Rimantadine
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Flumadine |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a698029 |
| Pregnancy category |
|
| Routes of administration | Oral |
| ATC code | |
| Legal status | |
| Legal status |
|
| Pharmacokinetic data | |
| Bioavailability | well absorbed |
| Protein binding | 40% |
| Metabolism | Hepatic hydroxylation and glucuronidation |
| Elimination half-life | 25.4 ± 6.3 hours |
| Excretion | Renal |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEMBL | |
| PDB ligand | |
| CompTox Dashboard (EPA) | |
| Chemical and physical data | |
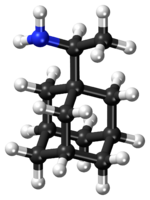
| Formula | C12H21N |
| Molar mass | 179.307 g·mol−1 |
| 3D model (JSmol) | |
| Chirality | Racemic mixture |
| |
| |
| (verify) | |
Rimantadine (INN, sold under the trade name Flumadine) is an orally administered antiviral drug[1] used to treat, and in rare cases prevent, influenzavirus A infection. When taken within one to two days of developing symptoms, rimantadine can shorten the duration and moderate the severity of influenza. Rimantadine can mitigate symptoms, including fever.[2] Both rimantadine and the similar drug amantadine are derivates of adamantane. Rimantadine is found to be more effective than amantadine because when used the patient displays fewer symptoms.[3] Rimantadine was approved by the Food and Drug Administration (FDA) in 1994.
Rimantadine was approved for medical use in 1993.[4] Seasonal H3N2 and 2009 pandemic flu samples tested have shown resistance to rimantadine, and it is no longer recommended to prescribe for treatment of the flu.[5]
Medical use[edit]
Influenza A[edit]
Rimantadine inhibits influenza activity by binding to amino acids in the M2 transmembrane channel and blocking proton transport across the M2 channel.[6] Rimantadine is believed to inhibit influenza's viral replication, possibly by preventing the uncoating of the virus's protective shells, which are the envelope and capsid. The M2 channel is known to be responsible for viral replication in the influenza virus. Genetic studies suggest that the virus M2 protein, an ion channel specified by virion M2 gene, plays an important role in the susceptibility of influenza A virus to inhibition by rimantadine.[citation needed]
Rimantadine is bound inside the pore to amantadine specific amino acid binding sites with hydrogen binding and van der Waals interactions.[7] The ammonium group (with neighboring water molecules) is positioned towards the C terminus with the amantadane group is positioned towards the N-terminus when bound inside the M2 pore.[citation needed]

Influenza resistance[edit]
Resistance to rimantadine can occur as a result of amino acid substitutions at certain locations in the transmembrane region of M2. This prevents binding of the antiviral to the channel.[8]
The mutation S31N binding site with rimantadine is shown in the image to the left. It shows rimantadine binding into lumenal (top) or peripheral (bottom) binding sites with influenza M2 channel Serine 31 (gold) or Asparagine 31 (blue).[citation needed]
Rimantadine enantiomers interactions with M2[edit]
Rimantadine, when sold as flumadine, is present as a racemic mixture; the R and S states are both present in the drug. Solid state NMR studies have shown that the R enantiomer has a stronger binding affinity to the M2 channel pore than the S-enantiomer of rimantadine.[9] Antiviral assay and electrophysiology studies show that there is no significant difference between the R and S enantiomers in binding affinity to amino acids in the M2 channel.[10] Since the enantiomers have similar binding affinity, they also have similar ability to block the channel pore and work as an effective antiviral.[citation needed] Rimantadine enantiomers R and S are pictured interacting with the M2 pore below to the right. This image shows that there is not a significant modeled difference between the R and S enantiomers.
