ETV6
ETV6 (i.e. translocation-Ets-leukemia virus) protein is a transcription factor that in humans is encoded by the ETV6 (previously known as TEL) gene. The ETV6 protein regulates the development and growth of diverse cell types, particularly those of hematological tissues. However, its gene, ETV6 frequently suffers various mutations that lead to an array of potentially lethal cancers, i.e., ETV6 is a clinically significant proto-oncogene in that it can fuse with other genes to drive the development and/or progression of certain cancers. However, ETV6 is also an anti-oncogene or tumor suppressor gene in that mutations in it that encode for a truncated and therefore inactive protein are also associated with certain types of cancers.
Gene[edit]
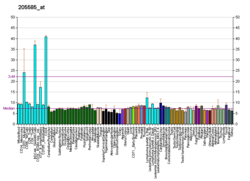
The human ETV6 gene is located at position "13.2" on the short (i.e. "p") arm of chromosome 12, i.e. its notated position is 12p13.2. The gene has 8 exons and two start codons, one located at exon 1 at the start of the gene and an alternative located upstream of exon 3. ETV6 codes for a full length protein consisting of 452 amino acids; the gene is expressed in virtually all cell types and tissues.[5][6] Mice depleted of the ETV6 gene by Gene knockout die between day 10.5 and 11.5 of embryonic life with defective yolk sac angiogenesis and extensive losses in mesenchymal and neural cells due to apoptosis. Other genetic manipulation studies in mice indicate that the gene is required for the development and maintenance of bone marrow-based blood cell formation and the vascular network.[5][7]
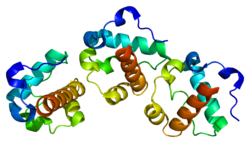
Protein[edit]
The human ETV6 protein is a member of the ETS transcription factor family; however, it more often acts to inhibit than stimulate transcription of its target genes. ETV6 protein contains 3 domains: a) the pointed N-terminal (i.e. PNT) domain which forms oligomer partners with itself as well as other transcription factors (e.g. FLI1) and is required for ETV6's transcriptional repressing activity; b) the central regulatory domain; and c) the C-terminal DNA-binding domain, ETS, which binds to the consensus DNA sequence, 5-GGAA/T-3 within a 9-to-10 bp sequence, in the target genes it regulates.[5][8] ETV6 interacts with other proteins that regulate the differentiation and growth of cells. It binds to and thereby inhibits FLI1, another member of the ETS transcription factor family, which is active in promoting the maturation of blood platelet-forming megakaryocytes and blocking the Cellular differentiation of erythroblasts into red blood cells; this results in the excessive proliferation and abnormal morphology of erythroblasts.[9][7] ETV6 likewise binds to HTATIP, a histone acetyl transferase that regulates the expression of various genes involved in gene transcription, DNA repair, and cellular apoptosis; this binding promotes the transcription-repressing activity of ETV6.[10]
Medical significance[edit]
Inherited mutations[edit]
Rare missense and other loss of function mutations in ETV6 cause thrombocytopenia 5, an autosomal dominant familial disease characterized by variable thrombocytopenia (blood platelet counts from 5% to 90% of normal), mild to modest bleeding tendencies, and bone marrow biopsy findings of abnormal appearing megakaryocytes (i.e. nuclei with fewer than the normal number of lobulations) and red cell macrocytosis.[7][11] Thrombocytopenia 5 is associated with an increased incidence of developing hematological (e.g. chronic myelomonocytic leukemia, acute myelocytic leukemia, B cell acute lymphoblastic leukemia, mixed phenotype acute leukemia, Myelodysplastic syndrome, and multiple myeloma) and non-hematological (e.g. skin and colon) cancers as well as non-malignant diseases such as refractory anemia myopathies, and gastroesophageal reflux disease.[11][12]
Two unrelated kindreds were found to have autosomal dominant inherited mutations in the ETV6 gene, one family with a germline DNA substitution termed L349P that lead to replacing leucine with proline at amino acid 349 in the DNA binding domain of the ETV6, the second, termed N385fs, in germline DNA caused the lose of five base pairs ETV6 and a truncated ETV6 protein. Both mutant proteins failed to enter cell nuclei normally and had a reduced capacity to target genes regulated by the normal ETV6 protein. Afflicted members of these families had low platelet counts (i.e. thrombocytopenia) and acute lymphoblastic leukemia. Fifteen members of the two kindreds had thrombocytopenia, five of whom also had acute lymphoblastic leukemia. The L249P kindred also had one family member with renal cell carcinoma and another family member with Duodenal cancer. The relationship of these two cancers to the L249P mutation has not been investigated. In all events these two familial thrombocytopenia syndromes appear distinctly different than the thrombocytopenia 5 syndrome.[13]
Treatment[edit]
