Speech–language pathology
This article needs additional citations for verification. (January 2024) |
| Speech-language pathology | |
|---|---|
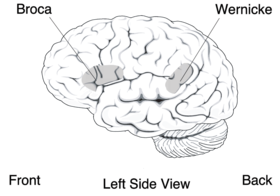 Broca's area (speech production) and Wernicke's area (language comprehension) | |
| MeSH | D013066 |
| Disability |
|---|
|
|
Speech–language pathology (also known as speech and language pathology or logopedics) is a healthcare and academic discipline concerning the evaluation, treatment, and prevention of communication disorders, including expressive and mixed receptive-expressive language disorders, voice disorders, speech sound disorders, speech disfluency, pragmatic language impairments, and social communication difficulties, as well as swallowing disorders across the lifespan. It is an allied health profession regulated by professional bodies including the American Speech-Language-Hearing Association (ASHA) and Speech Pathology Australia. The field of speech-language pathology is practiced by a clinician known as a speech-language pathologist (SLP)[1] or a speech and language therapist (SLT)[2]. SLPs also play an important role in the screening, diagnosis, and treatment of autism spectrum disorder (ASD), often in collaboration with pediatricians and psychologists.
History[edit]
The development of speech-language pathology into a profession took different paths in the various regions of the world. Three identifiable trends influenced the evolution of speech-language pathology in the United States during the late 19th century to early 20th century: the elocution movement, scientific revolution, and the rise of professionalism.[3] Groups of "speech correctionists" formed in the early 1900s. The American Academy of Speech Correction was founded in 1925, which became ASHA in 1978.[4]
The profession[edit]
Speech-language pathologists (SLPs) provide a wide range of services, mainly on an individual basis, but also as support for families, support groups, and providing information for the general public. SLPs work to assess levels of communication needs, make diagnoses based on the assessments, and then treat the diagnoses or address the needs.[5] Speech/language services begin with initial screening for communication and/or swallowing disorders and continue with assessment and diagnosis, consultation for the provision of advice regarding management, intervention, and treatment, and providing counseling and other followup services for these disorders. Services are provided in the following areas:
- Developmental language and early feeding neurodevelopment and prevention;
- cognitive aspects of communication (e.g., attention, memory, problem-solving, executive functions);
- speech (phonation, articulation, fluency, resonance, and voice including aeromechanical components of respiration);
- language (phonology, morphology, syntax, semantics, and pragmatic/social aspects of communication) including comprehension and expression in oral, written, graphic, and manual modalities; language processing; preliteracy and language-based literacy skills, phonological awareness;
- augmentative and alternative communication (AAC) for individuals with severe language and communication impairments;
- swallowing or other upper aerodigestive functions such as infant feeding and aeromechanical events (evaluation of esophageal function is for the purpose of referral to medical professionals);
- voice (hoarseness, dysphonia), poor vocal volume (hypophonia), abnormal (e.g., rough, breathy, strained) vocal quality. Research demonstrates voice therapy to be especially helpful with certain patient populations; individuals with Parkinson's Disease often develop voice issues as a result of their disease.[6]
- sensory awareness related to communication, swallowing, or other upper aerodigestive functions.
Speech, language, and swallowing disorders result from a variety of causes, such as a stroke,[7] brain injury,[8] hearing loss,[9] developmental delay,[10] a cleft palate,[11] cerebral palsy,[12] or emotional issues.[13]
A common misconception is that speech–language pathology is restricted to the treatment of articulation disorders (e.g., helping English-speaking individuals enunciate the traditionally difficult r) and/or the treatment of individuals who stutter but, in fact, speech–language pathology is concerned with a broad scope of speech, language, literacy, swallowing, and voice issues involved in communication,[14] some of which include:
- Word-finding and other semantic issues, either as a result of a specific language impairment (SLI) such as a language delay or as a secondary characteristic of a more general issue such as dementia.
- Social communication difficulties involving how people communicate or interact with others (pragmatics).
