Aripiprazole
 | |
 | |
| Clinical data | |
|---|---|
| Pronunciation | /ˌɛərɪˈpɪprəzoʊl/ AIR-ih-PIP-rə-zohl Abilify /əˈbɪlɪfaɪ/ ə-BIL-if-eye |
| Trade names | Abilify, Aristada, others |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a603012 |
| License data |
|
| Pregnancy category |
|
| Routes of administration | By mouth, intramuscular |
| Drug class | Atypical antipsychotic |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | 87%[4][5][6] |
| Protein binding | >99%[4][5][6] |
| Metabolism | Liver (mostly via CYP3A4 and 2D6[4][5][6]) |
| Elimination half-life | 75 hours (active metabolite is 94 hours)[4][5][6] |
| Excretion | Kidney (27%; <1% unchanged) feces (60%; 18% unchanged)[4][5][6] |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.112.532 |
| Chemical and physical data | |
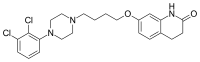
| Formula | C23H27Cl2N3O2 |
| Molar mass | 448.39 g·mol−1 |
| 3D model (JSmol) | |
| |
| |
| | |

Aripiprazole, sold under the brand names Abilify and Aristada, among others, is an atypical antipsychotic.[7] It is primarily used in the treatment of schizophrenia and bipolar disorder;[7] other uses include as an add-on treatment in major depressive disorder and obsessive compulsive disorder (OCD), tic disorders, and irritability associated with autism.[7] Aripiprazole is taken by mouth or via injection into a muscle.[7] A Cochrane review found low-quality evidence of effectiveness in treating schizophrenia.[8]
In adults, side effects with greater than 10% incidence include weight gain, headache, akathisia, insomnia, and gastrointestinal effects like nausea and constipation, and lightheadedness and twitching which is common in antidepressants and antipsychotics.[4][5][6][9][10] Side effects in children are similar, and include sleepiness, increased appetite, and stuffy nose.[9] Common side effects include vomiting, constipation, sleepiness, dizziness, weight gain and movement disorders.[7] Serious side effects may include neuroleptic malignant syndrome, tardive dyskinesia and anaphylaxis.[7] It is not recommended for older people with dementia-related psychosis due to an increased risk of death.[7] In pregnancy, there is evidence of possible harm to the fetus.[7][11] It is not recommended in women who are breastfeeding.[7] It has not been very well studied in people less than 18 years old.[7]
Aripiprazole was approved for medical use in the United States in 2002.[7] It is available as a generic medication.[12] In 2021, it was the 99th most commonly prescribed medication in the United States, with more than 6 million prescriptions.[13][14] It is on the World Health Organization's List of Essential Medicines.[15]
Medical uses[edit]
Aripiprazole is primarily used for the treatment of schizophrenia or bipolar disorder.[6][7][16]
Schizophrenia[edit]
The 2016 National Institute for Health and Care Excellence (NICE) guidance for treating psychosis and schizophrenia in children and young people recommended aripiprazole as a second line treatment after risperidone for people between 15 and 17 who are having an acute exacerbation or recurrence of psychosis or schizophrenia.[17] A 2014 NICE review of the depot formulation of the drug found that it might have a role in treatment as an alternative to other depot formulations of second generation antipsychotics for people who have trouble taking medication as directed or who prefer it.[18]
A 2014 Cochrane review comparing aripiprazole and other atypical antipsychotics found that it is difficult to determine differences as data quality is poor.[19] A 2011 Cochrane review comparing aripiprazole with placebo concluded that high dropout rates in clinical trials, and a lack of outcome data regarding general functioning, behavior, mortality, economic outcomes, or cognitive functioning make it difficult to definitively conclude that aripiprazole is useful for the prevention of relapse.[8] A Cochrane review found only low quality evidence of effectiveness in treating schizophrenia.[8] Accordingly, part of its methodology on quality of evidence is based on quantity of qualified studies.[20]
A 2013 review placed aripiprazole in the middle range of 15 antipsychotics for effectiveness, approximately as effective as haloperidol and quetiapine[21] and slightly more effective than ziprasidone, chlorpromazine, and asenapine, with better tolerability compared to the other antipsychotic drugs (4th best for reducing weight gain, 5th best for reducing extrapyramidal symptoms, best for reducing prolactin levels, 2nd best for prolongated QTc interval, and 5th best for sedative symptoms). The authors concluded that for acute psychotic episodes aripiprazole results in benefits in some aspects of the condition.[22]
In 2013 the World Federation of Societies for Biological Psychiatry recommended aripiprazole for the treatment of acute exacerbations of schizophrenia as a Grade 1 recommendation and evidence level A.[23]
The British Association for Psychopharmacology similarly recommends that all persons presenting with psychosis receive treatment with an antipsychotic, and that such treatment should continue for at least 1–2 years, as "There is no doubt that antipsychotic discontinuation is strongly associated with relapse during this period". The guideline further notes that "Established schizophrenia requires continued maintenance with doses of antipsychotic medication within the recommended range (Evidence level A)".[24]
The British Association for Psychopharmacology[24] and the World Federation of Societies for Biological Psychiatry suggest that there is little difference in effectiveness between antipsychotics in prevention of relapse, and recommend that the specific choice of antipsychotic be chosen based on each person's preference and side effect profile. The latter group recommends switching to aripiprazole when excessive weight gain is encountered during treatment with other antipsychotics.[23]
Bipolar disorder[edit]
Aripiprazole is effective for the treatment of acute manic episodes of bipolar disorder in adults, children, and adolescents.[25][26] Used as maintenance therapy, it is useful for the prevention of manic episodes, but is not useful for bipolar depression.[27][28] Thus, it is often used in combination with an additional mood stabilizer; however, co-administration with a mood stabilizer increases the risk of extrapyramidal side effects.[29] In September 2014, aripiprazole had a UK marketing authorization for up to twelve weeks of treatment for moderate to severe manic episodes in bipolar I disorder in young people aged thirteen and older. Aripiprazole in low doses of 2.5 mg can cause mania in those with Bipolar disorder. [30][31][32]
Major depression[edit]
Aripiprazole is an effective add-on treatment for major depressive disorder; however, there is a greater rate of side effects such as weight gain and movement disorders.[33][34][35] The overall benefit is small to moderate and its use appears to neither improve quality of life nor functioning.[33] Aripiprazole may interact with some antidepressants, especially selective serotonin reuptake inhibitors (SSRIs) that are metabolized by CYP2D6. There are known interactions with fluoxetine and paroxetine[36] and it appears lesser interactions with sertraline, escitalopram, citalopram and fluvoxamine. CYP2D6 inhibitors increase aripiprazole concentrations to 2–3 times their normal level.[9] When strong CYP2D6 SSRIs (such as fluoxetine, paroxetine) are co-administered, the FDA recommends dose monitoring, although it is not clear the SSRI dose should be lowered.[16][37][38][39]
Autism[edit]
Short-term data (8 weeks) shows reduced irritability, hyperactivity, inappropriate speech, and stereotypy, but no change in lethargic behaviours.[40] Adverse effects include weight gain, sleepiness, drooling and tremors.[40] It is suggested that children and adolescents need to be monitored regularly while taking this medication, to evaluate if this treatment option is still effective after long-term use and note if side effects are worsening. Further studies are needed to understand if this drug is helpful for children after long term use.[40]
Tic disorders[edit]
Aripiprazole is approved for the treatment of Tourette's syndrome and tic disorders.[41][42][43] It is effective, safe, and well-tolerated for this use per systematic reviews and meta-analyses.[44][45][46][47]
Obsessive–compulsive disorder[edit]
A 2014 systematic review and meta-analysis concluded that add-on therapy with low dose aripiprazole is an effective treatment for obsessive–compulsive disorder (OCD) that does not improve with selective serotonin reuptake inhibitors (SSRIs) alone.[48] The conclusion was based on the results of two relatively small, short-term trials, each of which demonstrated improvements in symptoms.[48][49][50][51] However, aripiprazole is cautiously recommended by a 2017 review on antipsychotics for OCD.[52] Aripiprazole is not currently approved for the treatment of OCD and is instead used off-label for this indication.[41] Depending on the dose, aripiprazole can increase impulse control issues in a small percentage of people. FDA Drug Safety Communication warned about this side effect.[53]
Adverse effects[edit]
In the elderly with dementia, there is an increased risk of death.[54] In children, adolescents and young adults, there is an increased risk of suicide.[54][55]
In adults, side effects with greater than 10% incidence include weight gain, mania, headache, akathisia, insomnia, delirium, and gastro-intestinal effects like nausea and constipation, and lightheadedness.[4][5][6][9][10] Side effects in children are similar, and include sleepiness, increased appetite, and stuffy nose.[9] A strong desire to gamble, binge eat, shop, and engage in sexual activity may also occur rarely.[56][57] These urges can be uncontrollable.[56]
Uncontrolled movement such as restlessness, tremors, and muscle stiffness may occur.[9]
Discontinuation[edit]