Family members with thrombocytopenia 5 need to be regularly monitored with complete blood count and blood smear screenings to detect the early changes brought on by the malignant transformations of this disease into hematological neoplasms. Patients who developed these transformations have generally been treated similarly to patients who have the same hematological neoplasms but on a non-familial basis. Patients developing non-malignant hematological or non-hematological solid tumor manifestations of thrombocytopenia 5 are also treated like to patients with the same but no-familial disease.[11][12]
The acute lymphoblastic leukemia associated with L349P or N385fs mutations in ETV6 appeared far less sensitive to standard chemotherapy for acute lymphoblastic leukemia with 2 among 3 family members moving rather quickly from chemotherapy to bone marrow transplantation and the third family member expiring. This suggest that these mutation-related forms of acute lymphoblastic leukemia require aggressive therapy.[13]
Acquired mutations[edit]
The ETV6 gene is prone to develop a wide range of acquired mutations in hematological precursor cells that lead to various types of leukemia and/or lymphoma. It may also suffer a smaller number of mutations in non-hematological tissues that leads to solid tumors. These mutations involve chromosome translocations which fuse the ETV6 on chromosome 12's the short (i.e. "p") arm ("q" stands for long arm) at position p13.2 (site notation: 12p12.2) near to a second gene on another chromosome or, more rarely, its own chromosome. This creates a fusion gene of the oncogene category which encodes a chimeric protein that promotes the malignant growth of its parent cells. It may be unclear which portion of the newly formed oncoprotein contributes to the ensuing malignancy but fusions between ETV6 and proteins with tyrosine kinase activity generally are converted from a protein with tightly regulated tyrosine kinase activity to an uncontrolled and continuously active tyrosine kinase that thereby promotes the malignant transformation of its parent cells.[14]
Hematological malignancies[edit]
The following table lists the more frequently occurring genes to which ETV6 fuses, the function of these genes, these genes' chromosomal locations, the notation designating the most common sites of the translocations of these fused genes, and the malignancies resulting from these translocations. These translocation mutations commonly occur in pluripotent hematopoietic stem cells that differentiate into various types of mature hematological cells. Consequently, a given mutation may lead to various types of hematological malignancies.[5][14] The table includes abbreviations for tyrosine kinase receptor (TK receptor), non-receptor tyrosine kinase (non-receptor TK), homeobox protein type of transcription factor (homeobox protein), acute lymphocytic leukemia (ALL), Philadelphia chromosome negative chronic myelogenous leukemia (Ph(-)CML), myelodysplastic syndrome (MDS), myeloproliferative neoplasm (MPN), and acute myeloid leukemia (AML). The presence of ETV6 gene mutations in myelodysplastic syndromes is associated with shortened survival.[15]
| Gene | function | location | notation | malignancies | gene | function | location | notation | malignancies | |
|---|---|---|---|---|---|---|---|---|---|---|
| PDGFRA | TK receptor | 4q12 | t(4;12)(q27?3;p13) | 40% to 50% of clonal eosinophilia patients | PDGFRB | TK receptor | 5q32 | t(5;12)(q31-33;p13) | rare clonal eosinophilia patients | |
| FLT3 | TK receptor | 13q12.2 | t(12;13)(q13.1;p12.3-13) | rare AML, ALL, and clonal eosinophilia patients | ABL1 | non-receptor TK | 9q34.12 | t(9;12)(q34;p13) | rare AML, B-cell or T-cell ALL, Ph(-)CML patients | |
| RUNX1 | transcription factor | 21q22.12 | t(12;21)(p13;q22) | 20-25% of pediatric ALL patients | PAX5 | homeobox protein | 9p13.2 | t(9;12)(q11;p13) | 1% of pediatric ALL patients | |
| MNX1 | homeobox protein | 7q36.3 | t(7:12)(q36;p13) | 20-30% of pediatric ALL patients less than 18 months old | MECOM | Transcription factor | 3q26.2 | t(3;12)(q26;p13) | rare MDS, MPN, and AML patients |
In addition to the fusion gene-producing translocations given in the table, ETV6 has been reported to fuse with other genes in very rare cases (i.e. 1-10 published reports). These translocations lead to one or more of the same types of hematological malignancies listed in the table. Thus, the ETV6 gene reportedly forms translocation-induced fusion genes with:[5] a) tyrosine kinase receptor gene FGFR3; b) non-receptor tyrosine kinase genes ABL2, NTRK3, JAK2, SYK, FRK, and LYN; c) transcription factor genes MN1 and PER1; d) homeobox protein transcription factor CDX2; e) Protein tyrosine phosphatase receptor-type R gene PTPRR;[16] f) transcriptional coactivator for nuclear hormone receptors gene NCOA2; f) Immunoglobulin heavy chain gene IGH;[17] g) enzyme genes TTL (adds and removes tyrosine residues on α-tubulin),[18] GOT1 (an Aspartate transaminase), and ACSL6 (a Long-chain-fatty-acid—CoA ligase); h) transporter gene ARNT (binds to ligand-bound aryl hydrocarbon receptor to aid in its movement to the nucleus where it promotes the expression of genes involved in xenobiotic metabolism); i) unknown function genes CHIC2,[19] MDS2,[20] FCHO2[21] and BAZ2A.;[22] and j) non-annotated gene STL (which has no long open reading frame[23]).
