once the immediate transplant-related complications are resolved.[31][32][33]
A compatible donor is found by doing additional HLA testing from the blood of potential donors. The HLA genes fall in two categories (types I and II). In general, mismatches of the type-I genes (i.e. HLA-A, HLA-B, or HLA-C) increase the risk of graft rejection. A mismatch of an HLA type II gene (i.e. HLA-DR or HLA-DQB1) increases the risk of graft-versus-host disease. In addition, a genetic mismatch as small as a single DNA base pair is significant, so perfect matches require knowledge of the exact DNA sequence of these genes for both donor and recipient. Leading transplant centers currently perform testing for all five of these HLA genes before declaring that a donor and recipient are HLA-identical.[citation needed]
Race and ethnicity are known to play a major role in donor recruitment drives, as members of the same ethnic group are more likely to have matching genes, including the genes for HLA.[34]
As of 2013[update], at least two commercialized allogeneic cell therapies have been developed, Prochymal and Cartistem.[35] Omidubicel was approved for medical use in the United States in April 2023.[36]
Sources and storage of cells[edit]
To limit the risks of transplanted stem-cell rejection or of severe graft-versus-host disease in allogeneic HSCT, the donor should preferably have the same HLA-typing as the recipient. About 25 to 30% of allogeneic HSCT recipients have an HLA-identical sibling. Even so-called "perfect matches" may have mismatched minor alleles that contribute to graft-versus-host disease.[citation needed]
Bone marrow[edit]
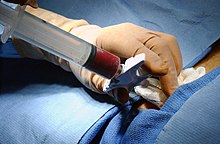
In the case of a bone-marrow transplant, the HSCs are removed from a large bone of the donor, typically the pelvis, through a large needle that reaches the center of the bone. The technique is referred to as a bone-marrow harvest and is performed under local or general anesthesia.[citation needed]
Peripheral blood stem cells[edit]

Peripheral blood stem cells[37] are now the most common source of stem cells for HSCT. They are collected from the blood through a process known as apheresis. The donor's blood is withdrawn through a sterile needle in one arm and passed through a machine that removes white blood cells. The red blood cells are returned to the donor. The peripheral stem cell yield is boosted with daily subcutaneous injections of granulocyte-colony stimulating factor, serving to mobilize stem cells from the donor's bone marrow into the peripheral circulation.[citation needed]
Amniotic fluid[edit]
Extracting stem cells from amniotic fluid is possible for both autologous and heterologous uses at the time of childbirth.[citation needed]
Storage of HSC[edit]
Unlike other organs, bone-marrow cells can be frozen (cryopreserved) for prolonged periods without damaging too many cells. This is a necessity with autologous HSCs because the cells must be harvested from the recipient months in advance of the transplant treatment. In the case of allogeneic transplants, fresh HSCs are preferred to avoid cell loss that might occur during the freezing and thawing process. Allogeneic cord blood is stored frozen at a cord blood bank because it is only obtainable at the time of childbirth. To cryopreserve HSCs, a preservative, dimethyl sulfoxide, must be added, and the cells must be cooled very slowly in a controlled-rate freezer to prevent osmotic cellular injury during ice-crystal formation. HSCs may be stored for years in a cryofreezer, which typically uses liquid nitrogen.[citation needed]
Conditioning regimens[edit]
Myeloablative[edit]
The chemotherapy or irradiation given immediately prior to a transplant is called the conditioning regimen, the purpose of which is to help eradicate the patient's disease prior to the infusion of HSCs and to suppress immune reactions. The bone marrow can be ablated (destroyed) with dose-levels that cause minimal injury to other tissues. In allogeneic transplants, a combination of cyclophosphamide with total body irradiation is conventionally employed. This treatment also has an immunosuppressive effect that prevents rejection of the HSCs by the recipient's immune system. The post-transplant prognosis often includes acute and chronic graft-versus-host disease that may be life-threatening. In certain leukemias, though, this can coincide with protection against cancer relapse owing to the graft-versus-tumor effect.[38] Autologous transplants may also use similar conditioning regimens, but many other chemotherapy combinations can be used depending on the type of disease.
Nonmyeloablative[edit]
A newer treatment approach, nonmyeloablative allogeneic transplantation, also termed reduced-intensity conditioning (RIC), uses doses of chemotherapy and radiation too low to eradicate all the bone-marrow cells of the recipient.[39]: 320–321 Instead, nonmyeloablative transplants run lower risks of serious infections and transplant-related mortality while relying upon the graft versus tumor effect to resist the inherent increased risk of cancer relapse.[40][41] Also significantly, while requiring high doses of immunosuppressive agents in the early stages of treatment, these doses are less than for conventional transplants.[42] This leads to a state of mixed chimerism early after transplant where both recipient and donor HSC coexist in the bone marrow space.[citation needed]
Decreasing doses of immunosuppressive therapy then allow donor T-cells to eradicate the remaining recipient HSCs and to induce the graft-versus-tumor effect. This effect is often accompanied by mild graft-versus-host disease, the appearance of which is often a surrogate marker for the emergence of the desirable graft versus tumor effect, and also serves as a signal to establish an appropriate dosage level for sustained treatment with low levels of immunosuppressive agents.[citation needed]
Because of their gentler conditioning regimens, these transplants are associated with a lower risk of transplant-related mortality, so allow patients who are considered too high-risk for conventional allogeneic HSCT to undergo potentially curative therapy for their disease. The optimal conditioning strategy for each disease and recipient has not been fully established, but RIC can be used in elderly patients unfit for myeloablative regimens, for whom a higher risk of cancer relapse may be acceptable.[39][41]
Engraftment[edit]
After several weeks of growth in the bone marrow, expansion of HSCs and their progeny is sufficient to normalize the blood cell counts and reinitiate the immune system. The offspring of donor-derived HSCs have been documented to populate many different organs of the recipient, including the heart, liver, and muscle, and these cells had been suggested to have the abilities of regenerating injured tissue in these organs. However, recent research has shown that such lineage infidelity does not occur as a normal phenomenon.[citation needed]
Chimerism monitoring is a method to monitor the balance between the patient's own stem cells and the new stem cells from a donor. In cases where the patient's own stem cells are increasing in number after treatment, the treatment may potentially not have worked as intended.[citation needed]