Parkinson's disease[edit]
Rimantadine, like its antiviral cousin amantadine, possesses some NMDA antagonistic properties and is used as an antiparkinsonic drug (i.e., in the treatment of Parkinson's disease). However, in general, neither rimantadine nor amantadine is a preferred agent for this therapy and would be reserved for cases of the disease that are less responsive to front-line treatments.[citation needed]
Other[edit]
Rimantadine is shown to be effective against other RNA-containing viruses. It can treat arboviruses like Saint Louis encephalitis and Sindbis. Other viruses that can be treated with Rimantadine include respiratory synctial[check spelling] and parainfluenza viruses.[11] Rimantadine has also been shown to treat chronic hepatitis C.[12]
Drug interactions[edit]
- Taking paracetamol (acetaminophen, Tylenol) or acetylsalicylic acid (aspirin) while taking rimantadine is known to reduce the body's uptake of rimantadine by approximately 12%.[13]
- Cimetidine also affects the body's uptake of rimantadine.[citation needed]
- Taking anticholinergic drugs with amantadine may increase underlying seizure disorders and aggravate congestive heart failure.[14]
Side effects[edit]
Rimantadine can produce gastrointestinal and central nervous system adverse effects. Approximately 6% of patients (compared to 4% of patients taking a placebo) reported side-effects at a dosage of 200 mg/d.[15] Common side effects include:
- nausea
- upset stomach
- nervousness
- tiredness
- lightheadedness
- trouble sleeping (insomnia)
- difficulty concentrating
- confusion
- anxiety
Rimantadine shows fewer CNS symptoms than its sister drug Amantadine.[16]
Synthesis[edit]

1-carboxyadamatanones are reduced with sodium borohydride to create racemic hydroxy acid. Excess methyllithium is then added to create methyl ketones which when reduced with lithium aluminum hydride gives the amine group.[17]
The synthesis pictured to the left is a synthesis of rimantadine as synthesized in Europe.
History[edit]
Rimantadine was discovered in 1963[18][19] and patented in 1965 in the US by William W. Prichard in Du Pont & Co., Wilmington, Delaware (patent on new chemical compound U.S. patent 3,352,912, 1965 and on the first method of synthesis U.S. patent 3,592,934, 1967).[20][21] Prichard's methods of synthesis of rimantadine from the corresponding ketone oxime were based on its reduction with lithium aluminum hydride.[citation needed]
See also[edit]
References[edit]
- ^ Govorkova EA, Fang HB, Tan M, Webster RG (December 2004). "Neuraminidase inhibitor-rimantadine combinations exert additive and synergistic anti-influenza virus effects in MDCK cells". Antimicrobial Agents and Chemotherapy. 48 (12): 4855–63. doi:10.1128/AAC.48.12.4855-4863.2004. PMC 529183. PMID 15561867.
- ^ Zimmerman RK (March 2007). "Rationing of influenza vaccine during a pandemic: ethical analyses". Vaccine. 25 (11): 2019–26. doi:10.1016/j.vaccine.2006.11.045. PMID 17258359.
- ^ Jefferson T, Demicheli V, Di Pietrantonj C, Rivetti D, et al. (Cochrane Acute Respiratory Infections Group) (April 2006). "Amantadine and rimantadine for influenza A in adults". The Cochrane Database of Systematic Reviews. 2006 (2): CD001169. doi:10.1002/14651858.CD001169.pub3. PMC 7068158. PMID 16625539.
- ^ Long SS, Pickering LK, Prober CG (2012). Principles and Practice of Pediatric Infectious Disease. Elsevier Health Sciences. p. 1502. ISBN 978-1437727029.
- ^ Antiviral Agents for the Treatment and Chemoprophylaxis of Influenza: Recommendations of the Advisory Committee on Immunization Practices (ACIP)
- ^ Vorobjev YN (April 2020). "An effective molecular blocker of ion channel of M2 protein as anti-influenza A drug". Journal of Biomolecular Structure and Dynamics. 39 (7): 2352–2363. doi:10.1080/07391102.2020.1747550. ISSN 0739-1102. PMID 32212957. S2CID 214681984.