The British National Formulary recommends a gradual withdrawal when discontinuing antipsychotics to avoid acute withdrawal syndrome or rapid relapse.[58] Symptoms of withdrawal commonly include nausea, vomiting, and loss of appetite.[59] Other symptoms may include restlessness, increased sweating, and trouble sleeping.[59] Less commonly there may be a feeling of the world spinning, numbness, or muscle pains.[59] Symptoms generally resolve after a short period of time.[59]
There is tentative evidence that discontinuation of antipsychotics can result in psychosis as a part of a withdrawal syndrome.[60] It may also result in reoccurrence of the condition that is being treated.[61] Rarely tardive dyskinesia can occur when the medication is stopped.[59]
Overdose[edit]
Children or adults who ingested acute overdoses have usually manifested central nervous system depression ranging from mild sedation to coma; serum concentrations of aripiprazole and dehydroaripiprazole in these people were elevated by up to 3–4 fold over normal therapeutic levels; as of 2008 no deaths had been recorded.[62][63]
Interactions[edit]
Aripiprazole is a substrate of CYP2D6 and CYP3A4. Coadministration with medications that inhibit (e.g. paroxetine, fluoxetine) or induce (e.g. carbamazepine) these metabolic enzymes are known to increase and decrease, respectively, plasma levels of aripiprazole.[64][16]
Precautions should be taken in people with an established diagnosis of diabetes mellitus who are started on atypical antipsychotics along with other medications that affect blood sugar levels and should be monitored regularly for worsening of glucose control. The liquid form (oral solution) of this medication may contain up to 15 grams of sugar per dose.[7]
Antipsychotics like aripiprazole and stimulant medications, such as amphetamine, are traditionally thought to have opposing effects to their effects on dopamine receptors: stimulants are thought to increase dopamine in the synaptic cleft, whereas antipsychotics are thought to decrease dopamine. However, it is an oversimplification to state the interaction as such, due to the differing actions of antipsychotics and stimulants in different parts of the brain, as well as the effects of antipsychotics on non-dopaminergic receptors. This interaction frequently occurs in the setting of comorbid attention-deficit hyperactivity disorder (ADHD) (for which stimulants are commonly prescribed) and off-label treatment of aggression with antipsychotics. Aripiprazole has been reported to provide some benefit in improving cognitive functioning in people with ADHD without other psychiatric comorbidities, though the results have been disputed. The combination of antipsychotics like aripiprazole with stimulants should not be considered an absolute contraindication.[65]
Chemistry[edit]
Aripiprazole belongs to the chemical class of drugs called 2,3-dichlorophenylpiperazines and is chemically related to cariprazine, nefazodone, etoperidone, and trazodone.[66][67] It is unusual in having twelve known crystalline polymorphs.[68][69]
Pharmacology[edit]
Pharmacodynamics[edit]
Aripiprazole was discovered in 1988 by scientists at the Japanese firm Otsuka Pharmaceutical.[41][70][71][72][73]
| Site | Ki (nM) | IA (%) | Action | Ref |
|---|---|---|---|---|
| SERT | 900 – 1260 | Reuptake Inhibitor | [77][75] | |
| NET | 1340 – 2840 | Reuptake inbibitor | [75] | |
| DAT | 2560 – 3880 | Reuptake inhibitor | [75] | |
| 5-HT1A | 1.7 – 6.4 | ~75% | Partial agonist | [75][78][77] |
| 5-HT1B | 570 – 1090 | ND | [75] | |
| 5-HT1D | 57 – 79 | ND | [75] | |
| 5-HT1E | 3000 – >10,000 | ND | [75] | |
| 5-HT2A | 6.7 – 39 | 12.7% | Partial Agonist /
Functional Antagonist |
[77][75][78] |
| 5-HT2B | 0.25 – 0.47 | Inverse agonist | [75] | |
| 5-HT2C | 11 – 197 | 82% | Partial agonist | [77][75][78] |
| 5-HT3 | 520 – 740 | ND | [75] | |
| 5-HT5A | 960 – 1520 | Full Agonist | [75] | |
| 5-HT6 | 475 – 665 | Antagonist | [77][75][78] | |
| 5-HT7 | 6.6 – 14 | Partial Agonist /
Functional Antagonist |
[75][78][77] | |
| α1A | 26 | Antagonist | [75][78] | |
| α1B | 35 | Antagonist | [75] | |
| α2A | 74.3 | Antagonist | [75][78] | |
| α2B | 102 | ND | [75][78] | |
| α2C | 38 | Antagonist | [75][78] | |
| β1 | 141 | ND | [75] | |
| β2 | 163 | ND | [75] | |
| D1 | 1290 – 2630 | Antagonist | [77][75] | |
| D2 | 2.2 – 4.4 | ~60% | Partial agonist | [75] |
| D2L | 0.65 – 0.83 | Antagonist | ||
| D3 | 4.3 – 15.1 | ~30% | Partial agonist | [77][75] |
| D4 | 417 – 603 | Partial agonist | [77][75] | |
| D5 | 1240 – 3940 | ND | [77][75] | |
| H1 | 22.5 – 27.7 | Antagonist | [75][78][77] | |
| H2 | >10,000 | ND | [75] | |
| H3 | 60 – 388 | ND | [75] | |
| H4 | >10,000 | ND | [75] | |
| M1 | 6,780 | ND | [75] | |
| M2 | 3,510 | ND | [75] | |
| M3 | 4,680 | ND | [75][78] | |
| M4 | 1,520 | ND | [75] | |
| M5 | 2,330 | ND | [75] | |
| NMDA (PCP1) |
59 – 1824 | Antagonist | [75] | |
| Values are Ki (nM). The smaller the value, the more strongly the drug binds to the site. All data are for human cloned proteins, except 5-HT3 (rat), D4 (human/rat), H3 (guinea pig), and NMDA/PCP (rat).[75]
IA = Intrinsic Activity | ||||
Aripiprazole's mechanism of action is different from those of the other FDA-approved atypical antipsychotics (e.g., clozapine, olanzapine, quetiapine, ziprasidone, and risperidone).[79][80][81][82] It shows differential engagement at the dopamine receptor (D2[75]). Aripiprazole is a partial agonist at dopamine D2 receptors, partial agonist at 5-HT1A receptors and an antagonist at 5-HT2A, receptors.[83][84]
It appears to show predominantly antagonist activity on postsynaptic D2 receptors and partial agonist activity on presynaptic D2 receptors,[85] D3,[75][86][87] and partially D4[75][80] and is a partial activator of serotonin (5-HT1A,[75][88][89] 5-HT2A,[75] 5-HT2B,[75] 5-HT6, and 5-HT7).[75][82] It also shows lower and likely insignificant effect on histamine (H1), epinephrine/norepinephrine (α), and otherwise dopamine (D4), as well as the serotonin transporter.[75][80] Aripiprazole acts by modulating neurotransmission overactivity of dopamine, which is thought to mitigate schizophrenia symptoms.[90]
There are studies to date confirming aripiprazole as an antagonist at alpha-adrenergic receptors such as α1A, α2A and α2C, the orthostatic hypotension observed with aripiprazole may be explained by its antagonist activity at adrenergic α1A receptors.[91]
As a pharmacologically unique antipsychotic with pronounced functional selectivity, characterization of this dopamine D2 partial agonist (with an intrinsic activity of ~25%)[92] as being similar to a full agonist but at a reduced level of activity presents a misleading oversimplification of its actions; for example, among other effects, aripiprazole has been shown, in vitro, to bind to and/or induce receptor conformations (i.e., facilitate receptor shapes) in such a way as to not only prevent receptor internalization (and, thus, lower receptor density) but even to lower the rate of receptor internalization below that of neurons not in the presence of agonists (including dopamine) or antagonists.[93] It is often the nature of partial agonists, including aripiprazole, to display a stabilizing effect (such as on mood in this case) with agonistic activity when there are low levels of endogenous neurotransmitters (such as dopamine) and antagonistic activity in the presence of high levels of agonists associated with events such as mania, psychosis, and drug use. In addition to aripiprazole's partial agonism and functional selectivity characteristics, its effectiveness may be mediated by its very high dopamine D2 receptor occupancy (approximately 32%, 53%, 72%, 80%, and 97% at daily dosages of 0.5 mg, 1 mg, 2 mg, 10 mg, and 40 mg respectively)[94][95] as well as balanced selectivity for pre- and postsynaptic receptors (as suggested by its equal affinity for both D2S and D2L receptor forms).[96] Aripiprazole has been characterized as possessing predominantly antagonistic activity on postsynaptic D2 receptors and partial agonist activity on presynaptic D2 receptors;[85] however, while this explanation intuitively explains the drug's efficacy as an antipsychotic, as degree of agonism is a function of more than a drug's inherent properties as well as in vitro demonstration of aripiprazole's partial agonism in cells expressing postsynaptic (D2L) receptors, it was noted that "It is unlikely that the differential actions of aripiprazole as an agonist, antagonist, or partial agonist were entirely due to differences in relative D2 receptor expression since aripiprazole was an antagonist in cells with the highest level of expression (4.6 pmol/mg) and a partial agonist in cells with an intermediate level of expression (0.5–1 pmol/mg). Instead, the current data are most parsimoniously explained by the "functional selectivity" hypothesis of Lawler et al. (1999)".[97] Aripiprazole is also a partial agonist of the D3 receptor.[75] In healthy human volunteers, D2 and D3 receptor occupancy levels are high, with average levels ranging between approximately 71% at 2 mg/day to approximately 96% at 40 mg/day.[86][87] Most atypical antipsychotics bind preferentially to extrastriatal receptors, but aripiprazole appears to be less preferential in this regard, as binding rates are high throughout the brain.[98]
Aripiprazole is also a partial agonist of the serotonin 5-HT1A receptor (intrinsic activity = 68%).[75][88][89] Casting doubt on the significance of aripiprazole's agonism of 5-HT1A receptors, a PET scan study of 12 patients receiving doses ranging from 10 to 30 mg found 5-HT1A receptor occupancy to be only 16% compared to ~90% for D2.[89] It is a very weak partial agonist of the 5-HT2A receptor (intrinsic activity = 12.7%),[75] and like other atypical antipsychotics, displays a functional antagonist profile at this receptor.[75] The drug differs from other atypical antipsychotics in having higher affinity for the D2 receptor than for the 5-HT2A receptor.[89] At the 5-HT2B receptor, aripiprazole has both great binding affinity and acts as a potent inverse agonist, "Aripiprazole decreased PI hydrolysis from a basal level of 61% down to a low of 30% at 1000 nM, with an EC50 of 11 nM".[75] Unlike other antipsychotics, aripiprazole is a high-efficacy partial agonist of the 5-HT2C receptor (intrinsic activity = 82%) and with relatively weak affinity;[75] this property may underlie the minimal weight gain seen in the course of therapy.[99] At the 5-HT7 receptor, aripiprazole is a very weak partial agonist with barely measurable intrinsic activity, and hence is a functional antagonist of this receptor.[75][82] Aripiprazole also shows lower but likely clinically insignificant affinity for a number of other sites, such as the histamine H1, α-adrenergic, and dopamine D4 receptors as well as the serotonin transporter, while it has negligible affinity for the muscarinic acetylcholine receptors.[75][80]