Complications[edit]
HSCT is associated with a high treatment-related mortality in the recipient, which limits its use to conditions that are themselves life-threatening. (The one-year survival rate has been estimated to be roughly 60%, although this figure includes deaths from the underlying disease, as well as from the transplant procedure.)[43] Major complications include veno-occlusive disease, mucositis, infections (sepsis), graft-versus-host disease, and the development of new malignancies.[citation needed]
Infection[edit]
Bone-marrow transplantation usually requires that the recipient's own bone marrow be destroyed (myeloablation). Prior to the administration of new cells (engraftment), patients may go for several weeks without appreciable numbers of white blood cells to help fight infection. This puts a patient at high risk of infections, sepsis, and septic shock, despite prophylactic antibiotics. However, antiviral medications, such as acyclovir and valacyclovir, are quite effective in prevention of HSCT-related outbreak of herpetic infection in seropositive patients.[44] The immunosuppressive agents employed in allogeneic transplants for the prevention or treatment of graft-versus-host disease further increase the risk of opportunistic infection. Immunosuppressive drugs are given for a minimum of six months after a transplantation, or much longer if required for the treatment of graft-versus-host disease. Transplant patients lose their acquired immunity, for example immunity to childhood diseases such as measles or polio. So, transplant patients must be retreated with childhood vaccines once they are off immunosuppressive medications.[citation needed]
Veno-occlusive disease[edit]
Severe liver injury can result from hepatic veno-occlusive disease (VOD), newly termed sinusoidal obstruction syndrome (SOS).[45] Elevated levels of bilirubin, hepatomegaly, and fluid retention are clinical hallmarks of this condition. The appreciation of the generalized cellular injury and obstruction in hepatic vein sinuses is now greater. Severe cases of SOS are associated with a high mortality rate. Anticoagulants or defibrotide may be effective in reducing the severity of VOD but may also increase bleeding complications. Ursodiol has been shown to help prevent VOD, presumably by facilitating the flow of bile.
Mucositis[edit]
The injury of the mucosal lining of the mouth and throat is a common regimen-related toxicity following ablative HSCT regimens. It is usually not life-threatening, but is very painful, and prevents eating and drinking. Mucositis is treated with pain medications plus intravenous infusions to prevent dehydration and malnutrition.[citation needed]
Hemorrhagic cystitis[edit]
The mucosal lining of the bladder is affected in about 5% of children undergoing HSCT. This causes hematuria (blood in urine), frequent urination, abdominal pain and thrombocytopenia.[46]
Graft-versus-host disease[edit]
Graft-versus-host disease (GvHD) is an inflammatory disease that is unique to allogeneic transplantation. It is an attack by the "new" bone marrow's immune cells against the recipient's tissues. This can occur even if the donor and recipient are HLA-identical because the immune system can still recognize other differences between their tissues. It is named graft-versus-host disease because the transplanted cells must accept the body rather than the body accepting the new cells.[47]
Acute GvHD typically occurs in the first three months after transplantation and may involve the skin, intestine, or liver. High-dose corticosteroids, such as prednisone, are a standard treatment, but this immunosuppressive treatment often leads to deadly infections. Chronic GvHD may also develop after allogeneic transplant. It is the major source of late treatment-related complications, although it less often results in death. In addition to inflammation, chronic GvHD may lead to the development of fibrosis, or scar tissue, similar to scleroderma; it may cause functional disability and require prolonged immunosuppressive therapy. GvHD is usually mediated by T cells, which react to foreign peptides presented on the major histocompatibility complex of the host.[citation needed]
Further research is needed to determine whether mesenchymal stromal cells can be use for prophylaxis and treatment of GvHD.[48]
Graft-versus-tumor effect[edit]
Graft-versus-tumor effect (GVT), or "graft versus leukemia" effect, is the beneficial aspect of the GvHD phenomenon. For example, HSCT patients with either acute, or in particular chronic, GvHD after an allogeneic transplant tend to have a lower risk of cancer relapse.[49][38] This is due to a therapeutic immune reaction of the grafted donor T lymphocytes against the diseased bone marrow of the recipient. This lower rate of relapse accounts for the increased success rate of allogeneic transplants, compared to transplants from identical twins, and indicates that allogeneic HSCT is a form of immunotherapy. GVT is the major benefit of transplants that do not employ the highest immunosuppressive regimens.
Graft versus tumor is mainly beneficial in diseases with slow progress, e.g. chronic leukemia, low-grade lymphoma, and in some cases multiple myeloma, but is less effective in rapidly growing acute leukemias.[50]
If cancer relapses after HSCT, another transplant can be performed, infusing the patient with a greater quantity of donor white blood cells (donor lymphocyte infusion).[50]
Malignancies[edit]
Patients after HSCT are at a higher risk for oral carcinoma. Post-HSCT oral cancer may have more aggressive behavior with poorer prognosis, when compared to oral cancer in non-HSCT patients.[51]
A meta-analysis showed that the risk of secondary cancers such as bone cancer, head and neck cancers, and melanoma, with standardized incidence ratios of 10.04 (3.48–16.61), 6.35 (4.76–7.93), and 3.52 (2.65–4.39), respectively, was significantly increased after HSCT. So, diagnostic tests for these cancers should be included in the screening program of these patients for the prevention and early detection of these cancers.[52]
Prognosis[edit]
Prognosis in HSCT varies widely dependent upon disease type, stage, stem-cell source, HLA-matched status (for allogeneic HSCT), and conditioning regimen. A transplant offers a chance for cure or long-term remission if the inherent complications of graft versus host disease, immunosuppressive treatments and the spectrum of opportunistic infections can be survived.[31][32] In recent years, survival rates have been gradually improving across almost all populations and subpopulations receiving transplants.[53]
Mortality for allogeneic stem cell transplantation can be estimated using the prediction model created by Sorror et al.,[54] using the Hematopoietic Cell Transplantation-Specific Comorbidity Index (HCT-CI). The HCT-CI was derived and validated by investigators at the Fred Hutchinson Cancer Research Center in the U.S. The HCT-CI modifies and adds to a well-validated comorbidity index, the Charlson Comorbidity Index (CCI) (Charlson, et al.)[55] The CCI was previously applied to patients undergoing allogeneic HCT, but appears to provide less survival prediction and discrimination than the HCT-CI scoring system.