At least 9 frameshift mutations in the'ETV6 gene have been associated with ~12% of adult T cell Acute lymphoblastic leukemia cases. These mutations involve insertions or deletions in the gene that lead to its encoding a truncated and therefore inactive ETV6 protein. These mutations commonly occur alongside mutations in another oncogene, NOTCH1, which is associated with T cell acute lymphoblastic lymphoma quite independently of ETV6. It is suggested that suppressor mutations in the ETV6 gene may be a contributing factor in the development ant/or progression of this leukemia type.[8][24][25]
Treatment[edit]
Patients developing hematological malignancies secondary to the ETV6 gene fusion to receptor tyrosine kinases and non-receptor tyrosine kinases may be sensitive to therapy with tyrosine kinase inhibitors.[26] For example, patients with clonal eosinophilias due to PDGFRA or PDGFRB fusion genes experience long-term, complete remission when treated with are highly sensitive tyrosine kinase inhibitor, gleevec.[14] Larotrectinib, entrectinib, merestinib, and server other broadly acting tyrosine kinase inhibitors target the NTRK3 gene. Many of these drugs are in phase 1 or phase 2 clinical trials for the treatment of ETV6-NTRK3-related solid tumors and may ultimately prove useful for treating hematologic malignancies associated with this fusion gene.[27] Clinical trials have found that the first generation tyrosine kinase inhibitors sorafenib, sunitinib, midostaurin, lestaurtinib have shown some promise in treating acute myelogenous leukemia associated with the FLT3-TKI fusion gene; the second generation tyrosine kinase inhibitors quizartinib and crenolanib which are highly selective in inhibiting the FLT3 protein, have shown significant promise in treating relapsed and refractory acute myelogenous leukemia related to the FLT3-TKI fusion gene.[28] One patient with ETV6-FLT3-related myeloid/lymphoid neoplasm obtained a short term remission on sunitinib and following relapse, on sorafenib suggesting that the cited FLT3 protein tyrosine kinase inhibitors may prove useful for treating ETV6-FLT-related hematologic malignancies.[29] Two patients suffering hematologic malignancies related to PCM1-JAK2 or BCR-JAK2 fusion genes experienced complete and cytogenetic remissions in response to the tyrosine kinase inhibitor ruxolitinib; while both remissions were short-term (12 months), these results suggest that tyrosine kinase inhibitors that target JAK2 may be of some use for treating hematologic malignancies associated with ETV6-JAK2 fusion stems.[14] An inhibitor of SYK tyrosine kinase, TAK-659 is currently undergoing Phase I clinical trials for advanced lymphoma malignancies and may prove to be useful in treating this disease when associated with the ETV6-SYK fusion gene.[30] It is possible that hematological malignancies associated with ETV6 gene fusions to either the SYK or FRK tyrosine kinase genes may someday be shown susceptible to tyrosine kinase inhibitor therapy. However, children with ETV6-RUNX1-associated acute lymphoblastic leukemia are in an especially good-risk subgroup and therefore have been almost uniformly treated with standard-risk chemotherapy protocols.[31]
Hematological malignancies associated with ETY6 gene fusions to other transcription factor genes appear to reflect a loss or gain in function of ETV6 and/or the other genes in regulating expression of their target genes; this results in the formation or lack of formation of products which influence cell growth, proliferation, and/or survival. In vitro studies of ETV6-RUNX, ETV6-MN1, ETV6-PER1, and ETV6-MECOM fusion genes support this notion. Thus, the ETV6-MECOM fusion gene is overexpressed because it is driven by the promoter derived from ETV6[5] whereas the ETV6-RUNX, ETV6-MN1, and ETV6-PER1 fusion genes produce chimeric proteins which lack ETV6 protein's gene-suppressing activity.[32] The chimeric protein products of ETV6 gene fusions with ARNT, TTL, BA22A, FCHO2, MDS2, and CHIC2 likewise lack ETV6 protein's transcription factor activity.[32] Gene fusions between ETV6 and the homeobox gens (i.e. CDX2, PAX5, and MNX1) produce chimeric proteins with lack either ETV6s and/or CDX2s, PAX5s or MNX1s transcription factor activity.[5] In all events, hematological malignancies associated with these fusion genes have been treated with standard chemotherapy protocols selected on the basis of the malignancies phenotype.