Since the actions of aripiprazole differ markedly across receptor systems aripiprazole was sometimes an antagonist (e.g., at 5-HT6 and D2L), sometimes an inverse agonist (e.g., 5-HT2B), sometimes a partial agonist (e.g., D2L), and sometimes a full agonist (D3, D4). Aripiprazole was frequently found to be a partial agonist, with an intrinsic activity that could be low (D2L, 5-HT2A, 5-HT7), intermediate (5-HT1A), or high (D4, 5-HT2C). This mixture of agonist actions at D2-dopamine receptors is consistent with the hypothesis that aripiprazole has "functionally selective" actions.[100] The "functional-selectivity" hypothesis proposes that a mixture of agonist/partial agonist/antagonist actions are likely. According to this hypothesis, agonists may induce structural changes in receptor conformations that are differentially "sensed" by the local complement of G proteins to induce a variety of functional actions depending upon the precise cellular milieu. The diverse actions of aripiprazole at D2-dopamine receptors are clearly cell-type specific (e.g., agonism, antagonism, partial agonism), and are most parsimoniously explained by the "functional selectivity" hypothesis.[75]
Since 5-HT2C receptors have been implicated in the control of depression, OCD, and appetite, partial agonism at the 5-HT2C receptor might be associated with therapeutic potential in obsessive compulsive disorder, obesity, and depression. 5-HT2C agonism has been demonstrated to induce anorexia via enhancement of serotonergic neurotransmission via activation of 5-HT2C receptors; it is conceivable that the 5-HT2C partial agonist actions of aripiprazole may, thus, be partly responsible for the minimal weight gain associated with this compound in clinical trials. In terms of potential action as an antiobsessional agent, it is worthwhile noting that a variety of 5-HT2A/5-HT2C agonists have shown promise as antiobsessional agents, yet many of these compounds are hallucinogenic, presumably due to 5-HT2A activation. Aripiprazole has a favorable pharmacological profile in being a 5-HT2A antagonist and a 5-HT2C partial agonist. Based on this profile, one can predict that aripiprazole may have antiobsessional and anorectic actions in humans.[75]
Wood and Reavill's (2007) review of published and unpublished data proposed that, at therapeutically relevant doses, aripiprazole may act essentially as a selective partial agonist of the D2 receptor without significantly affecting the majority of serotonin receptors.[85] A positron emission tomography imaging study found that 10 to 30 mg/day aripiprazole resulted in 85 to 95% occupancy of the D2 receptor in various brain areas (putamen, caudate, ventral striatum) versus 54 to 60% occupancy of the 5-HT2A receptor and only 16% occupancy of the 5-HT1A receptor.[101][89] It has been suggested that the low occupancy of the 5-HT1A receptor by aripiprazole may have been an erroneous measurement however.[102]
Aripiprazole acts by modulating neurotransmission overactivity on the dopaminergic mesolimbic pathway, which is thought to be a cause of positive schizophrenia symptoms.[90] Due to its agonist activity on D2 receptors, aripiprazole may also increase dopaminergic activity to optimal levels in the mesocortical pathways where it is reduced.[90]
Pharmacokinetics[edit]
Aripiprazole displays linear kinetics and has an elimination half-life of approximately 75 hours. Steady-state plasma concentrations are achieved in about 14 days. Cmax (maximum plasma concentration) is achieved 3–5 hours after oral dosing. Bioavailability of the oral tablets is about 90% and the drug undergoes extensive hepatic metabolization (dehydrogenation, hydroxylation, and N-dealkylation), principally by the enzymes CYP2D6 and CYP3A4. Its only known active metabolite is dehydro-aripiprazole, which typically accumulates to approximately 40% of the aripiprazole concentration. The parenteral drug is excreted only in traces, and its metabolites, active or not, are excreted via feces and urine.[80][16]
| Medication | Brand name | Class | Vehicle | Dosage | Tmax | t1/2 single | t1/2 multiple | logPc | Ref |
|---|---|---|---|---|---|---|---|---|---|
| Aripiprazole lauroxil | Aristada | Atypical | Watera | 441–1064 mg/4–8 weeks | 24–35 days | ? | 54–57 days | 7.9–10.0 | |
| Aripiprazole monohydrate | Abilify Maintena | Atypical | Watera | 300–400 mg/4 weeks | 7 days | ? | 30–47 days | 4.9–5.2 | |
| Bromperidol decanoate | Impromen Decanoas | Typical | Sesame oil | 40–300 mg/4 weeks | 3–9 days | ? | 21–25 days | 7.9 | [103] |
| Clopentixol decanoate | Sordinol Depot | Typical | Viscoleob | 50–600 mg/1–4 weeks | 4–7 days | ? | 19 days | 9.0 | [104] |
| Flupentixol decanoate | Depixol | Typical | Viscoleob | 10–200 mg/2–4 weeks | 4–10 days | 8 days | 17 days | 7.2–9.2 | [104][105] |
| Fluphenazine decanoate | Prolixin Decanoate | Typical | Sesame oil | 12.5–100 mg/2–5 weeks | 1–2 days | 1–10 days | 14–100 days | 7.2–9.0 | [106][107][108] |
| Fluphenazine enanthate | Prolixin Enanthate | Typical | Sesame oil | 12.5–100 mg/1–4 weeks | 2–3 days | 4 days | ? | 6.4–7.4 | [107] |
| Fluspirilene | Imap, Redeptin | Typical | Watera | 2–12 mg/1 week | 1–8 days | 7 days | ? | 5.2–5.8 | [109] |
| Haloperidol decanoate | Haldol Decanoate | Typical | Sesame oil | 20–400 mg/2–4 weeks | 3–9 days | 18–21 days | 7.2–7.9 | [110][111] | |
| Olanzapine pamoate | Zyprexa Relprevv | Atypical | Watera | 150–405 mg/2–4 weeks | 7 days | ? | 30 days | – | |
| Oxyprothepin decanoate | Meclopin | Typical | ? | ? | ? | ? | ? | 8.5–8.7 | |
| Paliperidone palmitate | Invega Sustenna | Atypical | Watera | 39–819 mg/4–12 weeks | 13–33 days | 25–139 days | ? | 8.1–10.1 | |
| Perphenazine decanoate | Trilafon Dekanoat | Typical | Sesame oil | 50–200 mg/2–4 weeks | ? | ? | 27 days | 8.9 | |
| Perphenazine enanthate | Trilafon Enanthate | Typical | Sesame oil | 25–200 mg/2 weeks | 2–3 days | ? | 4–7 days | 6.4–7.2 | [112] |
| Pipotiazine palmitate | Piportil Longum | Typical | Viscoleob | 25–400 mg/4 weeks | 9–10 days | ? | 14–21 days | 8.5–11.6 | [105] |
| Pipotiazine undecylenate | Piportil Medium | Typical | Sesame oil | 100–200 mg/2 weeks | ? | ? | ? | 8.4 | |
| Risperidone | Risperdal Consta | Atypical | Microspheres | 12.5–75 mg/2 weeks | 21 days | ? | 3–6 days | – | |
| Zuclopentixol acetate | Clopixol Acuphase | Typical | Viscoleob | 50–200 mg/1–3 days | 1–2 days | 1–2 days | 4.7–4.9 | ||
| Zuclopentixol decanoate | Clopixol Depot | Typical | Viscoleob | 50–800 mg/2–4 weeks | 4–9 days | ? | 11–21 days | 7.5–9.0 | |
| Note: All by intramuscular injection. Footnotes: a = Microcrystalline or nanocrystalline aqueous suspension. b = Low-viscosity vegetable oil (specifically fractionated coconut oil with medium-chain triglycerides). c = Predicted, from PubChem and DrugBank. Sources: Main: See template. | |||||||||
History[edit]

Aripiprazole was discovered by scientists at Otsuka Pharmaceutical and was called OPC-14597.[41][113] It was first published in 1995.[113][114] Otsuka initially developed the drug, and partnered with Bristol-Myers Squibb (BMS) in 1999 to complete development, obtain approvals, and market aripiprazole.[115]
It was approved by the US Food and Drug Administration (FDA) for schizophrenia in November 2002, and by the European Medicines Agency in June 2004;[116] for acute manic and mixed episodes associated with bipolar disorder on 1 October 2004; as an adjunct for major depressive disorder on 20 November 2007;[117] and to treat irritability in children with autism on 20 November 2009.[118] Likewise it was approved for use as a treatment for schizophrenia by the TGA of Australia in May 2003.[9]
Aripiprazole has been approved by the FDA for the treatment of both acute manic and mixed episodes, in people older than ten years.[119]
In 2006, the FDA required manufacturers to add a black box warning to the label, warning that older people who were given the drug for dementia-related psychosis were at greater risk of death.[120]
In 2007, aripiprazole was approved by the FDA for the treatment of unipolar depression when used adjunctively with an antidepressant medication.[16] That same year, BMS settled a case with the US government in which it paid $515 million; the case covered several drugs but the focus was on BMS's off-label marketing of aripiprazole for children and older people with dementia.[121]
In 2011 Otsuka and Lundbeck signed a collaboration to develop a depot formulation of aripiprazole.[122]
As of 2013, Abilify had annual sales of US$7 billion.[123] In 2013 BMS returned marketing rights to Otsuka, but kept manufacturing the drug.[124] Also in 2013, Otsuka and Lundbeck received US and European marketing approval for an injectable depot formulation of aripiprazole.[125][126]
Otsuka's US patent on aripiprazole expired on 20 October 2014, but due to a pediatric extension, a generic did not become available until 20 April 2015.[119] Barr Laboratories (now Teva Pharmaceuticals) initiated a patent challenge under the Hatch-Waxman Act in March 2007.[127] On 15 November 2010, this challenge was rejected by the U.S. District Court in New Jersey.[128]
Otsuka's European patent EP0367141 which would have expired on 26 October 2009, was extended by a Supplementary Protection Certificate (SPC) to 26 October 2014.,[129] The UK Intellectual Property Office decided[130] on 4 March 2015 that the SPC could not be further extended by six months under Regulation (EC) No 1901/2006. Even if the decision is successfully appealed, protection in Europe will not extend beyond 26 April 2015.