Patients who were successfully treated with HSCT and total body irradiation in childhood were found to have increased fat mass percentage, leading to significantly decreased exercise capacity in adulthood. This suggests patients who underwent successful treatment with HSCT have an increased predisposition to cardiovascular disease later in life.[56]
Risks to donor[edit]
The risks of a complication depend on patient characteristics, health care providers, and the apheresis procedure, and the colony-stimulating factor used (G-CSF). G-CSF drugs include filgrastim (Neupogen, Neulasta), and lenograstim (Graslopin).
Drug risks[edit]
Filgrastim is typically dosed in the 10 microgram/kg level for 4–5 days during the harvesting of stem cells. The documented adverse effects of filgrastim include splenic rupture, acute respiratory distress syndrome, alveolar hemorrhage, and allergic reactions (usually experienced in first 30 minutes).[57][58][59] In addition, platelet and hemoglobin levels dip postprocedurally, not returning to normal until after a month.[59]
The question of whether geriatrics (patients over 65) react the same as patients under 65 has not been sufficiently examined. Coagulation issues and inflammation of atherosclerotic plaques are known to occur as a result of G-CSF injection. G-CSF has also been described to induce genetic changes in agranulocytes of normal donors.[58] There is no statistically significant evidence either for or against the hypothesis that myelodysplasia (MDS) or acute myeloid leukaemia (AML) can be induced by G-CSF in susceptible individuals.[60]
Access risks[edit]
Blood is drawn from a peripheral vein in a majority of patients, but a central line to the jugular, subclavian, and femoral veins may be used. Adverse reactions during apheresis were experienced in 20% of women and 8% of men, these adverse events primarily consisted of numbness/tingling, multiple line attempts, and nausea.[59]
Clinical observations[edit]
A study involving 2,408 donors (aged 18–60 years) indicated that bone pain (primarily back and hips) as a result of filgrastim treatment is observed in 80% of donors.[59] Donation is not recommended for those with a history of back pain.[59] Other symptoms observed in more than 40 percent of donors include muscle pain, headache, fatigue, and difficulty sleeping.[59] These symptoms all returned to baseline 1 month after donation in the majority of patients.[59]
In one meta-study that incorporated data from 377 donors, 44% of patients reported having adverse side effects after peripheral blood HSCT.[60] Side effects included pain prior to the collection procedure as a result of G-CSF injections, and postprocedural generalized skeletal pain, fatigue, and reduced energy.[60]
Severe reactions[edit]
A study that surveyed 2,408 donors found that serious adverse events (requiring prolonged hospitalization) occurred in 15 donors (at a rate of 0.6%), although none of these events was fatal.[59] Donors were not observed to have higher than normal rates of cancer with up to 4–8 years of follow-up.[59] One study based on a survey of medical teams covered about 24,000 peripheral blood HSCT cases between 1993 and 2005, and found a serious cardiovascular adverse reaction rate of about one in 1,500.[58] This study reported a cardiovascular-related fatality risk within the first 30 days of HSCT of about two in 10,000.[58]
History[edit]
In 1939, a woman with aplastic anaemia received the first human bone marrow transfusion. This patient received regular blood transfusions, and an attempt was made to increase her leukocyte and platelet counts by intravenous bone marrow injection without unexpected reaction.[61]
Stem-cell transplantation was pioneered using bone marrow-derived stem cells by a team at the Fred Hutchinson Cancer Research Center from the 1950s through the 1970s led by E. Donnall Thomas, whose work was later recognized with a Nobel Prize in Physiology or Medicine. Thomas' work showed that bone-marrow cells infused intravenously could repopulate the bone marrow and produce new blood cells. His work also reduced the likelihood of developing a life-threatening graft-versus-host disease.[62] Collaborating with Eloise Giblett, a professor at the University of Washington, he discovered genetic markers that could confirm donor matches.
The first physician to perform a successful human bone-marrow transplant on a disease other than cancer was Robert A. Good at the University of Minnesota in 1968.[63] In 1975, John Kersey, also of the University of Minnesota, performed the first successful bone-marrow transplant to cure lymphoma. His patient, a 16-year-old-boy, is today the longest-living lymphoma transplant survivor.[64]
Donor registration and recruitment[edit]
At the end of 2012, 20.2 million people had registered their willingness to be a bone-marrow donor with one of the 67 registries from 49 countries participating in Bone Marrow Donors Worldwide. Around 17.9 million of these registered donors had been ABDR typed, allowing easy matching. A further 561,000 cord blood units had been received by one of 46 cord blood banks from 30 countries participating. The highest total number of bone-marrow donors registered were those from the U.S. (8.0 million), and the highest number per capita were those from Cyprus (15.4% of the population).[65]
Within the U.S., racial minority groups are the least likely to be registered, so are the least likely to find a potentially life-saving match. In 1990, only six African Americans were able to find a bone-marrow match, and all six had common European genetic signatures.[66]
Africans are more genetically diverse than people of European descent, which means that more registrations are needed to find a match. Bone marrow and cord blood banks exist in South Africa, and a new program is beginning in Nigeria.[66] Many people belonging to different races are requested to donate as a shortage of donors exists in African, mixed race, Latino, aboriginal, and many other communities.