- Language impairments, including difficulties creating sentences that are grammatical (syntax) and modifying word meaning (morphology).
- Literacy impairments (reading and writing) related to the letter-to-sound relationship (phonics), the word-to-meaning relationship (semantics), and understanding the ideas presented in a text (reading comprehension).
- Voice difficulties, such as a raspy voice, a voice that is too soft, or other voice difficulties that negatively impact a person's social or professional performance.
- Cognitive impairments (e.g. attention, memory, executive function) to the extent that they interfere with communication.
- Parent, caregiver, and other communication partner coaching.
Primary pediatric speech and language disorders include: (i) receptive and (ii) expressive language disorders, (iii) speech sound disorders, (iv) childhood apraxia of speech (CAS), (v) stuttering, and (vi) language-based learning disabilities.[15] Speech-language pathologists (SLPs) work with people of all ages.[16]
Swallowing disorders include difficulties in any phase of the swallowing process (i.e., oral, pharyngeal, esophageal), as well as functional dysphagia and feeding disorders. Swallowing disorders can occur at any age and can stem from multiple causes.[14]
Multi-discipline collaboration[edit]
SLPs collaborate with other health care professionals, often working as part of a multidisciplinary team. They can provide information and referrals to audiologists, physicians, dentists, nurses, nurse practitioners, occupational therapists, rehabilitation psychologists, dietitians, educators, behavior consultants (applied behavior analysis), and parents as dictated by the individual client's needs. For example, the treatment for patients with cleft lip and palate often requires multidisciplinary collaboration. Speech–language pathologists can be very beneficial in helping resolve speech problems associated with cleft lip and palate. Research has indicated that children who receive early language intervention are less likely to develop compensatory error patterns later in life, although speech therapy outcomes are usually better when surgical treatment is performed earlier.[17] Another area of collaboration relates to auditory processing disorders,[18] where SLPs can collaborate in assessments and provide intervention where there is evidence of speech, language, and/or other cognitive-communication disorders.
Working environments[edit]
SLPs work in a variety of clinical and educational settings. SLPs work in public and private hospitals, private practices, skilled nursing facilities (SNFs), long-term acute care (LTAC) facilities, hospice,[19] and home healthcare. SLPs may also work as part of the support structure in the education system, working in both public and private schools, colleges, and universities.[20] Some SLPs also work in community health, providing services at prisons and young offenders' institutions or providing expert testimony in applicable court cases.[21]

Following ASHA's 2005 approval of the delivery of speech/language services via video conference or telepractice, SLPs in the United States have begun to use this service model.[22]
Children with speech, language, and communication needs (SLCN) are particularly at risk of not being heard because of communication challenges. Speech-language pathologists (SLPs) can explain the significance of supporting communication as a tool for the child to shape and influence choices available to them in their lives, even though it is advised that children with SLCN can and should be actively involved as equal partners in decision-making about their communication needs. Building these skills is especially crucial for SLPs working in settings related to traditional education.[23]
Research[edit]
SLPs conduct research related to communication sciences and disorders, swallowing disorders, or other upper aerodigestive functions.
Experimental, empirical, and scientific methodologies that build on hypothesis testing and logical, deductive reasoning have dominated research in speech-language pathology. Other types of research in the field are complemented by qualitative research, which has also led to new insights, techniques, and research methods as well as new approaches in ways that are responsive to our customers and communities.[24]
Education and training[edit]
United States[edit]
In the United States, speech–language pathologists must hold a master's degree from an ASHA-accredited program. Following graduation and passing a nation-wide board exam, SLPs typically begin their Clinical Fellowship Year, during which they are granted a provisional license and receive guidance from their supervisor. At the end of this process, SLPs may choose to apply for ASHA's Certificate of Clinical Competence and apply for full state licensure. SLPs may additionally choose to earn advanced degrees such as a clinical doctorate in speech–language pathology, PhD, or EdD.