From April 2013 to March 2014, sales of Abilify amounted to almost $6.9 billion.[131]
In April 2015, the FDA announced the first generic versions.[132][133] In October 2015, aripiprazole lauroxil, a prodrug of aripiprazole that is administered via intramuscular injection once every four to six weeks for the treatment of schizophrenia, was approved by the FDA.[134][135]
In 2016, BMS settled cases with 42 US states that had charged BMS with off-label marketing to older people with dementia; BMS agreed to pay $19.5 million.[120][136]
In November 2017, the FDA approved Abilify MyCite, a digital pill containing a sensor intended to record when its consumer takes their medication.[137][138]
Aripiprazole was approved by the FDA for the treatment of bipolar disorder 1 and schizophrenia on April 27, 2023.[139][140]
In 2024, the European Commission approved apripiprazole for the maintenance treatment of schizophrenia.[141]
Society and culture[edit]
Legal status[edit]
| Regulatory administration (country)[142][143][144] | Schizophrenia | Acute mania | Bipolar maintenance | Major depressive disorder (as an adjunct) | Irritability in autism |
|---|---|---|---|---|---|
| Food and Drug Administration (US) | Yes | Yes | Yes (as an adjunct to lithium/valproate) | Yes | Yes (children and adolescents) |
| Therapeutic Goods Administration (AU) | Yes | Yes (as an adjunct to lithium/valproate) | Yes | No | No |
| Medicines and Healthcare products Regulatory Agency (UK) | Yes | Yes | Yes (to prevent mania) | No | No |
Classification[edit]
Aripiprazole has been described as the prototypical third-generation antipsychotic, as opposed to first-generation (typical) antipsychotics like haloperidol and second-generation (atypical) antipsychotics like clozapine.[145] It has received this classification due to its partial agonism of dopamine receptors, and is the first of its kind in this regard among antipsychotics, which before aripiprazole acted only as dopamine receptor antagonists.[145] The introduction of aripiprazole has led to a paradigm shift from a dopamine antagonist-based approach to a dopamine agonist-based approach for antipsychotic drug development.[145][146]
Brand names[edit]
- Abilify
- Aristada
- Arip MT
- Explemed
- Arivitae
Research[edit]
Attention deficit hyperactivity disorder[edit]
Aripiprazole was under development for the treatment of attention-deficit hyperactivity disorder (ADHD), but development for this indication was discontinued.[41] A 2017 meta review found only preliminary evidence (studies with small sample sizes and methodological problems) for aripiprazole in the treatment of ADHD.[147] A 2013 systematic review of aripiprazole for ADHD similarly reported that there is insufficient evidence of effectiveness to support aripiprazole as a treatment for the condition.[148] Although all 6 non-controlled open-label studies in the review reported effectiveness, two small randomized controlled trials found that aripiprazole did not significantly decrease ADHD symptoms.[148] A high rate of adverse effects with aripiprazole such as weight gain, sedation, and headache was noted.[148] Most research on aripiprazole for ADHD is in children and adolescents.[148][147] Evidence on aripiprazole specifically for adult ADHD appears to be limited to a single case report.[149][150]
Substance dependence[edit]
Aripiprazole has been studied for the treatment of amphetamine dependence and other substance use disorders, but more research is needed to support aripiprazole for these potential uses.[151][152][153][154] Available evidence of aripiprazole for amphetamine dependence is mixed.[151][152][153][154] Some studies have reported attenuation of the effects of amphetamines by aripiprazole, whereas other studies have reported both enhancement of the effects of amphetamines and increased use of amphetamines by aripiprazole.[151][152][153][154] As such, aripiprazole may not only be ineffective but potentially harmful for treatment of amphetamine dependence, and caution is warranted with regard to its use for such purposes.[151][152][153][154]
Other uses[edit]
Aripiprazole is under development for the treatment of agitation and pervasive child development disorders.[41] As of May 2021, it is in phase 3 clinical trials for these indications.[41]
References[edit]
- ^ "Aripiprazole Use During Pregnancy". Drugs.com. 22 August 2019. Retrieved 7 February 2020.
- ^ "FDA-sourced list of all drugs with black box warnings (Use Download Full Results and View Query links.)". nctr-crs.fda.gov. FDA. Retrieved 22 October 2023.
- ^ Anvisa (31 March 2023). "RDC Nº 784 - Listas de Substâncias Entorpecentes, Psicotrópicas, Precursoras e Outras sob Controle Especial" [Collegiate Board Resolution No. 784 - Lists of Narcotic, Psychotropic, Precursor, and Other Substances under Special Control] (in Brazilian Portuguese). Diário Oficial da União (published 4 April 2023). Archived from the original on 3 August 2023. Retrieved 16 August 2023.
- ^ a b c d e f g "Abilify (aripiprazole) tablet Abilify (aripiprazole) solution Abilify Discmelt (aripiprazole) tablet, orally disintegrating Abilify (aripiprazole) injection, solution [Otsuka America Pharmaceutical, Inc.]". DailyMed. Otsuka America Pharmaceutical, Inc. April 2013. Retrieved 22 October 2013.
- ^ a b c d e f g "Abilify Tablets, Orodispersible Tablets, Oral Solution – Summary of Product Characteristics (SPC)". electronic Medicines Compendium. Otsuka Pharmaceuticals (UK) Ltd. 20 September 2013. Archived from the original on 4 March 2016. Retrieved 22 October 2013.
- ^ a b c d e f g h "ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS" (PDF). European Medicines Agency. Otsuka Pharmaceutical Europe Ltd. Archived from the original (PDF) on 23 October 2013. Retrieved 22 October 2013.
- ^ a b c d e f g h i j k l m "Aripiprazole, ARIPiprazole Lauroxil Monograph for Professionals". Drugs.com. American Society of Health-System Pharmacists. Retrieved 26 February 2019.
- ^ a b c Belgamwar RB, El-Sayeh HG (August 2011). "Aripiprazole versus placebo for schizophrenia". The Cochrane Database of Systematic Reviews (8): CD006622. doi:10.1002/14651858.CD006622.pub2. PMID 21833956.
- ^ a b c d e f g "Product Information for Abilify Aripiprazole Tablets & Orally Disintegrating Tablets". TGA eBusiness Services. Bristol-Myers Squibb Australia Pty Ltd. 1 November 2012. Retrieved 22 October 2013.
- ^ a b "Abilify Discmelt, Abilify Maintena (aripiprazole) dosing, indications, interactions, adverse effects, and more". Medscape Reference. WebMD. Retrieved 22 October 2013.
- ^ "Prescribing medicines in pregnancy database". Australian Government. 3 March 2014. Retrieved 22 April 2014.
- ^ British national formulary: BNF 76 (76th ed.). Pharmaceutical Press. 2018. p. 392. ISBN 978-0-85711-338-2.
- ^ "The Top 300 of 2021". ClinCalc. Archived from the original on 15 January 2024. Retrieved 14 January 2024.
- ^ "Aripiprazole - Drug Usage Statistics". ClinCalc. Retrieved 14 January 2024.
- ^ World Health Organization (2023). The selection and use of essential medicines 2023: web annex A: World Health Organization model list of essential medicines: 23rd list (2023). Geneva: World Health Organization. hdl:10665/371090. WHO/MHP/HPS/EML/2023.02.
- ^ a b c d e "Abilify- aripiprazole tablet Abilify- aripiprazole solution Abilify- aripiprazole tablet, orally disintegrating Abilify- aripiprazole injection, solution". DailyMed. Retrieved 20 October 2020.
- ^ "Psychosis and schizophrenia in children and young people: recognition and management | Guidance and guidelines". nice.org.uk. UK: National Institute for Health and Care Excellence. October 2016.
- ^ "Schizophrenia: aripiprazole prolonged-release suspension for injection | Guidance and guidelines". UK: National Institute for Health and Care Excellence. 24 July 2013.
- ^ Khanna P, Suo T, Komossa K, et al. (January 2014). "Aripiprazole versus other atypical antipsychotics for schizophrenia". The Cochrane Database of Systematic Reviews. 2014 (1): CD006569. doi:10.1002/14651858.CD006569.pub5. PMC 4164478. PMID 24385408.
- ^ "Levels of Evidence". Cochrane.org. Archived from the original on 23 September 2020. Retrieved 12 September 2019.