Two registries in the U.S. recruit unrelated allogeneic donors: NMDP or Be the Match, and the Gift of Life Marrow Registry.
Research[edit]
HIV[edit]
In 2007, a team of doctors in Berlin, Germany, including Gero Hütter, performed a stem-cell transplant for leukemia patient Timothy Ray Brown, who was also HIV-positive.[67] From 60 matching donors, they selected a [CCR5]-Δ32 homozygous individual with two genetic copies of a rare variant of a cell surface receptor. This genetic trait confers resistance to HIV infection by blocking attachment of HIV to the cell. Roughly one in 1,000 people of European ancestry have this inherited mutation, but it is rarer in other populations.[68][69] The transplant was repeated a year later after a leukemia relapse. Over three years after the initial transplant, and despite discontinuing antiretroviral therapy, researchers cannot detect HIV in the transplant recipient's blood or in various biopsies of his tissues.[70] Levels of HIV-specific antibodies have also declined, leading to speculation that the patient may have been functionally cured of HIV, but scientists emphasise that this is an unusual case.[71] Potentially fatal transplant complications (the "Berlin patient" developed graft-versus-host disease and leukoencephalopathy) mean that the procedure could not be performed in others with HIV, even if sufficient numbers of suitable donors were found.[72][73]
In 2012, Daniel Kuritzkes reported results of two stem-cell transplants in patients with HIV. They did not, however, use donors with the Δ32 deletion. After their transplant procedures, both were put on antiretroviral therapies, during which neither showed traces of HIV in their blood plasma and purified CD4+ T cells using a sensitive culture method (less than 3 copies/ml). The virus was once again detected in both patients some time after the discontinuation of therapy.[74]
In 2019, a British man became the second to be cleared of HIV after receiving a bone-marrow transplant from a virus-resistant (Δ32) donor. This patient is being called "the London patient" (a reference to the famous Berlin patient).[75]
Multiple sclerosis[edit]
Since McAllister's 1997 report on a patient with multiple sclerosis (MS) who received a bone-marrow transplant for chronic myelogenous leukemia (CML),[76] over 600 reports have been published describing HSCTs performed primarily for MS.[77] These have been shown to "reduce or eliminate ongoing clinical relapses, halt further progression, and reduce the burden of disability in some patients" who have aggressive, highly active MS, "in the absence of chronic treatment with disease-modifying agents".[77] A randomized clinical trial including 110 patients showed that HSCT significantly prolonged time to disease progression compared to disease-modifying therapy.[78] Long-term outcome in patients with severe disease has showed that complete disease remission after HSCT is possible.[79]
Other autoimmune neurological diseases[edit]
HSCT can also be used for treating selected, severe cases of other autoimmune neurological diseases such as neuromyelitis optica, chronic inflammatory demyelinating polyneuropathy, and myasthenia gravis.[80]
References[edit]
- ^ Monga I, Kaur K, Dhanda S (March 2022). "Revisiting hematopoiesis: applications of the bulk and single-cell transcriptomics dissecting transcriptional heterogeneity in hematopoietic stem cells". Briefings in Functional Genomics. 21 (3): 159–176. doi:10.1093/bfgp/elac002. PMID 35265979.
- ^ a b Nabarrete, J. M.; Pereira, A. Z.; Garófolo, A.; Seber, A.; Venancio, A. M.; Grecco, C. E.; Bonfim, C. M.; Nakamura, C. H.; Fernandes, D.; Campos, D. J.; Oliveira, F. L.; Cousseiro, F. K.; Rossi, F. F.; Gurmini, J.; Viani, K. H.; Guterres, L. F.; Mantovani, L. F.; Darrigo Lg, Junior; Albuquerque, M. I.; Brumatti, M.; Neves, M. A.; Duran, N.; Villela, N. C.; Zecchin, V. G.; Fernandes, J. F. (2021). "Brazilian Nutritional Consensus in Hematopoietic Stem Cell Transplantation: Children and adolescents". Einstein. 19: eAE5254. doi:10.31744/einstein_journal/2021AE5254. PMC 8664291. PMID 34909973.
- ^ Forman SJ, Negrin RS, Antin JH, Appelbaum FR. Thomas' hematopoietic cell transplantation: stem cell transplantation. 5th ed. Vol. 2. New Jersey: Wiley-Blackwell; 2016. p.1416.
- ^ a b Felfly H, Haddad GG (2014). "Hematopoietic stem cells: potential new applications for translational medicine". Journal of Stem Cells. 9 (3): 163–197. PMID 25157450.
- ^ a b c d Park B, Yoo KH, Kim C (December 2015). "Hematopoietic stem cell expansion and generation: the ways to make a breakthrough". Blood Research. 50 (4): 194–203. doi:10.5045/br.2015.50.4.194. PMC 4705045. PMID 26770947.
- ^ Mahla RS (2016). "Stem Cells Applications in Regenerative Medicine and Disease Therapeutics". International Journal of Cell Biology. 2016 (7): 6940283. doi:10.1155/2016/6940283. PMC 4969512. PMID 27516776.
- ^ Tyndall A, Fassas A, Passweg J, Ruiz de Elvira C, Attal M, Brooks P, et al. (October 1999). "Autologous haematopoietic stem cell transplants for autoimmune disease – feasibility and transplant-related mortality. Autoimmune Disease and Lymphoma Working Parties of the European Group for Blood and Marrow Transplantation, the European League Against Rheumatism and the International Stem Cell Project for Autoimmune Disease". Bone Marrow Transplantation. 24 (7): 729–734. doi:10.1038/sj.bmt.1701987. PMID 10516675.