- ^ Drakopoulos A, Tzitzoglaki C, Ma C, Freudenberger K, Hoffmann A, Hu Y, et al. (February 2017). "Affinity of Rimantadine Enantiomers against Influenza A/M2 Protein Revisited". ACS Medicinal Chemistry Letters. 8 (2): 145–150. doi:10.1021/acsmedchemlett.6b00311. PMC 5312807. PMID 28217261.
- ^ Jing X, Ma C, Ohigashi Y, Oliveira FA, Jardetzky TS, Pinto LH, Lamb RA (August 2008). "Functional studies indicate amantadine binds to the pore of the influenza A virus M2 proton-selective ion channel". Proceedings of the National Academy of Sciences of the United States of America. 105 (31): 10967–72. Bibcode:2008PNAS..10510967J. doi:10.1073/pnas.0804958105. PMC 2492755. PMID 18669647.
- ^ Wright AK, Batsomboon P, Dai J, Hung I, Zhou HX, Dudley GB, Cross TA (February 2016). "Differential Binding of Rimantadine Enantiomers to Influenza A M2 Proton Channel". Journal of the American Chemical Society. 138 (5): 1506–9. doi:10.1021/jacs.5b13129. PMC 9328162. PMID 26804976.
- ^ Drakopoulos A, Tzitzoglaki C, Ma C, Freudenberger K, Hoffmann A, Hu Y, et al. (February 2017). "Affinity of Rimantadine Enantiomers against Influenza A/M2 Protein Revisited". ACS Medicinal Chemistry Letters. 8 (2): 145–150. doi:10.1021/acsmedchemlett.6b00311. PMC 5312807. PMID 28217261.
- ^ Zlydnikov DM, Kubar OI, Kovaleva TP, Kamforin LE (1981-05-01). "Study of rimantadine in the USSR: a review of the literature". Reviews of Infectious Diseases. 3 (3): 408–21. doi:10.1093/clinids/3.3.408. PMID 7025146.
- ^ Younossi ZM, Perrillo RP (1999). "The roles of amantadine, rimantadine, ursodeoxycholic acid, and NSAIDs, alone or in combination with alpha interferons, in the treatment of chronic hepatitis C". Seminars in Liver Disease. 19 (Suppl 1): 95–102. PMID 10349697.
- ^ "fda.gov". Food and Drug Administration. Archived from the original on June 30, 2005. Retrieved 2008-11-05.
- ^ Zimmerman RK (March 2007). "Rationing of influenza vaccine during a pandemic: ethical analyses". Vaccine. 25 (11): 2019–26. doi:10.1016/j.vaccine.2006.11.045. PMID 17258359.
- ^ "CDC - Influenza (Flu) | Antivirals: Side-Effects | REMOVED!". Retrieved 2008-11-05.
- ^ Zimmerman RK (March 2007). "Rationing of influenza vaccine during a pandemic: ethical analyses". Vaccine. 25 (11): 2019–26. doi:10.1016/j.vaccine.2006.11.045. PMID 17258359.
- ^ Manchand PS, Cerruti RL, Martin JA, Hill CH, Merrett JH, Keech E, et al. (July 1990). "Synthesis and antiviral activity of metabolites of rimantadine". Journal of Medicinal Chemistry. 33 (7): 1992–5. doi:10.1021/jm00169a029. PMID 2362279.
- ^ US patent 3352912 to W. W. Prichard
- ^ United States Patent № 4551552: Process for preparing rimantadine: Rimantadine and related compounds useful as antivirals were first described by Prichard in U.S. Pat. Nos. 3,352,912 and 3,592,934. Both patents describe the preparation of rimantadine from the corresponding ketone oxime by reduction with lithium aluminum hydride.
- ^ United States Patent № 4551552: Process for preparing rimantadine
- ^ Zlydnikov DM, Kubar OI, Kovaleva TP, Kamforin LE (1981). "Study of rimantadine in the USSR: a review of the literature". Reviews of Infectious Diseases. 3 (3): 408–21. doi:10.1093/clinids/3.3.408. PMID 7025146.