- ^ Huhn M, Nikolakopoulou A, Schneider-Thoma J, et al. (11 July 2019). "Comparative efficacy and tolerability of 32 oral antipsychotics for the acute treatment of adults with multi-episode schizophrenia: a systematic review and network meta-analysis". The Lancet. 394 (10202): 939–951. doi:10.1016/S0140-6736(19)31135-3. PMC 6891890. PMID 31303314.
- ^ Leucht S, Cipriani A, Spineli L, et al. (September 2013). "Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis". The Lancet. 382 (9896): 951–962. doi:10.1016/S0140-6736(13)60733-3. PMID 23810019. S2CID 32085212.
- ^ a b Hasan A, Falkai P, Wobrock T, et al. (February 2013). "World Federation of Societies of Biological Psychiatry (WFSBP) guidelines for biological treatment of schizophrenia, part 2: update 2012 on the long-term treatment of schizophrenia and management of antipsychotic-induced side effects". The World Journal of Biological Psychiatry. 14 (1): 2–44. doi:10.3109/15622975.2012.739708. PMID 23216388. S2CID 28750563.
- ^ a b Barnes TR (May 2011). "Evidence-based guidelines for the pharmacological treatment of schizophrenia: recommendations from the British Association for Psychopharmacology". Journal of Psychopharmacology. 25 (5): 567–620. doi:10.1177/0269881110391123. PMID 21292923. S2CID 40089561.
- ^ "Bipolar disorder: assessment and management". Recommendations; Guidance and guidelines. UK: National Institute for Health and Care Excellence. 24 September 2014.
1.1 Care for adults, children and young people across all phases of bipolar disorder
- ^ Brown R, Taylor MJ, Geddes J (December 2013). "Aripiprazole alone or in combination for acute mania". The Cochrane Database of Systematic Reviews. 12 (12): CD005000. doi:10.1002/14651858.CD005000.pub2. PMID 24346956.
- ^ De Fruyt J, Deschepper E, Audenaert K, et al. (May 2012). "Second generation antipsychotics in the treatment of bipolar depression: a systematic review and meta-analysis". Journal of Psychopharmacology. 26 (5): 603–617. doi:10.1177/0269881111408461. hdl:2268/196468. PMID 21940761. S2CID 57249815.
- ^ Gitlin M, Frye MA (May 2012). "Maintenance therapies in bipolar disorders". Bipolar Disorders. 14 (Suppl 2): 51–65. doi:10.1111/j.1399-5618.2012.00992.x. PMID 22510036. S2CID 21101054.
- ^ de Bartolomeis A, Perugi G (October 2012). "Combination of aripiprazole with mood stabilizers for the treatment of bipolar disorder: from acute mania to long-term maintenance". Expert Opinion on Pharmacotherapy. 13 (14): 2027–2036. doi:10.1517/14656566.2012.719876. PMID 22946707. S2CID 39065786.
- ^ "1 Recommendations - Bipolar disorder: assessment and management - Guidance". National Institute for Health and Care Excellence. 24 September 2014. Retrieved 3 April 2023.
- ^ "Aripiprazole for treating moderate to severe manic episodes in adolescents with bipolar I disorder". National Institute for Health and Care Excellence. May 2013. Retrieved 3 April 2023.
- ^ "The risks and benefits of high dose antipsychotic medication" (PDF). Royal College of Psychiatrists. 10 November 2014.
- ^ a b Spielmans GI, Berman MI, Linardatos E, et al. (March 2013). "Adjunctive atypical antipsychotic treatment for major depressive disorder: a meta-analysis of depression, quality of life, and safety outcomes". PLOS Medicine. 10 (3): e1001403. doi:10.1371/journal.pmed.1001403. PMC 3595214. PMID 23554581.
- ^ Nelson JC, Papakostas GI (September 2009). "Atypical antipsychotic augmentation in major depressive disorder: a meta-analysis of placebo-controlled randomized trials". The American Journal of Psychiatry. 166 (9): 980–991. doi:10.1176/appi.ajp.2009.09030312. PMID 19687129.
- ^ Komossa K, Depping AM, Gaudchau A, et al. (December 2010). "Second-generation antipsychotics for major depressive disorder and dysthymia". The Cochrane Database of Systematic Reviews (12): CD008121. doi:10.1002/14651858.CD008121.pub2. PMID 21154393.
- ^ Azuma J, Hasunuma T, Kubo M, et al. (January 2012). "The relationship between clinical pharmacokinetics of aripiprazole and CYP2D6 genetic polymorphism: effects of CYP enzyme inhibition by coadministration of paroxetine or fluvoxamine". European Journal of Clinical Pharmacology. 68 (1): 29–37. doi:10.1007/s00228-011-1094-4. PMC 3249179. PMID 21739267.
- ^ Hahn M, Roll SC (December 2016). "Dosing Recommendations of Aripiprazole Depot with Strong Cytochrome P450 3A4 Inhibitors: A Relapse Risk". Drug Safety: Case Reports. 3 (1): 5. doi:10.1007/s40800-016-0027-7. PMC 5005780. PMID 27747685.
- ^ Jallaq SA, Verba M, Strawn JR, et al. (February 2021). "CYP2D6 Phenotype Influences Aripiprazole Tolerability in Pediatric Patients with Mood Disorders". Journal of Child and Adolescent Psychopharmacology. 31 (1): 56–62. doi:10.1089/cap.2020.0058. PMC 8255312. PMID 32845723.
- ^ Hoffelt C, Gross T (January 2016). "A review of significant pharmacokinetic drug interactions with antidepressants and their management". The Mental Health Clinician. 6 (1): 35–41. doi:10.9740/mhc.2016.01.035. PMC 6009245. PMID 29955445.
- ^ a b c Hirsch LE, Pringsheim T (June 2016). "Aripiprazole for autism spectrum disorders (ASD)". The Cochrane Database of Systematic Reviews. 2016 (6): CD009043. doi:10.1002/14651858.CD009043.pub3. PMC 7120220. PMID 27344135.
- ^ a b c d e f g "Aripiprazole". adisInsight. springer.com. Springer. Retrieved 21 September 2021.
- ^ Janik P, Szejko N (2018). "Aripiprazole in treatment of Gilles de la Tourette syndrome – New therapeutic option". Neurologia I Neurochirurgia Polska. 52 (1): 84–87. doi:10.1016/j.pjnns.2017.10.015. PMID 29154107.
- ^ Müller-Vahl KR, Szejko N, Verdellen C, et al. (March 2022). "European clinical guidelines for Tourette syndrome and other tic disorders: summary statement". European Child & Adolescent Psychiatry. 31 (3): 377–382. doi:10.1007/s00787-021-01832-4. PMC 8940881. PMID 34244849.
- ^ Wang S, Wei YZ, Yang JH, et al. (August 2017). "The efficacy and safety of aripiprazole for tic disorders in children and adolescents: A systematic review and meta-analysis". Psychiatry Research. 254: 24–32. doi:10.1016/j.psychres.2017.04.013. PMID 28441584. S2CID 13792422.
- ^ Cox JH, Seri S, Cavanna AE (2016). "Safety and efficacy of aripiprazole for the treatment of pediatric Tourette syndrome and other chronic tic disorders". Pediatric Health, Medicine and Therapeutics. 7: 57–64. doi:10.2147/PHMT.S87121. PMC 5683285. PMID 29388585.
- ^ Zheng W, Li XB, Xiang YQ, et al. (January 2016). "Aripiprazole for Tourette's syndrome: a systematic review and meta-analysis". Human Psychopharmacology. 31 (1): 11–18. doi:10.1002/hup.2498. PMID 26310194. S2CID 5353158.
- ^ Yang CS, Huang H, Zhang LL, et al. (July 2015). "Aripiprazole for the treatment of tic disorders in children: a systematic review and meta-analysis". BMC Psychiatry. 15: 179. doi:10.1186/s12888-015-0504-z. PMC 4518630. PMID 26220447.
- ^ a b Veale D, Miles S, Smallcombe N, et al. (November 2014). "Atypical antipsychotic augmentation in SSRI treatment refractory obsessive-compulsive disorder: a systematic review and meta-analysis". BMC Psychiatry. 14 (1): 317. doi:10.1186/s12888-014-0317-5. PMC 4262998. PMID 25432131.
- ^ Veale D, Miles S, Smallcombe N, et al. (November 2014). "Atypical antipsychotic augmentation in SSRI treatment refractory obsessive-compulsive disorder: a systematic review and meta-analysis". BMC Psychiatry. 14: 317. doi:10.1186/s12888-014-0317-5. PMC 4262998. PMID 25432131.
- ^ Koran LM, Hanna GL, Hollander E, et al. (July 2007). "Practice guideline for the treatment of patients with obsessive-compulsive disorder". The American Journal of Psychiatry. 164 (7 Suppl): 5–53. PMID 17849776.
- ^ Fornaro M, Gabrielli F, Mattei C, et al. (December 2008). "Aripiprazole augmentation in poor insight obsessive-compulsive disorder: a case report". Annals of General Psychiatry. 7 (1): 26. doi:10.1186/1744-859X-7-26. PMC 2621216. PMID 19105842.
- ^ Pignon B, Tezenas du Montcel C, Carton L, et al. (November 2017). "The Place of Antipsychotics in the Therapy of Anxiety Disorders and Obsessive-Compulsive Disorders". Current Psychiatry Reports. 19 (12): 103. doi:10.1007/s11920-017-0847-x. PMID 29110139. S2CID 41312623.
- ^ "l FDA warns about new impulse-control problems associated with mental health drug aripiprazole (Abilify, Abilify Maintena, Aristada)". FDA.gov. US Food and Drug Administration. 9 February 2019. Retrieved 3 April 2023.