- ^ Burt RK, Loh Y, Pearce W, Beohar N, Barr WG, Craig R, et al. (February 2008). "Clinical applications of blood-derived and marrow-derived stem cells for nonmalignant diseases". JAMA. 299 (8): 925–936. doi:10.1001/jama.299.8.925. PMID 18314435.
- ^ EL-Sobky TA, El-Haddad A, Elsobky E, Elsayed SM, Sakr HM (March 2017). "Reversal of skeletal radiographic pathology in a case of malignant infantile osteopetrosis following hematopoietic stem cell transplantation". The Egyptian Journal of Radiology and Nuclear Medicine. 48 (1): 237–243. doi:10.1016/j.ejrnm.2016.12.013.
- ^ Hashemi Taheri AP, Radmard AR, Kooraki S, Behfar M, Pak N, Hamidieh AA, Ghavamzadeh A (September 2015). "Radiologic resolution of malignant infantile osteopetrosis skeletal changes following hematopoietic stem cell transplantation". Pediatric Blood & Cancer. 62 (9): 1645–1649. doi:10.1002/pbc.25524. PMID 25820806. S2CID 11287381.
- ^ Langereis EJ, den Os MM, Breen C, Jones SA, Knaven OC, Mercer J, et al. (March 2016). "Progression of Hip Dysplasia in Mucopolysaccharidosis Type I Hurler After Successful Hematopoietic Stem Cell Transplantation". The Journal of Bone and Joint Surgery. American Volume. 98 (5): 386–395. doi:10.2106/JBJS.O.00601. PMID 26935461. S2CID 207284951.
- ^ Alexander T, Arnold R, Hiepe F, Radbruch A (1 July 2016). "Resetting the immune system with immunoablation and autologous haematopoietic stem cell transplantation in autoimmune diseases". Clinical and Experimental Rheumatology. 34 (4 Suppl 98): 53–57. PMID 27586805.
- ^ Fassas, A.; Kimiskidis, V. K.; Sakellari, I.; Kapinas, K.; Anagnostopoulos, A.; Tsimourtou, V.; Sotirakoglou, K.; Kazis, A. (22 March 2011). "Long-term results of stem cell transplantation for MS: A single-center experience". Neurology. 76 (12): 1066–1070. doi:10.1212/WNL.0b013e318211c537. ISSN 0028-3878. PMID 21422458. S2CID 15117695.
- ^ Saccardi, Riccardo; Mancardi, Gian Luigi; Solari, Alessandra; Bosi, Alberto; Bruzzi, Paolo; Di Bartolomeo, Paolo; Donelli, Amedea; Filippi, Massimo; Guerrasio, Angelo; Gualandi, Francesca; La Nasa, Giorgio (15 March 2005). "Autologous HSCT for severe progressive multiple sclerosis in a multicenter trial: impact on disease activity and quality of life". Blood. 105 (6): 2601–2607. doi:10.1182/blood-2004-08-3205. ISSN 0006-4971. PMID 15546956. S2CID 22645544.
- ^ Bladé J, Samson D, Reece D, Apperley J, Björkstrand B, Gahrton G, et al. (September 1998). "Criteria for evaluating disease response and progression in patients with multiple myeloma treated by high-dose therapy and haemopoietic stem cell transplantation. Myeloma Subcommittee of the EBMT. European Group for Blood and Marrow Transplant". British Journal of Haematology. 102 (5): 1115–1123. doi:10.1046/j.1365-2141.1998.00930.x. PMID 9753033. S2CID 767838.
- ^ Pavletic SZ, Khouri IF, Haagenson M, King RJ, Bierman PJ, Bishop MR, et al. (August 2005). "Unrelated donor marrow transplantation for B-cell chronic lymphocytic leukemia after using myeloablative conditioning: results from the Center for International Blood and Marrow Transplant research". Journal of Clinical Oncology. 23 (24): 5788–5794. doi:10.1200/JCO.2005.03.962. PMID 16043827.
- ^ Locasciulli A, Oneto R, Bacigalupo A, Socié G, Korthof E, Bekassy A, et al. (January 2007). "Outcome of patients with acquired aplastic anemia given first line bone marrow transplantation or immunosuppressive treatment in the last decade: a report from the European Group for Blood and Marrow Transplantation (EBMT)". Haematologica. 92 (1): 11–18. doi:10.3324/haematol.10075. PMID 17229630.
- ^ Center for International Blood and Marrow Transplant Research. "CIBMTR Summary Slides I". Archived from the original on 14 December 2012.
- ^ Cai B, Guo M, Ai H (November 2018). "Microtransplantation: clinical applications and mechanisms". Curr Opin Hematol. 25 (6): 417–424. doi:10.1097/MOH.0000000000000470. PMID 30148720. S2CID 239799097.
- ^ Gratwohl A, Baldomero H, Aljurf M, Pasquini MC, Bouzas LF, Yoshimi A, et al. (April 2010). "Hematopoietic stem cell transplantation: a global perspective". JAMA. 303 (16): 1617–1624. doi:10.1001/jama.2010.491. PMC 3219875. PMID 20424252.
- ^ Gratwohl A, Pasquini MC, ALjurf M, et al. (2015). "One million haemopoietic stem-cell transplants: a retrospective observational study". Lancet Haematol. 2 (3): e91–100. doi:10.1016/S2352-3026(15)00028-9. PMID 26687803. Erratum in: Lancet Haematol. 2015 May; 2(5): e184
- ^ Charts from "Annual Report, 2014". World Marrow Donor Association.[permanent dead link]
- ^ Canellos, George (1997). "Lymphoma Update: 1997". The Oncologist. 2 (3): 181–183. doi:10.1634/theoncologist.2-3-181a.
- ^ Bruno B, Rotta M, Patriarca F, Mordini N, Allione B, Carnevale-Schianca F, et al. (March 2007). "A comparison of allografting with autografting for newly diagnosed myeloma". The New England Journal of Medicine. 356 (11): 1110–1120. doi:10.1056/NEJMoa065464. PMID 17360989. S2CID 2031300.