Methods of assessment[edit]
Many approaches exist to assess language, communication, speech and swallowing. Two main aspects of assessment can be to determine the extent of breakdown (impairment-level), or how communication can be supported (functional level). When evaluating impairment-based level of breakdown, therapists are trained to use a cognitive neuropsychological approach to assessment, to precisely determine what aspect of communication is impaired. Some therapists use assessments that are based on historic anatomical models of language, that have since been shown to be unreliable. These tools are often preferred by therapists working within a medical model, where medics request a 'type' of impairment, and a 'severity' rating. The broad tools available allow clinicians to precisely select the aspect of communication that they wish to assess.
Because school-based speech therapy is run under state guidelines and funds, the process of assessment and qualification is more strict. To qualify for in-school speech therapy, students must meet the state's criteria on language testing and speech standardization. Due to such requirements, some students may not be assessed in an efficient time frame or their needs may be undermined by criteria. For a private clinic, students are more likely to qualify for therapy because it is a paid service with more availability.
Clients and patients[edit]
Speech–language pathologists work with clients and patients who may present with a wide range of issues.
Infants and children[edit]
- Premature infants are at higher risk of feeding and later language needs and SLTS work with this cohort to prevent and support development of https://www.rcslt.org/speech-and-language-therapy/clinical-information/neonatal-care/#section-2
- Infants with injuries due to complications at birth, feeding and swallowing difficulties, including dysphagia
- Children with mild, moderate or severe:
- Genetic disorders that adversely affect speech, language and/or cognitive development including cleft palate, Down syndrome, DiGeorge syndrome
- Attention deficit hyperactivity disorder[25][26]
- Autism spectrum disorders,[27] including Asperger syndrome[28]
- Developmental delay
- Feeding disorders, including oral motor deficits
- Cranial nerve damage
- Hearing loss
- Craniofacial anomalies that adversely affect speech, language and/or cognitive development
- Language delay
- Specific language impairment
- Specific difficulties in producing sounds, called articulation disorders, (including vocalic /r/ and lisps)
- Pediatric traumatic brain injury
- Developmental verbal dyspraxia
- Cleft palate[29]
United States[edit]
In the US, some children are eligible to receive speech therapy services, including assessment and lessons through the public school system. If not, private therapy is readily available through personal lessons with a qualified speech–language pathologist or the growing field of telepractice.[30] Teleconferencing tools such as Skype are being used more commonly as a means to access remote locations in private therapy practice, such as in the geographically diverse south island of New Zealand.[31] More at-home or combination treatments have become readily available to address specific types of articulation disorders. The use of mobile applications in speech therapy is also growing as an avenue to bring treatment into the home.
United Kingdom[edit]
In the UK, children are entitled to an assessment by local NHS speech- and language-therapy teams, usually after referral by health visitors or education settings, but parents are also entitled to request an assessment directly.[32] If treatment is appropriate, an educational plan will be drawn up. Speech therapists often play a role in multi-disciplinary teams when a child has speech delay or disorder as part of a wider health condition. The Children's Commissioner for England reported in June 2019 that there was a postcode lottery; £291.65 a year per head was spent on services in some areas, while the budget in some areas was £30.94 or less. In 2018, 193,971 children in English primary schools were on the special educational needs register needing speech-therapy services.[33] Speech and language therapists work in acute settings and are often integrated into the MDT in multiple areas of speciality for neonatal, children and adult services. Areas include but not limited to; neonatal care, respiratory, ENT, gastrointestinal, stroke, Neurology,ICU, oncology and geriatric care