Solid Tumors[edit]
Mutations in the ETV6 gene are also associated with solid tumors. In particular, the ETV6-NTRK3 fusion gene occurs in and is thought or proposed to drive certain types of cancers. These cancers include secretory breast cancer (also termed juvenile breast cancer), mammary analogue secretory carcinoma of the parotid and other salivary glands, congenital fibrosarcoma, congenital mesoblastic nephroma, inflammatory myofibroblastic tumor, and radiation-induced papillary thyroid carcinoma.[8][33][34][35][27][36][32][37]
Treatment[edit]
The treatment of ETV6 gene-associated solid tumors has not advanced as far as that for ETV6 gene-associated hematological malignancies. It is proposed that tyrosine kinase inhibitors with specificity for NTRK3's tyrosine kinase activity in ETV6-NTRK3 gene-associated solid tumors may be of therapeutic usefulness. Entrectinib, a pan-NTRK as well as an ALK and ROS1 tyrosine kinase inhibitor has been found useful in treating a single patient with ETV6-NRTK3 fusion gene-associated mammary analogue secretory carcinoma and lends support to the clinical development of NTRK3-directed tyrosine kinase inhibitors to treat ETV6-NTRK3 fusion protein associated malignancies.[27] Three clinical trials are in the recruitment phase for determining the efficacy of treating a wide range of solid tumors associated with mutated, overactive tyrosine kinase proteins, including the ETV6-TRK3 protein, with larotrectinib, a non-selective inhibitor of NTRK1, NTRK2, and NTRK3 tyrosine kinases.[38]
See also[edit]
References[edit]
- ^ a b c GRCh38: Ensembl release 89: ENSG00000139083 – Ensembl, May 2017
- ^ a b c GRCm38: Ensembl release 89: ENSMUSG00000030199 – Ensembl, May 2017
- ^ "Human PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ "Mouse PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ a b c d e f g De Braekeleer E, Douet-Guilbert N, Morel F, Le Bris MJ, Basinko A, De Braekeleer M (August 2012). "ETV6 fusion genes in hematological malignancies: a review". Leukemia Research. 36 (8): 945–61. doi:10.1016/j.leukres.2012.04.010. PMID 22578774.
- ^ Online Mendelian Inheritance in Man (OMIM): ETS Variant Gene 6; ETV6 - 600618
- ^ a b c Songdej N, Rao AK (May 2017). "Hematopoietic transcription factor mutations: important players in inherited platelet defects". Blood. 129 (21): 2873–2881. doi:10.1182/blood-2016-11-709881. PMC 5445569. PMID 28416505.
- ^ a b c Sizemore GM, Pitarresi JR, Balakrishnan S, Ostrowski MC (June 2017). "The ETS family of oncogenic transcription factors in solid tumours". Nature Reviews. Cancer. 17 (6): 337–351. doi:10.1038/nrc.2017.20. PMID 28450705. S2CID 32483397.
- ^ Kwiatkowski BA, Bastian LS, Bauer TR, Tsai S, Zielinska-Kwiatkowska AG, Hickstein DD (July 1998). "The ets family member Tel binds to the Fli-1 oncoprotein and inhibits its transcriptional activity". The Journal of Biological Chemistry. 273 (28): 17525–30. doi:10.1074/jbc.273.28.17525. PMID 9651344.