- ^ Couri CE, Oliveira MC, Stracieri AB, Moraes DA, Pieroni F, Barros GM, et al. (April 2009). "C-peptide levels and insulin independence following autologous nonmyeloablative hematopoietic stem cell transplantation in newly diagnosed type 1 diabetes mellitus". JAMA. 301 (15): 1573–1579. doi:10.1001/jama.2009.470. PMID 19366777.
- ^ Penaforte-Saboia JG, Montenegro RM, Couri CE, Batista LA, Montenegro AP, Fernandes VO, et al. (23 November 2017). "Microvascular Complications in Type 1 Diabetes: A Comparative Analysis of Patients Treated with Autologous Nonmyeloablative Hematopoietic Stem-Cell Transplantation and Conventional Medical Therapy". Frontiers in Endocrinology. 8: 331. doi:10.3389/fendo.2017.00331. PMC 5703738. PMID 29218029.
- ^ D'Addio F, Valderrama Vasquez A, Ben Nasr M, Franek E, Zhu D, Li L, et al. (September 2014). "Autologous nonmyeloablative hematopoietic stem cell transplantation in new-onset type 1 diabetes: a multicenter analysis". Diabetes. 63 (9): 3041–3046. doi:10.2337/db14-0295. PMID 24947362.
- ^ Muraro, Paolo A.; Martin, Roland; Mancardi, Giovanni Luigi; Nicholas, Richard; Sormani, Maria Pia; Saccardi, Riccardo (July 2017). "Autologous haematopoietic stem cell transplantation for treatment of multiple sclerosis". Nature Reviews. Neurology. 13 (7): 391–405. doi:10.1038/nrneurol.2017.81. hdl:10044/1/50510. ISSN 1759-4766. PMID 28621766. S2CID 20836380.
- ^ Ge, Fangfang; Lin, Hong; Li, Zhuyi; Chang, Ting (March 2019). "Efficacy and safety of autologous hematopoietic stem-cell transplantation in multiple sclerosis: a systematic review and meta-analysis". Neurological Sciences. 40 (3): 479–487. doi:10.1007/s10072-018-3670-1. ISSN 1590-3478. PMID 30535563. S2CID 54461739.
- ^ Kate. "Public registry or private donation? – Information". bonemarrowtest.com. Archived from the original on 15 November 2012. Retrieved 2 May 2018.
- ^ a b Russell N, Bessell E, Stainer C, Haynes A, Das-Gupta E, Byrne J (2000). "Allogeneic haemopoietic stem cell transplantation for multiple myeloma or plasma cell leukaemia using fractionated total body radiation and high-dose melphalan conditioning". Acta Oncologica. 39 (7): 837–841. doi:10.1080/028418600750063596. PMID 11145442. S2CID 218897646.
- ^ a b Nivison-Smith I, Bradstock KF, Dodds AJ, Hawkins PA, Szer J (January 2005). "Haemopoietic stem cell transplantation in Australia and New Zealand, 1992–2001: progress report from the Australasian Bone Marrow Transplant Recipient Registry". Internal Medicine Journal. 35 (1): 18–27. doi:10.1111/j.1445-5994.2004.00704.x. PMID 15667464. S2CID 29779201.
- ^ Venkat, Chaya (19 July 2005). "The Only Real Cure Out There, for Now " Archived 30 May 2008 at the Wayback Machine. CLL Topics, Inc.
- ^ "Why race and ethnicity matter" Archived 1 February 2014 at the Wayback Machine. Be the Match. Retrieved 27 January 2014.
- ^ Simaria, Ana Sofia; et al. (March 2013). "Cost-effectiveness of Single-Use Technologies for Commercial Cell Therapy Manufacture". Am. Pharm. Rev.: 40. ISSN 1099-8012.
- ^ "FDA approves omidubicel to reduce time to neutrophil recovery and infection in patients with hematologic malignancies". U.S. Food and Drug Administration (FDA). 17 April 2023. Retrieved 20 April 2023.
- ^ Cutler C, Antin JH (2001). "Peripheral blood stem cells for allogeneic transplantation: a review". Stem Cells. 19 (2): 108–117. doi:10.1634/stemcells.19-2-108. PMID 11239165.
- ^ a b Toze CL, Galal A, Barnett MJ, Shepherd JD, Conneally EA, Hogge DE, et al. (November 2005). "Myeloablative allografting for chronic lymphocytic leukemia: evidence for a potent graft-versus-leukemia effect associated with graft-versus-host disease". Bone Marrow Transplantation. 36 (9): 825–830. doi:10.1038/sj.bmt.1705130. PMID 16151430.
- ^ a b Kaushansky, K; Lichtman, M; Beutler, E; Kipps, T; Prchal, J; Seligsohn, U. (2010). Williams Hematology (8th ed.). McGraw-Hill. ISBN 978-0071621519.
- ^ Alyea EP, Kim HT, Ho V, Cutler C, DeAngelo DJ, Stone R, et al. (October 2006). "Impact of conditioning regimen intensity on outcome of allogeneic hematopoietic cell transplantation for advanced acute myelogenous leukemia and myelodysplastic syndrome". Biology of Blood and Marrow Transplantation. 12 (10): 1047–1055. doi:10.1016/j.bbmt.2006.06.003. PMID 17067911.
- ^ a b Alyea EP, Kim HT, Ho V, Cutler C, Gribben J, DeAngelo DJ, et al. (February 2005). "Comparative outcome of nonmyeloablative and myeloablative allogeneic hematopoietic cell transplantation for patients older than 50 years of age". Blood. 105 (4): 1810–1814. doi:10.1182/blood-2004-05-1947. PMID 15459007.