Children and adults[edit]
- Puberphonia
- Neonatal care
- Respiratory
- ENT
- Cerebral palsy
- Head injury (Traumatic brain injury)
- Hearing loss and impairments
- Learning difficulties including
- Physical disabilities
- Speech disorders (such as oral dyspraxia)
- Stammering, stuttering (disfluency)
- Stroke
- Voice disorders (dysphonia)
- Language delay[37]
- Motor speech disorders (dysarthria or developmental verbal dyspraxia)
- Naming difficulties (anomia)
- Dysgraphia, agraphia
- Cognitive communication disorders
- Pragmatics
- Laryngectomies
- Tracheostomies
- Oncology (ear, nose or throat cancer)
Adults[edit]
- Adults with aphasia
- Adults with mild, moderate, or severe eating, feeding and swallowing difficulties, including dysphagia
- Adults recovering from significant tumors in the bronchus, lung, oropharynx, breast, and brain[38]
- Adults with mild, moderate, or severe language difficulties as a result of:
- Motor neuron diseases,
- Alzheimer's disease,
- Dementia,[39]
- Huntington's disease,
- Hearing loss
- Multiple sclerosis,
- Parkinson's disease,[40]
- Traumatic brain injury,
- Mental health issues
- Stroke
- Progressive neurological conditions such as cancer of the head, neck and throat (including laryngectomy)
- Aphasic[41]
- Adults seeking transgender-specific voice training, including voice feminization and voice masculinization[42]
See also[edit]
- All India Institute of Speech and Hearing (AIIMS)
- Applied linguistics
- Communicative disorders assistant
- List of university speech–language pathology departments
- List of voice disorders
- Motor theory of speech perception
- Neurolinguistics
- Online speech therapy
- Oral myology
- Origin of speech
- Speech acquisition
- Speech Buddies
- Speech perception
- Speech processing
- Speech repetition
References[edit]
- ^ Brady, Marian C.; Kelly, Helen; Godwin, Jon; Enderby, Pam; Campbell, Pauline (1 June 2016). "Speech and language therapy for aphasia following stroke". The Cochrane Database of Systematic Reviews. 2016 (6): CD000425. doi:10.1002/14651858.CD000425.pub4. hdl:1893/26112. ISSN 1469-493X. PMC 8078645. PMID 27245310.
- ^ "Speech and language therapy". RCSLT. Retrieved 27 January 2024.
- ^ Duchan, Judy (16 September 2021). "Judy Duchan's History of Speech-Language Pathology". Judy Duchan's History of Speech-Language Pathology. Retrieved 3 October 2022.
- ^ Duchan, Judith (1 December 2002). "What Do You Know About Your Profession's History? And Why Is It Important?". The ASHA Leader. 7 (23). doi:10.1044/leader.FTR.07232002.4 – via ASHAWire.
- ^ "Speech–Language Pathologists". ASHA.org. American Speech–Language–Hearing Association. Retrieved 6 April 2015.
- ^ Factor, Stewart; Weiner, William (2008). Parkinson's disease: Diagnosis & clinical management (2nd ed.). Demos Medical Publishing. pp. 77–83. ISBN 9781933864006.
- ^ Richards, Emma (June 2012). "Communication and swallowing problems after stroke". Nursing and Residential Care. 14 (6): 282–286. doi:10.12968/nrec.2012.14.6.282.
- ^ Zasler, Nathan D.; Katz, Douglas I.; Zafonte, Ross D.; Arciniegas, David B.; Bullock, M. Ross; Kreutzer, Jeffrey S., eds. (2013). Brain injury medicine principles and practice (2nd ed.). New York: Demos Medical. pp. 1086–1104, 1111–1117. ISBN 9781617050572.
- ^ Ching, Teresa Y. C. (2015). "Is early intervention effective in improving spoken language outcomes of children with congenital hearing loss?". American Journal of Audiology. 24 (3): 345–348. doi:10.1044/2015_aja-15-0007. PMC 4659415. PMID 26649545.
- ^ The Royal Children's Hospital, Melbourne. "Developmental Delay: An Information Guide for Parents" (PDF). The Royal Children's Hospital Melbourne. Retrieved 2 May 2016.
- ^ Bauman-Waengler, Jacqueline (2011). Articulatory and phonological impairments: a clinical focus (4th ed., International ed.). Harlow: Pearson Education. pp. 378–385. ISBN 9780132719957.