- ^ Nordentoft I, Jørgensen P (August 2003). "The acetyltransferase 60 kDa trans-acting regulatory protein of HIV type 1-interacting protein (Tip60) interacts with the translocation E26 transforming-specific leukaemia gene (TEL) and functions as a transcriptional co-repressor". The Biochemical Journal. 374 (Pt 1): 165–73. doi:10.1042/BJ20030087. PMC 1223570. PMID 12737628.
- ^ a b c Bannon SA, DiNardo CD (May 2016). "Hereditary Predispositions to Myelodysplastic Syndrome". International Journal of Molecular Sciences. 17 (6): 838. doi:10.3390/ijms17060838. PMC 4926372. PMID 27248996.
- ^ a b Zhang MY, Churpek JE, Keel SB, Walsh T, Lee MK, Loeb KR, Gulsuner S, Pritchard CC, Sanchez-Bonilla M, Delrow JJ, Basom RS, Forouhar M, Gyurkocza B, Schwartz BS, Neistadt B, Marquez R, Mariani CJ, Coats SA, Hofmann I, Lindsley RC, Williams DA, Abkowitz JL, Horwitz MS, King MC, Godley LA, Shimamura A (February 2015). "Germline ETV6 mutations in familial thrombocytopenia and hematologic malignancy". Nature Genetics. 47 (2): 180–5. doi:10.1038/ng.3177. PMC 4540357. PMID 25581430.
- ^ a b Topka S, Vijai J, Walsh MF, Jacobs L, Maria A, Villano D, Gaddam P, Wu G, McGee RB, Quinn E, Inaba H, Hartford C, Pui CH, Pappo A, Edmonson M, Zhang MY, Stepensky P, Steinherz P, Schrader K, Lincoln A, Bussel J, Lipkin SM, Goldgur Y, Harit M, Stadler ZK, Mullighan C, Weintraub M, Shimamura A, Zhang J, Downing JR, Nichols KE, Offit K (June 2015). "Germline ETV6 Mutations Confer Susceptibility to Acute Lymphoblastic Leukemia and Thrombocytopenia". PLOS Genetics. 11 (6): e1005262. doi:10.1371/journal.pgen.1005262. PMC 4477877. PMID 26102509.
- ^ a b c d Reiter A, Gotlib J (February 2017). "Myeloid neoplasms with eosinophilia". Blood. 129 (6): 704–714. doi:10.1182/blood-2016-10-695973. PMID 28028030.
- ^ Gangat N, Patnaik MM, Tefferi A (January 2016). "Myelodysplastic syndromes: Contemporary review and how we treat". American Journal of Hematology. 91 (1): 76–89. doi:10.1002/ajh.24253. PMID 26769228.
- ^ "PTPRR protein tyrosine phosphatase, receptor type R (human0". Entrez Gene.
- ^ "IGH immunoglobulin heavy locus (human )". Entrez Gene.
- ^ "TTL tubulin tyrosine ligase (human)". Entrez Gene.
- ^ "CHIC2 cysteine rich hydrophobic domain 2 (human)". Entrez Gene.
- ^ "MDS2 myelodysplastic syndrome 2 translocation associated". Entrez Gene.
- ^ "FCHO2 FCH domain only 2". Entrez Gene.
- ^ "BAZ2A bromodomain adjacent to zinc finger domain 2A". Entrez Gene.
- ^ Suto Y, Sato Y, Smith SD, Rowley JD, Bohlander SK (April 1997). "A t(6;12)(q23;p13) results in the fusion of ETV6 to a novel gene, STL, in a B-cell ALL cell line". Genes, Chromosomes & Cancer. 18 (4): 254–68. doi:10.1002/(sici)1098-2264(199704)18:4<254::aid-gcc3>3.0.co;2-#. PMID 9087565. S2CID 196600869.
- ^ Van Vlierberghe P, Ambesi-Impiombato A, Perez-Garcia A, Haydu JE, Rigo I, Hadler M, Tosello V, Della Gatta G, Paietta E, Racevskis J, Wiernik PH, Luger SM, Rowe JM, Rue M, Ferrando AA (December 2011). "ETV6 mutations in early immature human T cell leukemias". The Journal of Experimental Medicine. 208 (13): 2571–9. doi:10.1084/jem.20112239. PMC 3244026. PMID 22162831.