- ^ a b "Aripiprazole: MedlinePlus Drug Information". medlineplus.gov.
- ^ "DailyMed - ARIPIPRAZOLE- aripiprazole tablet". dailymed.nlm.nih.gov. Retrieved 4 November 2023.
BOXED WARNING WARNING: INCREASED MORTALITY IN ELDERLY PATIENTS WITH DEMENTIA-RELATED PSYCHOSIS and SUICIDAL THOUGHTS AND BEHAVIORS WITH ANTIDEPRESSANT DRUGS Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Aripiprazole tablets are not approved for the treatment of patients with dementia-related psychosis [see WARNINGS AND PRECAUTIONS (5.1)]. Antidepressants increased the risk of suicidal thoughts and behavior in children, adolescents, and young adults in short-term studies. These studies did not show an increase in the risk of suicidal thoughts and behavior with antidepressant use in patients over age 24; there was a reduction in risk with antidepressant use in patients aged 65 and older [see WARNINGS AND PRECAUTIONS (5.3)]. In patients of all ages who are started on antidepressant therapy, monitor closely for worsening, and for emergence of suicidal thoughts and behaviors. Advise families and caregivers of the need for close observation and communication with the prescriber [see WARNINGS AND PRECAUTIONS (5. 3)].
- ^ a b "Aripiprazole (Abilify, Abilify Maintena, Aristada): Drug Safety Communication – FDA Warns About New Impulse-control Problems". U.S. Food and Drug Administration (FDA). 3 May 2016. Retrieved 4 May 2016.
- ^ Grall-Bronnec M, Sauvaget A, Perrouin F, Leboucher J, Etcheverrigaray F, Challet-Bouju G, et al. (February 2016). "Pathological Gambling Associated With Aripiprazole or Dopamine Replacement Therapy: Do Patients Share the Same Features? A Review". Journal of Clinical Psychopharmacology. 36 (1): 63–70. doi:10.1097/JCP.0000000000000444. PMC 4700874. PMID 26658263.
- ^ Joint Formulary Committee, ed. (March 2009). "4.2.1". British National Formulary (57 ed.). United Kingdom: Royal Pharmaceutical Society of Great Britain. p. 192. ISBN 978-0-85369-845-6.
Withdrawal of antipsychotic drugs after long-term therapy should always be gradual and closely monitored to avoid the risk of acute withdrawal syndromes or rapid relapse.
- ^ a b c d e Haddad P, Haddad PM, Dursun S, Deakin B (2004). Adverse Syndromes and Psychiatric Drugs: A Clinical Guide. OUP Oxford. pp. 207–216. ISBN 978-0-19-852748-0.
- ^ Moncrieff J (July 2006). "Does antipsychotic withdrawal provoke psychosis? Review of the literature on rapid onset psychosis (supersensitivity psychosis) and withdrawal-related relapse". Acta Psychiatrica Scandinavica. 114 (1): 3–13. doi:10.1111/j.1600-0447.2006.00787.x. PMID 16774655. S2CID 6267180.
- ^ Sacchetti E, Vita A, Siracusano A, Fleischhacker W (2013). Adherence to Antipsychotics in Schizophrenia. Springer Science & Business Media. p. 85. ISBN 9788847026797.
- ^ Baselt RC (2008). Disposition of Toxic Drugs and Chemicals in Man (8th ed.). Foster City, CA: Biomedical Publications. pp. 105–6. ISBN 978-0-9626523-7-0.
- ^ Skov L, Johansen SS, Linnet K (January 2015). "Postmortem femoral blood reference concentrations of aripiprazole, chlorprothixene, and quetiapine". Journal of Analytical Toxicology. 39 (1): 41–44. doi:10.1093/jat/bku121. PMID 25342720.
- ^ "Abilify (Aripiprazole) – Warnings and Precautions". DrugLib.com. 14 February 2007. Archived from the original on 4 December 2008. Retrieved 8 December 2008.
- ^ Yanofski J (June 2010). "The dopamine dilemma: using stimulants and antipsychotics concurrently". Psychiatry. 7 (6): 18–23. PMC 2898838. PMID 20622942.
- ^ Akritopoulou-Zanze I (2012). "6. Arylpiperazine-Based 5-HT1A Receptor Partial Agonists and 5-HT2A Antagonists for the Treatment of Autism, Depression, Anxiety, Psychosis, and Schizophrenia". In Dinges J, Lamberth C (eds.). Bioactive heterocyclic compound classes pharmaceuticals. Weinheim: Wiley-VCH. ISBN 978-3-527-66445-0.
- ^ Dörwald FZ, ed. (2012). "46. Arylalkylamines". Lead optimization for medicinal chemists: pharmacokinetic properties of functional groups and organic compounds. Weinheim: Wiley-VCH. ISBN 978-3-527-64564-0.
- ^ Serezhkin VN, Savchenkov AV (2020). "Application of the Method of Molecular Voronoi–Dirichlet Polyhedra for Analysis of Noncovalent Interactions in Aripiprazole Polymorphs". Crystal Growth & Design. 20 (3): 1997–2003. doi:10.1021/acs.cgd.9b01645. S2CID 213824513.
- ^ Warren LR, McGowan E, Renton M, Morrison CA, Funnell NP (October 2021). "Direct evidence for distinct colour origins in ROY polymorphs". Chemical Science. 12 (38): 12711–12718. doi:10.1039/d1sc04051k. PMC 8494124. PMID 34703557.
- ^ Behere PB, Das A, Behere AP (2018). Clinical Psychopharmacology: An Update. Springer. p. 66. ISBN 9789811320927.
- ^ de Bartolomeis A, Tomasetti C, Iasevoli F (September 2015). "Update on the Mechanism of Action of Aripiprazole: Translational Insights into Antipsychotic Strategies Beyond Dopamine Receptor Antagonism". CNS Drugs. 29 (9): 773–799. doi:10.1007/s40263-015-0278-3. PMC 4602118. PMID 26346901.
- ^ "Otsuka's Antipsychotic Abilify Is Approved in Japan, January 23, 2006|News Releases". Otsuka Pharmaceutical Co., Ltd. Retrieved 6 October 2022.
- ^ Kikuchi T, Maeda K, Suzuki M, Hirose T, Futamura T, McQuade RD (June 2021). "Discovery research and development history of the dopamine D2 receptor partial agonists, aripiprazole and brexpiprazole". Neuropsychopharmacology Reports. 41 (2): 134–143. doi:10.1002/npr2.12180. PMC 8340839. PMID 33960741.
- ^ Roth BL, Driscol J. "PDSP Ki Database". Psychoactive Drug Screening Program (PDSP). University of North Carolina at Chapel Hill and the United States National Institute of Mental Health. Retrieved 14 August 2017.
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z aa ab ac ad ae af ag ah ai aj ak al am an ao ap aq ar as at au av aw ax ay az ba bb bc bd Shapiro DA, Renock S, Arrington E, Chiodo LA, Liu LX, Sibley DR, et al. (August 2003). "Aripiprazole, a novel atypical antipsychotic drug with a unique and robust pharmacology". Neuropsychopharmacology. 28 (8): 1400–1411. doi:10.1038/sj.npp.1300203. PMID 12784105.
- ^ Mohr P, Masopust J, Kopeček M (25 January 2022). "Dopamine Receptor Partial Agonists: Do They Differ in Their Clinical Efficacy?". Frontiers in Psychiatry. 12: 781946. doi:10.3389/fpsyt.2021.781946. PMC 8821167. PMID 35145438.
- ^ a b c d e f g h i j k Keck PE, McElroy SL (April 2003). "Aripiprazole: a partial dopamine D2 receptor agonist antipsychotic". Expert Opinion on Investigational Drugs. 12 (4): 655–662. doi:10.1517/13543784.12.4.655. PMID 12665420. S2CID 8654102.
- ^ a b c d e f g h i j k Kroeze WK, Hufeisen SJ, Popadak BA, Renock SM, Steinberg S, Ernsberger P, et al. (March 2003). "H1-histamine receptor affinity predicts short-term weight gain for typical and atypical antipsychotic drugs". Neuropsychopharmacology. 28 (3): 519–526. doi:10.1038/sj.npp.1300027. PMID 12629531.
- ^ Starrenburg FC, Bogers JP (April 2009). "How can antipsychotics cause Diabetes Mellitus? Insights based on receptor-binding profiles, humoral factors and transporter proteins". European Psychiatry. 24 (3): 164–170. doi:10.1016/j.eurpsy.2009.01.001. PMID 19285836. S2CID 42636469.
- ^ a b c d e "Abilify (Aripiprazole) – Clinical Pharmacology". DrugLib.com. 14 February 2007. Retrieved 8 December 2008.
- ^ Brunton L (2011). Goodman & Gilman's The Pharmacological Basis of Therapeutics (12th ed.). China: McGraw-Hill. pp. 406–410. ISBN 978-0-07-162442-8.
- ^ a b c Davies MA, Sheffler DJ, Roth BL (2004). "Aripiprazole: a novel atypical antipsychotic drug with a uniquely robust pharmacology". CNS Drug Reviews. 10 (4): 317–336. doi:10.1111/j.1527-3458.2004.tb00030.x. PMC 6741761. PMID 15592581.
- ^ Pae CU, Serretti A, Patkar AA, Masand PS (2008). "Aripiprazole in the treatment of depressive and anxiety disorders: a review of current evidence". CNS Drugs. 22 (5): 367–388. doi:10.2165/00023210-200822050-00002. PMID 18399707. S2CID 19757151.