- ^ "Speech and Language Therapy". CerebralPalsy.org. Retrieved 2 May 2016.
- ^ Cross, Melanie (2011). Children with social, emotional and behavioural difficulties and communication problems: there is always a reason (2nd ed.). London: Jessica Kingsley Publishers.
- ^ a b "Scope of Practice in Speech–Language Pathology". American Speech-Language-Hearing Association. 2016. doi:10.1044/policy.SP2016-00343.
- ^ Weeks, Katie (12 July 2016). "Speech and Language Disorders". Speech SF.
- ^ "Who Are Speech–Language Pathologists, and What Do They Do?". ASHA.org. Retrieved 3 May 2018.
- ^ Frățilă, Mihaela; Urtilă, Emil; Ștefănescu, Maria (October 2011). "Logopedia — criteriu de stabilire a momentului operator în chirurgia despicăturilor labio-palato-velare" [Speech therapy — criteria for determining the time of the surgical operation in surgery of labio-palato-velars cleft]. Revista de chirurgie oro-maxilo-facială și implantologie (in Romanian). 2 (2): 21–23. Archived from the original on 10 November 2013.
- ^ DeBonis, David A.; Moncrieff, Deborah (February 2008). "Auditory Processing Disorders: An Update for Speech–Language Pathologists". American Journal of Speech-Language Pathology. 17 (1): 4–18. doi:10.1044/1058-0360(2008/002). PMID 18230810. S2CID 1520146.
- ^ Pollens, Robin (October 2004). "Role of the Speech–Language Pathologist in Palliative Hospice Care". Journal of Palliative Medicine. 7 (5): 694–702. doi:10.1089/jpm.2004.7.694. PMID 15588361.[needs update]
- ^ "Health Careers". Health Careers.
- ^ "Speech and language therapy". Royal College of Speech and Language Therapists.
- ^ "ASHA Telepractice Position Statement". ASHA.org. American Speech–Language–Hearing Association. Retrieved 15 April 2010.
- ^ Gallagher, Aoife L.; Tancredi, Haley; Graham, Linda J. (2018). "Advancing the human rights of children with communication needs in school". International Journal of Speech-Language Pathology. 20 (1): 128–132. doi:10.1080/17549507.2018.1395478. hdl:10344/7789. PMID 29143564. S2CID 3473633.
- ^ Hersh, Deborah (2022). "New perspectives, theory, method, and practice: Qualitative research and innovation in speech-language pathology". International Journal of Speech-Language Pathology. 24 (5): 449–459. doi:10.1080/17549507.2022.2029942. PMID 35172643. S2CID 246902770. Retrieved 10 October 2022.
- ^ Bellani, M.; Moretti, A.; Perlini, C.; Brambilla, P. (December 2011). "Language disturbances in ADHD". Epidemiology and Psychiatric Sciences. 20 (4): 311–315. doi:10.1017/S2045796011000527. PMID 22201208.
- ^ "International Statistical Classification of Diseases and Related Health Problems 10th Revision (ICD-10) Version for 2010". World Health Organisation. 2010.
- ^ "Autism and Communication [NIDCD Health Information]". www.nidcd.nih.gov. Archived from the original on 27 October 2011.
- ^ "Asperger Syndrome Fact Sheet: National Institute of Neurological Disorders and Stroke (NINDS)". www.ninds.nih.gov. Archived from the original on 5 December 2004. Retrieved 15 January 2022.
- ^ Ogata, Y. (1997). "The Speech Therapy of Cleft Palate Patients as an Oral Rehabilitation". Journal of Dentistry Indonesia. 4 (3): 46–47. doi:10.14693/jdi.v4i3.758 (inactive 31 January 2024).
{{cite journal}}: CS1 maint: DOI inactive as of January 2024 (link) - ^ "Telepractice for SLPs and Audiologists". American Speech–Language–Hearing Association. Retrieved 19 December 2018.