- ^ Sanchez-Martin M, Ferrando A (March 2017). "The NOTCH1-MYC highway toward T-cell acute lymphoblastic leukemia". Blood. 129 (9): 1124–1133. doi:10.1182/blood-2016-09-692582. PMID 28115368.
- ^ Gotlib J (December 2015). "Tyrosine Kinase Inhibitors and Therapeutic Antibodies in Advanced Eosinophilic Disorders and Systemic Mastocytosis". Current Hematologic Malignancy Reports. 10 (4): 351–61. doi:10.1007/s11899-015-0280-3. PMID 26404639. S2CID 36630735.
- ^ a b c Khotskaya YB, Holla VR, Farago AF, Mills Shaw KR, Meric-Bernstam F, Hong DS (May 2017). "Targeting TRK family proteins in cancer". Pharmacology & Therapeutics. 173: 58–66. doi:10.1016/j.pharmthera.2017.02.006. PMID 28174090. S2CID 4243668.
- ^ Tsapogas P, Mooney CJ, Brown G, Rolink A (May 2017). "The Cytokine Flt3-Ligand in Normal and Malignant Hematopoiesis". International Journal of Molecular Sciences. 18 (6): 1115. doi:10.3390/ijms18061115. PMC 5485939. PMID 28538663.
- ^ Walz C, Erben P, Ritter M, Bloor A, Metzgeroth G, Telford N, Haferlach C, Haferlach T, Gesk S, Score J, Hofmann WK, Hochhaus A, Cross NC, Reiter A (August 2011). "Response of ETV6-FLT3-positive myeloid/lymphoid neoplasm with eosinophilia to inhibitors of FMS-like tyrosine kinase 3". Blood. 118 (8): 2239–42. doi:10.1182/blood-2011-03-343426. PMID 21705501.
- ^ Lam B, Arikawa Y, Cramlett J, Dong Q, de Jong R, Feher V, Grimshaw CE, Farrell PJ, Hoffman ID, Jennings A, Jones B, Matuszkiewicz J, Miura J, Miyake H, Natala SR, Shi L, Takahashi M, Taylor E, Wyrick C, Yano J, Zalevsky J, Nie Z (December 2016). "Discovery of TAK-659 an orally available investigational inhibitor of Spleen Tyrosine Kinase (SYK)". Bioorganic & Medicinal Chemistry Letters. 26 (24): 5947–5950. doi:10.1016/j.bmcl.2016.10.087. PMID 27839918.
- ^ Harrison CJ (2013). "Targeting signaling pathways in acute lymphoblastic leukemia: new insights" (PDF). Hematology. American Society of Hematology. Education Program. 2013: 118–25. doi:10.1182/asheducation-2013.1.118. PMID 24319172. S2CID 24762855.
- ^ a b c Kar A, Gutierrez-Hartmann A (2013). "Molecular mechanisms of ETS transcription factor-mediated tumorigenesis". Critical Reviews in Biochemistry and Molecular Biology. 48 (6): 522–43. doi:10.3109/10409238.2013.838202. PMC 4086824. PMID 24066765.
- ^ Tognon C, Knezevich SR, Huntsman D, Roskelley CD, Melnyk N, Mathers JA, Becker L, Carneiro F, MacPherson N, Horsman D, Poremba C, Sorensen PH (November 2002). "Expression of the ETV6-NTRK3 gene fusion as a primary event in human secretory breast carcinoma". Cancer Cell. 2 (5): 367–76. doi:10.1016/S1535-6108(02)00180-0. PMID 12450792.
- ^ Majewska H, Skálová A, Stodulski D, Klimková A, Steiner P, Stankiewicz C, Biernat W. "Mammary analogue secretory carcinoma of salivary glands: a new entity associated with ETV6 gene rearrangement." Virchows Arch. 2015 Mar;466(3):245-54. doi: 10.1007/s00428-014-1701-8. Epub 2014 Dec 12.
- ^ Argani P, Fritsch M, Kadkol SS, Schuster A, Beckwith JB, Perlman EJ (January 2000). "Detection of the ETV6-NTRK3 chimeric RNA of infantile fibrosarcoma/cellular congenital mesoblastic nephroma in paraffin-embedded tissue: application to challenging pediatric renal stromal tumors". Modern Pathology. 13 (1): 29–36. doi:10.1038/modpathol.3880006. PMID 10658907.
- ^ Skalova A, Michal M, Simpson RH (January 2017). "Newly described salivary gland tumors". Modern Pathology. 30 (s1): S27–S43. doi:10.1038/modpathol.2016.167. PMID 28060365.