- ^ Tuplin EW, Holahan MR (November 2017). "Aripiprazole, A Drug that Displays Partial Agonism and Functional Selectivity". Current Neuropharmacology. 15 (8): 1192–1207. doi:10.2174/1570159X15666170413115754. PMC 5725548. PMID 28412910.
- ^ a b c Wood M, Reavill C (June 2007). "Aripiprazole acts as a selective dopamine D2 receptor partial agonist". Expert Opinion on Investigational Drugs. 16 (6): 771–775. doi:10.1517/13543784.16.6.771. PMID 17501690. S2CID 42171115.
- ^ a b Kegeles LS, Slifstein M, Frankle WG, Xu X, Hackett E, Bae SA, et al. (December 2008). "Dose-occupancy study of striatal and extrastriatal dopamine D2 receptors by aripiprazole in schizophrenia with PET and [18F]fallypride". Neuropsychopharmacology. 33 (13): 3111–3125. doi:10.1038/npp.2008.33. PMID 18418366.
- ^ a b Yokoi F, Gründer G, Biziere K, Stephane M, Dogan AS, Dannals RF, et al. (August 2002). "Dopamine D2 and D3 receptor occupancy in normal humans treated with the antipsychotic drug aripiprazole (OPC 14597): a study using positron emission tomography and [11C]raclopride". Neuropsychopharmacology. 27 (2): 248–259. doi:10.1016/S0893-133X(02)00304-4. PMID 12093598.
- ^ a b Jordan S, Koprivica V, Chen R, Tottori K, Kikuchi T, Altar CA (April 2002). "The antipsychotic aripiprazole is a potent, partial agonist at the human 5-HT1A receptor". European Journal of Pharmacology. 441 (3): 137–140. doi:10.1016/S0014-2999(02)01532-7. PMID 12063084.
- ^ a b c d e Mamo D, Graff A, Mizrahi R, Shammi CM, Romeyer F, Kapur S (September 2007). "Differential effects of aripiprazole on D(2), 5-HT(2), and 5-HT(1A) receptor occupancy in patients with schizophrenia: a triple tracer PET study". The American Journal of Psychiatry. 164 (9): 1411–1417. doi:10.1176/appi.ajp.2007.06091479. PMID 17728427.
- ^ a b c Mailman RB, Murthy V (May 2010). "Third generation antipsychotic drugs: partial agonism or receptor functional selectivity?". Current Pharmaceutical Design. 16 (5): 488–501. doi:10.2174/138161210790361461. PMC 2958217. PMID 19909227.
- ^ "Aristada Initio (Aripiprazole Lauroxil Injectable Suspension): Uses, Dosage, Side Effects, Interactions, Warning". RxList. Retrieved 22 November 2022.
- ^ Burris KD, Molski TF, Xu C, Ryan E, Tottori K, Kikuchi T, et al. (July 2002). "Aripiprazole, a novel antipsychotic, is a high-affinity partial agonist at human dopamine D2 receptors". The Journal of Pharmacology and Experimental Therapeutics. 302 (1): 381–389. doi:10.1124/jpet.102.033175. PMID 12065741. S2CID 12919430.
- ^ Urban JD, Vargas GA, von Zastrow M, Mailman RB (January 2007). "Aripiprazole has functionally selective actions at dopamine D2 receptor-mediated signaling pathways". Neuropsychopharmacology. 32 (1): 67–77. doi:10.1038/sj.npp.1301071. PMID 16554739. S2CID 31846731.
- ^ Yokoi F, Gründer G, Biziere K, Stephane M, Dogan AS, Dannals RF, et al. (August 2002). "Dopamine D2 and D3 receptor occupancy in normal humans treated with the antipsychotic drug aripiprazole (OPC 14597): a study using positron emission tomography and [11C]raclopride". Neuropsychopharmacology. 27 (2): 248–259. doi:10.1016/S0893-133X(02)00304-4. PMID 12093598. S2CID 26101524.
- ^ Kegeles LS, Slifstein M, Frankle WG, Xu X, Hackett E, Bae SA, et al. (December 2008). "Dose-occupancy study of striatal and extrastriatal dopamine D2 receptors by aripiprazole in schizophrenia with PET and [18F]fallypride". Neuropsychopharmacology. 33 (13): 3111–3125. doi:10.1038/npp.2008.33. PMID 18418366. S2CID 33993650.
- ^ Tadori Y, Miwa T, Tottori K, Burris KD, Stark A, Mori T, Kikuchi T (May 2005). "Aripiprazole's low intrinsic activities at human dopamine D2L and D2S receptors render it a unique antipsychotic". European Journal of Pharmacology. 515 (1–3): 10–19. doi:10.1016/j.ejphar.2005.02.051. PMID 15894311.
- ^ Shapiro DA, Renock S, Arrington E, Chiodo LA, Liu LX, Sibley DR, et al. (August 2003). "Aripiprazole, a novel atypical antipsychotic drug with a unique and robust pharmacology". Neuropsychopharmacology. 28 (8): 1400–1411. doi:10.1038/sj.npp.1300203. PMID 12784105. S2CID 22568982.
- ^ "In This Issue". Am J Psychiatry. 165 (8): A46. August 2008. doi:10.1176/appi.ajp.2008.165.8.A46.
- ^ Zhang JY, Kowal DM, Nawoschik SP, Lou Z, Dunlop J (February 2006). "Distinct functional profiles of aripiprazole and olanzapine at RNA edited human 5-HT2C receptor isoforms". Biochemical Pharmacology. 71 (4): 521–529. doi:10.1016/j.bcp.2005.11.007. PMID 16336943.
- ^ Lawler CP, Prioleau C, Lewis MM, Mak C, Jiang D, Schetz JA, et al. (June 1999). "Interactions of the novel antipsychotic aripiprazole (OPC-14597) with dopamine and serotonin receptor subtypes". Neuropsychopharmacology. 20 (6): 612–627. doi:10.1016/S0893-133X(98)00099-2. PMID 10327430.
- ^ Mauri MC, Paletta S, Maffini M, Colasanti A, Dragogna F, Di Pace C, Altamura AC (2014). "Clinical pharmacology of atypical antipsychotics: an update". EXCLI Journal. 13: 1163–1191. PMC 4464358. PMID 26417330.
- ^ Kessler RM (September 2007). "Aripiprazole: what is the role of dopamine D(2) receptor partial agonism?". The American Journal of Psychiatry. 164 (9): 1310–1312. doi:10.1176/appi.ajp.2007.07071043. PMID 17728411. S2CID 1891586.
- ^ Parent M, Toussaint C, Gilson H (1983). "Long-term treatment of chronic psychotics with bromperidol decanoate: clinical and pharmacokinetic evaluation". Current Therapeutic Research. 34 (1): 1–6.
- ^ a b Jørgensen A, Overø KF (1980). "Clopenthixol and flupenthixol depot preparations in outpatient schizophrenics. III. Serum levels". Acta Psychiatrica Scandinavica. Supplementum. 279: 41–54. doi:10.1111/j.1600-0447.1980.tb07082.x. PMID 6931472.
- ^ a b Reynolds JE (1993). "Anxiolytic sedatives, hypnotics and neuroleptics.". Martindale: The Extra Pharmacopoeia (30th ed.). London: Pharmaceutical Press. pp. 364–623.
- ^ Ereshefsky L, Saklad SR, Jann MW, Davis CM, Richards A, Seidel DR (May 1984). "Future of depot neuroleptic therapy: pharmacokinetic and pharmacodynamic approaches". The Journal of Clinical Psychiatry. 45 (5 Pt 2): 50–9. PMID 6143748.
- ^ a b Curry SH, Whelpton R, de Schepper PJ, Vranckx S, Schiff AA (April 1979). "Kinetics of fluphenazine after fluphenazine dihydrochloride, enanthate and decanoate administration to man". British Journal of Clinical Pharmacology. 7 (4): 325–31. doi:10.1111/j.1365-2125.1979.tb00941.x. PMC 1429660. PMID 444352.
- ^ Young D, Ereshefsky L, Saklad SR, Jann MW, Garcia N (1984). Explaining the pharmacokinetics of fluphenazine through computer simulations. (Abstract.). 19th Annual Midyear Clinical Meeting of the American Society of Hospital Pharmacists. Dallas, Texas.
- ^ Janssen PA, Niemegeers CJ, Schellekens KH, Lenaerts FM, Verbruggen FJ, van Nueten JM, Marsboom RH, Hérin VV, Schaper WK (November 1970). "The pharmacology of fluspirilene (R 6218), a potent, long-acting and injectable neuroleptic drug". Arzneimittel-Forschung. 20 (11): 1689–98. PMID 4992598.
- ^ Beresford R, Ward A (January 1987). "Haloperidol decanoate. A preliminary review of its pharmacodynamic and pharmacokinetic properties and therapeutic use in psychosis". Drugs. 33 (1): 31–49. doi:10.2165/00003495-198733010-00002. PMID 3545764.
- ^ Reyntigens AJ, Heykants JJ, Woestenborghs RJ, Gelders YG, Aerts TJ (1982). "Pharmacokinetics of haloperidol decanoate. A 2-year follow-up". International Pharmacopsychiatry. 17 (4): 238–46. doi:10.1159/000468580. PMID 7185768.
- ^ Larsson M, Axelsson R, Forsman A (1984). "On the pharmacokinetics of perphenazine: a clinical study of perphenazine enanthate and decanoate". Current Therapeutic Research. 36 (6): 1071–88.
- ^ a b Grady MA, Gasperoni TL, Kirkpatrick P (June 2003). "Aripiprazole". Nature Reviews. Drug Discovery. 2 (6): 427–428. doi:10.1038/nrd1114. PMID 12790153.