- ^ "Speech Therapy Wellington - Vocalsaints LTD". Vocalsaints. Retrieved 19 December 2018.
- ^ "Help your baby learn to talk". nhs.uk. 21 December 2017. Retrieved 19 December 2018.
- ^ "Postcode lottery for speech therapy, says commissioner". BBC News. 11 June 2019. Retrieved 20 July 2019.
- ^ Ritter, Michaela J. (June 2009). "The Speech–Language Pathologist and Reading: Opportunities to Extend Services for the Children We Serve". Perspectives on School-Based Issues. 10 (2): 38–44. doi:10.1044/sbi10.2.38.
- ^ "The Role of the Speech-Language Pathologist". dyslexiahelp.umich.edu.
- ^ Richard, Gail J. (July 2011). "The Role of the Speech–Language Pathologist in Identifying and Treating Children With Auditory Processing Disorder". Language, Speech, and Hearing Services in Schools. 42 (3): 241–245. doi:10.1044/0161-1461(2011/09-0090). PMID 21757563.
- ^ "Speech Therapy Wellington | Vocalsaints LTD". VocalSaints.
- ^ "BiblioBoard". openresearchlibrary.org. Retrieved 25 October 2023.
- ^ Bryan, Karen; Maxim, Jane (January 2002). "Letter to the Editor". International Journal of Language & Communication Disorders. 37 (2): 215–222. doi:10.1080/13682820110119205. PMID 12012617.
- ^ Schulz, Geralyn M; Grant, Megan K (January 2000). "Effects of speech therapy and pharmacologic and surgical treatments on voice and speech in Parkinson's disease". Journal of Communication Disorders. 33 (1): 59–88. doi:10.1016/s0021-9924(99)00025-8. PMID 10665513.
- ^ Wilkinson, Ray (3 July 2014). "Intervening With Conversation Analysis in Speech and Language Therapy: Improving Aphasic Conversation". Research on Language and Social Interaction. 47 (3): 219–238. doi:10.1080/08351813.2014.925659. S2CID 143521296.
- ^ Adler, Richard K.; Hirsch, Sandy; Mordaunt, Michelle (2012). Voice and Communication Therapy for the Transgender/Transsexual Client: A Comprehensive Clinical Guide. San Diego: Plural Publishing. ISBN 9781597564700.[page needed]
Further reading[edit]
- Fisher, S. E.; Scharff, C. (April 2009). "FOXP2 as a molecular window into speech and language". Trends in Genetics. 25 (4): 166–77. doi:10.1016/j.tig.2009.03.002. hdl:11858/00-001M-0000-0012-CA31-7. PMID 19304338.
- "Discussion Meeting Issue 'Language in developmental and acquired disorders: converging evidence for models of language representation in the brain' - Table of Contents". Royal Society Publishing. 2014. Retrieved 31 December 2013.
- Nelson, H. D. (1 February 2006). "Screening for Speech and Language Delay in Preschool Children: Systematic Evidence Review for the US Preventive Services Task Force". Pediatrics. 117 (2): e298–e319. doi:10.1542/peds.2005-1467. PMID 16452337.
- Howell, Peter (2011). Recovery from stuttering. New York: Psychology Press / Taylor Francis Group. ISBN 978-1-84872-916-2. OCLC 814245820.
- Janes, Tina Leann; Zupan, Barbra; Signal, Tania (2021–02). "Community awareness of speech pathology: A regional perspective". Australian Journal of Rural Health.[1]
External links[edit]
- American Speech–Language–Hearing Association (ASHA) – Communication for a Lifetime
- National Institutes of Health – Voice, Speech, and Language
- The Royal College of Speech and Language Therapists
- Speech-Language Pathologists – O*Net Online
- ^ Janes, Tina Leann; Zupan, Barbra; Signal, Tania (February 2021). "Community awareness of speech pathology: A regional perspective". Australian Journal of Rural Health. 29 (1): 61–70. doi:10.1111/ajr.12680. ISSN 1038-5282. PMID 33274537.