- ^ Mielcarek M, Martin PJ, Leisenring W, Flowers ME, Maloney DG, Sandmaier BM, et al. (July 2003). "Graft-versus-host disease after nonmyeloablative versus conventional hematopoietic stem cell transplantation". Blood. 102 (2): 756–762. doi:10.1182/blood-2002-08-2628. PMID 12663454.
- ^ "MSK's One-Year Survival Rate after Allogeneic Bone Marrow Transplant Exceeds Expectations – Memorial Sloan Kettering Cancer Center". mskcc.org. 2012. Archived from the original on 13 October 2017. Retrieved 2 May 2018.
- ^ Elad S, Zadik Y, Hewson I, Hovan A, Correa ME, Logan R, et al. (August 2010). "A systematic review of viral infections associated with oral involvement in cancer patients: a spotlight on Herpesviridea". Supportive Care in Cancer. 18 (8): 993–1006. doi:10.1007/s00520-010-0900-3. PMID 20544224. S2CID 2969472.
- ^ "Sinusoidal Obstruction". livertox.nih.gov. Retrieved 30 July 2019.
- ^ Hamidieh, A. A.; Behfar, M.; Jabalameli, N.; Jalali, A.; Aliabadi, L. S.; Sadat Hosseini, A.; Basirpanah, S.; Ghavamzadeh, A. (2014). "Hemorrhagic Cystitis Following Hematopoietic Stem Cell Transplants in Children: Single Center Experience". Biology of Blood and Marrow Transplantation. 20 (2): S169–S170. doi:10.1016/j.bbmt.2013.12.275.
- ^ Shizuru JA, Jerabek L, Edwards CT, Weissman IL (February 1996). "Transplantation of purified hematopoietic stem cells: requirements for overcoming the barriers of allogeneic engraftment". Biology of Blood and Marrow Transplantation. 2 (1): 3–14. PMID 9078349.
- ^ Fisher SA, Cutler A, Doree C, Brunskill SJ, Stanworth SJ, Navarrete C, Girdlestone J (January 2019). Cochrane Haematological Malignancies Group (ed.). "Mesenchymal stromal cells as treatment or prophylaxis for acute or chronic graft-versus-host disease in haematopoietic stem cell transplant (HSCT) recipients with a haematological condition". The Cochrane Database of Systematic Reviews. 1 (1): CD009768. doi:10.1002/14651858.CD009768.pub2. PMC 6353308. PMID 30697701.
- ^ Baron F, Maris MB, Sandmaier BM, Storer BE, Sorror M, Diaconescu R, et al. (March 2005). "Graft-versus-tumor effects after allogeneic hematopoietic cell transplantation with nonmyeloablative conditioning". Journal of Clinical Oncology. 23 (9): 1993–2003. doi:10.1200/JCO.2005.08.136. hdl:2268/102049. PMID 15774790.
- ^ a b Memorial Sloan-Kettering Cancer Center > Blood & Marrow Stem Cell Transplantation > The Graft-versus-Tumor Effect Archived 4 July 2008 at the Wayback Machine Last Updated: 20 November 2003. Retrieved on 6 April 2009
- ^ Elad S, Zadik Y, Zeevi I, Miyazaki A, de Figueiredo MA, Or R (December 2010). "Oral cancer in patients after hematopoietic stem-cell transplantation: long-term follow-up suggests an increased risk for recurrence". Transplantation. 90 (11): 1243–1244. doi:10.1097/TP.0b013e3181f9caaa. PMID 21119507.
- ^ Heydari K, Shamshirian A, Lotfi-Foroushani P, Aref A, Hedayatizadeh-Omran A, Ahmadi M, et al. (October 2020). "The risk of malignancies in patients receiving hematopoietic stem cell transplantation: a systematic review and meta-analysis". Clinical & Translational Oncology. 22 (10): 1825–1837. doi:10.1007/s12094-020-02322-w. PMID 32108275. S2CID 211539024.
- ^ "Data analysis slides by Center for International Blood and Marrow Transplant Research". mcw.edu. Archived from the original on 6 August 2012. Retrieved 2 May 2018.
- ^ Sorror ML, Maris MB, Storb R, Baron F, Sandmaier BM, Maloney DG, Storer B (October 2005). "Hematopoietic cell transplantation (HCT)-specific comorbidity index: a new tool for risk assessment before allogeneic HCT". Blood. 106 (8): 2912–2919. doi:10.1182/blood-2005-05-2004. PMC 1895304. PMID 15994282.
- ^ Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987). "A new method of classifying prognostic comorbidity in longitudinal studies: development and validation". Journal of Chronic Diseases. 40 (5): 373–383. doi:10.1016/0021-9681(87)90171-8. PMID 3558716.
- ^ Öberg, Anders; Genberg, Margareta; Malinovschi, Andrei; Hedenström, Hans; Frisk, Per (February 2018). "Exercise capacity in young adults after hematopoietic cell transplantation in childhood". American Journal of Transplantation. 18 (2): 417–423. doi:10.1111/ajt.14456. ISSN 1600-6135. PMID 28787762. S2CID 1397521.
- ^ Neupogen Prescription information Archived 25 May 2010 at the Wayback Machine
- ^ a b c d Halter J, Kodera Y, Ispizua AU, Greinix HT, Schmitz N, Favre G, et al. (January 2009). "Severe events in donors after allogeneic hematopoietic stem cell donation". Haematologica. 94 (1): 94–101. doi:10.3324/haematol.13668. PMC 2625420. PMID 19059940.
- ^ a b c d e f g h i Pulsipher MA, Chitphakdithai P, Miller JP, Logan BR, King RJ, Rizzo JD, et al. (April 2009). "Adverse events among 2408 unrelated donors of peripheral blood stem cells: results of a prospective trial from the National Marrow Donor Program". Blood. 113 (15): 3604–3611. doi:10.1182/blood-2008-08-175323. PMC 2668845. PMID 19190248.