- ^ Alassiri AH, Ali RH, Shen Y, Lum A, Strahlendorf C, Deyell R, Rassekh R, Sorensen PH, Laskin J, Marra M, Yip S, Lee CH, Ng TL (August 2016). "ETV6-NTRK3 Is Expressed in a Subset of ALK-Negative Inflammatory Myofibroblastic Tumors". The American Journal of Surgical Pathology. 40 (8): 1051–61. doi:10.1097/PAS.0000000000000677. PMID 27259007. S2CID 25165398.
- ^ "Search for ETV6-NTRK". ClinicalTrials.gov.
Further reading[edit]
- Keung YK, Beaty M, Steward W, Jackle B, Pettnati M (October 2002). "Chronic myelocytic leukemia with eosinophilia, t(9;12)(q34;p13), and ETV6-ABL gene rearrangement: case report and review of the literature". Cancer Genetics and Cytogenetics. 138 (2): 139–42. doi:10.1016/S0165-4608(02)00609-X. PMID 12505259.
- Fainstein E, Einat M, Gokkel E, Marcelle C, Croce CM, Gale RP, Canaani E (December 1989). "Nucleotide sequence analysis of human abl and bcr-abl cDNAs". Oncogene. 4 (12): 1477–81. PMID 2687768.
- Buijs A, Sherr S, van Baal S, van Bezouw S, van der Plas D, Geurts van Kessel A, Riegman P, Lekanne Deprez R, Zwarthoff E, Hagemeijer A (April 1995). "Translocation (12;22) (p13;q11) in myeloproliferative disorders results in fusion of the ETS-like TEL gene on 12p13 to the MN1 gene on 22q11". Oncogene. 10 (8): 1511–9. PMID 7731705.
- Golub TR, Barker GF, Bohlander SK, Hiebert SW, Ward DC, Bray-Ward P, Morgan E, Raimondi SC, Rowley JD, Gilliland DG (May 1995). "Fusion of the TEL gene on 12p13 to the AML1 gene on 21q22 in acute lymphoblastic leukemia". Proceedings of the National Academy of Sciences of the United States of America. 92 (11): 4917–21. Bibcode:1995PNAS...92.4917G. doi:10.1073/pnas.92.11.4917. PMC 41818. PMID 7761424.
- Romana SP, Mauchauffé M, Le Coniat M, Chumakov I, Le Paslier D, Berger R, Bernard OA (June 1995). "The t(12;21) of acute lymphoblastic leukemia results in a tel-AML1 gene fusion". Blood. 85 (12): 3662–70. doi:10.1182/blood.V85.12.3662.bloodjournal85123662. PMID 7780150.
- Papadopoulos P, Ridge SA, Boucher CA, Stocking C, Wiedemann LM (January 1995). "The novel activation of ABL by fusion to an ets-related gene, TEL". Cancer Research. 55 (1): 34–8. PMID 7805037.
- Golub TR, Barker GF, Lovett M, Gilliland DG (April 1994). "Fusion of PDGF receptor beta to a novel ets-like gene, tel, in chronic myelomonocytic leukemia with t(5;12) chromosomal translocation". Cell. 77 (2): 307–16. doi:10.1016/0092-8674(94)90322-0. PMID 8168137. S2CID 30073372.
- Wlodarska I, Baens M, Peeters P, Aerssens J, Mecucci C, Brock P, Marynen P, Van den Berghe H (June 1996). "Biallelic alterations of both ETV6 and CDKN1B genes in a t(12;21) childhood acute lymphoblastic leukemia case". Cancer Research. 56 (11): 2655–61. PMID 8653712.
- Baens M, Peeters P, Guo C, Aerssens J, Marynen P (May 1996). "Genomic organization of TEL: the human ETS-variant gene 6". Genome Research. 6 (5): 404–13. doi:10.1101/gr.6.5.404. PMID 8743990.
- Bonaldo MF, Lennon G, Soares MB (September 1996). "Normalization and subtraction: two approaches to facilitate gene discovery". Genome Research. 6 (9): 791–806. doi:10.1101/gr.6.9.791. PMID 8889548.