- ^ Kikuchi T, Tottori K, Uwahodo Y, Hirose T, Miwa T, Oshiro Y, Morita S (July 1995). "7-(4-[4-(2,3-Dichlorophenyl)-1-piperazinyl]butyloxy)-3,4-dihydro-2(1H)-quinolinone (OPC-14597), a new putative antipsychotic drug with both presynaptic dopamine autoreceptor agonistic activity and postsynaptic D2 receptor antagonistic activity". The Journal of Pharmacology and Experimental Therapeutics. 274 (1): 329–336. PMID 7616416.
- ^ "B-MS reveals Ph III aripiprazole data – Pharmaceutical industry news". The Pharma Letter. 17 May 2000.
- ^ "Abilify Product information". Union Register of medicinal products. 8 June 2004. Retrieved 1 October 2023.
- ^ Hitti M (20 November 2007). "FDA OKs Abilify for Depression". WebMD. Archived from the original on 5 December 2008. Retrieved 8 December 2008.
- ^ Keating G (23 November 2009). "FDA OKs Abilify for child autism irritability". Reuters. Retrieved 22 September 2010.
- ^ a b "Patent and Exclusivity Search Results". Electronic Orange Book. U.S. Food and Drug Administration (FDA). Retrieved 8 December 2008.
- ^ a b Mitchell M (8 December 2016). "Bristol-Myers Squibb Agrees to $19.5M Settlement Over Abilify Marketing". The Legal Intelligencer.
- ^ Staton T. "Pharma's Top 11 Marketing Settlements: Bristol-Myers Squibb – Abilify". FiercePharma. Retrieved 4 June 2017.
- ^ "Press Release: Lundbeck and Otsuka Pharmaceutical sign historic agreement to deliver innovative medicines targeting psychiatric disorders worldwide (OMX:LUN)". Lundbeck. 11 November 2011. Archived from the original on 1 April 2012. Retrieved 4 June 2017.
- ^ Megan Brooks (30 January 2014). "Top 100 Selling Drugs of 2013". Medscape. Retrieved 15 October 2015.
- ^ "BMS cuts salesforce on revised Abilify deal". PM Live. 7 November 2012.
- ^ Sagonowsky E (1 December 2016). "Lundbeck, Otsuka seek Abilify Maintena nod in bipolar disorder". FiercePharma.
- ^ "Abilify Maintena 300mg & 400mg powder and solvent for prolonged-release suspension for injection and suspension for injection in pre filled syringe – Summary of Product Characteristics (SPC)". UK Electronic Medicines Compendium. Retrieved 4 June 2017.
- ^ "Barr Confirms Filing an Application with a Paragraph IV Certification for Abilify Tablets" (Press release). Barr Pharmaceuticals, Inc. 20 March 2007. Retrieved 23 December 2008.
- ^ Decker S, Randall T (15 November 2010). "Bristol-Myers Partner Otsuka Wins Abilify Ruling – Bloomberg Business". Bloomberg L.P. Archived from the original on 22 July 2016. Retrieved 13 May 2015.
- ^ B1 EP application 0367141 B1, Oshiro Y, Sato S, Kurahashi N, "Carbostyril derivatives", published 1 October 1996, assigned to Otsuka Pharmaceutical Co., Ltd.
- ^ "Patent decision". UK Intellectual Property Office. 19 September 2006.
- ^ Michaelson J (9 November 2014). "Mother's Little Anti-Psychotic Is Worth $6.9 Billion A Year". The Daily Beast.
- ^ "FDA approves first generic Abilify to treat mental illnesses". Food and Drug Administration. Archived from the original on 1 May 2015. Retrieved 28 April 2015.
- ^ "Latest News | Teva Pharmaceuticals". www.tevapharm.com. 20 May 2023.
- ^ Citrome L (2015). "Aripiprazole long-acting injectable formulations for schizophrenia: aripiprazole monohydrate and aripiprazole lauroxil". Expert Review of Clinical Pharmacology. 9 (2): 169–186. doi:10.1586/17512433.2016.1121809. PMID 26573020. S2CID 207208248.
- ^ "Aristada (aripiprazole lauroxil) FDA Approval History". Drugs.com. Retrieved 11 May 2018.
- ^ Staton T (14 December 2016). "Bristol-Myers to pay $19.5 million in Abilify off-label marketing settlement". FiercePharma.
- ^ "FDA approves pill with sensor that digitally tracks if patients have ingested their medication" (Press release). U.S. Food and Drug Administration (FDA). Retrieved 29 November 2017.
- ^ Belluck P (13 November 2017). "First Digital Pill Approved to Worries About Biomedical 'Big Brother'". The New York Times. ISSN 0362-4331. Retrieved 29 November 2017.
- ^ "Expert Q&A: Exploring a New Long-Acting Injectable for Bipolar I Disorder". bpHope.com. 8 May 2023. Retrieved 16 April 2024.
- ^ "FDA Approves Aripiprazole as First Once-Every-2-Months Long-Acting Injectable for Schizophrenia, Bipolar I Disorder". Pharmacy Times. 28 April 2023. Retrieved 16 April 2024.
- ^ "Otsuka and Lundbeck's schizophrenia treatment gains EC approval". Pharmaceutical Technology. 28 March 2024. Retrieved 16 April 2024.
- ^ Joint Formulary Committee. British National Formulary (BNF) 79. Pharmaceutical Pr; 2020.
- ^ "Australian Medicines Handbook 2013 [Internet]". Retrieved 20 September 2013.
- ^ Truven Health Analytics, Inc. DRUGDEX System (Internet) [cited 2013 Jun 25]. Greenwood Village, CO: Thomsen Healthcare; 2013.
- ^ a b c Casey AB, Canal CE (June 2017). "Classics in Chemical Neuroscience: Aripiprazole". ACS Chemical Neuroscience. 8 (6): 1135–1146. doi:10.1021/acschemneuro.7b00087. PMC 5495458. PMID 28368577.
- ^ de Bartolomeis A, Tomasetti C, Iasevoli F (September 2015). "Update on the Mechanism of Action of Aripiprazole: Translational Insights into Antipsychotic Strategies Beyond Dopamine Receptor Antagonism". CNS Drugs. 29 (9): 773–799. doi:10.1007/s40263-015-0278-3. PMC 4602118. PMID 26346901.
- ^ a b De Crescenzo F, Cortese S, Adamo N, Janiri L (February 2017). "Pharmacological and non-pharmacological treatment of adults with ADHD: a meta-review". Evidence-Based Mental Health. 20 (1): 4–11. doi:10.1136/eb-2016-102415. PMC 10699262. PMID 27993933. S2CID 24904076.
- ^ a b c d Ghanizadeh A (October 2013). "Systematic review of clinical trials of aripiprazole for treating attention deficit hyperactivity disorder". Neurosciences. 18 (4): 323–329. PMID 24141455.
- ^ Buoli M, Serati M, Cahn W (2016). "Alternative pharmacological strategies for adult ADHD treatment: a systematic review". Expert Review of Neurotherapeutics. 16 (2): 131–144. doi:10.1586/14737175.2016.1135735. PMID 26693882. S2CID 33004517.
- ^ Kikukawa S (May 2008). "Effectiveness of aripiprazole in treatment of adults with attention deficit disorder and restless legs syndrome". The International Journal of Neuropsychopharmacology. 11 (3): 439–440. doi:10.1017/S1461145707008310. PMID 18208634.
- ^ a b c d Brackins T, Brahm NC, Kissack JC (December 2011). "Treatments for methamphetamine abuse: a literature review for the clinician". Journal of Pharmacy Practice. 24 (6): 541–550. doi:10.1177/0897190011426557. PMID 22095579. S2CID 37335642.
- ^ a b c d Brunetti M, Di Tizio L, Dezi S, Pozzi G, Grandinetti P, Martinotti G (October 2012). "Aripiprazole, alcohol and substance abuse: a review". European Review for Medical and Pharmacological Sciences. 16 (10): 1346–1354. PMID 23104650.
- ^ a b c d Karila L, Weinstein A, Aubin HJ, Benyamina A, Reynaud M, Batki SL (June 2010). "Pharmacological approaches to methamphetamine dependence: a focused review". British Journal of Clinical Pharmacology. 69 (6): 578–592. doi:10.1111/j.1365-2125.2010.03639.x. PMC 2883750. PMID 20565449.
- ^ a b c d Elkashef A, Vocci F, Hanson G, White J, Wickes W, Tiihonen J (2008). "Pharmacotherapy of methamphetamine addiction: an update". Substance Abuse. 29 (3): 31–49. doi:10.1080/08897070802218554. PMC 2597382. PMID 19042205.
Further reading[edit]
- Dean L (2016). "Aripiprazole Therapy and CYP2D6 Genotype". In Pratt VM, McLeod HL, Rubinstein WS, et al. (eds.). Medical Genetics Summaries. National Center for Biotechnology Information (NCBI). PMID 28520375. Bookshelf ID: NBK385288.
External links[edit]
- "Mechanism of Action of Aripiprazole". Psychopharmacology Institute.
- 2,3-Dichlorophenylpiperazines
- 5-HT2A antagonists
- 5-HT2B antagonists
- 5-HT2C agonists
- 5-HT7 antagonists
- Alpha-1 blockers
- Alpha-2 blockers
- Atypical antipsychotics
- Drugs developed by Bristol Myers Squibb
- D2 antagonists
- D2-receptor agonists
- D3 antagonists
- D3 receptor agonists
- Ethers
- H1 receptor antagonists
- Mood stabilizers
- Otsuka Pharmaceutical
- Serotonin-dopamine activity modulators
- Tetrahydroquinolines
- Treatment of autism