- ^ a b c Pamphilon D, Siddiq S, Brunskill S, Dorée C, Hyde C, Horowitz M, Stanworth S (October 2009). "Stem cell donation--what advice can be given to the donor?". British Journal of Haematology. 147 (1): 71–76. doi:10.1111/j.1365-2141.2009.07832.x. PMC 3409390. PMID 19681886.
- ^ "Aplastic Anemia Treated with Daily Transfusions and Intravenous Marrow: Case Report Treated with Daily". Annals of Internal Medicine. 13 (2): 357. 1 August 1939. doi:10.7326/0003-4819-13-2-357. ISSN 0003-4819.
- ^ Thomas ED, Lochte HL, Lu WC, Ferrebee JW (September 1957). "Intravenous infusion of bone marrow in patients receiving radiation and chemotherapy". The New England Journal of Medicine. 257 (11): 491–496. doi:10.1056/NEJM195709122571102. PMID 13464965.
- ^ Saxon, Wolfgang (18 June 2003). "Robert A. Good, 81, Founder of Modern Immunology, Dies". The New York Times. Archived from the original on 4 November 2012.
- ^ The Bone Marrow Foundation. "Cancer Research Pioneer Dies". Archived from the original on 6 October 2013. Retrieved 6 October 2013.
- ^ "WMDA" (PDF). WMDA. Archived from the original on 20 December 2013.
- ^ a b McNeil, Donald (11 May 2012). "Finding a Match, and a Mission: Helping Blacks Survive Cancer". The New York Times. Archived from the original on 5 March 2014. Retrieved 15 May 2012.
- ^ "German HIV patient cured after stem cell transplant". Belfast Telegraph. 15 December 2010. Retrieved 15 December 2010.
- ^ "Bone marrow 'cures HIV patient'". BBC News. 13 November 2008. Archived from the original on 7 January 2009. Retrieved 2 January 2009.
- ^ Novembre J, Galvani AP, Slatkin M (November 2005). "The geographic spread of the CCR5 Delta32 HIV-resistance allele". PLOS Biology. 3 (11): e339. doi:10.1371/journal.pbio.0030339. PMC 1255740. PMID 16216086.
- ^ Allers K, Hütter G, Hofmann J, Loddenkemper C, Rieger K, Thiel E, Schneider T (March 2011). "Evidence for the cure of HIV infection by CCR5Δ32/Δ32 stem cell transplantation". Blood. 117 (10): 2791–2799. doi:10.1182/blood-2010-09-309591. PMID 21148083. S2CID 27285440.
- ^ "Transplanting Hope: Stem Cell Experiment Raises Eyebrows at CROI". aidsmeds.com. 11 March 2008. Archived from the original on 26 January 2016. Retrieved 2 May 2018.
- ^ Levy JA (February 2009). "Not an HIV cure, but encouraging new directions". The New England Journal of Medicine. 360 (7): 724–725. doi:10.1056/NEJMe0810248. PMID 19213687.
- ^ van Lunzen J, Fehse B, Hauber J (June 2011). "Gene therapy strategies: can we eradicate HIV?". Current HIV/AIDS Reports. 8 (2): 78–84. doi:10.1007/s11904-011-0073-9. PMID 21331536. S2CID 43463970.
- ^ "HIV returns in two Boston patients after bone marrow transplants". CNN. 9 December 2013. Archived from the original on 8 December 2013.
- ^ Mandavilli, Apoorva (4 March 2019). "H.I.V. Is Reported Cured in a Second Patient, a Milestone in the Global AIDS Epidemic". The New York Times.
- ^ McAllister LD, Beatty PG, Rose J (February 1997). "Allogeneic bone marrow transplant for chronic myelogenous leukemia in a patient with multiple sclerosis". Bone Marrow Transplantation. 19 (4): 395–397. doi:10.1038/sj.bmt.1700666. PMID 9051253.
- ^ a b Atkins HL, Freedman MS (January 2013). "Hematopoietic stem cell therapy for multiple sclerosis: top 10 lessons learned". Neurotherapeutics. 10 (1): 68–76. doi:10.1007/s13311-012-0162-5. PMC 3557353. PMID 23192675.
- ^ Burt RK, Balabanov R, Burman J, Sharrack B, Snowden JA, Oliveira MC, et al. (January 2019). "Effect of Nonmyeloablative Hematopoietic Stem Cell Transplantation vs Continued Disease-Modifying Therapy on Disease Progression in Patients With Relapsing-Remitting Multiple Sclerosis: A Randomized Clinical Trial". JAMA. 321 (2): 165–174. doi:10.1001/jama.2018.18743. PMC 6439765. PMID 30644983.
- ^ Tolf A, Fagius J, Carlson K, Åkerfeldt T, Granberg T, Larsson EM, Burman J (November 2019). "Sustained remission in multiple sclerosis after hematopoietic stem cell transplantation". Acta Neurologica Scandinavica. 140 (5): 320–327. doi:10.1111/ane.13147. PMID 31297793. S2CID 195894616.
- ^ Burman J, Tolf A, Hägglund H, Askmark H (February 2018). "Autologous haematopoietic stem cell transplantation for neurological diseases". Journal of Neurology, Neurosurgery, and Psychiatry. 89 (2): 147–155. doi:10.1136/jnnp-2017-316271. PMC 5800332. PMID 28866625.
Further reading[edit]
- Cote GM, Hochberg EP, Muzikansky A, Hochberg FH, Drappatz J, McAfee SL, et al. (January 2012). "Autologous stem cell transplantation with thiotepa, busulfan, and cyclophosphamide (TBC) conditioning in patients with CNS involvement by non-Hodgkin lymphoma". Biology of Blood and Marrow Transplantation. 18 (1): 76–83. doi:10.1016/j.bbmt.2011.07.006. PMID 21749848.
External links[edit]
- Bone marrow transplant – What happens on NHS Choices
- HCT-CI (Sorror et al. 2005) online calculator