- Hillier LD, Lennon G, Becker M, Bonaldo MF, Chiapelli B, Chissoe S, Dietrich N, DuBuque T, Favello A, Gish W, Hawkins M, Hultman M, Kucaba T, Lacy M, Le M, Le N, Mardis E, Moore B, Morris M, Parsons J, Prange C, Rifkin L, Rohlfing T, Schellenberg K, Bento Soares M, Tan F, Thierry-Meg J, Trevaskis E, Underwood K, Wohldman P, Waterston R, Wilson R, Marra M (September 1996). "Generation and analysis of 280,000 human expressed sequence tags". Genome Research. 6 (9): 807–28. doi:10.1101/gr.6.9.807. PMID 8889549.
- Andreasson P, Johansson B, Arheden K, Billström R, Mitelman F, Höglund M (June 1997). "Deletions of CDKN1B and ETV6 in acute myeloid leukemia and myelodysplastic syndromes without cytogenetic evidence of 12p abnormalities". Genes, Chromosomes & Cancer. 19 (2): 77–83. doi:10.1002/(SICI)1098-2264(199706)19:2<77::AID-GCC2>3.0.CO;2-X. PMID 9171997. S2CID 27083284.
- Lacronique V, Boureux A, Valle VD, Poirel H, Quang CT, Mauchauffé M, Berthou C, Lessard M, Berger R, Ghysdael J, Bernard OA (November 1997). "A TEL-JAK2 fusion protein with constitutive kinase activity in human leukemia". Science. 278 (5341): 1309–12. Bibcode:1997Sci...278.1309L. doi:10.1126/science.278.5341.1309. PMID 9360930.
- Knezevich SR, McFadden DE, Tao W, Lim JF, Sorensen PH (February 1998). "A novel ETV6-NTRK3 gene fusion in congenital fibrosarcoma". Nature Genetics. 18 (2): 184–7. doi:10.1038/ng0298-184. PMID 9462753. S2CID 7390311.
- Kwiatkowski BA, Bastian LS, Bauer TR, Tsai S, Zielinska-Kwiatkowska AG, Hickstein DD (July 1998). "The ets family member Tel binds to the Fli-1 oncoprotein and inhibits its transcriptional activity". The Journal of Biological Chemistry. 273 (28): 17525–30. doi:10.1074/jbc.273.28.17525. PMID 9651344.
- Hannemann JR, McManus DM, Kabarowski JH, Wiedemann LM (July 1998). "Haemopoietic transformation by the TEL/ABL oncogene". British Journal of Haematology. 102 (2): 475–85. doi:10.1046/j.1365-2141.1998.00803.x. PMID 9695962. S2CID 25904172.
- Chakrabarti SR, Sood R, Ganguly S, Bohlander S, Shen Z, Nucifora G (June 1999). "Modulation of TEL transcription activity by interaction with the ubiquitin-conjugating enzyme UBC9". Proceedings of the National Academy of Sciences of the United States of America. 96 (13): 7467–72. Bibcode:1999PNAS...96.7467R. doi:10.1073/pnas.96.13.7467. PMC 22109. PMID 10377438.
- Cools J, Bilhou-Nabera C, Wlodarska I, Cabrol C, Talmant P, Bernard P, Hagemeijer A, Marynen P (September 1999). "Fusion of a novel gene, BTL, to ETV6 in acute myeloid leukemias with a t(4;12)(q11-q12;p13)". Blood. 94 (5): 1820–4. doi:10.1182/blood.V94.5.1820. PMID 10477709.
- Yagasaki F, Jinnai I, Yoshida S, Yokoyama Y, Matsuda A, Kusumoto S, Kobayashi H, Terasaki H, Ohyashiki K, Asou N, Murohashi I, Bessho M, Hirashima K (November 1999). "Fusion of TEL/ETV6 to a novel ACS2 in myelodysplastic syndrome and acute myelogenous leukemia with t(5;12)(q31;p13)". Genes, Chromosomes & Cancer. 26 (3): 192–202. doi:10.1002/(SICI)1098-2264(199911)26:3<192::AID-GCC2>3.0.CO;2-E. PMID 10502316.
- Wai DH, Knezevich SR, Lucas T, Jansen B, Kay RJ, Sorensen PH (February 2000). "The ETV6-NTRK3 gene fusion encodes a chimeric protein tyrosine kinase that transforms NIH3T3 cells". Oncogene. 19 (7): 906–15. doi:10.1038/sj.onc.1203396. PMID 10702799.
External links[edit]
- ETV6+protein,+human at the U.S. National Library of Medicine Medical Subject Headings (MeSH)
- Drosophila anterior open - The Interactive Fly
This article incorporates text from the United States National Library of Medicine, which is in the public domain.